J Korean Soc Spine Surg.
2019 Dec;26(4):166-171. 10.4184/jkss.2019.26.4.166.
Three-Column Fracture in the Thoracolumbar Junction Caused by Low-Energy Trauma in a Patient with Baastrup Disease: A Case Report
- Affiliations
-
- 1Department of Orthopedic Surgery, Inje University Seoul Paik Hospital, Seoul, Korea. hd1404@hanafos.com
- KMID: 2467946
- DOI: http://doi.org/10.4184/jkss.2019.26.4.166
Abstract
- STUDY DESIGN: Case report.
OBJECTIVES
We report a case of 3-column fracture caused by low-energy trauma in a patient with Baastrup disease who complained of acute radiating pain and motor weakness in the lower limbs after 3 weeks of conservative treatment. Subsequently, posterior fusion surgery was performed. SUMMARY OF LITERATURE REVIEW: Baastrup disease is characterized by enlargement and close approximation of adjacent spinous processes, and it mostly affects the L4-5 level of the spine. In patients with Baastrup disease affecting multiple levels of the lumbar spine, low-energy trauma can cause an unstable 3-column fracture with neurological compromise. Early recognition and surgical treatment prior to the emergence of a neurological deficit are required.
MATERIALS AND METHODS
An 84-year-old woman presented with back pain after falling down backward and colliding with the edge of a shelf at ground level. Considering the patient's general condition