Korean J Radiol.
2000 Jun;1(2):65-72. 10.3348/kjr.2000.1.2.65.
Percutaneous Placement of Self-expandable Metallic Biliary Stents in Malignant Extrahepatic Strictures: Indications of Transpapillary and Suprapapillary Methods
- Affiliations
-
- 1Department of Radiology, Yong-dong Severance Hospital, Yonsei University College of Medicine, Seoul, Korea. stent@medikorea.net
- KMID: 966475
- DOI: http://doi.org/10.3348/kjr.2000.1.2.65
Abstract
OBJECTIVE
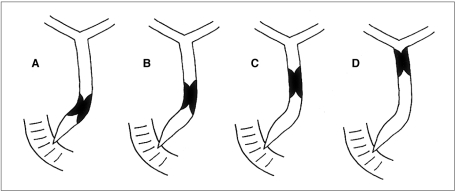
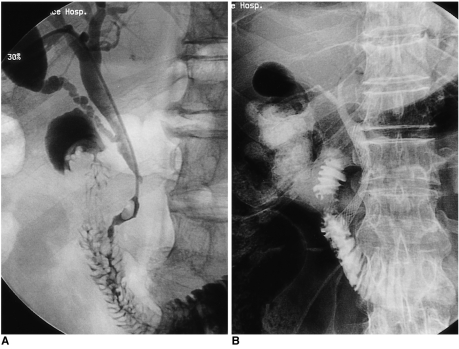
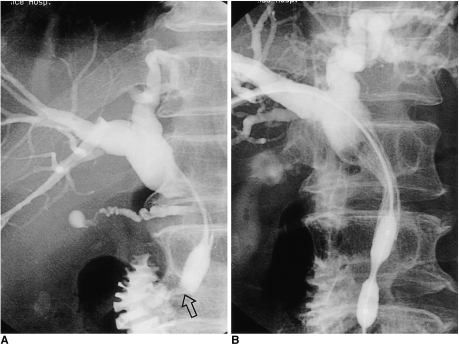
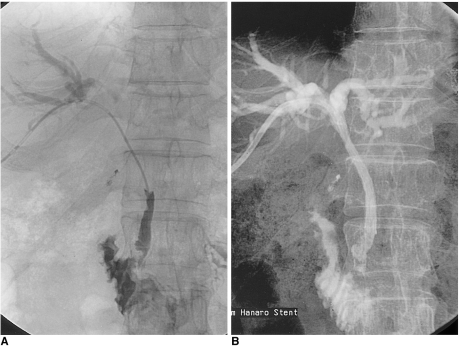
To compare the efficacy of suprapapillary and transpapillary meth-ods of transhepatic biliary metallic stent placement in malignant biliary strictures and to specify the indications of each method applied. MATERIALS AND METHODS: Stents were placed in 59 patients. Strictures were cat-egorized as type A (within 3 cm of the ampulla, n = 27), type B (over 3 cm from ampulla, n = 7), type C (within 3 cm of the bending portion, n = 9), or type D (over 3 cm above the bending portion, n=16). The stenting method was suprapapillary in 34 cases and transpapillary in 25. The rates of initial and long-term patency and of early recurrence were compared. RESULTS: Initial patency rates for the suprapapillary and transpapillary methods were 1/7 (14.3%) and 20/20 (100%) respectively for type A (p < 0.0001), 4/5 (80.0%) and 2/2 for type B, 3/7 (42.9%) and 2/2 for type C, and 15/16 (93.8%) and 0/0 for type D. Early recurrence rates were 7/30 (23.3%) using the suprapap-illary method and 4/29 (13.8%) using the transpapillary method (p = 0.51). The long-term patency rate did not differ significantly according to either type (p =0.37) or method (p = 0.62). CONCLUSION: For good initial patency, the transpapillary method is recommended for strictures of the distal extrahepatic duct near the ampulla and just above the bending portion. Long-term patency is not influenced by the stenting method employed.
Keyword
MeSH Terms
Figure
Reference
-
1. Wilson MW. The application of metallic stents in malignant biliary obstruction. Tech in vasc Intervent Radiol. 1999; 2:39–52.
