Ann Pediatr Endocrinol Metab.
2022 Jun;27(2):142-147. 10.6065/apem.2142006.003.
Three pediatric patients with primary hyperparathyroidism caused by parathyroid adenoma
- Affiliations
-
- 1Department of Pediatrics, Chungbuk National University Hospital, Chungbuk National University College of Medicine, Cheongju, Korea
- 2Department of Pediatrics, Asan Medical Center Children's Hospital, University of Ulsan College of Medicine, Seoul, Korea
- KMID: 2531279
- DOI: http://doi.org/10.6065/apem.2142006.003
Abstract
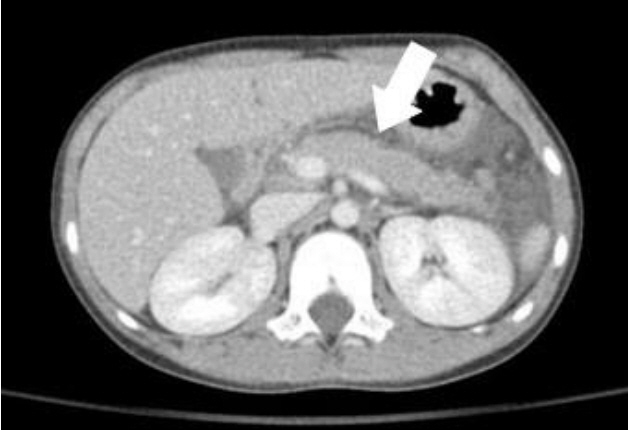
- Primary hyperparathyroidism (PHPT) is a hypercalcemia disorder with inappropriately normal or increased serum parathyroid hormone (PTH) levels resulting from excessive secretion of PTH from one or more of the parathyroid glands. PHPT is uncommon in infants and children, with an estimated incidence of 2–5 cases per 100,000 persons. Patients with PHPT usually present with bone pain, urolithiasis, or nephrolithiasis, as well as nonspecific symptoms such as fatigue and weakness. Asymptomatic hypercalcemia may also be detected incidentally. Only a few cases of pediatric PHPT have been reported in Korea. We present three patients (a 9-year-old girl, a 14-year-old boy, and a 14-year-old girl) with PHPT who manifested variable clinical features of hypercalcemia. The first and second patients each had a parathyroid adenoma and presented with abdominal pain caused by pancreatitis and a ureter stone, respectively. The third patient had an ectopic mediastinal parathyroid adenoma and presented with gait disturbance and weakness of the lower extremities. All of the patients underwent surgical resection of parathyroid adenoma, and their serum calcium levels subsequently normalized without medication.
Figure
Reference
-
References
1. Akerstrom G, Hellman P, Hessman O, Segersten U, Westin G. Parathyroid glands in calcium regulation and human disease. Ann N Y Acad Sci. 2005; 1040:53–8.2. Goltzman D, Mannstadt M, Marcocci C. Physiology of the calcium-parathyroid hormone-vitamin D axis. Front Horm Res. 2018; 50:1–13.3. Griebeler ML, Kearns AE, Ryu E, Hathcock MA, Melton LJ 3rd, Wermers RA. Secular trends in the incidence of primary hyperparathyroidism over five decades (1965-2010). Bone. 2015; 73:1–7.4. Khan AA, Hanley DA, Rizzoli R, Bollerslev J, Young JE, Rejnmark L, et al. Primary hyperparathyroidism: review and recommendations on evaluation, diagnosis, and management. A Canadian and international consensus. Osteoporos Int. 2017; 28:1–19.5. Stack BC, Bodenner D, editors. Medical and surgical treatment of parathyroid diseases: an evidence-based approach. Cham (Switzerland): Springer International Publishing;2017. p. 593–604.6. Park WH, Bae BJ, Choi SO. Primary hyperparathyroidism due to parathyroid adenoma. J Korean Assoc Pediatr Surg. 2000; 6:68–9.7. Kang MJ, Hong HS, Chung SJ, Lee YA, Shin CH, Yang SW. Body composition and bone density reference data for Korean children, adolescents, and young adults according to age and sex: results of the 2009-2010 Korean National Health and Nutrition Examination Survey (KNHANES). J Bone Miner Metab. 