Ann Rehabil Med.
2017 Feb;41(1):153-157. 10.5535/arm.2017.41.1.153.
Diagnostic Challenge of Diffusion Tensor Imaging in a Patient With Hemiplegia After Traumatic Brain Injury
- Affiliations
-
- 1Department of Physical Medicine and Rehabilitation, Chung-Ang University College of Medicine, Seoul, Korea. sihyun92@cau.ac.kr
- 2Department of Neurology, Chung-Ang University College of Medicine, Seoul, Korea.
- KMID: 2383690
- DOI: http://doi.org/10.5535/arm.2017.41.1.153
Abstract
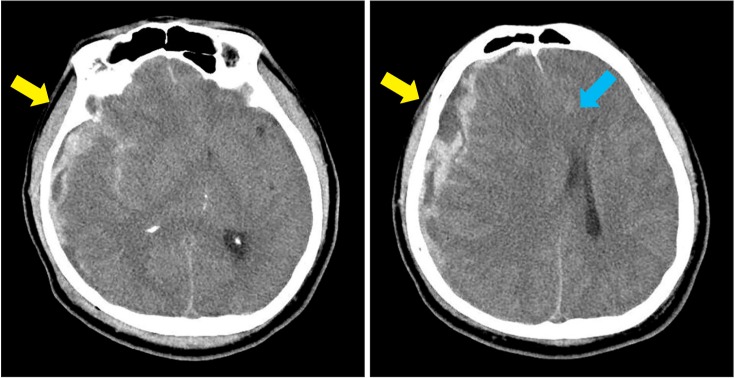
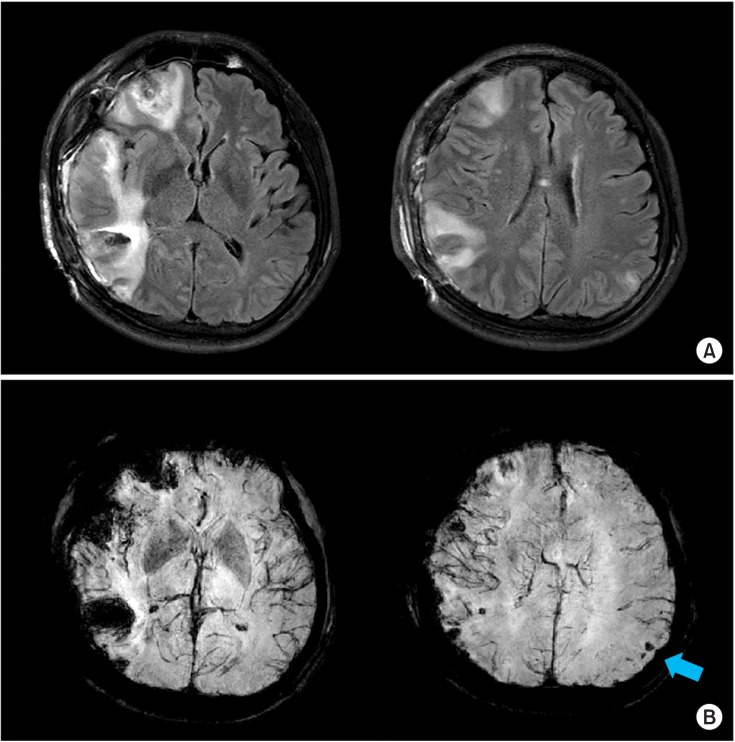
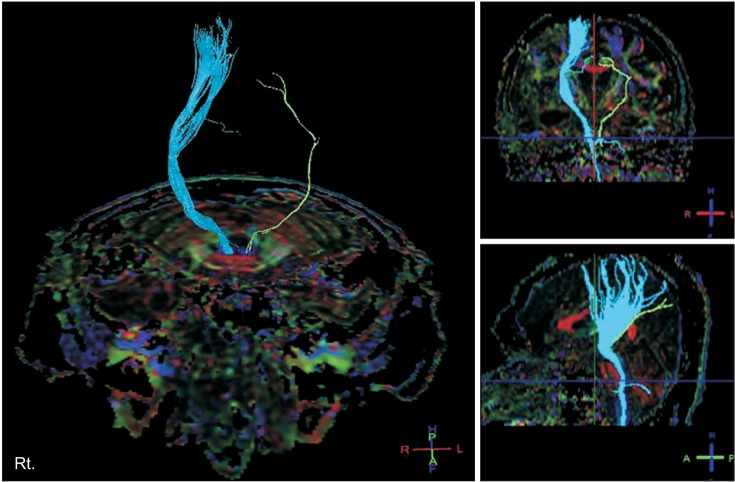
- A 51-year-old man showed hemiplegia on his right side after a traumatic brain injury (TBI). On initial brain computed tomography (CT) scan, an acute subdural hemorrhage in the right cerebral convexity and severe degrees of midline shifting and subfalcine herniation to the left side were evident. On follow-up brain magnetic resonance imaging (MRI), there were multiple microhemorrhages in the left parietal and occipital subcortical regions. To explain the occurrence of right hemiplegia after brain damage which dominantly on the right side of brain, we used diffusion tensor imaging (DTI) to reconstruct the corticospinal tract (CST), which showed nearly complete injury on the left CST. We also performed motor-evoked potentials, and stimulation of left motor cortex evoked no response on both sides of upper extremity. We report a case of patient with hemiplegia after TBI and elucidation of the case by DTI rather than CT and MRI.
MeSH Terms
Figure
Cited by 1 articles
-
Delayed Extensive White Matter Injury Caused by a Subdural Hemorrhage and Role of Corticospinal Tract Integrity
Kyoung Bo Lee, Sang Cheol Yoon, Joon Sung Kim, Bo Young Hong, Jung Geun Park, Won Jin Sung, Hye Jung Park, Seong Hoon Lim
Brain Neurorehabil. 2019;12(2):. doi: 10.12786/bn.2019.12.e15.
Reference
-
1. Xu J, Rasmussen IA, Lagopoulos J, Haberg A. Diffuse axonal injury in severe traumatic brain injury visualized using high-resolution diffusion tensor imaging. J Neurotrauma. 2007; 24:753–765. PMID: 17518531.
Article2. Nakayama N, Okumura A, Shinoda J, Yasokawa YT, Miwa K, Yoshimura SI, et al. Evidence for white matter disruption in traumatic brain injury without macroscopic lesions. J Neurol Neurosurg Psychiatr. 2006; 77:850–855. PMID: 16574734.
Article3. Yeo SS, Jang SH. Corticospinal tract recovery in a patient with traumatic transtentorial herniation. Neural Regen Res. 2013; 8:469–473. PMID: 25206689.4. Mori S, Zhang J. Principles of diffusion tensor imaging and its applications to basic neuroscience research. Neuron. 2006; 51:527–539. PMID: 16950152.
Article5. Shin HW, Sohn YH. Interhemispheric transfer of paired associative stimulation-induced plasticity in the human motor cortex. Neuroreport. 2011; 22:166–170. PMID: 21263361.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Central Pain Due to Traumatic Axonal Injury of the Spinothalamic Tract in Patients with Mild Traumatic Brain Injury
- Analysis of Diffuse Axonal Injury Using Diffusion Tensor Imaging in Traumatic Brain Injury Patients
- Diagnostic History of Traumatic Axonal Injury in Patients with Cerebral Concussion and Mild Traumatic Brain Injury
- Diffusion Tensor Tractography in Two Cases of Kernohan-Woltman Notch Phenomenon
- Usefulness of Diffusion Tensor Imaging in Unexplained Ipsilateral Hemiplegia