J Korean Diabetes.
2020 Dec;21(4):216-220. 10.4093/jkd.2020.21.4.216.
Medical Nutrition Therapy Using Continuous Glucose Monitoring System
- Affiliations
-
- 1Department of Food Service and Nutrition Care, Seoul National University Hospital, Seoul, Korea
- KMID: 2511890
- DOI: http://doi.org/10.4093/jkd.2020.21.4.216
Abstract
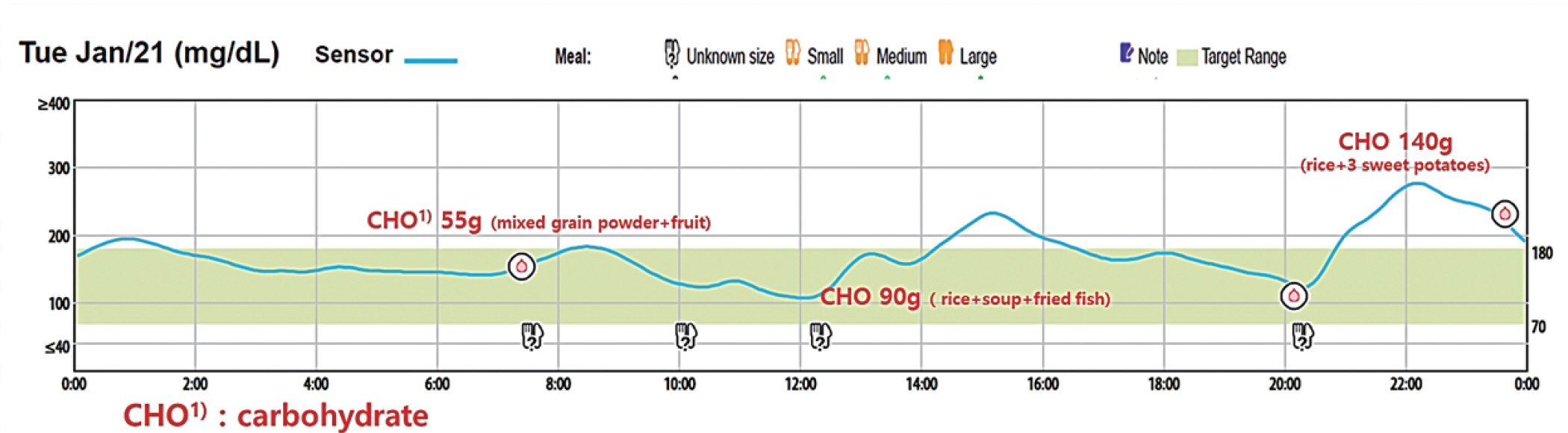
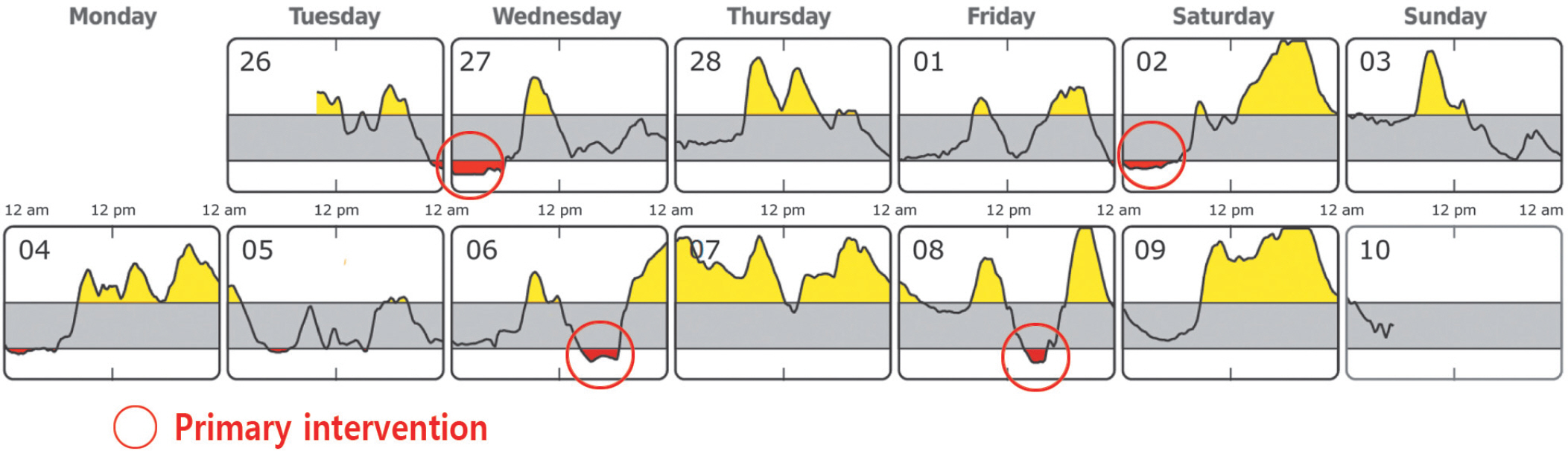
- Medical nutrition therapy plays an integral role in diabetes management. There is no “one-size-fits-all” eating pattern for those with diabetes, and meal planning should be individualized. For many people with diabetes, glucose monitoring is key for glycemic control. Continuous glucose monitoring (CGM) metrics are suggested to provide a personalized diabetes management plan. Use of CGM continues to expand in clinical practice. Integrating CGM results into diabetes management can be useful for guiding medical nutrition therapy and physical activity, preventing hypoglycemia, and adjusting medications. Clinical dietitians should develop personalized nutrition management using CGM to help people with diabetes optimize dietary intake.
