J Rhinol.
2023 Nov;30(3):173-176. 10.18787/jr.2023.00032.
A Case of Extramedullary Plasmacytoma in Both Maxillary Sinuses
- Affiliations
-
- 1Department of Otorhinolaryngology and Biomedical Research Institute, Pusan National University School of Medicine, Pusan National University Hospital, Busan, Republic of Korea
- 2Department of Pathology, Pusan National University School of Medicine, Pusan National University Hospital, Busan, Republic of Korea
- KMID: 2548196
- DOI: http://doi.org/10.18787/jr.2023.00032
Abstract
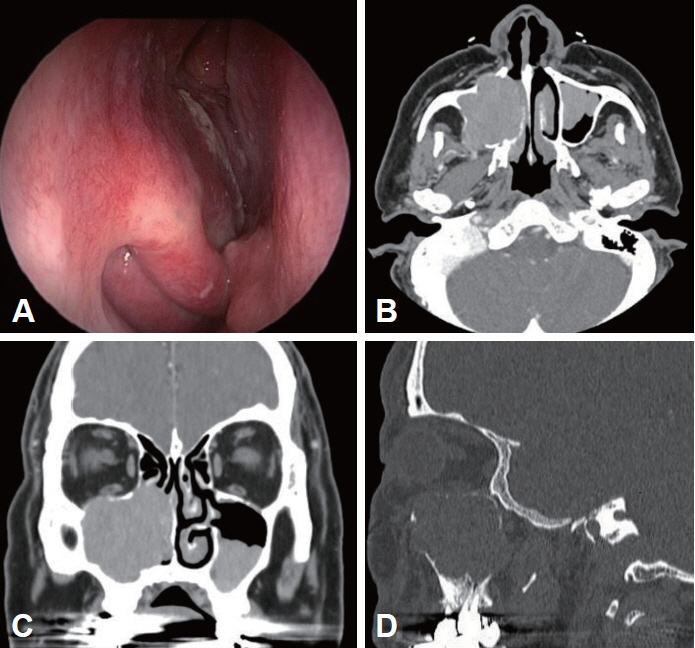
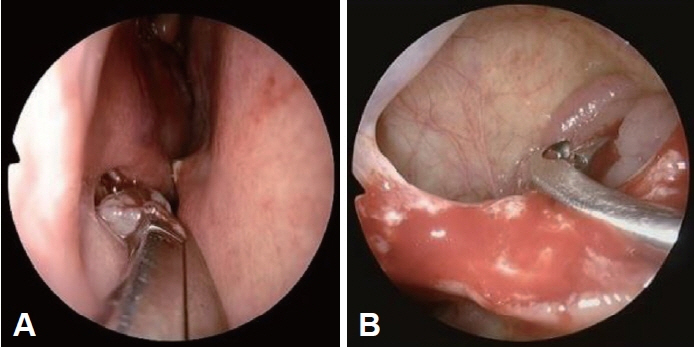
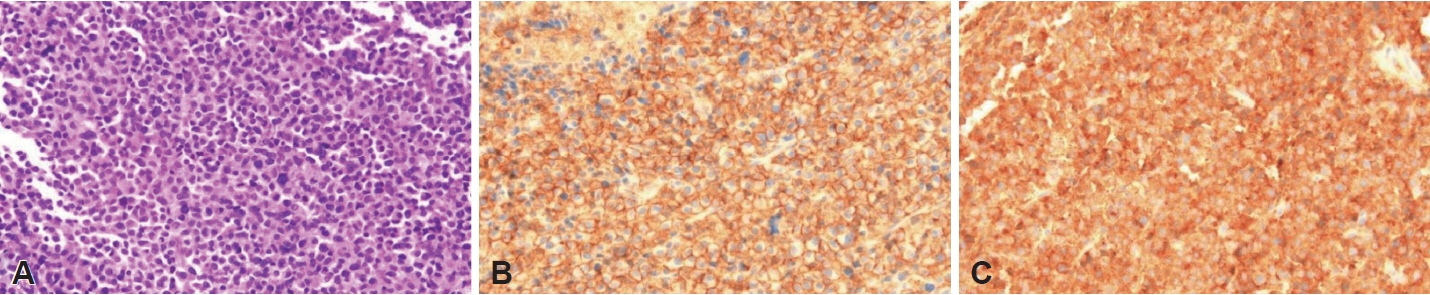
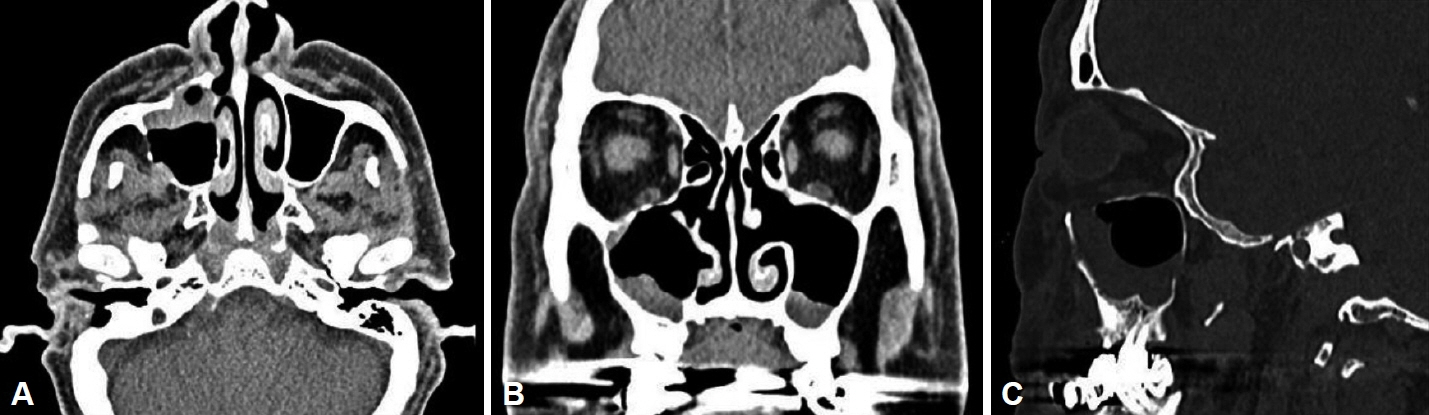
- Plasmacytoma is a rare hematolymphoid malignancy. The three types of plasmacytoma, according to clinical features and morphological characteristics, include solitary bone plasmacytoma, extramedullary plasmacytoma (EMP), and multiple myeloma (MM). Although EMP of the head and neck region accounts for approximately 3% of all plasma cell tumors, the involvement of both paranasal sinuses is extremely rare. Herein, we describe a rare case of EMP involving both maxillary sinuses in a 73-year-old male patient who had achieved complete remission from MM following chemotherapy 2 years ago. The EMP was treated successfully with radiotherapy.
Figure
Reference
-
References
1. Batsakis JG, Medeiros JL, Luna MA, El-Naggar AK. Plasma cell dyscrasias and the head and neck. Ann Diagn Pathol. 2002; 6(2):129–40.2. Köse M, Buraniqi E, Akpinar TS, Kayacan SM, Tükek T. Relapse of multiple myeloma presenting as extramedullary plasmacytomas in multiple organs. Case Rep Hematol. 2015; 2015:452305.
Article3. Weinstock M, Ghobrial IM. Extramedullary multiple myeloma. Leuk Lymphoma. 2013; 54(6):1135–41.
Article4. Bansal R, Rakshit S, Kumar S. Extramedullary disease in multiple myeloma. Blood Cancer J. 2021; 11(9):161.
