Cancer Res Treat.
2017 Apr;49(2):518-525. 10.4143/crt.2016.299.
Magnetic Resonance Imaging–Detected Intracranial Extension in the T4 Classification Nasopharyngeal Carcinoma with Intensity-Modulated Radiotherapy
- Affiliations
-
- 1Department of Radiation Oncology, Cancer Hospital, Chinese Academy of Medical Sciences, Peking Union Medical College, Beijing, China. jingweiluo2013@163.com
- 2Department of Radiation Oncology, Zhejiang Cancer Hospital, Hangzhou, China.
- 3Zhejiang Key Laboratory of Radiation Oncology, Hangzhou, China.
- KMID: 2378125
- DOI: http://doi.org/10.4143/crt.2016.299
Abstract
- PURPOSE
This study was conducted is to identify the prognostic value and staging categories of magnetic resonance imaging (MRI)-detected intracranial extension in nasopharyngeal carcinoma (NPC) with intensity-modulated radiotherapy (IMRT) to determine whether it is necessary to subclassify the T4 classification NPC.
MATERIALS AND METHODS
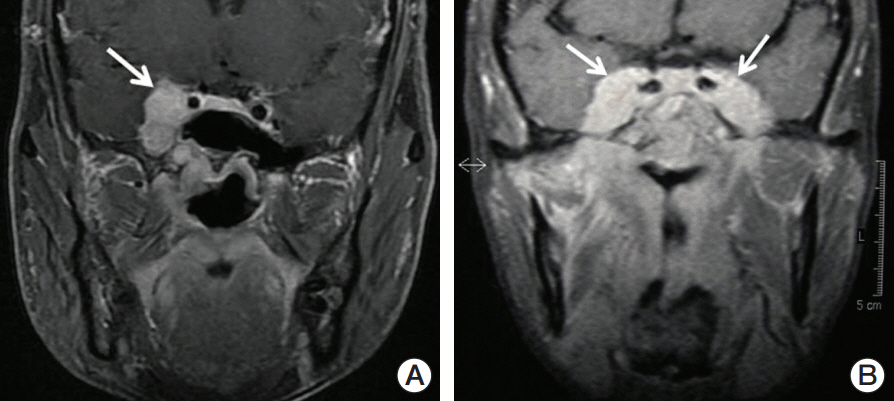
A total of 335 nonmetastatic T4 classification NPC patients with MRI treated between March 2004 and June 2011 by radical IMRT were included. The T4 classification patients were subclassified into two grades (T4a, without intracranial extension vs. T4b, with intracranial extension) according to the site of invasion.
RESULTS
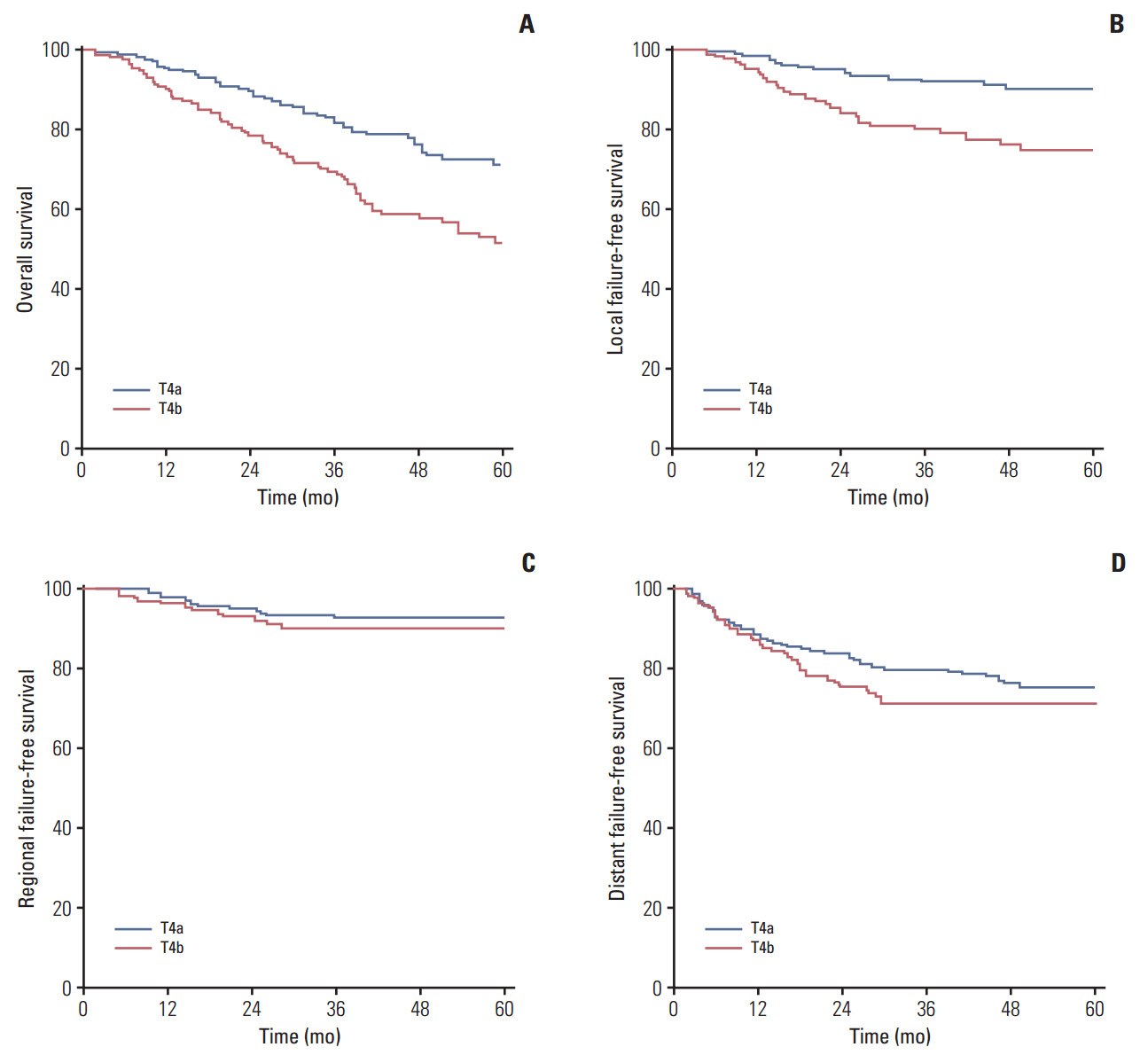
The frequency of intracranial extension was 40.9% (137 of 335 patients). Multivariate analysis identified subclassification (T4a vs. T4b) as an independent prognostic factor for local failure-free survival (p=0.049; hazard ratio [HR], 0.498) and overall survival (p=0.004; HR, 0.572); however, it had no effect on regional failure-free survival or distant failure-free survival (p > 0.050).
CONCLUSION
