Yonsei Med J.
2019 Dec;60(12):1164-1173. 10.3349/ymj.2019.60.12.1164.
Controlling Nutritional Status Score is Associated with All-Cause Mortality in Patients with Antineutrophil Cytoplasmic Antibody-Associated Vasculitis
- Affiliations
-
- 1Division of Rheumatology, Department of Internal Medicine, Yonsei University College of Medicine, Seoul, Korea. sangwonlee@yuhs.ac
- 2Institute for Immunology and Immunological Disease, Yonsei University College of Medicine, Seoul, Korea.
- KMID: 2463795
- DOI: http://doi.org/10.3349/ymj.2019.60.12.1164
Abstract
- PURPOSE
The controlling nutritional status (CONUT) score was developed to detect undernutrition in patients. Here, we investigated whether the CONUT score estimated at diagnosis could help predict poor outcomes [all-cause mortality, relapse, and end-stage renal disease (ESRD)] of antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV).
MATERIALS AND METHODS
We retrospectively reviewed and collated data, including baseline characteristics, clinical manifestations (to calculate AAV-specific indices), and laboratory results, from 196 newly diagnosed AAV patients. Serum albumin, peripheral lymphocyte, and total cholesterol levels (at diagnosis) were used to calculate CONUT scores.
RESULTS
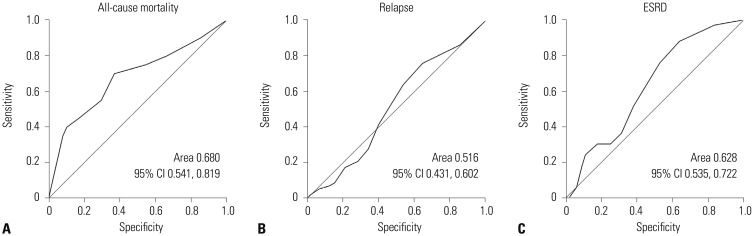
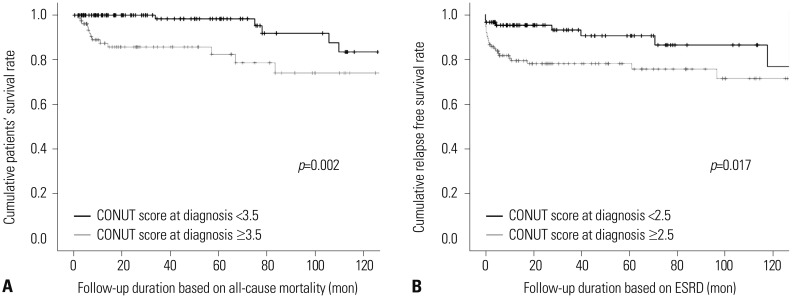
In total, 111 patients had high CONUT scores (≥3), which showed higher frequency of myeloperoxidase-ANCA and ANCA positivity, and demonstrated higher AAV-specific indices. The optimal cut-offs of CONUT score (at diagnosis) for predicting all-cause mortality and ESRD were ≥3.5 and ≥2.5, respectively. Patients with CONUT scores higher than the cut-off at diagnosis exhibited lower cumulative and ESRD-free survival rates compared to those with lower scores than the cut-off. In multivariable analyses, diabetes mellitus [hazard ratio (HR): 4.394], five-factor score (HR: 3.051), and CONUT score ≥3.5 (HR: 4.307) at diagnosis were independent predictors of all-cause mortality, while only serum creatinine (HR: 1.714) was an independent predictor of ESRD occurrence.
CONCLUSION
CONUT score at diagnosis is associated with all-cause mortality in AAV patients.
