J Korean Diabetes.
2016 Jun;17(2):139-145. 10.4093/jkd.2016.17.2.139.
Emphysematous Gastritis with Concomitant Portal Venous Air and Acute Necrotizing Esophagitis in Type 1 Diabetes with Diabetic Ketoacidosis: A Case Report and Literature Review of a Rare Complication in Diabetes
- Affiliations
-
- 1Division of Endocrinology, Department of Internal Medicine, Hanyang University Medical Center, Hanyang University College of Medicine, Seoul, Korea. ahnyh@hanyang.ac.kr
- 2Division of Endocrinology, Department of Internal Medicine, Hanyang University Guri Hospital, Hanyang University College of Medicine, Guri, Korea.
- 3Division of Gastroenterology, Department of Internal Medicine, Hanyang University Medical Center, Hanyang University College of Medicine, Seoul, Korea.
- 4Department of Thoracic and Cardiovascular Surgery, Hanyang University Medical Center, Hanyang University College of Medicine, Seoul, Korea.
- KMID: 2328580
- DOI: http://doi.org/10.4093/jkd.2016.17.2.139
Abstract
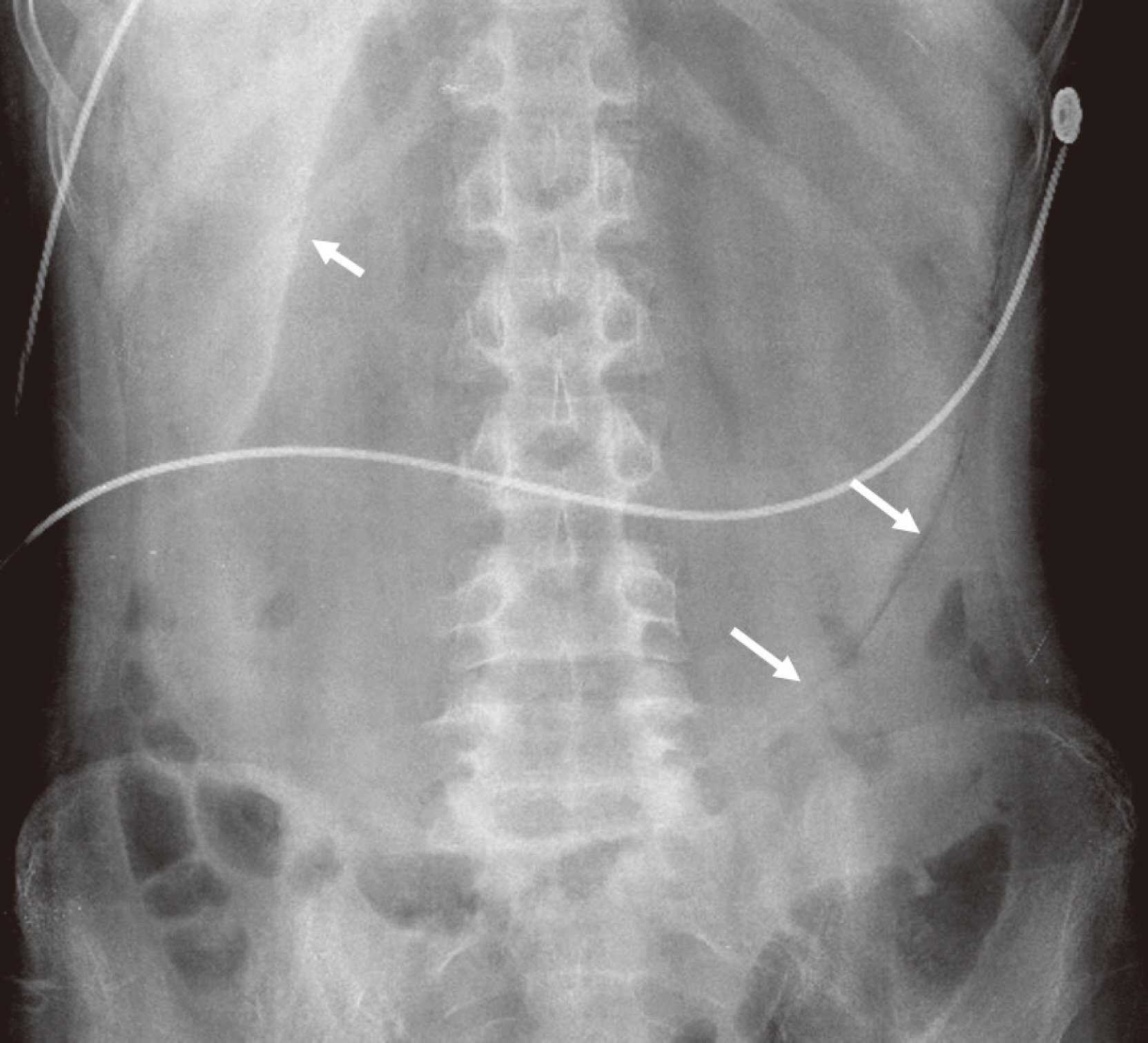
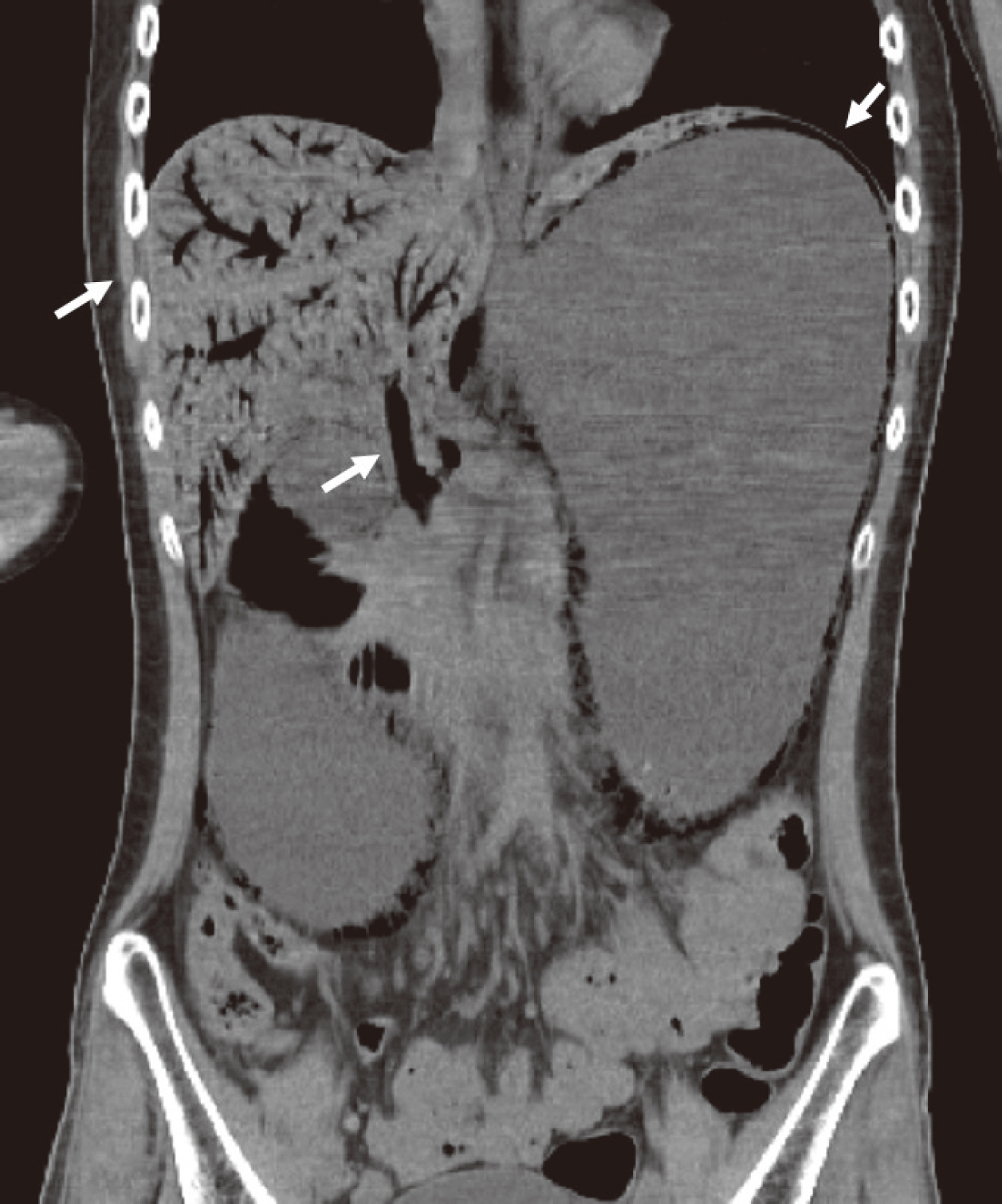
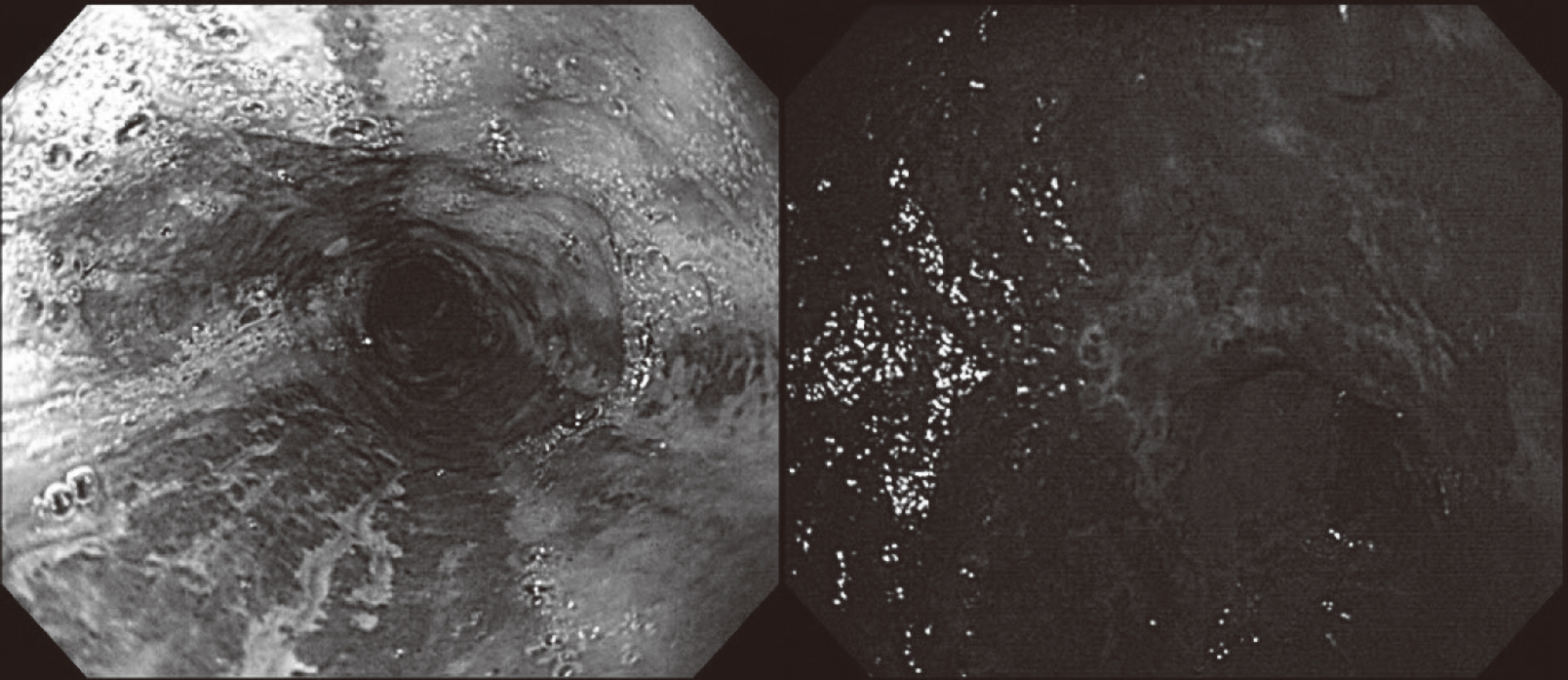
- Emphysematous gastritis is a rare disorder characterized by emphysematous change of the gastric wall due to infection with a gas-forming organism. Acute necrotizing esophagitis is a rare disorder with an unknown pathogenesis. Above two disorders rarely occur together, only three global cases have been reported to date. Such a case has never been reported in Korea, we report a novel case of severe emphysematous gastritis with concomitant portal venous air and acute necrotizing esophagitis in type 1 diabetes presenting with diabetic ketoacidosis. A 24-year-old man known to have type 1 diabetes and pulmonary tuberculosis was brought to the emergency room for epigastric pain with vomiting. His body mass index was 14.7, and the laboratory findings demonstrated leukocytosis and acidosis, as well as elevated serum glucose, ketone, and C-reactive protein levels. Enhanced computed tomography showed portal vein gas and edematous wall thickening without enhancement in the stomach wall, with air density along the stomach and esophageal wall. The patient required surgical intervention of total gastrectomy and cervical esophagostomy followed by esophagocolostomy and esophageal reconstruction. Early radiologic diagnosis and clinical suspicion of this disease and prompt intervention including antibiotics, decompression, and surgery are important for a good prognosis.
