Ann Hepatobiliary Pancreat Surg.
2019 Nov;23(4):377-384. 10.14701/ahbps.2019.23.4.377.
Extremely high white blood cell counts on postoperative day 1 do not predict severe complications following distal pancreatectomy
- Affiliations
-
- 1Department of Surgery, Yonsei University College of Medicine, Seoul, Korea. cmkang@yuhs.ac
- 2Division of Hepatobiliary and Pancreatic Surgery, Department of Surgery, Yonsei University College of Medicine, Seoul, Korea.
- 3Pancreatobiliary Cancer Clinic, Yonsei Cancer Center, Severance Hospital, Seoul, Korea.
- KMID: 2464328
- DOI: http://doi.org/10.14701/ahbps.2019.23.4.377
Abstract
- BACKGROUNDS/AIMS
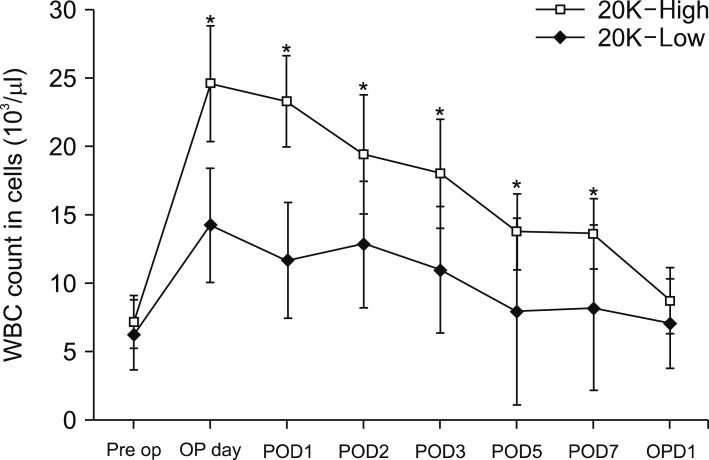
Distal pancreatectomy(DP) is associated with high morbidity. In clinical practice, postoperative white blood cell(WBC) counts are useful indicators of infection complications. The aim of this study was to determine the relevance of extremely high postoperative day (POD)1 WBC counts after DP and their relationship to perioperative outcomes.
METHODS
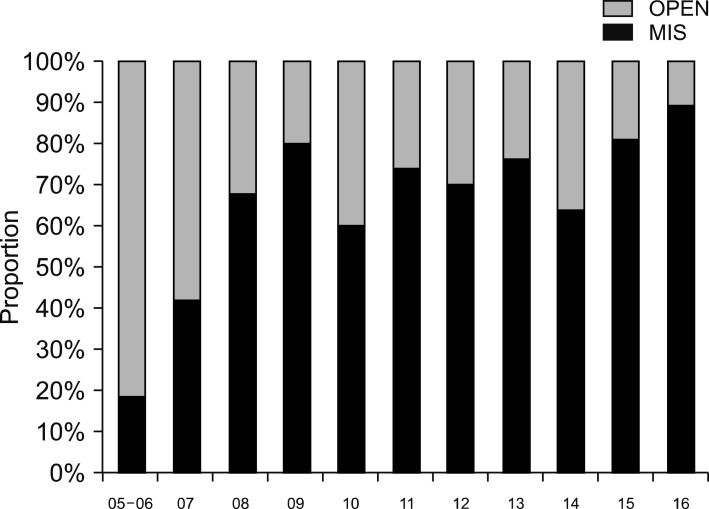
From December 2005 to December 2016, data from patients who had open or minimally invasive DP surgery (robot or laparoscopy, MIS) for benign or borderline malignant tumors were retrospectively reviewed. Patients were divided into groups based on POD1 WBC count (>20K, High and <20K, Low) for comparisons.