MeSH Terms
-
Anti-Neutrophil Cytoplasmic Antibody-Associated Vasculitis
Antibodies, Antineutrophil Cytoplasmic
Cholesterol
Creatinine
Cytoplasm*
Diabetes Mellitus
Diagnosis
Humans
Kidney Failure, Chronic
Lymphocytes
Malnutrition
Mortality*
Nutritional Status*
Recurrence
Retrospective Studies
Serum Albumin
Survival Rate
Vasculitis*
Antibodies, Antineutrophil Cytoplasmic
Cholesterol
Creatinine
Serum Albumin
Figure
Reference
-
1. Jennette JC, Falk RJ, Bacon PA, Basu N, Cid MC, Ferrario F, et al. 2012 revised International Chapel Hill Consensus Conference Nomenclature of Vasculitides. Arthritis Rheum. 2013; 65:1–11. PMID: 23045170.
Article2. Jennette JC, Falk RJ, Andrassy K, Bacon PA, Churg J, Gross WL, et al. Nomenclature of systemic vasculitides. Proposal of an international consensus conference. Arthritis Rheum. 1994; 37:187–192. PMID: 8129773.3. Tan JA, Dehghan N, Chen W, Xie H, Esdaile JM, Avina-Zubieta JA. Mortality in ANCA-associated vasculitis: ameta-analysis of observational studies. Ann Rheum Dis. 2017; 76:1566–1574. PMID: 28468793.
Article4. Elefante E, Monti S, Bond M, Lepri G, Quartuccio L, Talarico R, et al. One year in review 2017: systemic vasculitis. Clin Exp Rheumatol. 2017; 35 Suppl 103:5–26.5. Kristensen T, Gregersen JW, Krag SR, Ivarsen P. The relation between histopathological classification and renal outcome, ANCA subtype and treatment regimens in ANCA-associated vasculitis. Clin Exp Rheumatol. 2016; 34(3 Suppl 97):S105–S110. PMID: 27241586.6. Furuta S, Chaudhry AN, Arimura Y, Dobashi H, Fujimoto S, Homma S, et al. Comparison of the phenotype and outcome of granulomatosis with polyangiitis between UK and Japanese cohorts. J Rheumatol. 2017; 44:216–222. PMID: 27803133.
Article7. Furuta S, Chaudhry AN, Hamano Y, Fujimoto S, Nagafuchi H, Makino H, et al. Comparison of phenotype and outcome in microscopic polyangiitis between Europe and Japan. J Rheumatol. 2014; 41:325–333. PMID: 24429174.
Article8. Moon JS, Ahn SS, Park YB, Lee SK, Lee SW. C-reactive protein to serum albumin ratio is an independent predictor of all-cause mortality in patients with ANCA-associated vasculitis. Yonsei Med J. 2018; 59:865–871. PMID: 30091320.
Article9. Ahn SS, Yoo J, Jung SM, Song JJ, Park YB, Lee SW. Clinical role of albumin to globulin ratio in microscopic polyangiitis: a retrospective monocentric study. Clin Rheumatol. 2019; 38:487–494. PMID: 30218289.
Article10. Ahn SS, Jung SM, Song JJ, Park YB, Lee SW. Neutrophil to lymphocyte ratio at diagnosis can estimate vasculitis activity and poor prognosis in patients with ANCA-associated vasculitis: a retrospective study. BMC Nephrol. 2018; 19:187. PMID: 30064369.
Article11. Yoo J, Ahn SS, Jung SM, Song JJ, Park YB, Lee SW. Delta neutrophil index is associated with vasculitis activity and risk of relapse in ANCA-associated vasculitis. Yonsei Med J. 2018; 59:397–405. PMID: 29611402.
Article12. Kim Y, Choi H, Jung SM, Song JJ, Park YB, Lee SW. Systemic immune-inflammation index could estimate the cross-sectional high activity and the poor outcomes in immunosuppressive drugnaïve patients with antineutrophil cytoplasmic antibody-associated vasculitis. Nephrology. 2019; 24:711–717. PMID: 30203901.
Article13. Choi H, Kim Y, Jung SM, Song JJ, Park YB, Lee SW. Low serum complement 3 level is associated with severe ANCA-associated vasculitis at diagnosis. Clin Exp Nephrol. 2019; 23:223–230. PMID: 30168048.
