Nutr Res Pract.
2012 Aug;6(4):315-321.
Effects of kimchi supplementation on blood pressure and cardiac hypertrophy with varying sodium content in spontaneously hypertensive rats
- Affiliations
-
- 1Department of Food and Nutrition and Institute of Health Sciences, Korea University, San 1, Jeongreung-dong, Seongbuk-gu, Seoul 136-703, Korea. mjshin@korea.ac.kr
- 2DAESANG FNF Corporation, Seoul 131-220, Korea.
Abstract
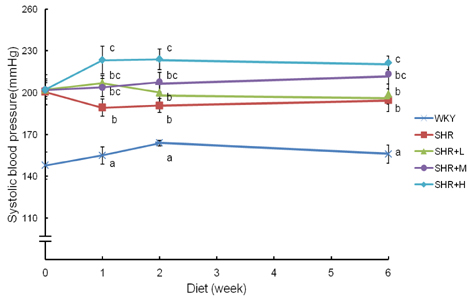
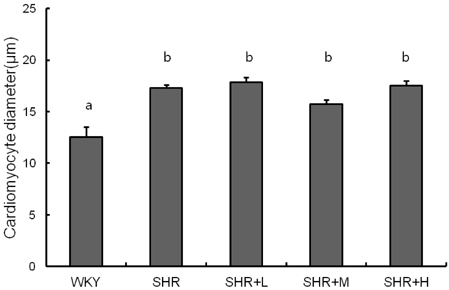
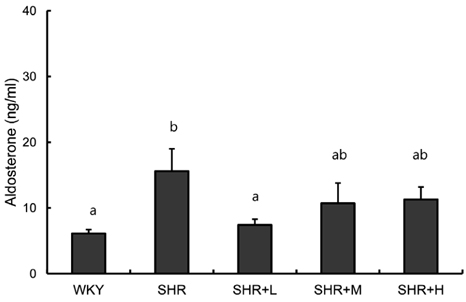
- We tested the effects of dietary intake of freeze-dried Korean traditional fermented cabbage (generally known as kimchi) with varying amounts of sodium on blood pressure and cardiac hypertrophy in spontaneously hypertensive rats (SHRs). Wistar-Kyoto rats (WKY), as a control group, received a regular AIN-76 diet, and the SHRs were divided into four groups. The SHR group was fed a regular diet without kimchi supplementation, the SHR-L group was fed the regular diet supplemented with low sodium kimchi containing 1.4% salt by wet weight, which was provided in a freeze-dried form, the SHR-M group was supplemented with medium levels of sodium kimchi containing 2.4% salt, and the SHR-H group was supplemented with high sodium kimchi containing 3.0% salt. Blood pressure was measured over 6 weeks, and cardiac hypertrophy was examined by measuring heart and left ventricle weights and cardiac histology. SHRs showed higher blood pressure compared to that in WKY rats, which was further elevated by consuming high sodium containing kimchi but was not influenced by supplementing with low sodium kimchi. None of the SHR groups showed significant differences in cardiac and left ventricular mass or cardiomyocyte size. Levels of serum biochemical parameters, including blood urea nitrogen, creatinine, glutamic-oxaloacetic transaminase, glutamic-pyruvic transaminase, sodium, and potassium were not different among the groups. Elevations in serum levels of aldosterone in SHR rats decreased in the low sodium kimchi group. These results suggest that consuming low sodium kimchi may not adversely affect blood pressure and cardiac function even under a hypertensive condition.
Keyword
MeSH Terms
-
Alanine Transaminase
Aldosterone
Animals
Aspartate Aminotransferases
Blood Pressure
Blood Urea Nitrogen
Brassica
Cardiomegaly
Creatinine
Diet
Heart
Heart Ventricles
Myocytes, Cardiac
Potassium
Rats
Rats, Inbred SHR
Rats, Inbred WKY
Sodium
Weights and Measures
Alanine Transaminase
Aldosterone
Aspartate Aminotransferases
Creatinine
Potassium
Sodium
Figure
Reference
-
1. Lee JS, Heo GY, Lee JW, Oh YJ, Park JA, Park YH, Pyun YR, Ahn JS. Analysis of kimchi microflora using denaturing gradient gel electrophoresis. Int J Food Microbiol. 2005. 102:143–150.
Article2. Lee J, Hwang KT, Heo MS, Lee JH, Park KY. Resistance of Lactobacillus plantarum KCTC 3099 from Kimchi to oxidative stress. J Med Food. 2005. 8:299–304.
Article3. Hur HJ, Lee KW, Lee HJ. Production of nitric oxide, tumor necrosis factor-alpha and interleukin-6 by RAW264.7 macrophage cells treated with lactic acid bacteria isolated from kimchi. Biofactors. 2004. 21:123–125.
