J Korean Med Sci.
2012 Jun;27(6):668-673. 10.3346/jkms.2012.27.6.668.
Magnetoencephalography in Pediatric Lesional Epilepsy Surgery
- Affiliations
-
- 1Department of Pediatrics, Seoul National University Bundang Hospital, Seongnam, Korea. neuroandy@snubh.org
- 2Department of Pediatrics, Seoul National University Children's Hospital, Seoul National University College of Medicine, Seoul, Korea.
- 3Pediatric Clinical Neuroscience Center, Seoul National University Children's Hospital, Seoul National University College of Medicine, Seoul, Korea.
- 4MEG Center, Seoul National University Hospital, Seoul, Korea.
- 5Department of Neurosurgery, Seoul National University Hospital, Seoul National University College of Medicine, Seoul, Korea.
- KMID: 1421620
- DOI: http://doi.org/10.3346/jkms.2012.27.6.668
Abstract
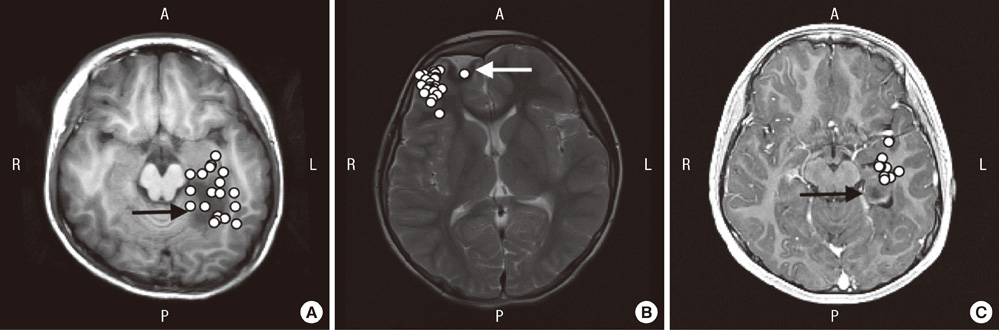
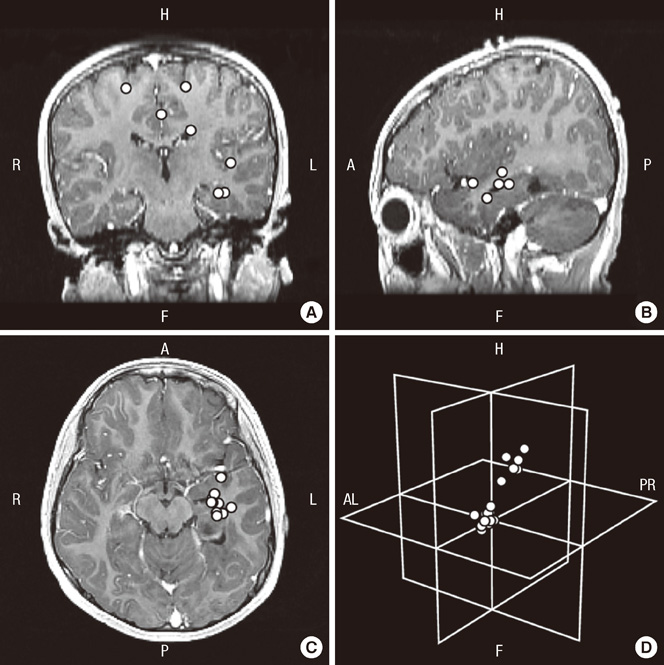
- This study was performed to assess the usefulness of magnetoencephalography (MEG) as a presurgical evaluation modality in Korean pediatric patients with lesional localization-related epilepsy. The medical records and MEG findings of 13 pediatric patients (6 boys and 7 girls) with localization-related epilepsy, who underwent epilepsy surgery at Seoul National University Children's Hospital, were retrospectively reviewed. The hemispheric concordance rate was 100% (13/13 patients). The lobar or regional concordance rate was 77% (10/13 patients). In most cases, the MEG spike sources were clustered in the proximity of the lesion, either at one side of the margin (nine patients) or around the lesion (one patient); clustered spike sources were distant from the lesion in one patient. Among the patients with clustered spike sources near the lesion, further extensions (three patients) and distal scatters (three patients) were also observed. MEG spike sources were well lateralized and localized even in two patients without focal epileptiform discharges in the interictal scalp electroencephalography. Ten patients (77%) achieved Engel class I postsurgical seizure outcome. It is suggested that MEG is a safe and useful presurgical evaluation modality in pediatric patients with lesion localization-related epilepsy.