and age, she was initially treated with close observation and placement of a spinal brace with serial radiographic follow-up.
RESULTS
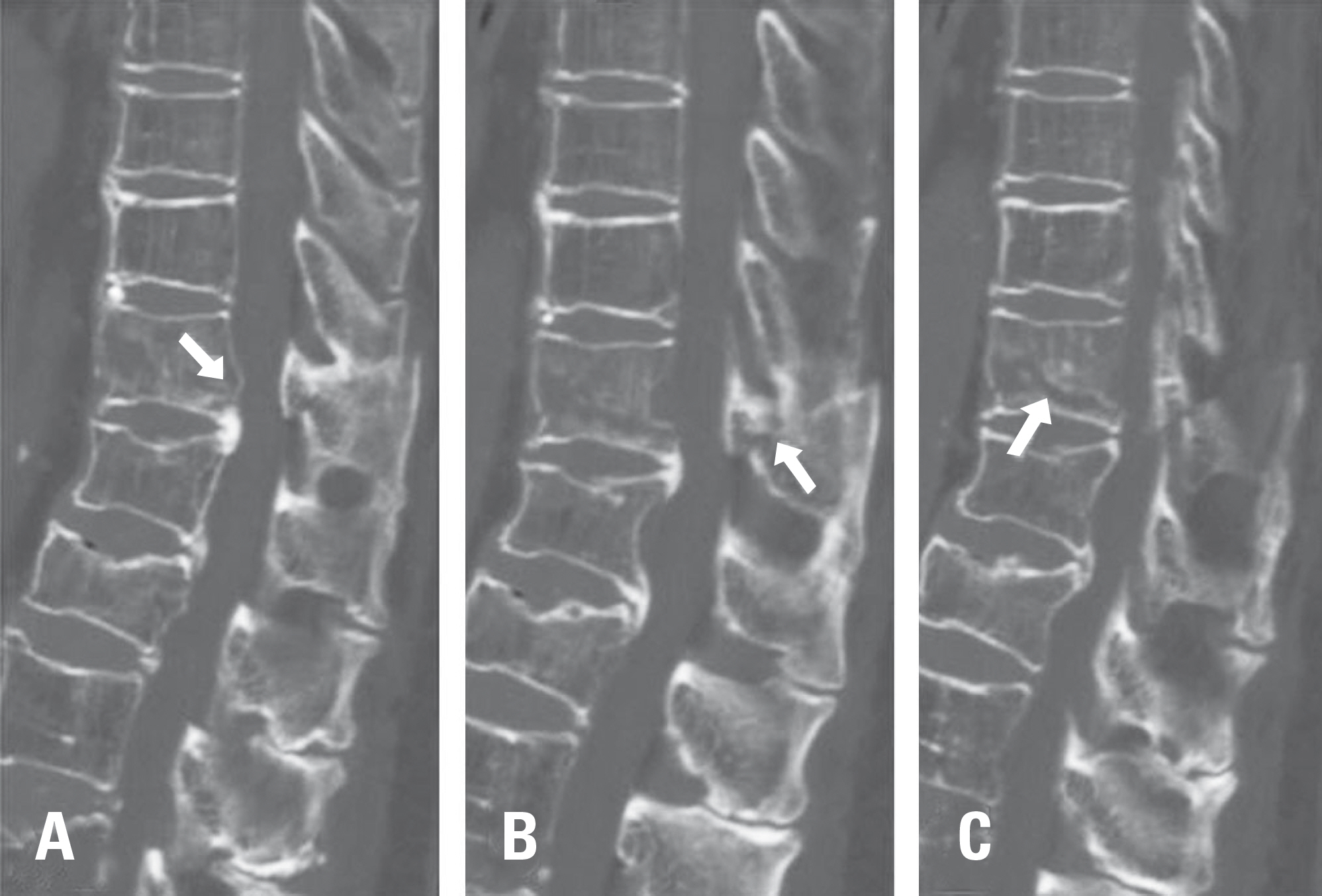
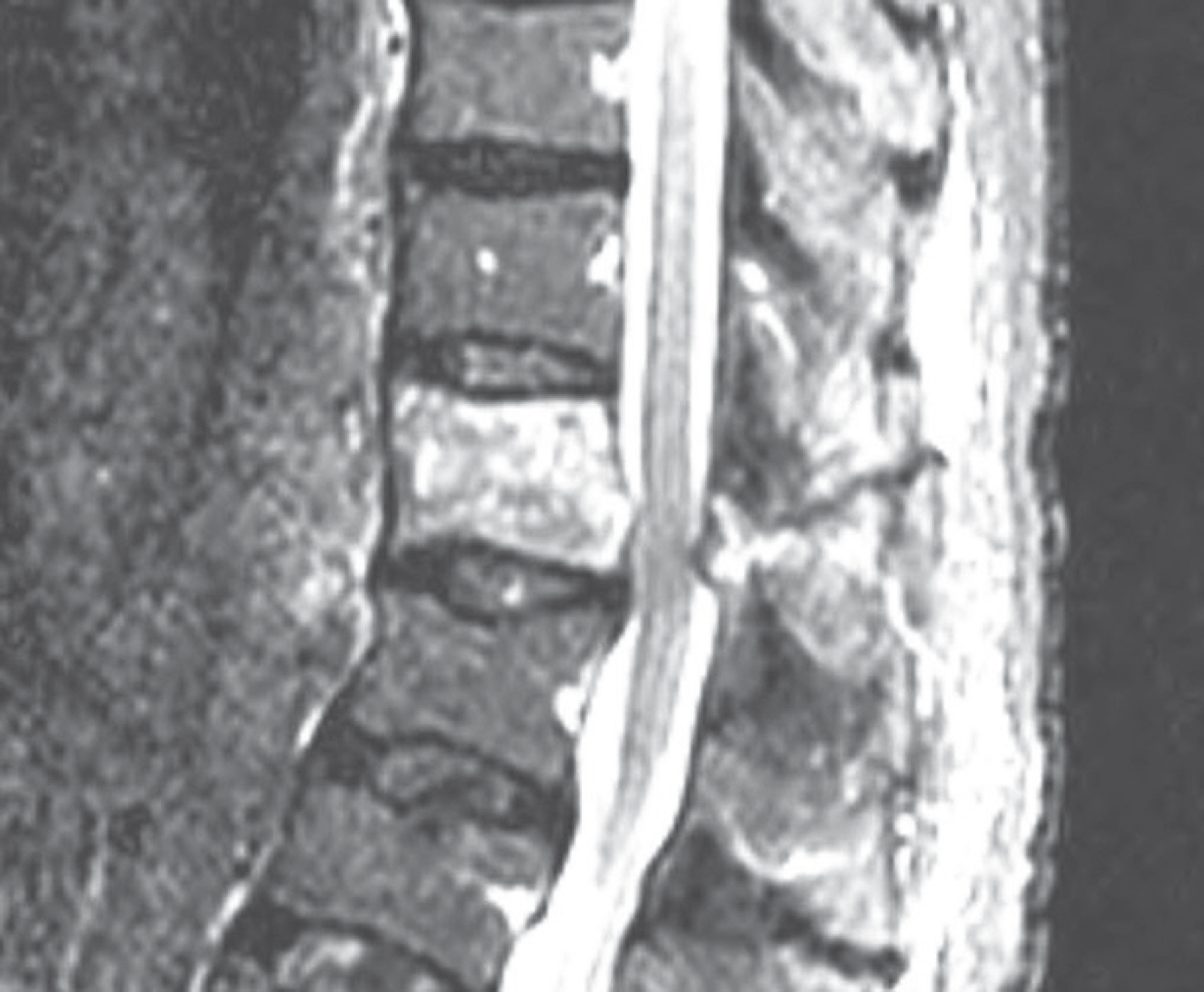
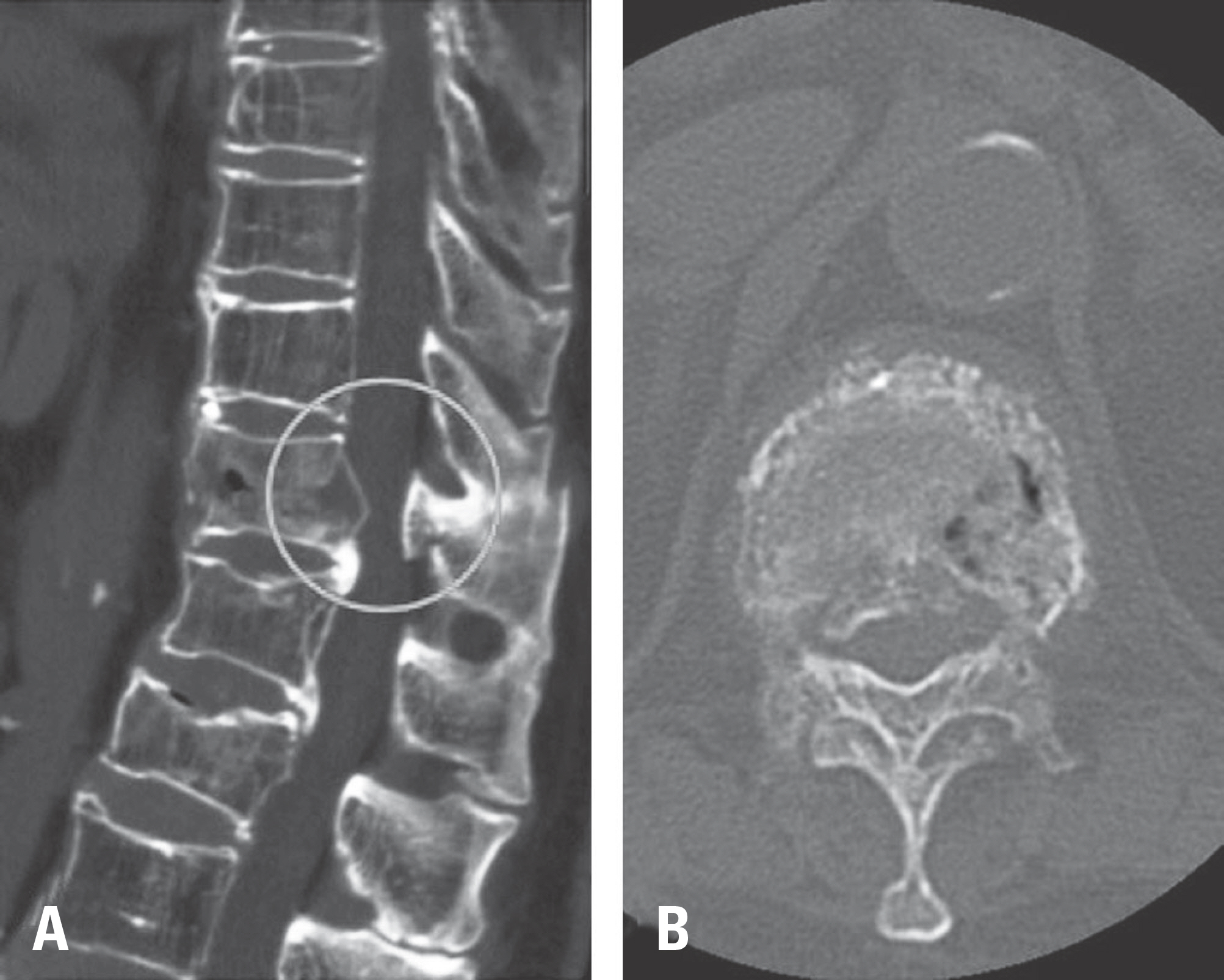
Computed tomography found 3-column fracture at the T11 level, which is quite rare in cases of minor trauma. At a 3-week follow-up, she complained of gradual lower extremity weakness, and her general lower extremity motor function decreased to grade 1-2. The patient underwent posterior fusion 2 levels above and below the affected vertebral body (T9-10-12-L1). Surgery was uneventful and the patient's motor function recovered.