RESULTS
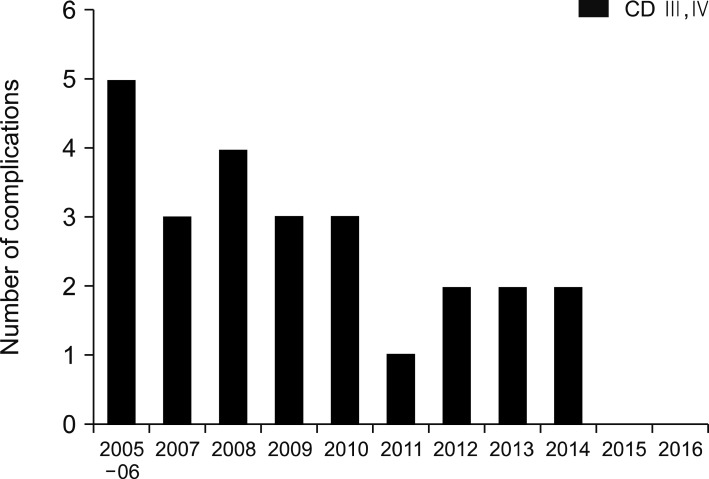
Twelve patients (4.6%) were categorized into the High group. There were significant differences in age (p=0.019), BMI (p=0.010), and spleen-preserving rate (p=0.002) between the High and Low groups. In binary logistic regression analysis, the risk factors for severe complication was age (p=0.032) and open DP (p=0.005), not POD1 WBC count.
CONCLUSIONS
Extremely high WBC count after POD1 after DP was not associated with severe complications, but was associated with splenectomy. Surgical methods and age were associated with severe complications.
Keyword
MeSH Terms
Figure
Reference
-
1. Lillemoe KD, Kaushal S, Cameron JL, Sohn TA, Pitt HA, Yeo CJ. Distal pancreatectomy: indications and outcomes in 235 patients. Ann Surg. 1999; 229:693–698. discussion 698-700. PMID: 10235528.
Article2. Kneuertz PJ, Patel SH, Chu CK, Fisher SB, Maithel SK, Sarmiento JM, et al. Laparoscopic distal pancreatectomy: trends and lessons learned through an 11-year experience. J Am Coll Surg. 2012; 215:167–176. PMID: 22632910.
Article3. Stauffer JA, Coppola A, Mody K, Asbun HJ. Laparoscopic versus open distal pancreatectomy for pancreatic adenocarcinoma. World J Surg. 2016; 40:1477–1484. PMID: 26847665.
Article4. Fahy BN, Frey CF, Ho HS, Beckett L, Bold RJ. Morbidity, mortality, and technical factors of distal pancreatectomy. Am J Surg. 2002; 183:237–241. PMID: 11943118.
Article5. Kelly KJ, Greenblatt DY, Wan Y, Rettammel RJ, Winslow E, Cho CS, et al. Risk stratification for distal pancreatectomy utilizing ACS-NSQIP: preoperative factors predict morbidity and mortality. J Gastrointest Surg. 2011; 15:250–259. discussion 259-261. PMID: 21161427.
Article6. Fox AM, Pitzul K, Bhojani F, Kaplan M, Moulton CA, Wei AC, et al. Comparison of outcomes and costs between laparoscopic distal pancreatectomy and open resection at a single center. Surg Endosc. 2012; 26:1220–1230. PMID: 22179451.
Article7. Nakamura M, Wakabayashi G, Miyasaka Y, Tanaka M, Morikawa T, Unno M, et al. Study Group of JHBPS. JSEPS. Multicenter comparative study of laparoscopic and open distal pancreatectomy using propensity score-matching. J Hepatobiliary Pancreat Sci. 2015; 22:731–736. PMID: 26087943.
Article8. Haga Y, Beppu T, Doi K, Nozawa F, Mugita N, Ikei S, et al. Systemic inflammatory response syndrome and organ dysfunction following gastrointestinal surgery. Crit Care Med. 1997; 25:1994–2000. PMID: 9403749.
Article9. Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004; 240:205–213. PMID: 15273542.10. Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, et al. International Study Group on Pancreatic Fistula Definition. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery. 2005; 138:8–13. PMID: 16003309.
Article11. Sugimoto M, Gotohda N, Kato Y, Takahashi S, Kinoshita T, Shibasaki H, et al. Risk factor analysis and prevention of postoperative pancreatic fistula after distal pancreatectomy with stapler use. J Hepatobiliary Pancreat Sci. 2013; 20:538–544. PMID: 23430057.
Article12. Lillemoe KD, Cameron JL, Kim MP, Campbell KA, Sauter PK, Coleman JA, et al. Does fibrin glue sealant decrease the rate of pancreatic fistula after pancreaticoduodenectomy? Results of a prospective randomized trial. J Gastrointest Surg. 2004; 8:766–772. discussion 772-774. PMID: 15531229.