Keyword
MeSH Terms
-
Adolescent
Brain/radionuclide imaging
Brain Diseases/pathology
Child
Child, Preschool
Epilepsies, Partial/pathology/*surgery
Female
Ganglioglioma/pathology
Humans
Infant
Magnetic Resonance Imaging
*Magnetoencephalography
Male
Malformations of Cortical Development/pathology
Neoplasms, Neuroepithelial/pathology
Positron-Emission Tomography
Retrospective Studies
Seizures/diagnosis
Figure
Reference
-
1. Cohen D. Magnetoencephalography: evidence of magnetic fields produced by alpha-rhythm currents. Science. 1968. 161:784–786.2. Ricci GB, Romani GL, Salustri C, Pizzella V, Torrioli G, Buonomo S, Peresson M, Modena I. Study of focal epilepsy by multichannel neuromagnetic measurements. Electroencephalogr Clin Neurophysiol. 1987. 66:358–368.3. Gallen CC, Hirschkoff EC, Buchanan DS. Magnetoencephalography and magnetic source imaging. Capabilities and limitations. Neuroimaging Clin N Am. 1995. 5:227–249.4. Stefan H, Hummel C, Scheler G, Genow A, Druschky K, Tilz C, Kaltenhäuser M, Hopfengärtner R, Buchfelder M, Romstöck J. Magnetic brain source imaging of focal epileptic activity: a synopsis of 455 cases. Brain. 2003. 126:2396–2405.5. Knowlton RC, Laxer KD, Aminoff MJ, Roberts TP, Wong ST, Rowley HA. Magnetoencephalography in partial epilepsy: clinical yield and localization accuracy. Ann Neurol. 1997. 42:622–631.6. Pataraia E, Simos PG, Castillo EM, Billingsley RL, Sarkari S, Wheless JW, Maggio V, Maggio W, Baumgartner JE, Swank PR, et al. Does magnetoencephalography add to scalp video-EEG as a diagnostic tool in epilepsy surgery? Neurology. 2004. 62:943–948.7. Paulini A, Fischer M, Rampp S, Scheler G, Hopfengärtner R, Kaltenhäuser M, Dörfler A, Buchfelder M, Stefan H. Lobar localization information in epilepsy patients: MEG - a useful tool in routine presurgical diagnosis. Epilepsy Res. 2007. 76:124–130.8. Bast T. Wyllie E, Cascino G, Gidal B, editors. Magnetoencephalography. Wyllie's treatment of epilepsy: principles and practice. 2011. Philadelphia: Lippincott Williams & Wilkins;869–875.9. Commission on Classification and Terminology of the International League Against Epilepsy. Proposal for revised clinical and electroencephalographic classification of epileptic seizures. Epilepsia. 1981. 22:489–501.10. Blume WT, Lüders HO, Mizrahi E, Tassinari C, van Emde Boas W, Engel J Jr. Glossary of descriptive terminology for ictal semiology: report of the ILAE task force on classification and terminology. Epilepsia. 2001. 42:1212–1218.11. Engel J Jr, VanNess P, Rasmussen T, Ojemann L. Engel J, editor. Outcome with respect to epileptic seizures. Surgical treatment of the epilepsies. 1993. 2nd ed. New York: Raven Press;609–621.12. Ochi A, Otsubo H, Iida K, Oishi M, Elliott I, Weiss SK, Kutomi T, Nakayama T, Sharma R, Chuang SH, et al. Identifying the primary epileptogenic hemisphere from electroencephalographic (EEG) and magnetoencephalographic dipole lateralizations in children with intractable epilepsy. J Child Neurol. 2005. 20:885–892.13. Otsubo H, Ochi A, Elliott I, Chuang SH, Rutka JT, Jay V, Aung M, Sobel DF, Snead OC. MEG predicts epileptic zone in lesional extrahippocampal epilepsy: 12 pediatric surgery cases. Epilepsia. 2001. 42:1523–1530.14. Minassian BA, Otsubo H, Weiss S, Elliott I, Rutka JT, Snead OC 3rd. Magnetoencephalographic localization in pediatric epilepsy surgery: comparison with invasive intracranial electroencephalography. Ann Neurol. 1999. 46:627–633.15. Knowlton RC, Elgavish RA, Limdi N, Bartolucci A, Ojha B, Blount J, Burneo JG, Ver Hoef L, Paige L, Faught E, et al. Functional imaging: I. Relative predictive value of intracranial electroencephalography. Ann Neurol. 2008. 64:25–34.16. Sutherling WW, Mamelak AN, Thyerlei D, Maleeva T, Minazad Y, Philpott L, Lopez N. Influence of magnetic source imaging for planning intracranial EEG in epilepsy. Neurology. 2008. 71:990–996.17. Funke M, Constantino T, Van Orman C, Rodin E. Magnetoencephalography and magnetic source imaging in epilepsy. Clin EEG Neurosci. 2009. 40:271–280.18. Seo JH, Holland K, Rose D, Rozhkov L, Fujiwara H, Byars A, Arthur T, DeGrauw T, Leach JL, Gelfand MJ, et al. Multimodality imaging in the surgical treatment of children with nonlesional epilepsy. Neurology. 2011. 76:41–48.19. Bast T, Oezkan O, Rona S, Stippich C, Seitz A, Rupp A, Fauser S, Zentner J, Rating D, Scherg M. EEG and MEG source analysis of single and averaged interictal spikes reveals intrinsic epileptogenicity in focal cortical dysplasia. Epilepsia. 2004. 45:621–631.20. Iida K, Otsubo H, Matsumoto Y, Ochi A, Oishi M, Holowka S, Pang E, Elliott I, Weiss SK, Chuang SH, et al. Characterizing magnetic spike sources by using magnetoencephalography-guided neuronavigation in epilepsy surgery in pediatric patients. J Neurosurg. 2005. 102:187–196.21. Oishi M, Kameyama S, Masuda H, Tohyama J, Kanazawa O, Sasagawa M, Otsubo H. Single and multiple clusters of magnetoencephalographic dipoles in neocortical epilepsy: significance in characterizing epileptogenic zone. Epilepsia. 2006. 47:355–364.22. RamachandranNair R, Otsubo H, Shroff MM, Ochi A, Weiss SK, Rutka JT, Snead OC 3rd. MEG predicts outcome following surgery for intractable epilepsy in children with normal or nonfocal MRI findings. Epilepsia. 2007. 48:149–157.