Urogenit Tract Infect.
2016 Apr;11(1):7-11. 10.14777/uti.2016.11.1.7.
National Trends of Antimicrobial Resistance in Uncomplicated Cystitis
- Affiliations
-
- 1Department of Urology, The Catholic University of Korea, St. Vincent's Hospital, Suwon, Korea. lee.seungju@gmail.com
- KMID: 2319422
- DOI: http://doi.org/10.14777/uti.2016.11.1.7
Abstract
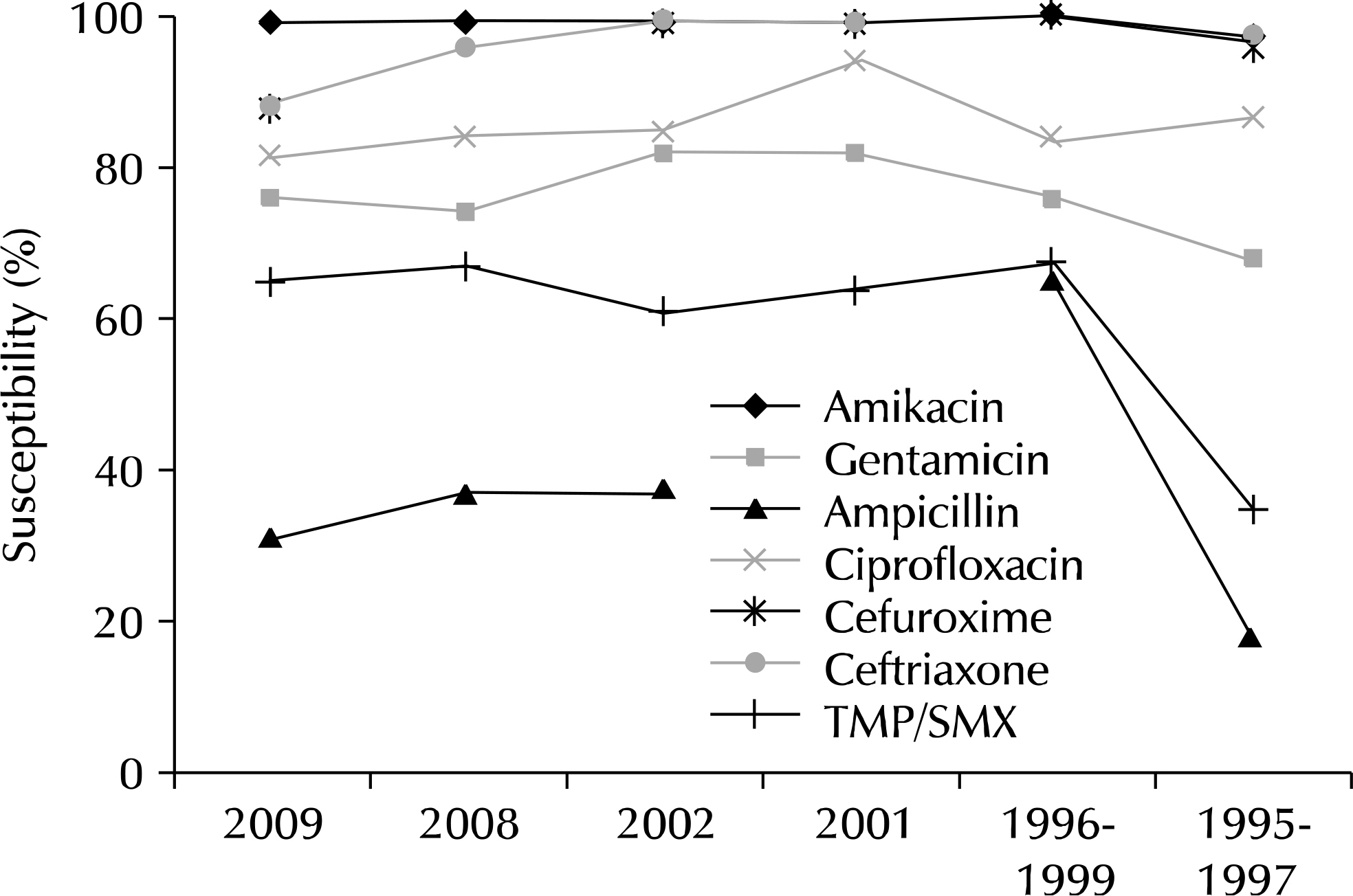
- Acute uncomplicated cystitis is a common bacterial infection of the urinary bladder in women. Antibiotic resistance against Escherichia coli is increasing nationwide in Korea; therefore, we reviewed the local available data regarding acute cystitis. The recently determined susceptibilities of E. coli to gentamicin, fluoroquinolone, 3rd generation cephalosporin, and amikacin are 75%, 85-95%, 95%, and 97%, respectively. The resistance rates of E. coli to trimethoprim/sulfamethoxazole, fluoroquinolone, and even 3rd generation cephalosporin are higher in Korea compared with other countries, however, the studies that determined those resistance rates included data collected at tertiary referral hospitals, which may have been overestimated. Continuous monitoring of antibiotic resistance and opportune establishment and revision of treatment guidelines are required for the optimal management of acute cystitis.