For patients with T4 classification NPC, those with MRI-detected intracranial extension are more likely to experience local failure and death after IMRT than patients without intracranial extension. According to the site of invasion, subclassification of T4 patients as T4a or T4b has prognostic value in NPC.
Keyword
MeSH Terms
Figure
Reference
-
References
1. Lee AW, Ma BB, Ng WT, Chan AT. Management of nasopharyngeal carcinoma: current practice and future perspective. J Clin Oncol. 2015; 33:3356–64.
Article2. Ng WT, Yuen KT, Au KH, Chan OS, Lee AW. Staging of nasopharyngeal carcinoma: the past, the present and the future. Oral Oncol. 2014; 50:549–54.3. Edge SB, Compton CC. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol. 2010; 17:1471–4.
Article4. Chen L, Liu LZ, Chen M, Li WF, Yin WJ, Lin AH, et al. Prognostic value of subclassification using MRI in the t4 classification nasopharyngeal carcinoma intensity-modulated radiotherapy treatment. Int J Radiat Oncol Biol Phys. 2012; 84:196–202.
Article5. Lee AW, Ng WT, Chan LL, Hung WM, Chan CC, Sze HC, et al. Evolution of treatment for nasopharyngeal cancer: success and setback in the intensity-modulated radiotherapy era. Radiother Oncol. 2014; 110:377–84.6. Cao CN, Luo JW, Gao L, Yi JL, Huang XD, Wang K, et al. Clinical outcomes and patterns of failure after intensity-modulated radiotherapy for T4 nasopharyngeal carcinoma. Oral Oncol. 2013; 49:175–81.
Article7. Chong VF, Fan YF, Khoo JB. Nasopharyngeal carcinoma with intracranial spread: CT and MR characteristics. J Comput Assist Tomogr. 1996; 20:563–9.
Article8. Cao CN, Luo JW, Gao L, Yi JL, Huang XD, Wang K, et al. Update report of T4 classification nasopharyngeal carcinoma after intensity-modulated radiotherapy: an analysis of survival and treatment toxicities. Oral Oncol. 2015; 51:190–4.
