Allergy Asthma Immunol Res.
2013 Jul;5(4):189-196. 10.4168/aair.2013.5.4.189.
Immunopathogenesis of Allergic Asthma: More Than the Th2 Hypothesis
- Affiliations
-
- 1Department of Life Science, Pohang University of Science and Technology (POSTECH), Pohang, Korea. juinea@postech.ac.kr
- KMID: 2260311
- DOI: http://doi.org/10.4168/aair.2013.5.4.189
Abstract
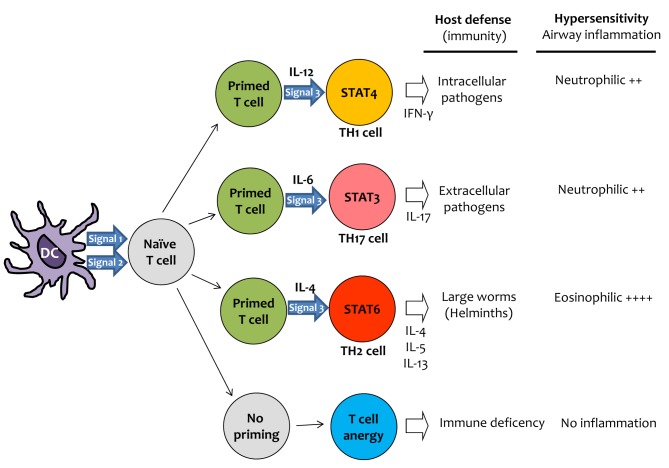
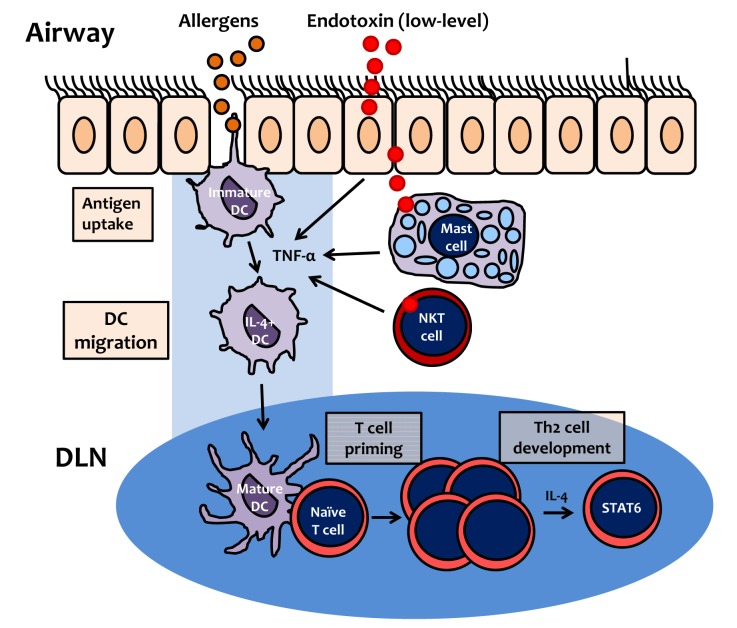
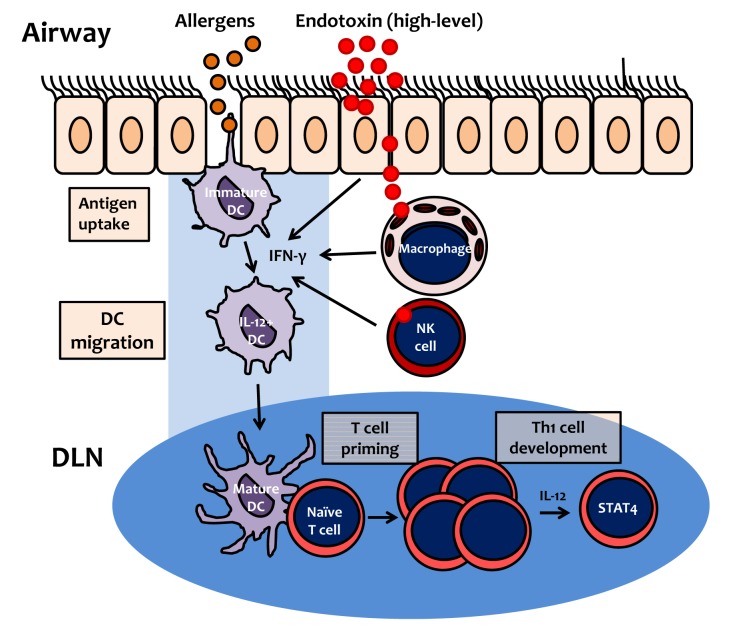
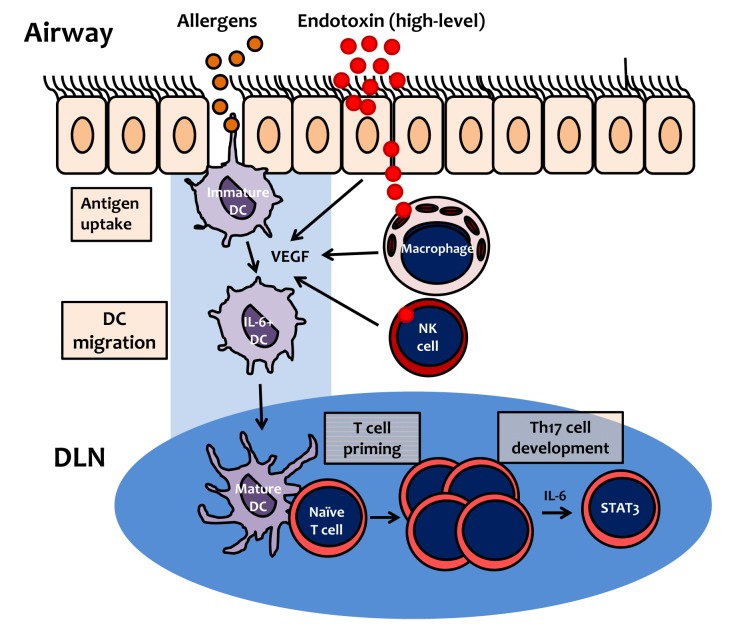
- Asthma is a chronic obstructive airway disease that involves inflammation of the respiratory tract. Biological contaminants in indoor air can induce innate and adaptive immune responses and inflammation, resulting in asthma pathology. Epidemiologic surveys indicate that the prevalence of asthma is higher in developed countries than in developing countries. The prevalence of asthma in Korea has increased during the last several decades. This increase may be related to changes in housing styles, which result in increased levels of indoor biological contaminants, such as house dust mite-derived allergens and bacterial products such as endotoxin. Different types of inflammation are observed in those suffering from mild-to-moderate asthma compared to those experiencing severe asthma, involving markedly different patterns of inflammatory cells and mediators. As described in this review, these inflammatory profiles are largely determined by the involvement of different