Korean J Perinatol.
2013 Dec;24(4):310-314. 10.14734/kjp.2013.24.4.310.
A Case of Neonatal Isoimmune Hemolytic Disease due to Anti-Mi(a) Antibody with Massive Fetomaternal Hemorrhage
- Affiliations
-
- 1Department of Pediatrics, Kwangju Christian Hospital, Gwangju, Korea. youjuhee@daum.net
- KMID: 2072309
- DOI: http://doi.org/10.14734/kjp.2013.24.4.310
Abstract
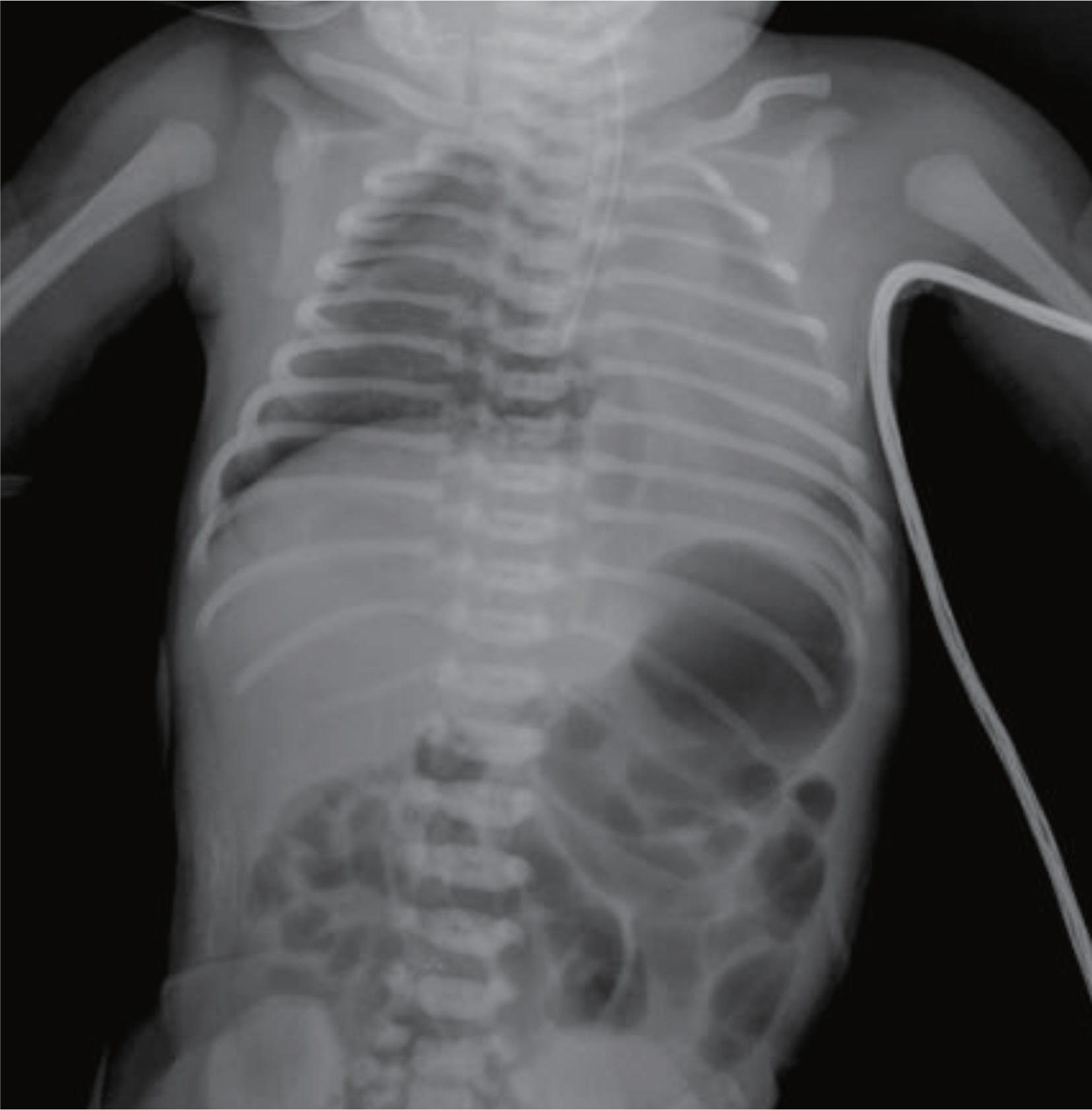
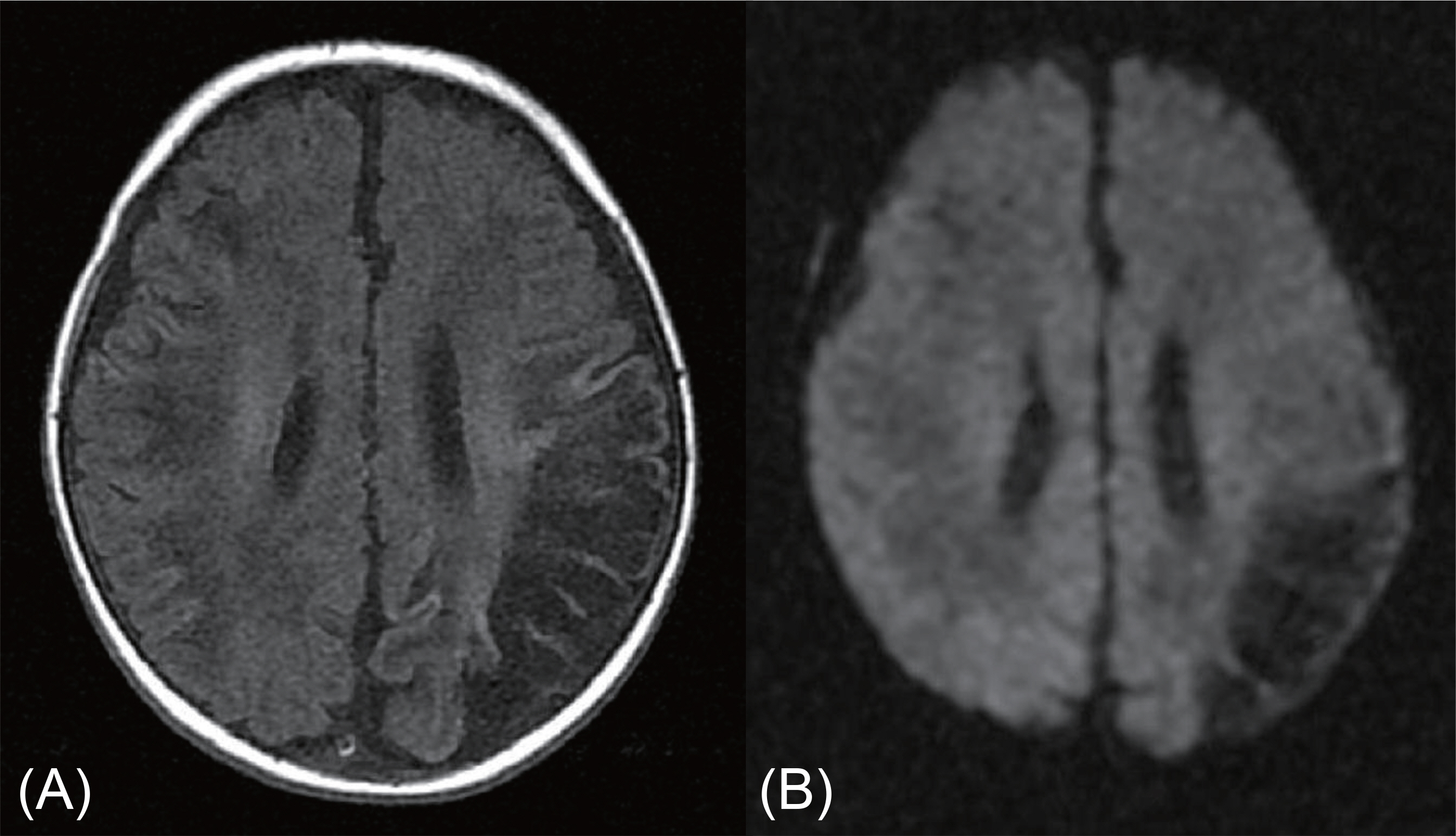
- Authors experienced a newborn treated with severe anemia transferred to our hospital due to pulselessness and apnea shortly after birth. Laboratory analysis of the blood on admission revealed hemoglobin 3.1 g/dL, reticulocyte 11.0%. Kleihauer-Betke test for fetal hemoglobin from maternal blood was seen Hgb F 7%, then we suggested almost 180 ml fetomaternal hemorrhage. But, anemia was not improved despite repeated packed RBC transfusion. So, we evaluated the other cause of intractable anemia. The results were as follows; the Coombs' test was positive. The antibody identification test using mother's serum revealed anti-Mia antibody. The patient improved with supportive treatment, but got hypoxic brain injury due to massive fetomaternal hemorrhage. At day 29, the infant was doing well and was discharged. We report a case of neonatal isoimmune hemolytic disease due to anti-Mia with massive fetomaternal hemorrhage with a brief review of the related literatures.
