Yonsei Med J.
2019 Dec;60(12):1138-1145. 10.3349/ymj.2019.60.12.1138.
Oncologic Outcomes of Extended Lymphadenectomy without Liver Resection for T1/T2 Gallbladder Cancer
- Affiliations
-
- 1Division of Hepatobiliary and Pancreatic Surgery, Department of Surgery, Yonsei University College of Medicine, Seoul, Korea. wjlee@yuhs.ac
- 2Department of Surgery, National Health Insurance Service Ilsan Hospital, Goyang, Korea.
- 3Pancreatobiliary Cancer Center, Yonsei Cancer Center, Severance Hospital, Seoul, Korea.
- KMID: 2463792
- DOI: http://doi.org/10.3349/ymj.2019.60.12.1138
Abstract
- PURPOSE
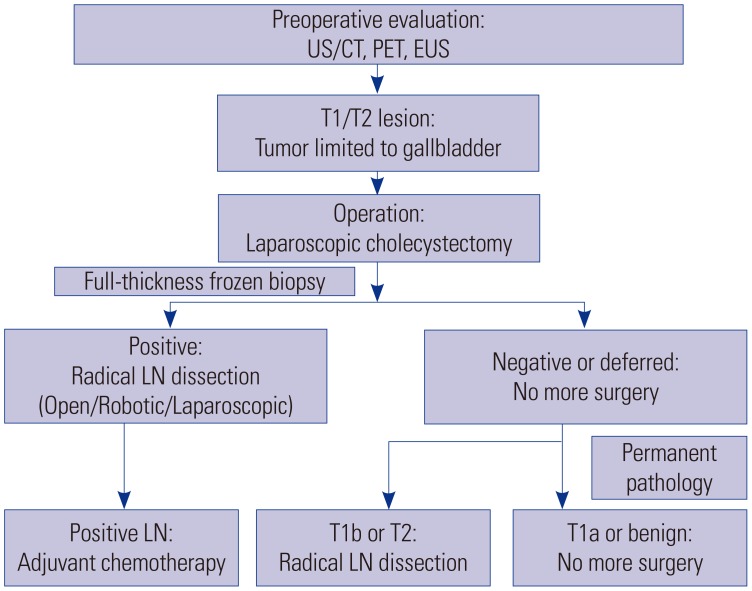
This study provides a standardized operative strategical algorithm that can be applied to patients with T1/T2 gallbladder cancer (GBC). Our aim was to determine the oncologic outcome of radical cholecystectomy with para-aortic lymph node dissection without liver resection in T1/T2 GBC.
MATERIALS AND METHODS
From January 2005 to December 2017, 164 patients with GBC underwent operations by a single surgeon at Severance Hospital. A retrospective review was performed for 113 of these patients, who were pathologically determined to be in stages T1 and T2 according to American Joint Committee on Cancer 7th guidelines.
RESULTS
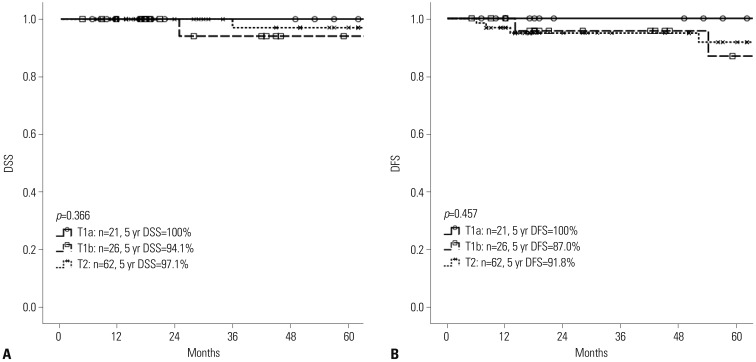
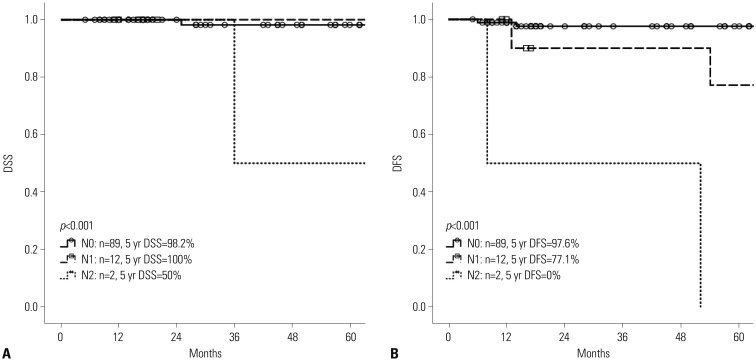
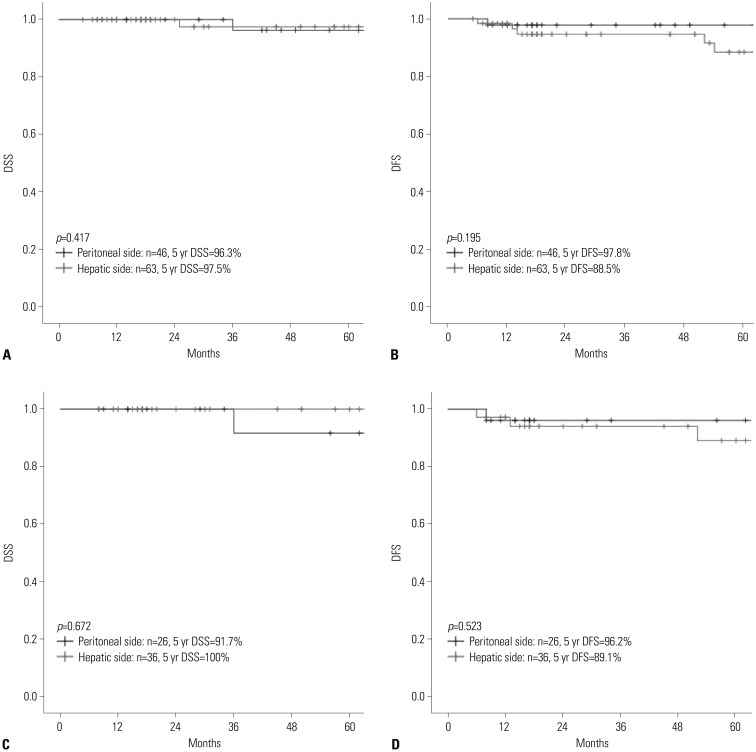
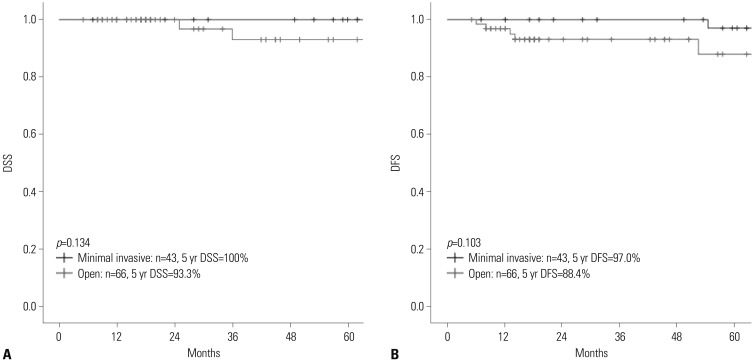
Of the 113 patients, 109 underwent curative resection for T1/T2 GBC; four patients who underwent palliative operations without radical cholecystectomies were excluded from further analyses. For all T1b and T2 lesions, radical cholecystectomy with para-aortic lymph node dissection was performed without liver resection. There were four GBC-related mortalities, and 5-year disease-specific survival was 97.0%. The median follow-up was 50 months (range: 5-145 months). In all T stages, the median was not reached for survival analysis. Five-year disease-specific survival for T1a, T1b, and T2 were 100%, 94.1%, and 97.1%, respectively. Five-year disease-free survival for T1a, T1b, and T2 were 100%, 87.0%, and 91.8%, respectively.