Article5. Kyle RA, Rajkumar SV. Multiple myeloma. N Engl J Med. 2004; 351(18):1860–73.
Article6. Firsova MV, Mendeleeva LP, Kovrigina AM, Solovev MV, Savchenko VG. Plasmacytoma in patients with multiple myeloma: morphology and immunohistochemistry. BMC Cancer. 2020; 20(1):346.
Article7. Ching AS, Khoo JB, Chong VF. CT and MR imaging of solitary extramedullary plasmacytoma of the nasal tract. AJNR Am J Neuroradiol. 2002; 23(10):1632–6.8. Lee DJ, Hong SD, Yu MS, Heo SJ, Kim JY, Jung TY, et al. Differential diagnosis of sinonasal extramedullary plasmacytoma, non-Hodgkin’s lymphoma, and squamous cell carcinoma using CT scan and MRI. Iran J Radiol. 2021; 18(2):e111764.
Article9. Hsi ED, Yegappan S. Lymphoma immunophenotyping: a new era in paraffin-section immunohistochemistry. Adv Anat Pathol. 2001; 8(4):218–39.
Article10. Bayer-Garner IB, Prieto VG, Smoller BR. Detection of clonality with kappa and lambda immunohistochemical analysis in cutaneous plasmacytomas. Arch Pathol Lab Med. 2004; 128(6):645–8.11. Lee JH, Kim SH. Treatment of relapsed and refractory multiple myeloma. Blood Res. 2020; 55(S1):S43–53.
Article12. Barlogie B, Anaissie E, van Rhee F, Shaughnessy JD Jr, Szymonifka J, Hoering A, et al. Reiterative survival analyses of total therapy 2 for multiple myeloma elucidate follow-up time dependency of prognostic variables and treatment arms. J Clin Oncol. 2010; 28(18):3023–7.
Article13. Bladé J, Beksac M, Caers J, Jurczyszyn A, von Lilienfeld-Toal M, Moreau P, et al. Extramedullary disease in multiple myeloma: a systematic literature review. Blood Cancer J. 2022; 12(3):45.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- A Case of Extramedullary Plasmacytoma of the Hypopharynx
- Extramedullary Plasmacytoma of the Frontal Sinus
- A Case of Multiple Extramedullary Plasmacytoma Arising from Both Nasal Cavity and Nasopharynx
- A Case of Extramedullary Plasmacytoma of the Larynx
- Extramedullary Plasmacytoma of the Gallbladder: A Case Report