T helper cell subsets, which orchestrate the recruitment and activation of inflammatory cells. It is becoming clear that T helper cells other than Th2 cells are involved in the pathogenesis of asthma; specifically, both Th1 and Th17 cells are crucial for the development of neutrophilic inflammation in the airways, which is related to corticosteroid resistance. Development of therapeutics that suppress these immune and inflammatory cells may provide useful asthma treatments in the future.
Keyword
MeSH Terms
Figure
Cited by 3 articles
-
Animal allergy in veterinarian researchers
Cheol-Woo Kim
Allergy Asthma Respir Dis. 2016;4(6):387-388. doi: 10.4168/aard.2016.4.6.387.An Alternative Dendritic Cell-Induced Murine Model of Asthma Exhibiting a Robust Th2/Th17-Skewed Response
Sang Chul Park, Hongmin Kim, Yeeun Bak, Dahee Shim, Kee Woong Kwon, Chang-Hoon Kim, Joo-Heon Yoon, Sung Jae Shin
Allergy Asthma Immunol Res. 2020;12(3):537-555. doi: 10.4168/aair.2020.12.3.537.Anti-Interleukin-9 Antibody Increases the Effect of Allergen-Specific Immunotherapy in Murine Allergic Rhinitis
Ji-Hyeon Shin, Do Hyun Kim, Boo-Young Kim, Sung Won Kim, Se Hwan Hwang, Joohyung Lee, Soo Whan Kim
Allergy Asthma Immunol Res. 2017;9(3):237-246. doi: 10.4168/aair.2017.9.3.237.
Reference
-
1. Agostinis F, Foglia C, Landi M, Cottini M, Lombardi C, Canonica GW, Passalacqua G. The safety of sublingual immunotherapy with one or multiple pollen allergens in children. Allergy. 2008; 63:1637–1639. PMID: 19032238.
