J Korean Ophthalmol Soc.
2015 Aug;56(8):1304-1309. 10.3341/jkos.2015.56.8.1304.
A Case of Joubert Syndrome Accompanied with Retinal Abnormality
- Affiliations
-
- 1Department of Ophthalmology, Pusan National University School of Medicine, Busan, Korea. hychoi@pusan.ac.kr
- KMID: 2215088
- DOI: http://doi.org/10.3341/jkos.2015.56.8.1304
Abstract
- PURPOSE
Joubert syndrome is a rare disorder which affects the cerebellum and the brain stem. Herein, we report a case of Joubert syndrome accompanied with retinal abnormality.
CASE SUMMARY
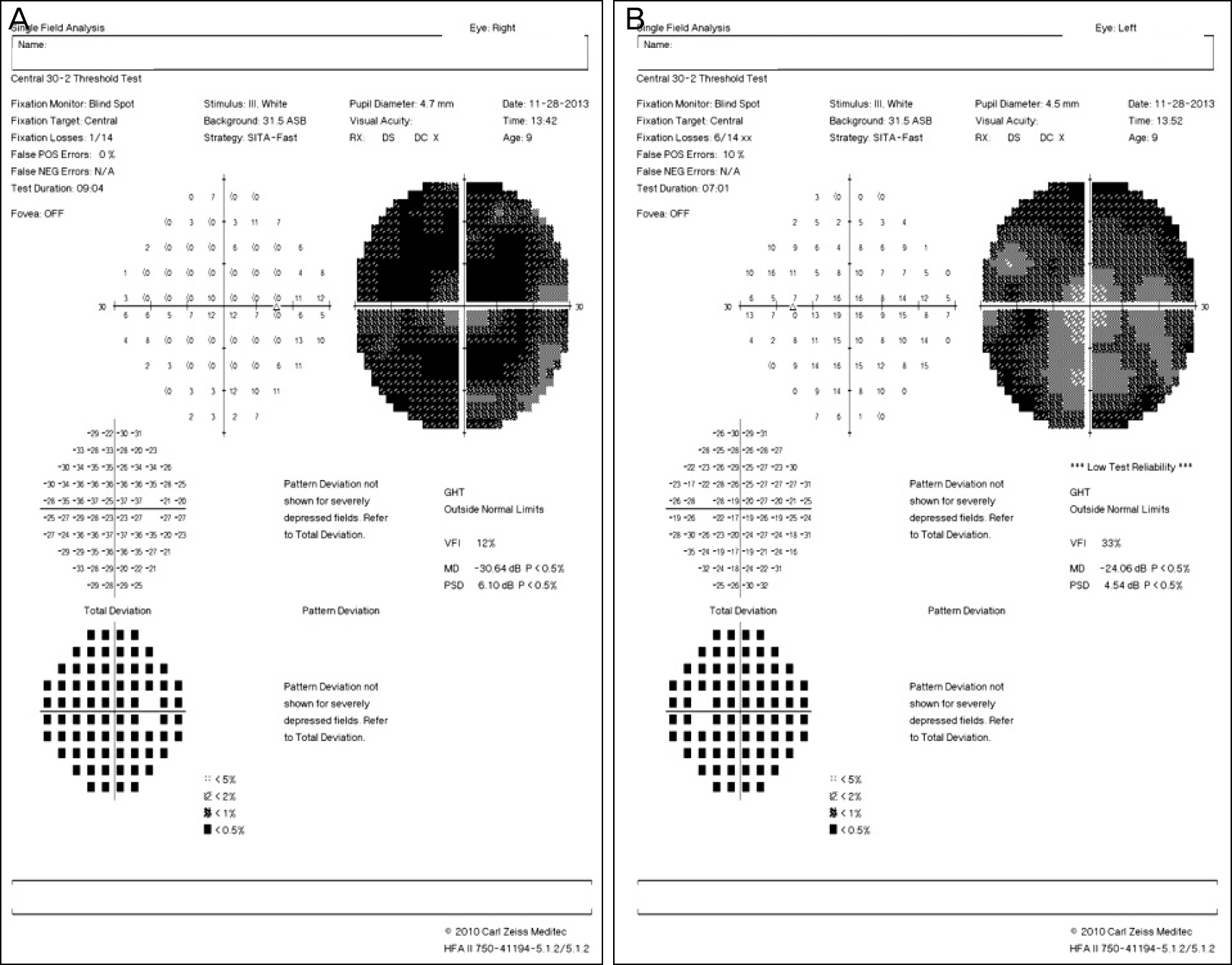
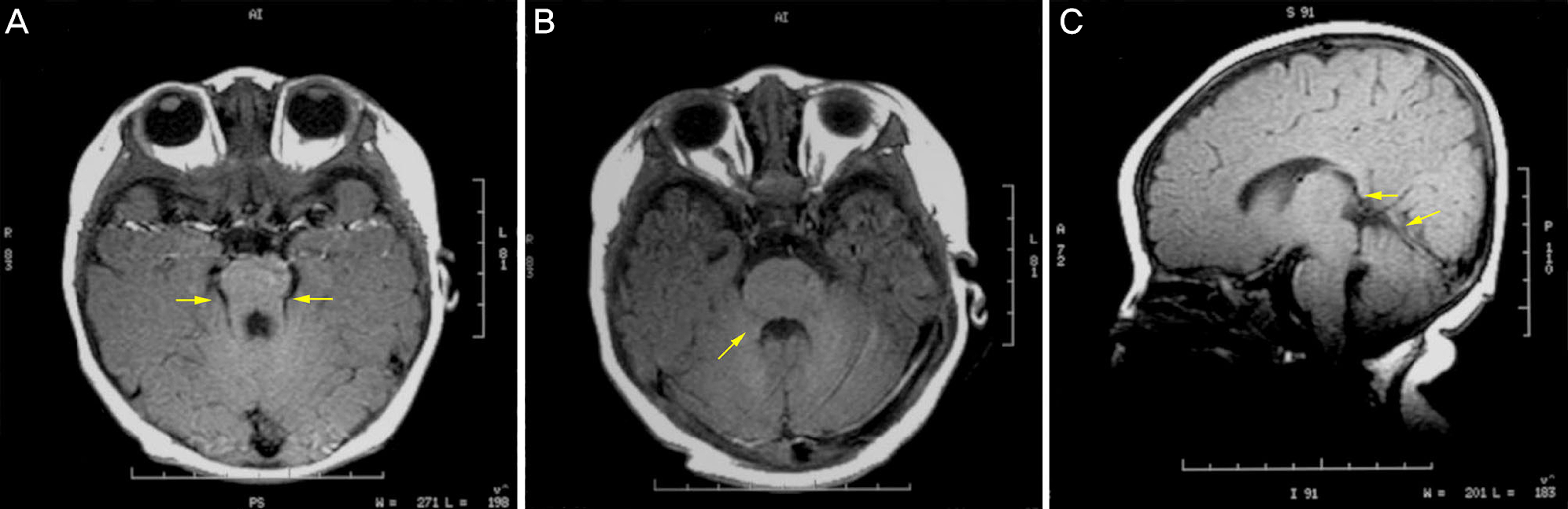
A 9-year-old female visited our hospital with chief complaints of low vision in both eyes, nystagmus, and lack of gaze movement. The best-corrected visual acuity in her right eye was 20/80 and in the left 20/80 and heterotropia was not observed. She appeared to have incomplete total color blindness on the color vision test. The anterior segment test showed no abnormal findings other than diffuse pigmentation and degeneration of the peripheral retina, vascular attenuation, and pale optic disc in both eyes on fundus examination. The patient showed overall developmental delay and decreased muscle tension, but genetic and congenital metabolic disease tests were normal. The molar tooth sign of the midbrain, defect in the lower part of the cerebellum and dilatation of the fourth ventricle were observed on magnetic resonance imaging.
CONCLUSIONS
Appropriate evaluation of retinitis pigmentosa and visual function should be performed in Joubert syndrome patients.