MeSH Terms
Figure
Cited by 1 articles
-
The Association between Chronic Inflammation and Recurrent Cystitis in Women
Hong Chung
Urogenit Tract Infect. 2016;11(3):86-92. doi: 10.14777/uti.2016.11.03.86.
Reference
-
References
1. Hooton TM. Fluoroquinolones and resistance in the treatment of uncomplicated urinary tract infection. Int J Antimicrob Agents. 2003; 22(Suppl 2):65–72.
Article2. Fihn SD. Clinical practice. Acute uncomplicated urinary tract infection in women. N Engl J Med. 2003; 349:259–66.3. Foxman B, Barlow R, D'Arcy H, Gillespie B, Sobel JD. Urinary tract infection: self-reported incidence and associated costs. Ann Epidemiol. 2000; 10:509–15.4. Car J. Urinary tract infections in women: diagnosis and management in primary care. BMJ. 2006; 332:94–7.
Article5. Lee SJ, Lee DS, Choe HS, Shim BS, Kim CS, Kim ME, et al. Antimicrobial resistance in community-acquired urinary tract infections: results from the Korean Antimicrobial Resistance Monitoring System. J Infect Chemother. 2011; 17:440–6.6. Shin J, Kim J, Wie SH, Cho YK, Lim SK, Shin SY, et al. Fluoroquinolone resistance in uncomplicated acute pyelonephritis: epidemiology and clinical impact. Microb Drug Resist. 2012; 18:169–75.
Article7. Lee SJ, Lee SD, Cho IR, Sim BS, Lee JG, Kim CS, et al. Antimicrobial susceptibility of uropathogens causing acute uncomplicated cystitis in female outpatients in South Korea: a multicentre study in 2002. Int J Antimicrob Agents. 2004; 24(Suppl 1):S61–4.
Article8. Wie SH, Choi SM, Lee DG, Kim SY, Kim SI, Yoo JH, et al. Antibiotic sensitivity of the causative organisms and use of antibiotics in women with community-acquired acute pyelonephritis. Korean J Infect Dis. 2002; 34:353–9.9. Kim SW, Lee JY, Park WJ, Cho YH, Yoon MS. Antibiotic sensitivity to the causative organism of acute simple urinary tract infection for recent 3 years. Korean J Infect Dis. 2000; 32:380–7.10. Min HJ. Acute pyelonephritis: clinical study and consideration about inpatient therapy. Korean J Med. 1998; 55:232–44.11. Gupta K, Hooton TM, Naber KG, Wullt B, Colgan R, Miller LG, et al. Infectious Diseases Society of America; European Society for Microbiology and Infectious Diseases. International clinical practice guidelines for the treatment of acute uncomplicated cystitis and pyelonephritis in women: a 2010 update by the Infectious Diseases Society of America and the European Society for Microbiology and Infectious Diseases. Clin Infect Dis. 2011; 52:e103–20.
Article12. Kim ME, Ha US, Cho YH. Prevalence of antimicrobial resistance among uropathogens causing acute uncomplicated cystitis in female outpatients in South Korea: a multicentre study in 2006. Int J Antimicrob Agents. 2008; 31(Suppl 1):S15–8.