CONCLUSIONS
In patients with Baastrup disease affecting multiple levels of the lumbar spine, based on our experience, low-energy trauma can cause an unstable 3-column fracture with neurological compromise. We highly recommend scrutiny of the interspinous space in elderly patients, especially those with a spinal fracture caused by low-energy trauma.
MeSH Terms
Figure
Reference
-
1. Bywaters EG, Evans S. The lumbar interspinous bursae and Baastrup's syndrome. An autopsy study. Rheumatol Int. 1982; 2(2):87–96.2. Kwong Y, Rao N, Latief K. MDCT findings in Baastrup disease: disease or normal feature of the aging spine? AJR Am J Roentgenol. 2011 May; 196(5):1156–9. DOI: 10.2214/AJR.10.5719.
Article3. Maes R, Morrison WB, Parker L, et al. Lumbar interspinous bursitis (Baastrup disease) in a symptomatic population: prevalence on magnetic resonance imaging. Spine (Phila Pa 1976). 2008 Apr 1; 33(7):E211–5. DOI: 10.1097/BRS.0b013e318169614a.4. Pinto PS, Boutin RD, Resnick D. Spinous process fractures associated with Baastrup disease. Clin Imaging. 2004 May-Jun; 28(3):219–22. DOI: 10.1016/S0899-7071 (03)00156-6.
Article5. Alonso F, Bryant E, Iwanaga J, et al. Baastrup's Disease: A Comprehensive Review of the Extant Literature. World Neurosurg. 2017 May; 101:331–4. DOI: 10.1016/j.wneu.2017.02.004.
Article6. Beks JW. Kissing spines: fact or fancy? Acta Neurochir (Wien). 1989; 100(3-4):134–5.
Article7. Jacobson HG, Tausend ME, Shapiro JH, et al. The sway-back syndrome. Am J Roentgenol Radium Ther Nucl Med. 1958 Apr; 79(4):677–83.8. Baastrup CI. On the Spinous Processes of the Lumbar Vertebrae and the Soft Tissues Between them, and on Pathological Changes in that Region. Acta Radiologica. 1933; 14(1):52–5. DOI: 10.3109/00016923309132353.
Article9. Rustagi T, Drazin D, Oner C, et al. Fractures in Spinal Ankylosing Disorders: A Narrative Review of Disease and Injury Types, Treatment Techniques, and Outcomes. J Orthop Trauma. 2017 Sep; 31(Suppl 4):S57–s74. DOI: 10.1097/bot.0000000000000953.
Article10. Mata S, Fortin PR, Fitzcharles MA, et al. A controlled study of diffuse idiopathic skeletal hyperostosis. Clinical features and functional status. Medicine (Baltimore). 1997 Mar; 76(2):104–17. DOI: 10.1097/00005792-199703000-00003.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- One Stage Three Column Fixation by Posterior Approach in Thoracolumbar Junction Lesion
- Pain Around the Posterior Iliac Crest of Thoracolumbar Origin
- Long Term Follow-up of the Stable Fractures Around Thoracolumbar Spinal Junction (Conservative Management vs. Operative Intervention)
- Relationship between Simple X-ray and CT Findings on the Degree of Canal Encroachment in Burst Fracture of Thoracolumbar Junction
- Mechanisms and Classifications of Thoracolumbar Fractures