Clin Orthop Surg.
2020 Mar;12(1):37-42. 10.4055/cios.2020.12.1.37.
Lupus and Perioperative Complications in Elective Primary Total Hip or Knee Arthroplasty
- Affiliations
-
- 1Department of Orthopaedic Surgery, The Johns Hopkins Hospital, Baltimore, MD, USA. hkhanuj1@jhmi.edu
- KMID: 2470048
- DOI: http://doi.org/10.4055/cios.2020.12.1.37
Abstract
- BACKGROUND
The number of patients with systemic lupus erythematosus (herein, lupus) undergoing total hip arthroplasty (THA) or total knee arthroplasty (TKA) is increasing. There is disagreement about the effect of lupus on perioperative complication rates. We hypothesized that lupus would be associated with higher complication rates in patients who undergo elective primary THA or TKA.
METHODS
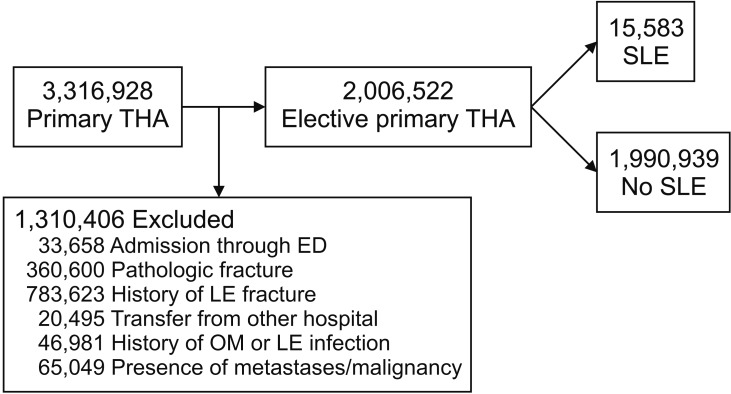
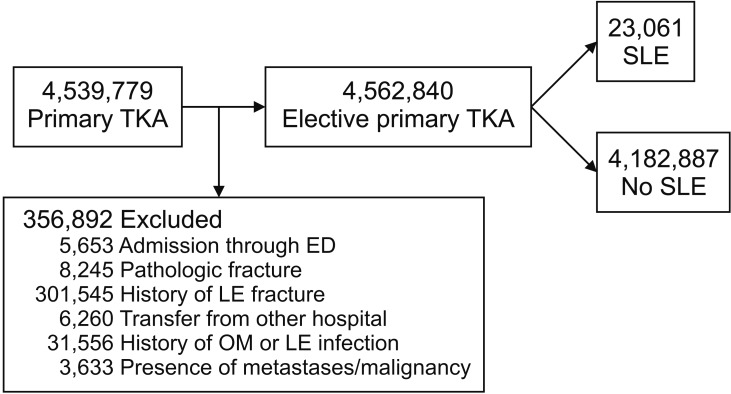
Records of more than 6.2 million patients from the National Inpatient Sample who underwent elective primary THA or TKA from 2000 to 2009 were reviewed. Patients with lupus (n = 38,644) were compared with those without lupus (n = 6,173,826). Major complications were death, pulmonary embolism, myocardial infarction, stroke, pneumonia, and acute renal failure. Minor complications were wound infection, seroma, deep vein thrombosis, hip dislocation, wound dehiscence, and hematoma. Patient age, sex, duration of hospital stay, and number of Elixhauser comorbidities were assessed for both groups. Multivariate logistic regression models using comorbidities, age, and sex as covariates were used to assess the association of lupus with major and minor perioperative complications. The alpha level was set to 0.001.
RESULTS
Among patients who underwent THA, those with lupus were younger (mean age, 56 vs. 65 years), were more likely to be women (87% vs. 56%), had longer hospital stays (mean, 4.0 vs. 3.8 days), and had more comorbidities (mean, 2.5 vs. 1.4) than those without lupus (all p < 0.001). In patients with THA, lupus was independently associated with major complications (odds ratio [OR], 1.4; 95% confidence interval [CI], 1.1 to 1.7) and minor complications (OR, 1.2; 95% CI, 1.0 to 1.5). Similarly, among patients who underwent TKA, those with lupus were younger (mean, 62 vs. 67 years), were more likely to be women (93% vs. 64%), had longer hospital stays (mean, 3.8 vs. 3.7 days), and had more comorbidities (mean, 2.8 vs. 1.7) than those without lupus (all p < 0.001). However, in TKA patients, lupus was not associated with greater odds of major complications (OR, 1.2; 95% CI, 0.9 to 1.4) or minor complications (OR, 1.1; 95% CI, 0.9 to 1.3).
CONCLUSIONS
Lupus is an independent risk factor for major and minor perioperative complications in elective primary THA but not TKA.
Keyword
MeSH Terms
-
Acute Kidney Injury
Arthroplasty, Replacement, Hip
Arthroplasty, Replacement, Knee*
Comorbidity
Female
Hematoma
Hip Dislocation
Hip*
Humans
Inpatients
Knee*
Length of Stay
Logistic Models
Lupus Erythematosus, Systemic
Myocardial Infarction
Pneumonia
Pulmonary Embolism
Risk Factors
Seroma
Stroke
Venous Thrombosis
Wound Infection
Wounds and Injuries
Figure
Reference
-
1. Borchers AT, Naguwa SM, Shoenfeld Y, Gershwin ME. The geoepidemiology of systemic lupus erythematosus. Autoimmun Rev. 2010; 9(5):A277–A287. PMID: 20036343.