CONCLUSION
Our results suggest that the current operative protocol can be applied to minimal invasive operations for GBC with similar oncologic outcomes as open approach. For T1/T2 GBC, radical cholecystectomy, including para-aortic lymph node dissection, can be performed safely with favorable oncologic outcomes.
MeSH Terms
Figure
Reference
-
1. Hueman MT, Vollmer CM Jr, Pawlik TM. Evolving treatment strategies for gallbladder cancer. Ann Surg Oncol. 2009; 16:2101–2115. PMID: 19495882.
Article2. Lazcano-Ponce EC, Miquel JF, Muñoz N, Herrero R, Ferrecio C, Wistuba II, et al. Epidemiology and molecular pathology of gallbladder cancer. CA Cancer J Clin. 2001; 51:349–364. PMID: 11760569.
Article3. Lee SE, Kim KS, Kim WB, Kim IG, Nah YW, Ryu DH, et al. Practical guidelines for the surgical treatment of gallbladder cancer. J Korean Med Sci. 2014; 29:1333–1340. PMID: 25368485.
Article4. Randi G, Franceschi S, La Vecchia C. Gallbladder cancer worldwide: geographical distribution and risk factors. Int J Cancer. 2006; 118:1591–1602. PMID: 16397865.
Article5. Lee SE, Jang JY, Lim CS, Kang MJ, Kim SW. Systematic review on the surgical treatment for T1 gallbladder cancer. World J Gastroenterol. 2011; 17:174–180. PMID: 21245989.
Article6. Kim DH, Kim SH, Choi GH, Kang CM, Kim KS, Choi JS, et al. Role of cholecystectomy and lymph node dissection in patients with T2 gallbladder cancer. World J Surg. 2013; 37:2635–2640. PMID: 23959341.
Article7. Hoehn RS, Wima K, Ertel AE, Meier A, Ahmad SA, Shah SA, et al. Adjuvant therapy for gallbladder cancer: an analysis of the National Cancer Data Base. J Gastrointest Surg. 2015; 19:1794–1801. PMID: 26293376.