MeSH Terms
-
Acidosis
Anti-Bacterial Agents
Blood Glucose
Body Mass Index
C-Reactive Protein
Decompression
Diabetic Ketoacidosis*
Diagnosis
Emergency Service, Hospital
Esophagitis*
Esophagostomy
Gastrectomy
Gastritis*
Humans
Korea
Leukocytosis
Portal Vein
Prognosis
Stomach
Tuberculosis, Pulmonary
Vomiting
Young Adult
Anti-Bacterial Agents
C-Reactive Protein
Figure
Reference
-
References
1. Moosvi A, Saravolatz LD, Wong DH, Simms SM. Emphysematous gastritis: case report and review. Rev Infect Dis. 1990; 12:848–55.
Article2. van Mook WN, van der Geest S, Goessens ML, Schoon EJ, Ramsay G. Gas within the wall of the stomach due to emphysematous gastritis: case report and review. Eur J Gastroenterol Hepatol. 2002; 14:1155–60.
Article3. Day A, Sayegh M. Acute oesophageal necrosis: a case report and review of the literature. Int J Surg. 2010; 8:6–14.
Article4. McKelvie P, Fink MA. A fatal case of emphysematous gastritis and esophagitis. Pathology. 1994; 26:490–2.
Article5. Miller C, Florman S, Kim-Schluger L, Lento P, De La Garza J, Wu J, Xie B, Zhang W, Bottone E, Zhang D, Schwartz M. Fulminant and fatal gas gangrene of the stomach in a healthy live liver donor. Liver Transpl. 2004; 10:1315–9.
Article6. Agarwal N, Kumar S, Sharma MS, Agrawal R, Joshi M. Emphysematous gastritis causing gastric and esophageal necrosis in a young boy. Acta Gastroenterol Belg. 2009; 72:354–6.7. Lee SM, Kim GH, Kang DH, Kim TO, Song GA, Kim S. Education and imaging. Gastrointestinal: emphysematous gastritis. J Gastroenterol Hepatol. 2007; 22:2036.8. Park JP, Bae SS, Baek IY, Kim HS, Kim BS, Seo HE, Son KR, Kwon SH. A Case of acute emphysematous gastritis associated with invasive aspergillosis. Korean J Helicobacter Up Gastrointest Res. 2013; 13:50–4.
Article9. Kim GY, Ward J, Henessey B, Peji J, Godell C, Desta H, Arlin S, Tzagournis J, Thomas F. Phlegmonous gastritis: case report and review. Gastrointest Endosc. 2005; 61:168–74.
Article10. Schatz TP, Nassif MO, Farma JM. Extensive portal venous gas: unlikely etiology and outcome. Int J Surg Case Rep. 2015; 8:134–6.
Article11. Sahoo MR, Kumar AT, Jaiswal S, Bhujabal SN. Acute dilatation, ischemia, and necrosis of stomach without perforation. Case Rep Surg. 2013; 2013:984594.
Article12. Turan M, Sen M, Canbay E, Karadayi K, Yildiz E. Gastric necrosis and perforation caused by acute gastric dilatation: report of a case. Surg Today. 2003; 33:302–4.13. Franken EA Jr, Fox M, Smith JA, Smith WL. Acute gastric dilatation in neglected children. AJR Am J Roentgenol. 1978; 130:297–9.
Article14. Wayne E, Ough M, Wu A, Liao J, Andresen KJ, Kuehn D, Wilkinson N. Management algorithm for pneumatosis intestinalis and portal venous gas: treatment and outcome of 88 consecutive cases. J Gastrointest Surg. 2010; 14:437–48.
Article15. Gurvits GE, Shapsis A, Lau N, Gualtieri N, Robilotti JG. Acute esophageal necrosis: a rare syndrome. J Gastroenterol. 2007; 42:29–38.
Article16. Moretó M, Ojembarrena E, Zaballa M, Tánago JG, Ibánez S. Idiopathic acute esophageal necrosis: not necessarily a terminal event. Endoscopy. 1993; 25:534–8.
Article17. Ben Soussan E, Savoye G, Hochain P, Hervé S, Antonietti M, Lemoine F, Ducrotté P. Acute esophageal necrosis: a 1-year prospective study. Gastrointest Endosc. 2002; 56:213–7.18. Augusto F, Fernandes V, Cremers MI, Oliveira AP, Lobato C, Alves AL, Pinho C, de Freitas J. Acute necrotizing esophagitis: a large retrospective case series. Endoscopy. 2004; 36:411–5.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Emphysematous Gastritis with Concomitant Portal Venous Air
- Diabetic Ketoacidosis Associated with Emphysematous Gastritis: A Case Report
- A Case of Severe Diabetic Ketoacidosis in a Child with Type 2 Diabetes
- Postmortem Diagnosis of Diabetic Ketoacidosis: An Autopsy Case
- A Case of Ketosis-Prone Type 2 Diabetes Mellitus