Article2. Manniche L, Forman W. Sacred luxuries: fragrance, aromatherapy, and cosmetics in Ancient Egypt. New York, NY: Cornell University Press;1999.3. Opolski M, Wilson I. Asthma and depression: a pragmatic review of the literature and recommendations for future research. Clin Pract Epidemiol Ment Health. 2005; 1:18. PMID: 16185365.4. Louis R, Lau LC, Bron AO, Roldaan AC, Radermecker M, Djukanović R. The relationship between airways inflammation and asthma severity. Am J Respir Crit Care Med. 2000; 161:9–16. PMID: 10619791.
Article5. Vrugt B, Wilson S, Underwood J, Bron A, de Bruyn R, Bradding P, Holgate ST, Djukanovic R, Aalbers R. Mucosal inflammation in severe glucocorticoid-dependent asthma. Eur Respir J. 1999; 13:1245–1252. PMID: 10445597.
Article8. Kroegel C. Global Initiative for Asthma (GINA) guidelines: 15 years of application. Expert Rev Clin Immunol. 2009; 5:239–249. PMID: 20477002.
Article9. Lazarus SC. Clinical practice. Emergency treatment of asthma. N Engl J Med. 2010; 363:755–764. PMID: 20818877.10. Worldwide variation in prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and atopic eczema: ISAAC. The International Study of Asthma and Allergies in Childhood (ISAAC) Steering Committee. Lancet. 1998; 351:1225–1232. PMID: 9643741.11. Bateman ED, Hurd SS, Barnes PJ, Bousquet J, Drazen JM, FitzGerald M, Gibson P, Ohta K, O'Byrne P, Pedersen SE, Pizzichini E, Sullivan SD, Wenzel SE, Zar HJ. Global strategy for asthma management and prevention: GINA executive summary. Eur Respir J. 2008; 31:143–178. PMID: 18166595.
Article12. Denlinger LC, Sorkness CA, Chinchilli VM, Lemanske RF Jr. Guideline-defining asthma clinical trials of the National Heart, Lung, and Blood Institute's Asthma Clinical Research Network and Childhood Asthma Research and Education Network. J Allergy Clin Immunol. 2007; 119:3–11. quiz 12-3. PMID: 17141853.13. Moore WC, Meyers DA, Wenzel SE, Teague WG, Li H, Li X, D'Agostino R Jr, Castro M, Curran-Everett D, Fitzpatrick AM, Gaston B, Jarjour NN, Sorkness R, Calhoun WJ, Chung KF, Comhair SA, Dweik RA, Israel E, Peters SP, Busse WW, Erzurum SC, Bleecker ER. National Heart, Lung, and Blood Institute's Severe Asthma Research Program. Identification of asthma phenotypes using cluster analysis in the Severe Asthma Research Program. Am J Respir Crit Care Med. 2010; 181:315–323. PMID: 19892860.
Article14. Wills-Karp M, Luyimbazi J, Xu X, Schofield B, Neben TY, Karp CL, Donaldson DD. Interleukin-13: central mediator of allergic asthma. Science. 1998; 282:2258–2261. PMID: 9856949.
Article15. Holt PG, Macaubas C, Stumbles PA, Sly PD. The role of allergy in the development of asthma. Nature. 1999; 402:B12–B17. PMID: 10586890.
Article16. Savelkoul HF, Seymour BW, Sullivan L, Coffman RL. IL-4 can correct defective IgE production in SJA/9 mice. J Immunol. 1991; 146:1801–1805. PMID: 1826012.17. Dent LA, Strath M, Mellor AL, Sanderson CJ. Eosinophilia in transgenic mice expressing interleukin 5. J Exp Med. 1990; 172:1425–1431. PMID: 2230651.
Article18. Iwamoto I, Nakajima H, Endo H, Yoshida S. Interferon gamma regulates antigen-induced eosinophil recruitment into the mouse airways by inhibiting the infiltration of CD4+ T cells. J Exp Med. 1993; 177:573–576. PMID: 8093895.
Article19. Lack G, Bradley KL, Hamelmann E, Renz H, Loader J, Leung DY, Larsen G, Gelfand EW. Nebulized IFN-gamma inhibits the development of secondary allergic responses in mice. J Immunol. 1996; 157:1432–1439. PMID: 8759723.20. Turner MO, Hussack P, Sears MR, Dolovich J, Hargreave FE. Exacerbations of asthma without sputum eosinophilia. Thorax. 1995; 50:1057–1061. PMID: 7491553.