MeSH Terms
Figure
Reference
-
References
1. Joubert M, Eisenring JJ, Robb JP, Andermann F. Familial agenesis of the cerebellar vermis. A syndrome of episodic hyperpnea, abnor-mal eye movements, ataxia, and retardation. Neurology. 1969; 19:813–25.
Article2. Maria BL, Boltshauser E, Palmer SC, Tran TX. Clinical features and revised diagnostic criteria in Joubert syndrome. J Child Neurol. 1999; 14:583–90. discussion 590-1.
Article3. Merritt L. Recognition of the clinical signs and symptoms of Joubert syndrome. Adv Neonatal Care. 2003; 3:178–86. quiz 187-8.
Article4. Boltshauser E, Isler W. Joubert syndrome: episodic hyperpnea, ab-normal eye movements, retardation and ataxia, associated with dysplasia of the cerebellar vermis. Neuropadiatrie. 1977; 8:57–66.
Article5. Yang HK, Yu YS, Hwang JM. Joubert syndrome associated with Leber's congenital amaurosis. J Korean Ophthalmol Soc. 2008; 49:1360–3.
Article6. Lambert SR, Kriss A, Gresty M. . Joubert syndrome. Arch Ophthalmol. 1989; 107:709–13.
Article7. Saraiva JM, Baraitser M. Joubert syndrome: a review. Am J Med Genet. 1992; 43:726–31.
Article8. Maria BL, Hoang KB, Tusa RJ. . "Joubert syndrome" revisited: key ocular motor signs with magnetic resonance imaging correlation. J Child Neurol. 1997; 12:423–30.
Article9. Maria BL, Quisling RG, Rosainz LC. . Molar tooth sign in Joubert syndrome: clinical, radiologic, and pathologic significance. J Child Neurol. 1999; 14:368–76.
Article10. Hodgkins PR, Harris CM, Shawkat FS. . Joubert syndrome: long-term follow-up. Dev Med Child Neurol. 2004; 46:694–9.
Article11. Keskinbora KH. Ocular and oculomotor findings of Joubert syndrome. J Pediatr Ophthalmol Strabismus. 2008; 45:5–6.
Article12. Khan AO, Oystreck DT, Seidahmed MZ. . Ophthalmic features of Joubert syndrome. Ophthalmology. 2008; 115:2286–9.
Article13. Sturm V, Leiba H, Menke MN. . Ophthalmological findings in Joubert syndrome. Eye (Lond). 2010; 24:222–5.
Article14. Romani M, Micalizzi A, Valente EM. Joubert syndrome: con-genital cerebellar ataxia with the molar tooth. Lancet Neurol. 2013; 12:894–905.
Article15. Pellegrino JE, Lensch MW, Muenke M, Chance PF. Clinical and molecular analysis in Joubert syndrome. Am J Med Genet. 1997; 72:59–62.
Article16. Satran D, Pierpont ME, Dobyns WB. Cerebello-oculo-renal syn-dromes including Arima, Senior-Löken and COACH syndromes: more than just variants of Joubert syndrome. Am J Med Genet. 1999; 86:459–69.
Article17. al-Talabani JA, Shubbar AI, Sobkey E. Cranial sonographic find-ings in Joubert's syndrome. J Clin Ultrasound. 1999; 27:41–4.18. Hildebrandt F, Zhou W. Nephronophthisis-associated ciliopathies. J Am Soc Nephrol. 2007; 18:1855–71.
Article19. Berson EL, Rosner B, Sandberg MA, Dryja TP. Ocular findings in patients with autosomal dominant retinitis pigmentosa and a rho-dopsin gene defect (Pro-23-His). Arch Ophthalmol. 1991; 109:92–101.
Article20. Hartong DT, Berson EL, Dryja TP. Retinitis pigmentosa. Lancet. 2006; 368:1795–809.
Article21. Bujakowska K, Maubaret C, Chakarova CF. . Study of gene- targeted mouse models of splicing factor gene Prpf31 implicated in human autosomal dominant retinitis pigmentosa (RP). Invest Ophthalmol Vis Sci. 2009; 50:5927–33.