J Rhinol.
2019 Nov;26(2):122-126. 10.18787/jr.2019.26.2.122.
Two Cases of Actinomycosis with Aspergillosis in Unilateral Paranasal Sinuses
- Affiliations
-
- 1Department of Otorhinolaryngology-Head and Neck Surgery, School of Medicine, Kyung Hee University, Seoul, Korea. drkimsw@hanmail.net
- 2Department of Otorhinolaryngology-Head and Neck Surgery, Graduate School, Kyung Hee University, Seoul, Korea.
- KMID: 2465545
- DOI: http://doi.org/10.18787/jr.2019.26.2.122
Abstract
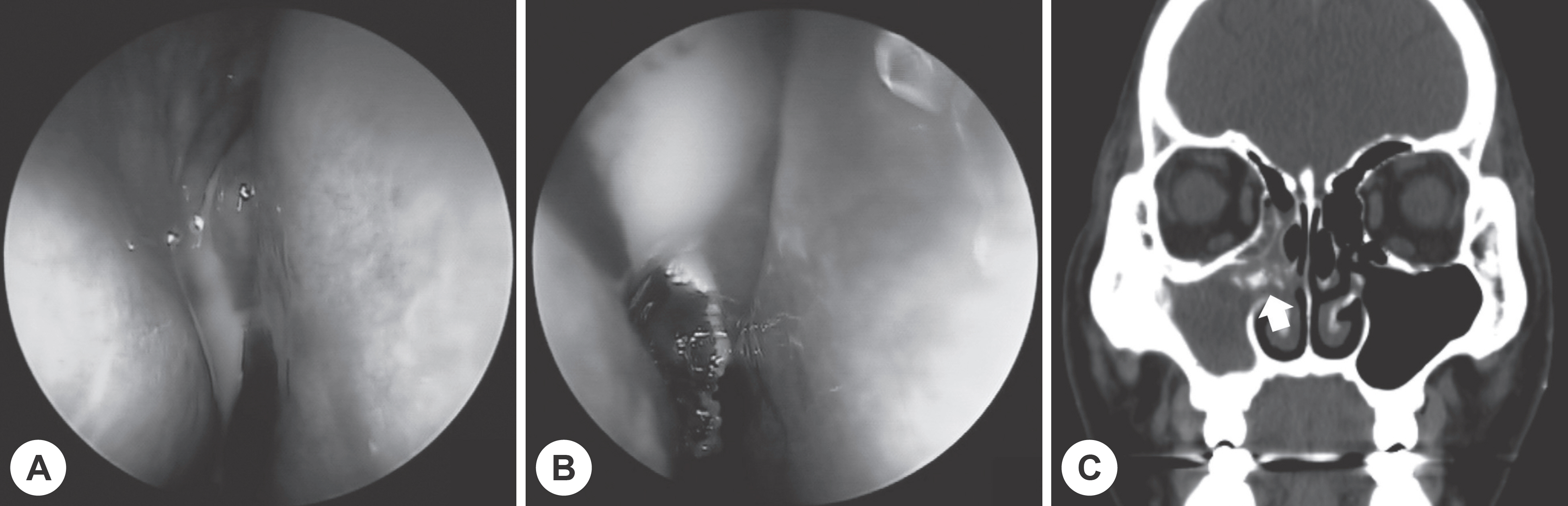
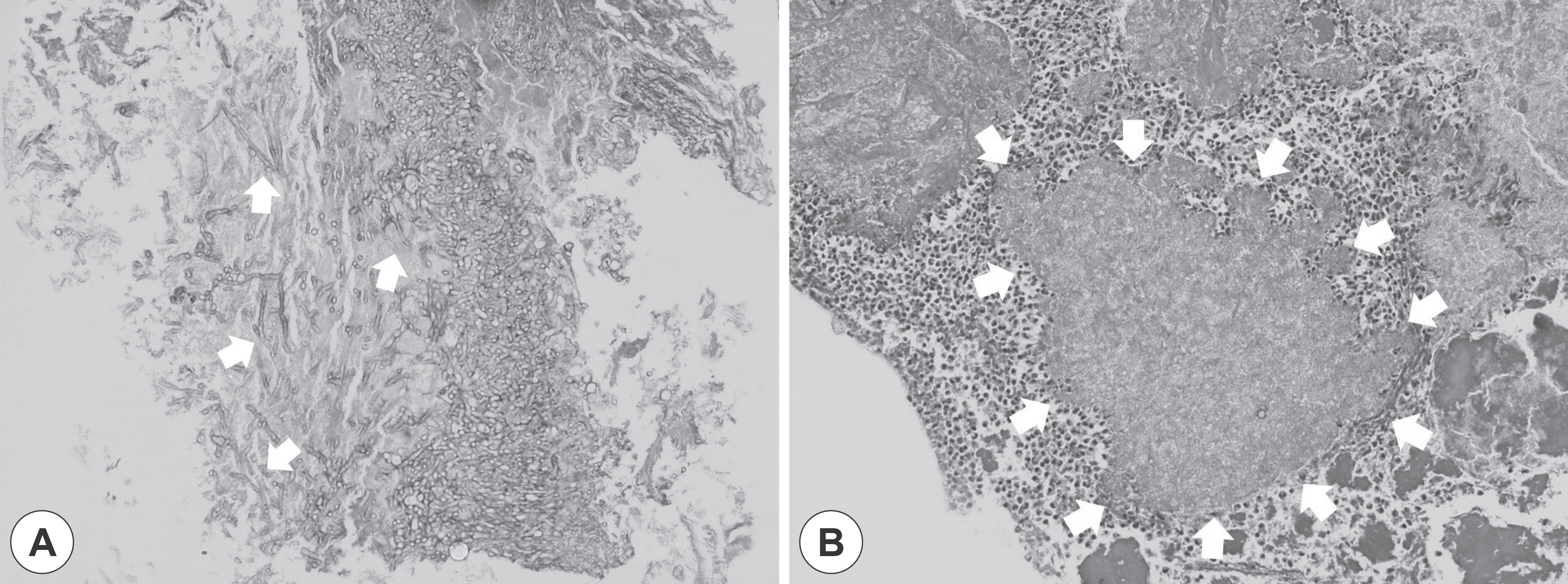
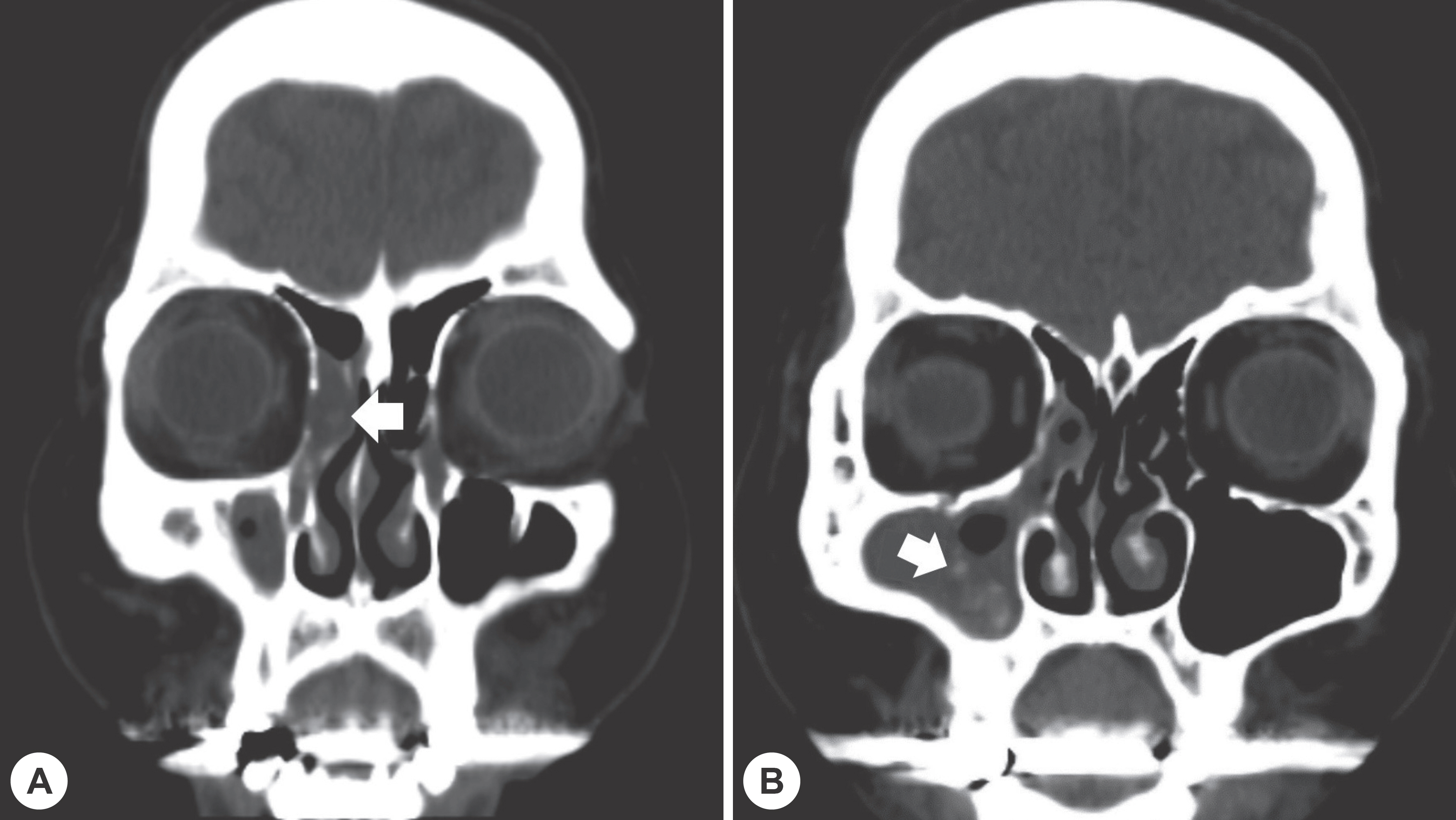
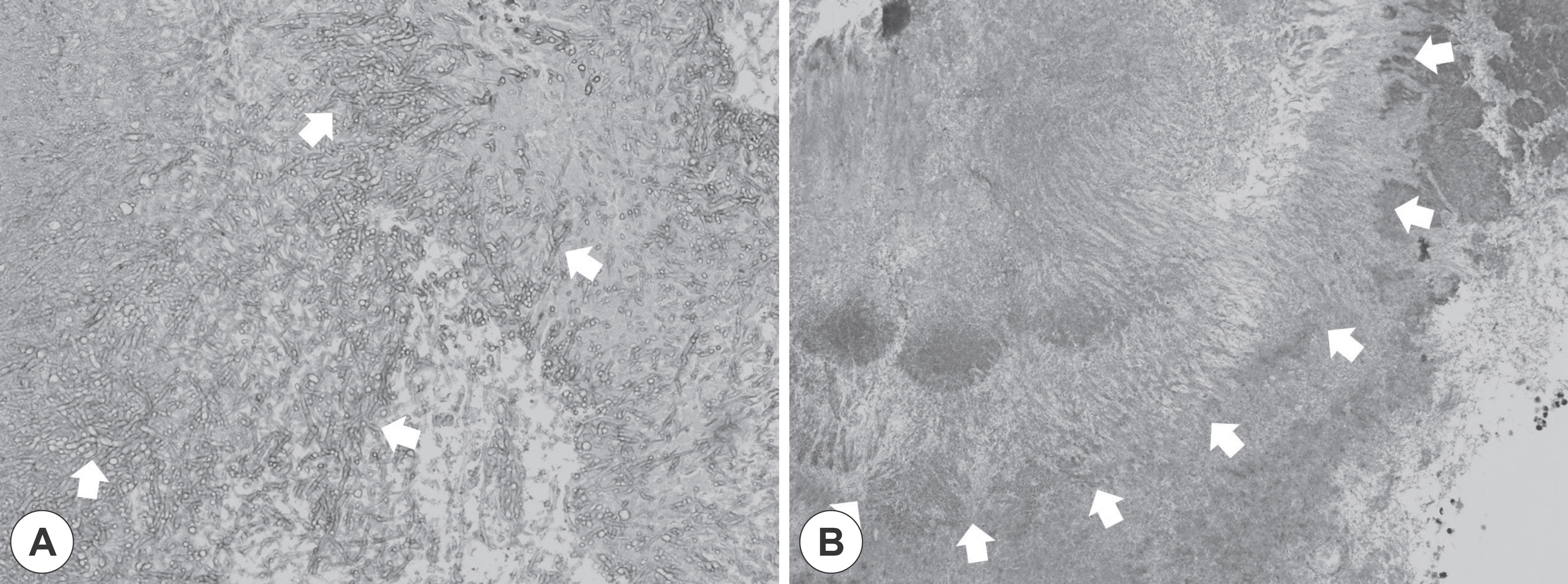
- Actinomycosis of paranasal sinus is a very rare disease that is caused by infection of Actinomyces species that were present in oral or nasal flora due to trauma or dental treatment. Actinomycosis shows a local calcified lesion associated with soft tissue density on computed tomography, which is similar to fungal sinusitis. Actinomycosis associated with fungal ball due to Aspergillus affecting sinus ventilation has been rarely reported. We experienced two cases of actinomycosis associated with fungal ball and successfully treated with endoscopic sinus surgery and oral antibiotics for 3 months without recurrence.