Article4. Park KY, Cho EJ, Rhee SH, Jung KO, Yi SJ, Jhun BH. Kimchi and an active component, beta-sitosterol, reduce oncogenic H-Ras (v12)-induced DNA synthesis. J Med Food. 2003. 6:151–156.
Article5. Kim HJ, Lee JS, Chung HY, Song SH, Suh H, Noh JS, Song YO. 3-(4'-hydroxyl-3',5'-dimethoxyphenyl)propionic acid, an active principle of kimchi, inhibits development of atherosclerosis in rabbits. J Agric Food Chem. 2007. 55:10486–10492.
Article6. Lee YM, Kwon MJ, Kim JK, Suh HS, Choi JS, Song YO. Isolation and identification of active principle in Chinese cabbage Kimchi responsible for antioxidant effect. Korean J Food Sci Technol. 2004. 36:129–133.7. Noh JS, Kim HJ, Kwon MJ, Song YO. Active principle of kimchi, 3-(4'-hydroxyl-3',5'-dimethoxyphenyl)propionic acid, retards fatty streak formation at aortic sinus of apolipoprotein E knockout mice. J Med Food. 2009. 12:1206–1212.
Article8. Islam MS, Choi H. Antidiabetic effect of Korean traditional Baechu (Chinese cabbage) kimchi in a type 2 diabetes model of rats. J Med Food. 2009. 12:292–297.
Article9. Son SM, Park YS, Lim HJ, Kim SB, Jeong YS. Sodium intakes of Korean adults with 24-hour urine analysis and dish frequency questionnaire and comparison of sodium intakes according to the regional area and dish group. Korean J Community Nutr. 2007. 12:545–558.10. Park HR, Jeong GO, Lee SL, Kim JY, Kang SA, Park KY, Ryou HJ. Workers intake too much salt from dishes of eating out and food service cafeterias; direct chemical analysis of sodium content. Nutr Res Pract. 2009. 3:328–333.
Article11. Breslin PA, Beauchamp GK. Salt enhances flavour by suppressing bitterness. Nature. 1997. 387:563.
Article12. Lida M, Ueda K, Okayama A, Kodama K, Sawai K, Shibata S, Tanaka S, Keijnkai T, Horibe H, Minowa M, Yanagawa H, Hashimoto T. Nippon Data 80 Research Group. Impact of elevated blood pressure on mortality from all causes, cardiovascular diseases, heart disease and stroke among Japanese: 14 year follow-up of randomly selected population from Japanese -- Nippon data 80. J Hum Hypertens. 2003. 17:851–857.
Article13. Agarwal R. Blood pressure components and the risk for end-stage renal disease and death in chronic kidney disease. Clin J Am Soc Nephrol. 2009. 4:830–837.
Article14. Kearney PM, Whelton M, Reynolds K, Whelton PK, He J. Worldwide prevalence of hypertension: a systematic review. J Hypertens. 2004. 22:11–19.15. Pereira M, Lunet N, Azevedo A, Barros H. Differences in prevalence, awareness, treatment and control of hypertension between developing and developed countries. J Hypertens. 2009. 27:963–975.
Article16. Law MR. Epidemiologic evidence on salt and blood pressure. Am J Hypertens. 1997. 10:42S–45S.
Article17. Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D, Obarzanek E, Conlin PR, Miller ER 3rd, Simons-Morton DG, Karanja N, Lin PH. DASH-Sodium Collaborative Research Group. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med. 2001. 344:3–10.
Article18. Svetkey LP, Simons-Morton DG, Proschan MA, Sacks FM, Conlin PR, Harsha D, Moore TJ. Effect of the dietary approaches to stop hypertension diet and reduced sodium intake on blood pressure control. J Clin Hypertens (Greenwich). 2004. 6:373–381.
Article19. Midgley JP, Matthew AG, Greenwood CM, Logan AG. Effect of reduced dietary sodium on blood pressure: a meta-analysis of randomized controlled trials. JAMA. 1996. 275:1590–1597.
Article20. Chrysant SG, Walsh GM, Kem DC, Frohlich ED. Hemodynamic and metabolic evidence of salt sensitivity in spontaneously hypertensive rats. Kidney Int. 1979. 15:33–37.
Article21. Yi SH, Park SY, Jeong DH, Kim JY, Lee AJ, Shin HA, Moon JH, Lee JH, Kim SE, Ryou HJ, Om AS. Survey research of homemade and commercial cabbage(Baechu) kimchi on physicochemical quality characteristics. Korean J Food Cookery Sci. 2009. 25:671–676.22. Pollock DM, Polakowski JS, Divish BJ, Opgenorth TJ. Angiotensin blockade reverses hypertension during long-term nitric oxide synthase inhibition. Hypertension. 1993. 21:660–666.