Article21. Wenzel SE, Schwartz LB, Langmack EL, Halliday JL, Trudeau JB, Gibbs RL, Chu HW. Evidence that severe asthma can be divided pathologically into two inflammatory subtypes with distinct physiologic and clinical characteristics. Am J Respir Crit Care Med. 1999; 160:1001–1008. PMID: 10471631.
Article22. Marguet C, Jouen-Boedes F, Dean TP, Warner JO. Bronchoalveolar cell profiles in children with asthma, infantile wheeze, chronic cough, or cystic fibrosis. Am J Respir Crit Care Med. 1999; 159:1533–1540. PMID: 10228122.
Article23. Gibson PG, Simpson JL, Saltos N. Heterogeneity of airway inflammation in persistent asthma : evidence of neutrophilic inflammation and increased sputum interleukin-8. Chest. 2001; 119:1329–1336. PMID: 11348936.24. Green RH, Brightling CE, Woltmann G, Parker D, Wardlaw AJ, Pavord ID. Analysis of induced sputum in adults with asthma: identification of subgroup with isolated sputum neutrophilia and poor response to inhaled corticosteroids. Thorax. 2002; 57:875–879. PMID: 12324674.
Article25. Wanner A, Abraham WM, Douglas JS, Drazen JM, Richerson HB, Ram JS. NHLBI Workshop Summary. Models of airway hyperresponsiveness. Am Rev Respir Dis. 1990; 141:253–257. PMID: 2297181.26. Turner DJ, Myron P, Powell WS, Martin JG. The role of endogenous corticosterone in the late-phase response to allergen challenge in the brown Norway rat. Am J Respir Crit Care Med. 1996; 153:545–550. PMID: 8564095.
Article27. Dybas JM, Andresen CJ, Schelegle ES, McCue RW, Callender NN, Jackson AC. Deep-breath frequency in bronchoconstricted monkeys (Macaca fascicularis). J Appl Physiol. 2006; 100:786–791. PMID: 16467390.
Article28. Marsh WR, Irvin CG, Murphy KR, Behrens BL, Larsen GL. Increases in airway reactivity to histamine and inflammatory cells in bronchoalveolar lavage after the late asthmatic response in an animal model. Am Rev Respir Dis. 1985; 131:875–879. PMID: 4003939.29. Dunn CJ, Elliott GA, Oostveen JA, Richards IM. Development of a prolonged eosinophil-rich inflammatory leukocyte infiltration in the guinea-pig asthmatic response to ovalbumin inhalation. Am Rev Respir Dis. 1988; 137:541–547. PMID: 3345036.
Article30. Mosmann TR, Cherwinski H, Bond MW, Giedlin MA, Coffman RL. Two types of murine helper T cell clone. I. Definition according to profiles of lymphokine activities and secreted proteins. J Immunol. 1986; 136:2348–2357. PMID: 2419430.31. Boehm U, Klamp T, Groot M, Howard JC. Cellular responses to interferon-gamma. Annu Rev Immunol. 1997; 15:749–795. PMID: 9143706.32. Kim YK, Oh SY, Jeon SG, Park HW, Lee SY, Chun EY, Bang B, Lee HS, Oh MH, Kim YS, Kim JH, Gho YS, Cho SH, Min KU, Kim YY, Zhu Z. Airway exposure levels of lipopolysaccharide determine type 1 versus type 2 experimental asthma. J Immunol. 2007; 178:5375–5382. PMID: 17404323.
Article33. Kim YS, Hong SW, Choi JP, Shin TS, Moon HG, Choi EJ, Jeon SG, Oh SY, Gho YS, Zhu Z, Kim YK. Vascular endothelial growth factor is a key mediator in the development of T cell priming and its polarization to type 1 and type 17 T helper cells in the airways. J Immunol. 2009; 183:5113–5120. PMID: 19786548.