MeSH Terms
Figure
Reference
-
1). Nathan DG., Orkin SH., Ginsburg D., Look AT. Nathan and Oski's hematology of infancy and childhood. 6th ed.W.B. Saunders Co;2003. p. 56–85.2). Janet MR. Rennie & Robertson's Textbook of neonatology. 5th ed.Churchill Livingstone ELSEVIER;2012. p. 761–3.3). Moncharmont P., Dupraz FJ., Vignal M., Rigal D. Meyer F. Debeaux P. Haemolytic disease of the newborn infant. long term efficiency of the screening and the prevention of alloimmunization in the mother: thirty years of experience. Arch Gynecol Obstet. 1991. 248:175–80.4). Levine P., Katzin EM., Bernham L. Isoimmunization in pregnancy, its possible bearing on the etiology of erythroblastosis fetalis. JAMA. 1941. 116:825–7.5). Kim WB., Yoo KS., Lee DH., Kang DY., Shin SM., Lee SJ. A case of hemolytic disease of newborn due to anti-E. Korean J Hematol. 1981. 16:39–42.6). Lee SE., Kim J., Yoon MS., Song EY., Han KS. A case of hemolytic disease of the newborn due to anti-Mia antibody. Korean J Blood Transfus. 2004. 15:231–5.7). Giacoia GP. Severe fetomaternal hemorrhage: a review. Obstet Gynecol Surv. 1997. 52:372–80.8). Daniels GL., Moulds JJ., Anstee DJ., Bird GW., Brodheim E., Cartron JP, et al. ISBT working party on terminology for red cell surface antigens: São Paulo Report. Vox Sang. 1993 June. 65:77–80.
Article9). Walker RH. Technical manual. 10th ed.Arlington, VA: American Association of Blood Banks;1990. p. 293.10). Han KS., Park MH., Cho HI. Transfusion medicine. 3rd ed.Seoul: Korea Medical Book Publisher;2006. p. 279–84.11). Giblett ER. Blood group alloantibodies: an assessment of some laboratory practice. Transfusion. 1977. 17:299–308.12). Boral LI., Nenry JB. The type and screen: a safe alternative and supplement in selected surgical procedures. Transfusion. 1977. 17:163–8.
Article13). Sung NH., Jeon TY., Lee EY., Chung JS., Cho GJ., Kim HH. Prevalence and specificity of unexpected antibody using antibody screening test including Dia and Mia cells. Korean J Lab Med. 2005. 25:340–6.14). Cleghorn TE. A memorandum on the Miltenberger blood groups. Vox Sang. 1966. 11:219–22.
Article15). Tipett P., Reid ME., Poole J., Green CA., Daniels GL., Anstee DJ. The Miltenberger subsystem: is it obsolescent? Transfus Med Rev. 1992. 6:170–82.16). Chandanayingyong D., Pejrachandra S. Studies on the Miltenberger complex frequency in Thailand and family studies. Vox sang. 1975. 28:152–5.
Article17). Broadberry RE., Lin M. The incidence and significance of anti-"Mia" in Taiwan. Transfusion. 1994. 34:349–52.
Article18). Mak KH., Banks JA., Lubenko A., Chua KM., Torres de Jardine AL., Yan KF. A survey of the incidence of Milten-berger antibodies among Hong Kong Chinese blood donors. Transfusion. 1994. 34:238–41.
Article19). Christine AG., Sherin UD. Avery's diseases of the newborn. 9th ed.Elsevier;2012. p. 1087–92.20). Kim WB., Lee DH., Kang DY. The incidence of irregular antibodies in Korean blood donors, pregnant and multiparous women. Korean J Pathol. 1982. 16:243–9.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Two Cases of Hemolytic Disease of the Newbom due to Anti-E Antibody in Sisters
- Two cases of massive fetomaternal hemorrhage treated by exchange transfusion
- Neonatal Severe Anemia Due to Massive Fetomaternal Hemorrhage
- A Case of Hemolytic Disease in a Newborn Due to Anti-Jk(b)
- Clinical & Hematologic Observation of Neonatal Hemolytic Disease due to Minor Blood Group Isoimmunization