Article13. Yu Y, Zhou W, Chen Y, Ding Y, Ma Y. Epidemiological and antibiotic resistant study on extended-spectrum beta-lactamase-producing Escherichia coli and Klebsiella pneumoniae in Zhejiang Province. Chin Med J (Engl). 2002; 115:1479–82.14. Johnson L, Sabel A, Burman WJ, Everhart RM, Rome M, MacKenzie TD, et al. Emergence of fluoroquinolone resistance in outpatient urinary Escherichia coli isolates. Am J Med. 2008; 121:876–84.
Article15. Kahlmeter G. The ECO.SENS Project: a prospective, multinational, multicentre epidemiological survey of the prevalence and antimicrobial susceptibility of urinary tract pathogens–interim report. J Antimicrob Chemother. 2000; 46(Suppl 1):15–22. ; discussion 63–5.
Article16. Baudry-Simner PJ, Singh A, Karlowsky JA, Hoban DJ, Zhanel GG. Canadian Antimicrobial Resistance Alliance. Mechanisms of reduced susceptibility to ciprofloxacin in Escherichia coli isolates from Canadian hospitals. Can J Infect Dis Med Microbiol. 2012; 23:e60–4.17. Hawkey PM, Jones AM. The changing epidemiology of resistance. J Antimicrob Chemother. 2009; 64(Suppl 1):i3–10.
Article18. Stamey TA, Fair WR, Timothy MM, Millar MA, Mihara G, Lowery YC. Serum versus urinary antimicrobial concentrations in cure of urinary-tract infections. N Engl J Med. 1974; 291:1159–63.
Article19. Masterton RG, Bochsler JA. High-dosage co-amoxiclav in a single dose versus 7 days of co-trimoxazole as treatment of uncomplicated lower urinary tract infection in women. J Antimicrob Chemother. 1995; 35:129–37.
Article20. McCarty JM, Richard G, Huck W, Tucker RM, Tosiello RL, Shan M, et al. A randomized trial of short-course ciprofloxacin, ofloxacin, or trimethoprim/sulfamethoxazole for the treatment of acute urinary tract infection in women. Ciprofloxacin Urinary Tract Infection Group. Am J Med. 1999; 106:292–9.21. Fang GD, Brennen C, Wagener M, Swanson D, Hilf M, Zadecky L, et al. Use of ciprofloxacin versus use of aminoglycosides for therapy of complicated urinary tract infection: prospective, randomized clinical and pharmacokinetic study. Antimicrob Agents Chemother. 1991; 35:1849–55.
Article22. Lee SE, Choi H, Kim YK. A clinical study of oral fosfomycin (fosmycin) in the treatment of lower urinary tract infection. Korean J Urol. 1984; 25:167–72.23. Kim KY, Kim CS, Lim DH. The ciprofloxacin resistance pattern of escherichia coli isolated from female patients with community-acquired urinary tract infection in the Jeonnam and Gwangju region for the recent 2-years. Korean J Urol. 2008; 49:540–8.
Article24. Ryu KH, Kim MK, Jeong YB. A recent study on the antimicrobial sensitivity of the organisms that cause urinary tract Infection. Korean J Urol. 2007; 48:638–45.
Article25. Lee YW, Chang SK. Clinical efficacy of pivmecillinam (Selexid(R)) in lower urinary tract infections. Korean J Urol. 1983; 24:413–7.26. Clinical guideline for the diagnosis and treatment of urinary tract infections: asymptomatic bacteriuria, uncomplicated & complicated urinary tract infections, bacterial prostatitis. Infect Chemother. 2011; 43:1–25.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Acute uncomplicated cystitis in the emergency department: prevalence of antimicrobial resistance among uropathogens and appropriate antimicrobial treatment
- In-Vitro Susceptibility Study of Oral Antibiotics to Escherichia coli, Isolated From Acute Uncomplicated Cystitis in Female Outpatients
- The Choice of Empirical Treatment of Uncomplicated Cystitis: No Longer Free Ride
- Efficacy of Cefcapene Pivoxil for Empirical Therapy of Acute Uncomplicated Cystitis
- Diagnosis and treatment of women with recurrent urinary tract infection