Article8. Ma N, Cheng H, Qin B, Zhong R, Wang B. Adjuvant therapy in the treatment of gallbladder cancer: a meta-analysis. BMC Cancer. 2015; 15:615. PMID: 26337466.
Article9. Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004; 240:205–213. PMID: 15273542.10. Blalock A. A statistical study of eight hundred and eighty-eight cases of biliary tract disease. Johns Hopkins Hosp Bull. 1924; 35:391–409.11. Itano O, Oshima G, Minagawa T, Shinoda M, Kitago M, Abe Y, et al. Novel strategy for laparoscopic treatment of pT2 gallbladder carcinoma. Surg Endosc. 2015; 29:3600–3607. PMID: 25740638.
Article12. Lee H, Choi DW, Park JY, Youn S, Kwon W, Heo JS, et al. Surgical strategy for T2 gallbladder cancer according to tumor location. Ann Surg Oncol. 2015; 22:2779–2786. PMID: 25519930.
Article13. Zimmitti G, Manzoni A, Guerini F, Ramera M, Bertocchi P, Aroldi F, et al. Current role of minimally invasive radical cholecystectomy for gallbladder cancer. Gastroenterol Res Pract. 2016; 7684915. PMID: 27885325.
Article14. Yoon YS, Han HS, Cho JY, Choi Y, Lee W, Jang JY, et al. Is laparoscopy contraindicated for gallbladder cancer? A 10-year prospective cohort study. J Am Coll Surg. 2015; 221:847–853. PMID: 26272017.
Article15. Kang CM, Lee WJ, Choi GH, Kim JY, Kim KS, Choi JS, et al. Does “clinical” R0 have validity in the choice of simple cholecystectomy for gallbladder carcinoma? J Gastrointest Surg. 2007; 11:1309–1316. PMID: 17682825.
Article16. Ito M, Mishima Y. Lymphatic drainage of the gallbladder. J Hepatobiliary Pancreat Surg. 1994; 1:302–308.
Article17. Tsukada K, Hatakeyama K, Kurosaki I, Uchida K, Shirai Y, Muto T, et al. Outcome of radical surgery for carcinoma of the gallbladder according to the TNM stage. Surgery. 1996; 120:816–821. PMID: 8909516.
Article18. Ogura Y, Mizumoto R, Isaji S, Kusuda T, Matsuda S, Tabata M. Radical operations for carcinoma of the gallbladder: present status in Japan. World J Surg. 1991; 15:337–343. PMID: 1853612.
Article19. Kondo S, Nimura Y, Hayakawa N, Kamiya J, Nagino M, Uesaka K. Regional and para-aortic lymphadenectomy in radical surgery for advanced gallbladder carcinoma. Br J Surg. 2000; 87:418–422. PMID: 10759735.
Article20. Lee H, Kwon W, Han Y, Kim JR, Kim SW, Jang JY. Optimal extent of surgery for early gallbladder cancer with regard to long-term survival: a meta-analysis. J Hepatobiliary Pancreat Sci. 2018; 25:131–141. PMID: 29117469.
Article21. Sternby Eilard M, Lundgren L, Cahlin C, Strandell A, Svanberg T, Sandström P. Surgical treatment for gallbladder cancer–a systematic literature review. Scand J Gastroenterol. 2017; 52:505–514. PMID: 28270039.22. Jung W, Jang JY, Kang MJ, Chang YR, Shin YC, Chang J, et al. Effects of surgical methods and tumor location on survival and recurrence patterns after curative resection in patients with T2 gallbladder cancer. Gut Liver. 2016; 10:140–146. PMID: 26347513.
Article23. Horiguchi A, Miyakawa S, Ishihara S, Miyazaki M, Ohtsuka M, Shimizu H, et al. Gallbladder bed resection or hepatectomy of segments 4a and 5 for pT2 gallbladder carcinoma: analysis of Japanese registration cases by the study group for biliary surgery of the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J Hepatobiliary Pancreat Sci. 2013; 20:518–524. PMID: 23430053.
Article24. Pitt SC, Jin LX, Hall BL, Strasberg SM, Pitt HA. Incidental gallbladder cancer at cholecystectomy: when should the surgeon be suspicious? Ann Surg. 2014; 260:128–133. PMID: 24509205.25. Eltawil KM, Gustafsson BI, Kidd M, Modlin IM. Neuroendocrine tumors of the gallbladder: an evaluation and reassessment of management strategy. J Clin Gastroenterol. 2010; 44:687–695. PMID: 20375728.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Effects of Surgical Methods and Tumor Location on Survival and Recurrence Patterns after Curative Resection in Patients with T2 Gallbladder Cancer
- Challenges in Implementing Endoscopic Resection for T2 Colorectal Cancer
- Extent of Surgical Resection in Gallbladder Cancer
- The technique of laparoscopic and robotic extended cholecystectomy for gallbladder cancer
- The Survival Rate of Gallbladder Carcinoma Based on the presence of Lymph Node Metastasis and the Depth of the Primary Tumor Invasion