Article34. Tanaka T, Katada Y, Higa S, Fujiwara H, Wang W, Saeki Y, Ohshima S, Okuda Y, Suemura M, Kishimoto T. Enhancement of T helper2 response in the absence of interleukin (IL-)6; an inhibition of IL-4-mediated T helper2 cell differentiation by IL-6. Cytokine. 2001; 13:193–201. PMID: 11237426.35. Greenfeder S, Umland SP, Cuss FM, Chapman RW, Egan RW. Th2 cytokines and asthma. The role of interleukin-5 in allergic eosinophilic disease. Respir Res. 2001; 2:71–79. PMID: 11686868.36. Pope SM, Brandt EB, Mishra A, Hogan SP, Zimmermann N, Matthaei KI, Foster PS, Rothenberg ME. IL-13 induces eosinophil recruitment into the lung by an IL-5- and eotaxin-dependent mechanism. J Allergy Clin Immunol. 2001; 108:594–601. PMID: 11590387.
Article37. Lukacs NW, Strieter RM, Chensue SW, Kunkel SL. Interleukin-4-dependent pulmonary eosinophil infiltration in a murine model of asthma. Am J Respir Cell Mol Biol. 1994; 10:526–532. PMID: 8179915.
Article38. Shimoda K, van Deursen J, Sangster MY, Sarawar SR, Carson RT, Tripp RA, Chu C, Quelle FW, Nosaka T, Vignali DA, Doherty PC, Grosveld G, Paul WE, Ihle JN. Lack of IL-4-induced Th2 response and IgE class switching in mice with disrupted Stat6 gene. Nature. 1996; 380:630–633. PMID: 8602264.39. Fish SC, Donaldson DD, Goldman SJ, Williams CM, Kasaian MT. IgE generation and mast cell effector function in mice deficient in IL-4 and IL-13. J Immunol. 2005; 174:7716–7724. PMID: 15944273.
Article40. Punnonen J, Aversa G, Cocks BG, McKenzie AN, Menon S, Zurawski G, de Waal Malefyt R, de Vries JE. Interleukin 13 induces interleukin 4-independent IgG4 and IgE synthesis and CD23 expression by human B cells. Proc Natl Acad Sci U S A. 1993; 90:3730–3734. PMID: 8097323.
Article41. Mangan PR, Harrington LE, O'Quinn DB, Helms WS, Bullard DC, Elson CO, Hatton RD, Wahl SM, Schoeb TR, Weaver CT. Transforming growth factor-beta induces development of the T(H)17 lineage. Nature. 2006; 441:231–234. PMID: 16648837.42. Korn T, Bettelli E, Oukka M, Kuchroo VK. IL-17 and Th17 Cells. Annu Rev Immunol. 2009; 27:485–517. PMID: 19132915.
Article43. Molet S, Hamid Q, Davoine F, Nutku E, Taha R, Pagé N, Olivenstein R, Elias J, Chakir J. IL-17 is increased in asthmatic airways and induces human bronchial fibroblasts to produce cytokines. J Allergy Clin Immunol. 2001; 108:430–438. PMID: 11544464.
Article44. Schnyder-Candrian S, Togbe D, Couillin I, Mercier I, Brombacher F, Quesniaux V, Fossiez F, Ryffel B, Schnyder B. Interleukin-17 is a negative regulator of established allergic asthma. J Exp Med. 2006; 203:2715–2725. PMID: 17101734.
Article45. McKinley L, Alcorn JF, Peterson A, Dupont RB, Kapadia S, Logar A, Henry A, Irvin CG, Piganelli JD, Ray A, Kolls JK. TH17 cells mediate steroid-resistant airway inflammation and airway hyperresponsiveness in mice. J Immunol. 2008; 181:4089–4097. PMID: 18768865.
Article46. Kawaguchi M, Kokubu F, Kuga H, Matsukura S, Hoshino H, Ieki K, Imai T, Adachi M, Huang SK. Modulation of bronchial epithelial cells by IL-17. J Allergy Clin Immunol. 2001; 108:804–809. PMID: 11692108.
Article47. Mould AW, Ramsay AJ, Matthaei KI, Young IG, Rothenberg ME, Foster PS. The effect of IL-5 and eotaxin expression in the lung on eosinophil trafficking and degranulation and the induction of bronchial hyperreactivity. J Immunol. 2000; 164:2142–2150. PMID: 10657668.