Keyword
MeSH Terms
Figure
Reference
-
References
1. Könönen E, Wade WG. Actinomyces and related organisms in human infections. Clin Microbiol Rev. 2015; 28(2):419–42.
Article2. Moghimi M, Salentijn E, Debets-Ossenkop Y, Karagozoglu KH, Forouzanfar T. Treatment of cervicofacial actinomycosis: a report of 19 cases and review of literature. Med Oral Patol Oral Cir Bucal. 2013; 18(4):e627–32.
Article3. Kim SJ, Lee EJ, Lee JH, Bae WY. A Case of Aspergillosis and Actinomycosis of Each Side of Maxillary Sinuses. Korean J Otorhinolaryngol-Head Neck Surg. 2017; 60(9):471–4.
Article4. Pagella F, Matti E, De Bernardi F, Semino L, Cavanna C, Marone P, et al. Paranasal sinus fungus ball: diagnosis and management. Mycoses. 2007; 50(6):451–6.
Article5. Vinay BH, Mohan A, Haritha P, Lakshmi KR. A rare coexistence of aspergillosis with actinomycosis. J Oral Maxillofac Pathol. 2017; 21(2):277–81.
Article6. Lee JH, Jun KH, Yun KJ. A Case of Actinomycosis of Maxillary Sinus. Korean J Otorhinolaryngol-Head Neck Surg. 2007; 50(1):80–2.7. Roth M, Montone KT. Actinomycosis of the paranasal sinuses: a case report and review. Otolaryngol Head Neck Surg. 1996; 114(6):818–21.
Article8. Kim BS, Kim KS, Choi JS. A Case of Actinomycosis of the Maxillary Sinus Accompanied with Fungal Ball. J Rhinol. 2010; 17(1):57–9.9. Damante JH, Sant'Ana E, Soares CT, Moreira CR. Chronic sinusitis unresponsive to medical therapy: a case of maxillary sinus actinomycosis focusing on computed tomography findings. Dentomaxillofac Radiol. 2006; 35(3):213–6.
Article10. Choi JW, Lee TB, Hwang SH, Kim BH. A Rare Case of Actinomycosis in Nasal Cavity with Aspergillus Sinusitis. Korean J Otorhinolaryngol-Head Neck Surg. 1997; 40(12):1844–7.11. Woo HJ, Bae CH, Song SY, Choi YS, Kim YD. Actinomycosis of the paranasal sinus. Otolaryngol Head Neck Surg. 2008; 139(3):460–2.
Article12. Cardoso IC, de Mattos Oliveira F, Hochhegger B, Severo LC. Sphe-noid sinus fungus ball by filaments of actinomycetes and Aspergillus fumigatus. Mycopathologia. 2015; 179(5–6):471–3.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- A Case of Aspergillosis and Actinomycosis of Each Side of Maxillary Sinuses
- Aspergillosis of the paranasal sinuses: diagnostic significance of the computed tomography
- A Case of Isolated Frontal Sinus Aspergillosis
- A Case of Actinomycosis of the Maxillary Sinus Accompanied with Fungal Ball
- A Case of Prostatic Aspergillosis