Article23. Dahl LK, Love RA. Evidence for relationship between sodium (chloride) intake and human essential hypertension. AMA Arch Intern Med. 1954. 94:525–531.
Article24. Mancilha-Carvalho Jde J, Souza e Silva NA. The Yanomami Indians in the INTERSALT Study. Arq Bras Cardiol. 2003. 80:289–300.25. Frohlich ED, Varagic J. The role of sodium in hypertension is more complex than simply elevating arterial pressure. Nat Clin Pract Cardiovasc Med. 2004. 1:24–30.
Article26. Moser M, Hebert PR. Prevention of disease progression, left ventricular hypertrophy and congestive heart failure in hypertension treatment trials. J Am Coll Cardiol. 1996. 27:1214–1218.
Article27. Toto RD. Treatment of hypertension in chronic kidney disease. Semin Nephrol. 2005. 25:435–439.
Article28. Yu HC, Burrell LM, Black MJ, Wu LL, Dilley RJ, Cooper ME, Johnston CI. Salt induces myocardial and renal fibrosis in normotensive and hypertensive rats. Circulation. 1998. 98:2621–2628.
Article29. Leenen FH, Yuan B. Dietary-sodium-induced cardiac remodeling in spontaneously hypertensive rat versus Wistar-Kyoto rat. J Hypertens. 1998. 16:885–892.
Article30. Frohlich ED, Chien Y, Sesoko S, Pegram BL. Relationship between dietary sodium intake, hemodynamics, and cardiac mass in SHR and WKY rats. Am J Physiol. 1993. 264:R30–R34.
Article31. Gu JW, Anand V, Shek EW, Moore MC, Brady AL, Kelly WC, Adair TH. Sodium induces hypertrophy of cultured myocardial myoblasts and vascular smooth muscle cells. Hypertension. 1998. 31:1083–1087.
Article32. Varagic J, Frohlich ED, Díez J, Susic D, Ahn J, González A, López B. Myocardial fibrosis, impaired coronary hemodynamics, and biventricular dysfunction in salt-loaded SHR. Am J Physiol Heart Circ Physiol. 2006. 290:H1503–H1509.
Article33. Daniels SD, Meyer RA, Loggie JM. Determinants of cardiac involvement in children and adolescents with essential hypertension. Circulation. 1990. 82:1243–1248.
Article34. Cuspidi C, Vaccarella A, Negri F, Sala C. Resistant hypertension and left ventricular hypertrophy: an overview. J Am Soc Hypertens. 2010. 4:319–324.
Article35. Partovian C, Benetos A, Pommiès JP, Mischler W, Safar ME. Effects of a chronic high-salt diet on large artery structure: role of endogenous bradykinin. Am J Physiol. 1998. 274:H1423–H1428.36. MacGregor GA, Markandu ND, Roulston JE, Jones JC, Morton JJ. Maintenance of blood pressure by the renin-angiotensin system in normal man. Nature. 1981. 291:329–331.
Article37. He FJ, MacGregor GA. Salt, blood pressure and the renin-angiotensin system. J Renin Angiotensin Aldosterone Syst. 2003. 4:11–16.
Article38. Dzau V. The cardiovascular continuum and renin-angiotensin-aldosterone system blockade. J Hypertens Suppl. 2005. 23:S9–S17.
Article39. Lorell BH, Carabello BA. Left ventricular hypertrophy: pathogenesis, detection, and prognosis. Circulation. 2000. 102:470–479.40. Rettig R, Folberth C, Kopf D, Stauss H, Unger T. Role of the kidney in the pathogenesis of primary hypertension. Clin Exp Hypertens A. 1990. 12:957–1002.
Article41. Fukuda S, Tsuchikura S, Iida H. Age-related changes in blood pressure, hematological values, concentrations of serum biochemical constituents and weights of organs in the SHR/Izm, SHRSP/Izm and WKY/Izm. Exp Anim. 2004. 53:67–72.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Electron Microscopic Study of Enalapril Effect on Left Ventricular Hypertrophy in Spontaneously Hypertensive Rat
- Antihypertensive Properties of Dried Radish Leaves Powder in Spontaneously Hypertensive Rats
- The Effet of Nifedipine on the Blood Pressure, Water and Cation Balance of the Lens in Spontaneous Hypertensive Rats
- Epigallocatechin-3 gallate prevents cardiac hypertrophy induced by pressure overload in rats
- Supplementary Effect of Lentinus Edodes on Serum and Hepatic Lipid Levels in Spontaneously Hypertensive Rat