Article48. Wang Z, Zheng T, Zhu Z, Homer RJ, Riese RJ, Chapman HA Jr, Shapiro SD, Elias JA. Interferon gamma induction of pulmonary emphysema in the adult murine lung. J Exp Med. 2000; 192:1587–1600. PMID: 11104801.49. Lee BJ, Moon HG, Shin TS, Jeon SG, Lee EY, Gho YS, Lee CG, Zhu Z, Elias JA, Kim YK. Protective effects of basic fibroblast growth factor in the development of emphysema induced by interferon-gamma. Exp Mol Med. 2011; 43:169–178. PMID: 21297377.50. Lee CG, Homer RJ, Zhu Z, Lanone S, Wang X, Koteliansky V, Shipley JM, Gotwals P, Noble P, Chen Q, Senior RM, Elias JA. Interleukin-13 induces tissue fibrosis by selectively stimulating and activating transforming growth factor beta(1). J Exp Med. 2001; 194:809–821. PMID: 11560996.51. Olenchock SA, May JJ, Pratt DS, Morey PR. Occupational exposures to airborne endotoxins in agriculture. Prog Clin Biol Res. 1987; 231:475–487. PMID: 3588637.52. Michel O, Ginanni R, Duchateau J, Vertongen F, Le Bon B, Sergysels R. Domestic endotoxin exposure and clinical severity of asthma. Clin Exp Allergy. 1991; 21:441–448. PMID: 1913267.
Article53. Lipworth BJ, Jackson CM. Safety of inhaled and intranasal corticosteroids: lessons for the new millennium. Drug Saf. 2000; 23:11–33. PMID: 10915030.54. Holt PG. Parasites, atopy, and the hygiene hypothesis: resolution of a paradox? Lancet. 2000; 356:1699–1701. PMID: 11095252.
Article55. Voelker R. The hygiene hypothesis. JAMA. 2000; 283:1282.
Article56. Looringh van Beeck FA, Hoekstra H, Brunekreef B, Willemse T. Inverse association between endotoxin exposure and canine atopic dermatitis. Vet J. 2011; 190:215–219. PMID: 21130010.
Article57. Illi S, von Mutius E, Lau S, Bergmann R, Niggemann B, Sommerfeld C, Wahn U. MAS Group. Early childhood infectious diseases and the development of asthma up to school age: a birth cohort study. BMJ. 2001; 322:390–395. PMID: 11179155.
Article58. von Mutius E, Illi S, Hirsch T, Leupold W, Keil U, Weiland SK. Frequency of infections and risk of asthma, atopy and airway hyperresponsiveness in children. Eur Respir J. 1999; 14:4–11. PMID: 10489821.
Article59. Simpson JL, Grissell TV, Douwes J, Scott RJ, Boyle MJ, Gibson PG. Innate immune activation in neutrophilic asthma and bronchiectasis. Thorax. 2007; 62:211–218. PMID: 16844729.
Article60. Hnizdo E. Lung function loss associated with occupational dust exposure in metal smelting. Am J Respir Crit Care Med. 2010; 181:1162–1163. PMID: 20535848.
Article61. Park JH, Gold DR, Spiegelman DL, Burge HA, Milton DK. House dust endotoxin and wheeze in the first year of life. Am J Respir Crit Care Med. 2001; 163:322–328. PMID: 11179100.
Article62. Dosman JA, Fukushima Y, Senthilselvan A, Kirychuk SP, Lawson JA, Pahwa P, Cormier Y, Hurst T, Barber EM, Rhodes CS. Respiratory response to endotoxin and dust predicts evidence of inflammatory response in volunteers in a swine barn. Am J Ind Med. 2006; 49:761–766. PMID: 16917830.
Article63. Eisenbarth SC, Piggott DA, Huleatt JW, Visintin I, Herrick CA, Bottomly K. Lipopolysaccharide-enhanced, toll-like receptor 4-dependent T helper cell type 2 responses to inhaled antigen. J Exp Med. 2002; 196:1645–1651. PMID: 12486107.
Article64. Gereda JE, Leung DY, Thatayatikom A, Streib JE, Price MR, Klinnert MD, Liu AH. Relation between house-dust endotoxin exposure, type 1 T-cell development, and allergen sensitisation in infants at high risk of asthma. Lancet. 2000; 355:1680–1683. PMID: 10905243.
Article65. Akbari O, Freeman GJ, Meyer EH, Greenfield EA, Chang TT, Sharpe AH, Berry G, DeKruyff RH, Umetsu DT. Antigen-specific regulatory T cells develop via the ICOS-ICOS-ligand pathway and inhibit allergen-induced airway hyperreactivity. Nat Med. 2002; 8:1024–1032. PMID: 12145647.