Article14. Ignacio de Ulíbarri J, González-Madroño A, de Villar NG, González P, González B, Mancha A, et al. CONUT: a tool for controlling nutritional status. First validation in a hospital population. Nutr Hosp. 2005; 20:38–45.15. Liang RF, Li JH, Li M, Yang Y, Liu YH. The prognostic role of controlling nutritional status scores in patients with solid tumors. Clin Chim Acta. 2017; 474:155–158. PMID: 28964833.
Article16. Nakagomi A, Kohashi K, Morisawa T, Kosugi M, Endoh I, Kusama Y, et al. Nutritional status is associated with inflammation and predicts a poor outcome in patients with chronic heart failure. J Atheroscler Thromb. 2016; 23:713–727. PMID: 26782970.
Article17. Rus VA, Chitu M, Cernea S, Benedek I, Hodas R, Zavate R, et al. Altered nutritional status, inflammation and systemic vulnerability in patients with acute myocardial infarction undergoing percutaneous coronary revascularisation: a prospective study in a level 3 cardiac critical care unit. Nutr Diet. 2019; 5. 07. DOI: 10.1111/1747-0080.12536. [Epub].
Article18. Mukhtyar C, Lee R, Brown D, Carruthers D, Dasgupta B, Dubey S, et al. Modification and validation of the Birmingham Vasculitis Activity Score (version 3). Ann Rheum Dis. 2009; 68:1827–1832. PMID: 19054820.
Article19. Stone JH, Hoffman GS, Merkel PA, Min YI, Uhlfelder ML, Hellmann DB, et al. A disease-specific activity index for Wegener's granulomatosis: modification of the Birmingham Vasculitis Activity Score. International Network for the Study of the Systemic Vasculitides (INSSYS). Arthritis Rheum. 2001; 44:912–920. PMID: 11318006.20. Guillevin L, Pagnoux C, Seror R, Mahr A, Mouthon L, Le Toumelin P, et al. The Five-Factor Score revisited: assessment of prognoses of systemic necrotizing vasculitides based on the French Vasculitis Study Group (FVSG) cohort. Medicine (Baltimore). 2011; 90:19–27. PMID: 21200183.21. Mukhtyar C, Hellmich B, Jayne D, Flossmann O, Luqmani R. Remission in antineutrophil cytoplasmic antibody-associated systemic vasculitis. Clin Exp Rheumatol. 2006; 24(6 Suppl 43):S-93–S-98.22. Hasegawa M, Hattori K, Sugiyama S, Asada H, Yamashita H, Takahashi K, et al. A retrospective study on the outcomes of MPO-ANCAassociated vasculitis in dialysis-dependent patients. Mod Rheumatol. 2016; 26:110–114. PMID: 25967129.
Article23. Titeca-Beauport D, Francois A, Lobbedez T, Guerrot D, Launay D, Vrigneaud L, et al. Early predictors of one-year mortality in patients over 65 presenting with ANCA-associated renal vasculitis: a retrospective, multicentre study. BMC Nephrol. 2018; 19:317. PMID: 30413153.
Article24. Murray CJ, Atkinson C, Bhalla K, Birbeck G, Burstein R, Chou D, et al. The state of US health, 1990-2010: burden of diseases, injuries, and risk factors. JAMA. 2013; 310:591–608. PMID: 23842577.25. Nago N, Ishikawa S, Goto T, Kayaba K. Low cholesterol is associated with mortality from stroke, heart disease, and cancer: the Jichi Medical School Cohort Study. J Epidemiol. 2011; 21:67–74. PMID: 21160131.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- ANCA : The Marker Antibody of Vasculitis
- ANCA-Associated Vasculitis Presenting with Hypertrophic Pachymeningitis
- ANCA-Associated Vasculitic Neuropathy with Concurrent Pulmonary Tuberculosis
- A Case of Propylthiouracil-induced Lupus Erythematosus Accompanied by Antineutrophil Cytoplasmic Antibody-positive Vasculitis
- Co-existing proteinase 3-antineutrophil cytoplasmic antibody-associated vasculitis with immunoglobulin A nephropathy