J Korean Ophthalmol Soc.
2020 Feb;61(2):209-213. 10.3341/jkos.2020.61.2.209.
Manual Preparation of Donor Lenticule Using Artificial Anterior Chamber for Descemet's Membrane Stripping Endothelial Keratoplasty
- Affiliations
-
- 1Department of Ophthalmology, Chuncheon Sacred Heart Hospital, Hallym University College of Medicine, Chuncheon, Korea.
- 2Department of Ophthalmology, Yeouido St. Mary's Hospital, College of Medicine, The Catholic University of Koea, Seoul, Korea. huanghs@hanmail.net
- KMID: 2470745
- DOI: http://doi.org/10.3341/jkos.2020.61.2.209
Abstract
- PURPOSE
To report a patient with a pseudophakic bullous keratopathy (PBK) who underwent Descemet's membrane stripping endothelial keratoplasty (DSEK) with manual preparation of the donor corneal graft.
CASE SUMMARY
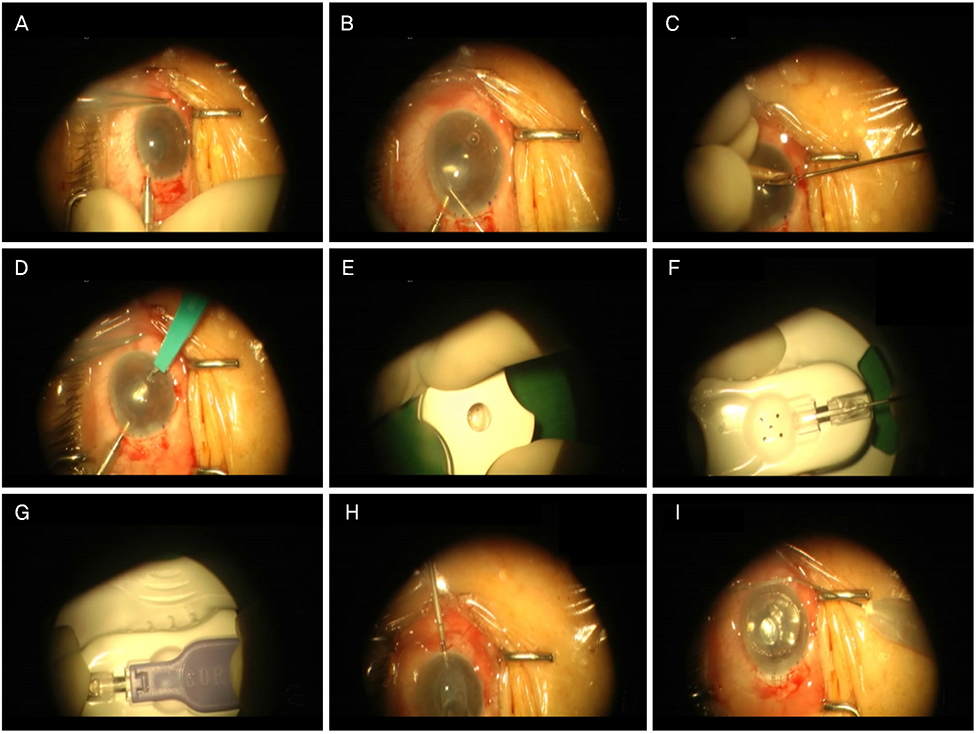
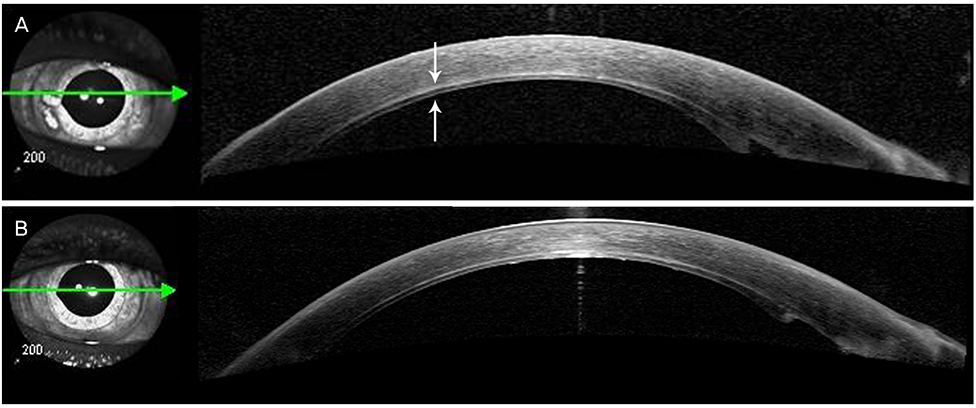
A 61-year-old female presented with visual disturbance in her right eye. Five months prior, she was treated with phacoemulsification and intraocular lens exchange surgery of the right eye, and a very severe corneal edema was revealed by slit-lamp examination. We diagnosed PBK and planned DSEK with manual preparation of a donor corneal graft because of the non-availability of a microkeratome or a femtosecond laser. After making the corneal graft using an artificial anterior chamber, crescent knife and cornea dissector, the keratoplasty proceeded using the graft. Three months after surgery, her graft was well-maintained on the right eye. The patient's visual acuity was 0.3, and the corneal endothelial cell count was 1,844/mm².
CONCLUSIONS
Manual preparation of the donor corneal graft for DSEK is suitable as a second choice treatment method when the availability of surgical devices is limited.
Keyword
MeSH Terms
Figure
Reference
-
1. Melles GR, Eggink FA, Lander F, et al. A surgical technique for posterior lamellar keratoplasty. Cornea. 1998; 17:618–626.
Article2. Price FW Jr, Price MO. Descemet’s stripping with endothelial keratoplasty in 200 eyes: Early challenges and techniques to enhance donor adherence. J Cataract Refract Surg. 2006; 32:411–418.3. Gorovoy MS. Descemet-stripping automated endothelial keratoplasty. Cornea. 2006; 25:886–889.
Article4. Cheng YY, Pels E, Nuijts RM. Femtosecond-laser-assisted Descemet’s stripping endothelial keratoplasty. J Cataract Refract Surg. 2007; 33:152–155.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- A Case of Double Descemet's Membrane after Penetrating Keratoplasty Converted from Deep Anterior Lamellar Keratoplasty
- Descemet Membrane Endothelial Keratoplasty to Treat Graft Failure after Descemet Stripping Endothelial Keratoplasty
- The Correlations between Donor Endothelial Lenticule Thickness and Visual Prognosis in DSAEK
- Early Result of Femtosecond Laser Assisted Descemet's Membrane Stripping Endothelial Keratoplasty
- Effects of a Novel Push-through Technique Using the Implantable Collamer Lens Injector System for Graft Delivery during Endothelial Keratoplasty