Article2. Gordon RL, Ring EJ, LaBerge JM, Doherty MM. Malignant biliary obstruction: treatment with expandable metallic stents-follow up of 50 consecutive patients. Radiology. 1992; 182:697–701. PMID: 1371362.3. Lee BH, Choe DH, Lee JH, Kim KH, Chin SY. Metallic stents in malignant biliary obstruction: prospective long-term clinical results. AJR. 1997; 168:741–745. PMID: 9057527.
Article4. Lameris JS, Stocker J, Nijs HG, et al. Malignant biliary obstruction: percutaneous use of self-expandable stents. Radiology. 1991; 179:703–707. PMID: 2027978.
Article5. Becker CD, Glattli A, Maibach R, Baer HU. Percutaneous palliation of malignant obstructive jaundice with the Wallstent endoprosthesis: follow-up and reintervention in patients with hilar and non-hilar obstruction. J Vasc Intervent Radiol. 1993; 4:597–604.
Article6. Lee MJ, Dawson SL, Mueller PR, et al. Percutaneous management of hilar biliary malignancies with metallic endoprostheses: results, technical problems, and causes of failure. RadioGraphics. 1993; 13:1249–1263. PMID: 8290722.
Article7. Lee BH, Do YS, Byun HS, Kim KH, Jin SY. Metallic stents for management of malignant biliary obstruction. J Korean Radiol Soc. 1992; 28:959–967.
Article8. Murphy BL, Mueller PR. Metallic biliary stents: technical points on optimizing results. Semin Intervent Radiol. 1996; 13:55–67.
Article9. Liu Q, Khay G, Cotton B. Feasibility of stent placement above the sphincter of Oddi ("Inside-Stent") for patients with malignant biliary obstruction. Endoscopy. 1998; 30:687–690. PMID: 9865557.
Article10. Stoker J, Lameris JS. Complications of percutaneously inserted biliary Wallstents. J Vasc Intervent Radiol. 1993; 4:767–772.
Article11. Dawson SL, Lee MJ, Mueller PR. Metal endoprostheses in malignant biliary obstruction. Semin Intervent Radiol. 1991; 8:242–251.
Article12. Roebuck DJ, Stanley P, Katz MD, Parry RL, Haight MA. Gastrointestinal hemorrhage due to duodenal erosion by a biliary Wallstent. Cardiovasc Intervent Radiol. 1998; 21:63–65. PMID: 9473549.
Article13. Van Steenbergen W, Van Aken L, Ponette E. Acute pancreatitis complicating the insertion of a self-expandable biliary metal stent. Endoscopy. 1992; 24:440–442. PMID: 1505495.
Article14. Yarze JC, Poulos AM, Fritz HP, Herlihy KJ. Treatment of metallic biliary stent-induced duodenal ulceration using endoscopic laser therapy. Dig Dis Sci. 1997; 42:6–9. PMID: 9009109.15. Ee H, Laurence BH. Haemorrhage due to erosion of a metal biliary stent through the duodenal wall. Endoscopy. 1992; 24:431–432. PMID: 1505493.
Article16. Bismuth H. Blumgast LH, editor. Postoperative strictures of the bile duct. The biliary tract. 1982. Edinburgh: Churchill Livingstone;p. 207–218.17. Lee BH, Do YS, Lee JH, Kim KH, Chin SY. New self-expandable spiral metallic stent: preliminary clinical evaluation in malignant biliary obstruction. J Vasc Intervent Radiol. 1995; 6:635–640.
Article18. Lindner HH. Clinical anatomy. 1989. Connecticut: Appleton & Lange;p. 418–422.19. Huibregtse K. The Wallstent for malignant biliary obstruction. Gastrointest Endosc Clin North Am. 1999; 9:491–501.
Article20. Lee BH, Kim KH, Chin SY. Mechanical characteristics of self-expandable metallic stents: in vitro study with three types of stresses. J Korean Radiol Soc. 1998; 39:497–502.21. Roh HG, Kang SG, Cho YK, et al. Physical property and MR imaging of self-expandable metallic stents. J Korean Radiol Soc. 1998; 39:503–509.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Prophylactic endoscopic transpapillary gallbladder stenting to prevent acute cholecystitis induced after metallic stent placement for malignant biliary strictures: a retrospective study in Japan
- Current Status of Biliary Metal Stents
- Percutaneous placement of self-expandable metallic stents in patients with obstructive jaundice due to hepatocellular carcinoma
- Biliary Endoprosthese by the Use of Expandable Metallic Stents
- Complex percutaneous biliary procedures: Review and contributions of a high volume team