Article2. Kamen DL. Environmental influences on systemic lupus erythematosus expression. Rheum Dis Clin North Am. 2014; 40(3):401–412. PMID: 25034153.
Article3. Esdaile JM, Danoff D, Rosenthall L, Gutkowski A. Deforming arthritis in systemic lupus erythematosus. Ann Rheum Dis. 1981; 40(2):124–126. PMID: 7224685.
Article4. Issa K, Pierce TP, Scillia AJ, Festa A, Harwin SF, Mont MA. Midterm outcomes following total knee arthroplasty in lupus patients. J Arthroplasty. 2016; 31(3):655–657. PMID: 26601634.
Article5. Mourao AF, Amaral M, Caetano-Lopes J, Isenberg D. An analysis of joint replacement in patients with systemic lupus erythematosus. Lupus. 2009; 18(14):1298–1302. PMID: 19850657.
Article6. Stratta P, Marcuccio C, Campo A, et al. Improvement in relative survival of patients with vasculitis: study of 101 cases compared to the general population. Int J Immunopathol Pharmacol. 2008; 21(3):631–642. PMID: 18831931.
Article7. Stratta P, Mesiano P, Campo A, et al. Life expectancy of women with lupus nephritis now approaches that of the general population. Int J Immunopathol Pharmacol. 2009; 22(4):1135–1141. PMID: 20074480.
Article8. Mont MA, Glueck CJ, Pacheco IH, Wang P, Hungerford DS, Petri M. Risk factors for osteonecrosis in systemic lupus erythematosus. J Rheumatol. 1997; 24(4):654–662. PMID: 9101497.9. Mok MY, Farewell VT, Isenberg DA. Risk factors for avascular necrosis of bone in patients with systemic lupus erythematosus: is there a role for antiphospholipid antibodies? Ann Rheum Dis. 2000; 59(6):462–467. PMID: 10834864.
Article10. Apostolopoulos D, Morand EF. It hasn't gone away: the problem of glucocorticoid use in lupus remains. Rheumatology (Oxford). 2017; 56(suppl_1):i114–i122. PMID: 28013208.
Article11. Di Franco M, Bazzichi L, Casale R, Sarzi-Puttini P, Atzeni F. Pain in systemic connective tissue diseases. Best Pract Res Clin Rheumatol. 2015; 29(1):53–62. PMID: 26266999.
Article12. Mertelsmann-Voss C, Lyman S, Pan TJ, Goodman SM, Figgie MP, Mandl LA. US trends in rates of arthroplasty for inflammatory arthritis including rheumatoid arthritis, juvenile idiopathic arthritis, and spondyloarthritis. Arthritis Rheumatol. 2014; 66(6):1432–1439. PMID: 24591462.
Article13. Bernatsky S, Boivin JF, Joseph L, et al. Mortality in systemic lupus erythematosus. Arthritis Rheum. 2006; 54(8):2550–2557. PMID: 16868977.
Article14. Trager J, Ward MM. Mortality and causes of death in systemic lupus erythematosus. Curr Opin Rheumatol. 2001; 13(5):345–351. PMID: 11604587.
Article15. Meacock R, Dale N, Harrison MJ. The humanistic and economic burden of systemic lupus erythematosus: a systematic review. Pharmacoeconomics. 2013; 31(1):49–61. PMID: 23329592.16. Roberts JE, Mandl LA, Su EP, et al. Patients with systemic lupus erythematosus have increased risk of short-term adverse events after total hip arthroplasty. J Rheumatol. 2016; 43(8):1498–1502. PMID: 27307529.
Article17. Centers for Disease control and Prevention. ICD-9-CM: International Classification of Diseases, ninth revision, clinical modification. Washington, DC: Department of Health and Human Services;2011.18. Quan H, Sundararajan V, Halfon P, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005; 43(11):1130–1139. PMID: 16224307.
Article19. Mertelsmann-Voss C, Lyman S, Pan TJ, Goodman S, Figgie MP, Mandl LA. Arthroplasty rates are increased among US patients with systemic lupus erythematosus: 1991-2005. J Rheumatol. 2014; 41(5):867–874. PMID: 24692528.
Article20. Abu-Shakra M, Buskila D, Shoenfeld Y. Osteonecrosis in patients with SLE. Clin Rev Allergy Immunol. 2003; 25(1):13–24. PMID: 12794257.
Article21. Shah UH, Mandl LA, Mertelsmann-Voss C, et al. Systemic lupus erythematosus is not a risk factor for poor outcomes after total hip and total knee arthroplasty. Lupus. 2015; 24(9):900–908. PMID: 25595621.
Article22. Ponnusamy KE, Kim TJ, Khanuja HS. Perioperative blood transfusions in orthopaedic surgery. J Bone Joint Surg Am. 2014; 96(21):1836–1844. PMID: 25378512.
Article23. Chen Y, Chen Z, Cui S, Li Z, Yuan Z. Topical versus systemic tranexamic acid after total knee and hip arthroplasty: a meta-analysis of randomized controlled trials. Medicine (Baltimore). 2016; 95(41):e4656. PMID: 27741100.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- The Association of Delirium with Perioperative Complications in Primary Elective Total Hip Arthroplasty
- Total Hip Replacement Arthroplasty in Patient with Idiopathic Thrombocytopenic Purpura: Clinical Experience of Perioperative Management
- Patient Blood Management in Hip Replacement Arthroplasty
- Geometric Total Knee Arthroplasty: A Case Report
- Total Hip Arthroplasty for Ankylosed Hip