Article66. Kaplan MH, Schindler U, Smiley ST, Grusby MJ. Stat6 is required for mediating responses to IL-4 and for development of Th2 cells. Immunity. 1996; 4:313–319. PMID: 8624821.67. Zhu J, Guo L, Watson CJ, Hu-Li J, Paul WE. Stat6 is necessary and sufficient for IL-4's role in Th2 differentiation and cell expansion. J Immunol. 2001; 166:7276–7281. PMID: 11390477.
Article68. Neurath MF, Finotto S, Glimcher LH. The role of Th1/Th2 polarization in mucosal immunity. Nat Med. 2002; 8:567–573. PMID: 12042806.
Article69. Wills-Karp M. Immunologic basis of antigen-induced airway hyperresponsiveness. Annu Rev Immunol. 1999; 17:255–281. PMID: 10358759.
Article70. Gavett SH, O'Hearn DJ, Li X, Huang SK, Finkelman FD, Wills-Karp M. Interleukin 12 inhibits antigen-induced airway hyperresponsiveness, inflammation, and Th2 cytokine expression in mice. J Exp Med. 1995; 182:1527–1536. PMID: 7595222.
Article71. Szabo SJ, Sullivan BM, Peng SL, Glimcher LH. Molecular mechanisms regulating Th1 immune responses. Annu Rev Immunol. 2003; 21:713–758. PMID: 12500979.
Article72. Zhou L, Ivanov II, Spolski R, Min R, Shenderov K, Egawa T, Levy DE, Leonard WJ, Littman DR. IL-6 programs T(H)-17 cell differentiation by promoting sequential engagement of the IL-21 and IL-23 pathways. Nat Immunol. 2007; 8:967–974. PMID: 17581537.
Article73. Senger DR, Van de Water L, Brown LF, Nagy JA, Yeo KT, Yeo TK, Berse B, Jackman RW, Dvorak AM, Dvorak HF. Vascular permeability factor (VPF, VEGF) in tumor biology. Cancer Metastasis Rev. 1993; 12:303–324. PMID: 8281615.
Article74. Lee YC, Lee HK. Vascular endothelial growth factor in patients with acute asthma. J Allergy Clin Immunol. 2001; 107:1106. PMID: 11398093.
Article75. Hoshino M, Takahashi M, Aoike N. Expression of vascular endothelial growth factor, basic fibroblast growth factor, and angiogenin immunoreactivity in asthmatic airways and its relationship to angiogenesis. J Allergy Clin Immunol. 2001; 107:295–301. PMID: 11174196.
Article76. Hahn RG. Endotoxin boosts the vascular endothelial growth factor (VEGF) in rabbits. J Endotoxin Res. 2003; 9:97–100. PMID: 12803882.
Article77. Lee CG, Link H, Baluk P, Homer RJ, Chapoval S, Bhandari V, Kang MJ, Cohn L, Kim YK, McDonald DM, Elias JA. Vascular endothelial growth factor (VEGF) induces remodeling and enhances TH2-mediated sensitization and inflammation in the lung. Nat Med. 2004; 10:1095–1103. PMID: 15378055.
Article78. Kim YS, Choi SJ, Tae YM, Lee BJ, Jeon SG, Oh SY, Gho YS, Zhu Z, Kim YK. Distinct roles of vascular endothelial growth factor receptor-1- and receptor-2-mediated signaling in T cell priming and Th17 polarization to lipopolysaccharide-containing allergens in the lung. J Immunol. 2010; 185:5648–5655. PMID: 20921519.
Article79. Thorne PS, Kulhánková K, Yin M, Cohn R, Arbes SJ Jr, Zeldin DC. Endotoxin exposure is a risk factor for asthma: the national survey of endotoxin in United States housing. Am J Respir Crit Care Med. 2005; 172:1371–1377. PMID: 16141442.80. Cho SH, Park HW, Rosenberg DM. The current status of asthma in Korea. J Korean Med Sci. 2006; 21:181–187. PMID: 16614498.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- CpG DNA for Treatment of Allergic Diseases
- Stem cell therapy in animal models of allergic airway diseases
- Prostaglandin D2 and TH2 Inflammation in the Pathogenesis of Bronchial Asthma
- Mechanism of Allergic Asthma Pathogenesis by Protease Allergen
- Allergic rhinitis, sinusitis and asthma: evidence for respiratory system integration