Article13. Parikh P, Shiloach M, Cohen ME, Bilimoria KY, Ko CY, Hall BL, et al. Pancreatectomy risk calculator: an ACS-NSQIP resource. HPB (Oxford). 2010; 12:488–497. PMID: 20815858.
Article14. Da Silva M, Cleghorn MC, Elnahas A, Jackson TD, Okrainec A, Quereshy FA. Postoperative day one neutrophil-to-lymphocyte ratio as a predictor of 30-day outcomes in bariatric surgery patients. Surg Endosc. 2017; 31:2645–2650. PMID: 27743125.
Article15. Giaccaglia V, Salvi PF, Cunsolo GV, Sparagna A, Antonelli MS, Nigri G, et al. Procalcitonin, as an early biomarker of colorectal anastomotic leak, facilitates enhanced recovery after surgery. J Crit Care. 2014; 29:528–532. PMID: 24798346.
Article16. Kumar S, Mehta Y, Vats M, Chand R, Kapoor P, Trehan N. An observational study to know the association of leukocytosis and fever with infection in post cardiac surgery patients. Indian Heart J. 2007; 59:316–322. PMID: 19126936.17. Raymond DP, Crabtree TD, Pelletier SJ, Gleason TG, Banas LE, Patel S, et al. Extremes of white blood cell count do not independently predict outcome among surgical patients with infection. Am Surg. 2000; 66:1124–1130. discussion 1130-1131. PMID: 11149583.18. Velanovich V. Case-control comparison of laparoscopic versus open distal pancreatectomy. J Gastrointest Surg. 2006; 10:95–98. PMID: 16368497.
Article19. Nigri GR, Rosman AS, Petrucciani N, Fancellu A, Pisano M, Zorcolo L, et al. Metaanalysis of trials comparing minimally invasive and open distal pancreatectomies. Surg Endosc. 2011; 25:1642–1651. PMID: 21184115.
Article20. Venkat R, Edil BH, Schulick RD, Lidor AO, Makary MA, Wolfgang CL. Laparoscopic distal pancreatectomy is associated with significantly less overall morbidity compared to the open technique: a systematic review and meta-analysis. Ann Surg. 2012; 255:1048–1059. PMID: 22511003.21. Mehrabi A, Hafezi M, Arvin J, Esmaeilzadeh M, Garoussi C, Emami G, et al. A systematic review and meta-analysis of laparoscopic versus open distal pancreatectomy for benign and malignant lesions of the pancreas: it's time to randomize. Surgery. 2015; 157:45–55. PMID: 25482464.22. Ricci C, Casadei R, Taffurelli G, Toscano F, Pacilio CA, Bogoni S, et al. Laparoscopic versus open distal pancreatectomy for ductal adenocarcinoma: a systematic review and meta-analysis. J Gastrointest Surg. 2015; 19:770–781. PMID: 25560180.
Article23. Cesaretti M, Bifulco L, Costi R, Zarzavadjian Le Bian A. Pancreatic resection in the era of laparoscopy: State of Art. A systematic review. Int J Surg. 2017; 44:309–316. PMID: 28689866.
Article24. de Rooij T, van Hilst J, van Santvoort H, Boerma D, van den Boezem P, Daams F, et al. Dutch Pancreatic Cancer Group. Minimally invasive versus open distal pancreatectomy (LEOPARD): a multicenter patient-blinded randomized controlled trial. Ann Surg. 2019; 269:2–9. PMID: 30080726.25. Tsiouris A, Cogan CM, Velanovich V. Distal pancreatectomy with or without splenectomy: comparison of postoperative outcomes and surrogates of splenic function. HPB (Oxford). 2011; 13:738–744. PMID: 21929675.
Article26. Tezuka K, Kimura W, Hirai I, Moriya T, Watanabe T, Yano M. Postoperative hematological changes after spleen-preserving distal pancreatectomy with preservation of the splenic artery and vein. Dig Surg. 2012; 29:157–164. PMID: 22572950.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Relationship between White Blood Cell Counts and the Metabolic Syndrome
- Role of Distal Pancreatectomy on the Prognosis of Gastric Cancer Patients Undergoing Total Gastrectomy
- Erythrocyte Sedimentation Rate, C-Reactive Protein, and White Blood Cell Count after Lumbar Discectomy
- Current status of robotic surgery for pancreatic tumors
- Utilization of end to side inverted mattress pancreaticojejunostomy for Duval procedure: A case report