Figure
Cited by 1 articles
-
Individualized Medical Nutrition Therapy for Diabetic Patients according to Diabetes Medication
Juyeon Park
J Korean Diabetes. 2022;23(1):50-56. doi: 10.4093/jkd.2022.23.1.50.
Reference
-
1. American Diabetes Association. 6. Glycemic targets: Standards of Medical Care in Diabetes-2020. Diabetes Care. 2020. 43(Suppl 1):S66–76.2. Cappon G., Vettoretti M., Sparacino G., Facchinetti A. Continuous glucose monitoring sensors for diabetes management: a review of technologies and applications. Diabetes Metab J. 2019. 43:383–97.
Article3. Block JM., Buckingham B. Use of real-time continuous glucose monitoring technology in children and adolescents. Diabetes Spectr. 2008. 21:84–90.
Article4. Battelino T., Danne T., Bergenstal RM., Amiel SA., Beck R., Biester T, et al. Clinical targets for continuous glucose monitoring data interpretation: recommendations from the international consensus on time in range. Diabetes Care. 2019. 42:1593–603.5. Nelms M., Sucher KP. Nutrition therapy and pathophysiology. 4th ed.Boston: Cengage;2020. p. 504–17.6. Ministry of Health and Welfare. Job standards and practical toolkits for clinical nutrition therapy. Sejong: Ministry of Health and Welfare;2014. p. 9–37.7. Johnson ML., Martens TW., Criego AB., Carlson AL., Simonson GD., Bergenstal RM. Utilizing the ambulatory glucose profile to standardize and implement continuous glucose monitoring in clinical practice. Diabetes Technol Ther. 2019. 21(S2):S217–25.
Article8. Ajjan RA., Cummings MH., Jennings P., Leelarathna L., Rayman G., Wilmot EG. Optimising use of rate-of-change trend arrows for insulin dosing decisions using the FreeStyle Libre flash glucose monitoring system. Diab Vasc Dis Res. 2019. 16:3–12.
Article9. Aleppo G., Laffel LM., Ahmann AJ., Hirsch IB., Kruger DF., Peters A, et al. A practical approach to using trend arrows on the Dexcom G5 CGM system for the management of adults with diabetes. J Endocr Soc. 2017. 1:1445–60.
Article10. Bell KJ., Smart CE., Steil GM., Brand-Miller JC., King B., Wolpert HA. Impact of fat, protein, and glycemic index on postprandial glucose control in type 1 diabetes: implications for intensive diabetes management in the continuous glucose monitoring era. Diabetes Care. 2015. 38:1008–15.
Article11. American Diabetes Association. 5. Facilitating behavior change and well-being to improve health outcomes: Standards of Medical Care in Diabetes-2020. Diabetes Care. 2020. 43(Suppl 1):S48–65.12. Kang YG. Application of Continuous Glucose Monitoring System (CGMS) and patient education. J Korean Diabetes. 2011. 12:159–62.
Article13. Evert AB., Franz MJ. American Diabetes Association guide to nutrition therapy for diabetes. 3rd ed.Arlington: American Diabetes Association;2017. p. 465–82.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Application of Continuous Glucose Monitoring System (CGMS) and Patient Education
- Glucose Management Using Continuous Glucose Monitors
- Adjustment of Insulin Therapy: New Insights from Continuous Glucose Monitoring
- New Technology for Type 1 Diabetes
- The Occurrence and Management of Adverse Skin Events due to Continuous Glucose Monitoring