2016; 34:429–39.8. Ruda JM, Hollenbeak CS, Stack BC Jr. A systematic review of the diagnosis and treatment of primary hyperparathyroidism from 1995 to 2003. Otolaryngol Head Neck Surg. 2005; 132:359–72.9. Merlino JI, Ko K, Minotti A, McHenry CR. The false negative technetium-99m-sestamibi scan in patients with primary hyperparathyroidism: correlation with clinical factors and operative findings. Am Surg. 2003; 69:225–9. discussion 229-30.10. Lumachi F, Zucchetta P, Marzola MC, Boccagni P, Angelini F, Bui F, et al. Advantages of combined technetium-99m-sestamibi scintigraphy and high-resolution ultrasonography in parathyroid localization: comparative study in 91 patients with primary hyperparathyroidism. Eur J Endocrinol. 2000; 143:755–60.11. Boggs E, Szymusiak J. Common in adults and often overlooked in pediatrics: primary hyperparathyroidism in an adolescent patient. Pediatrics. 2018; 141:490.12. Vanstone MB, Udelsman RD, Cheng DW, Carpenter TO. Rapid correction of bone mass after parathyroidectomy in an adolescent with primary hyperparathyroidism. J Clin Endocrinol Metab. 2011; 96:E347–50.13. Shah VN, Bhadada SK, Bhansali A, Behera A, Mittal BR, Bhavin V. Influence of age and gender on presentation of symptomatic primary hyperparathyroidism. J Postgrad Med. 2012; 58:107–11.14. Misgar RA, Mathew V, Pandit K, Chowdhury S. Primary hyperparathyroidism presenting as recurrent acute pancreatitis: a case report and review of literature. Indian J Endocrinol Metab. 2011; 15:54–6.15. Bai HX, Giefer M, Patel M, Orabi AI, Husain SZ. The association of primary hyperparathyroidism with pancreatitis. J Clin Gastroenterol. 2012; 46:656–61.16. Mithöfer K, Fernández-Del Castillo C, Frick TW, Lewandrowski KB, Rattner DW, Warshaw AL. Acute hypercalcemia causes acute pancreatitis and ectopic trypsinogen activation in the rat. Gastroenterology. 1995; 109:239–46.17. Alghamdi AA, Ahmad MM, Almalki MH. Slipped capital femoral epiphysis and primary hyperparathyroidism: a case report. Clin Med Insights Endocrinol Diabetes. 2016; 9:73–76.18. Papavasiliou KA, Kapetanos GA, Kirkos JM, Beslikas TA, Dimitriadou AS, Papavasiliou VA. The pathogenetic influence of i-parathyroid hormone on slipped capital femoral epiphysis. Towards a new etiologic approach? J Musculoskelet Neuronal Interact. 2003; 3:251–7.19. Eapen E, Grey V, Don-Wauchope A, Atkinson SA. Bone health in childhood: usefulness of biochemical biomarkers. EJIFCC. 2008; 19:123–36.20. Eriksen EF. Cellular mechanisms of bone remodeling. Rev Endocr Metab Disord. 2010; 11:219–27.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Parathyroid Adenoma without Hyperparathyroidism Presenting as a Large Neck Mass
- A Case of Hyperparathyroidism Caused by Intrathyroidal Parathyroid Adenoma
- A case of primary hyperparathyroidism caused by parathyroid adenoma
- Primary Hyperparathyroidism by Parathyroid Gland Adenoma (Report of 2 cases with Review of the Literature)
- Giant Parathyroid Adenoma in the Posterior Mediastinum