Article9. Huang XD, Yi JL, Gao L, Xu GZ, Jin J, Yang WZ, et al. Multicenter phase II clinical trial of humanized anti-epidermal factor receptor monoclonal antibody h-R3 combined with radiotherapy for locoregionally advanced nasopharyngeal carcinoma. Zhonghua Zhong Liu Za Zhi. 2007; 29:197–201.10. Hu YC, Chang CH, Chen CH, Ger LP, Liu WS, Lin LC, et al. Impact of intracranial extension on survival in stage IV nasopharyngeal carcinoma: identification of a subset of patients with better prognosis. Jpn J Clin Oncol. 2011; 41:95–102.
Article11. Groome PA, Schulze K, Boysen M, Hall SF, Mackillop WJ. A comparison of published head and neck stage groupings in carcinomas of the oral cavity. Head Neck. 2001; 23:613–24.
Article12. Sun X, Su S, Chen C, Han F, Zhao C, Xiao W, et al. Long-term outcomes of intensity-modulated radiotherapy for 868 patients with nasopharyngeal carcinoma: an analysis of survival and treatment toxicities. Radiother Oncol. 2014; 110:398–403.
Article13. Lin S, Pan J, Han L, Guo Q, Hu C, Zong J, et al. Update report of nasopharyngeal carcinoma treated with reduced-volume intensity-modulated radiation therapy and hypothesis of the optimal margin. Radiother Oncol. 2014; 110:385–9.
Article14. Ng WT, Lee MC, Hung WM, Choi CW, Lee KC, Chan OS, et al. Clinical outcomes and patterns of failure after intensity-modulated radiotherapy for nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2011; 79:420–8.
Article15. Dinshaw KA, Agarwal JP, Ghosh-Laskar S, Gupta T, Shrivastava SK. Radical radiotherapy in head and neck squamous cell carcinoma: an analysis of prognostic and therapeutic factors. Clin Oncol (R Coll Radiol). 2006; 18:383–9.
Article16. Liu L, Liang S, Li L, Mao Y, Tang L, Tian L, et al. Prognostic impact of magnetic resonance imaging-detected cranial nerve involvement in nasopharyngeal carcinoma. Cancer. 2009; 115:1995–2003.
Article17. Cheng SH, Tsai SY, Yen KL, Jian JJ, Feng AC, Chan KY, et al. Prognostic significance of parapharyngeal space venous plexus and marrow involvement: potential landmarks of dissemination for stage I-III nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys. 2005; 61:456–65.
Article18. Hung TM, Chen CC, Lin CY, Ng SH, Kang CJ, Huang SF, et al. Prognostic value of prepontine cistern invasion in nasopharyngeal carcinoma treated by intensity-modulated radiotherapy. Oral Oncol. 2014; 50:228–33.
Article19. Loong HH, Chan AT. Controversies in the systemic treatment of nasopharyngeal carcinoma. Oral Oncol. 2014; 50:785–90.
Article20. Baujat B, Audry H, Bourhis J, Chan AT, Onat H, Chua DT, et al. Chemotherapy in locally advanced nasopharyngeal carcinoma: an individual patient data meta-analysis of eight randomized trials and 1753 patients. Int J Radiat Oncol Biol Phys. 2006; 64:47–56.
Article21. Langendijk JA, Leemans CR, Buter J, Berkhof J, Slotman BJ. The additional value of chemotherapy to radiotherapy in locally advanced nasopharyngeal carcinoma: a meta-analysis of the published literature. J Clin Oncol. 2004; 22:4604–12.
Article22. Blanchard P, Lee A, Marguet S, Leclercq J, Ng WT, Ma J, et al. Chemotherapy and radiotherapy in nasopharyngeal carcinoma: an update of the MAC-NPC meta-analysis. Lancet Oncol. 2015; 16:645–55.
Article23. Niu X, Chang X, Gao Y, Hu C, Kong L. Using neoadjuvant chemotherapy and replanning intensity-modulated radiotherapy for nasopharyngeal carcinoma with intracranial invasion to protect critical normal tissue. Radiat Oncol. 2013; 8:226.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Prognostic Value and Staging Classification of Lymph Nodal Necrosis in Nasopharyngeal Carcinoma after Intensity-Modulated Radiotherapy
- Paranasal Sinus Invasion in Nasopharyngeal Carcinoma after Intensity-Modulated Radiotherapy
- Longitudinal Assessment of Intravoxel Incoherent Motion Diffusion Weighted Imaging in Evaluating the Radio-sensitivity of Nasopharyngeal Carcinoma Treated with Intensity-Modulated Radiation Therapy
- Is the Use of Intensity-Modulated Radiotherapy Beneficial for Pancreatic Cancer Patients?
- A Case of Nasopharyngeal Angiofibroma with Intracranial Extension Occurred in Female