Anesth Pain Med.
2023 Jan;18(1):57-64. 10.17085/apm.22207.
Herpes zoster after COVID-19 vaccination, aspect of pain medicine: a retrospective, single-center study
- Affiliations
-
- 1Department of Anesthesiology and Pain Medicine, Presbyterian Medical Center, Jeonju, Korea
- KMID: 2540335
- DOI: http://doi.org/10.17085/apm.22207
Abstract
- Background
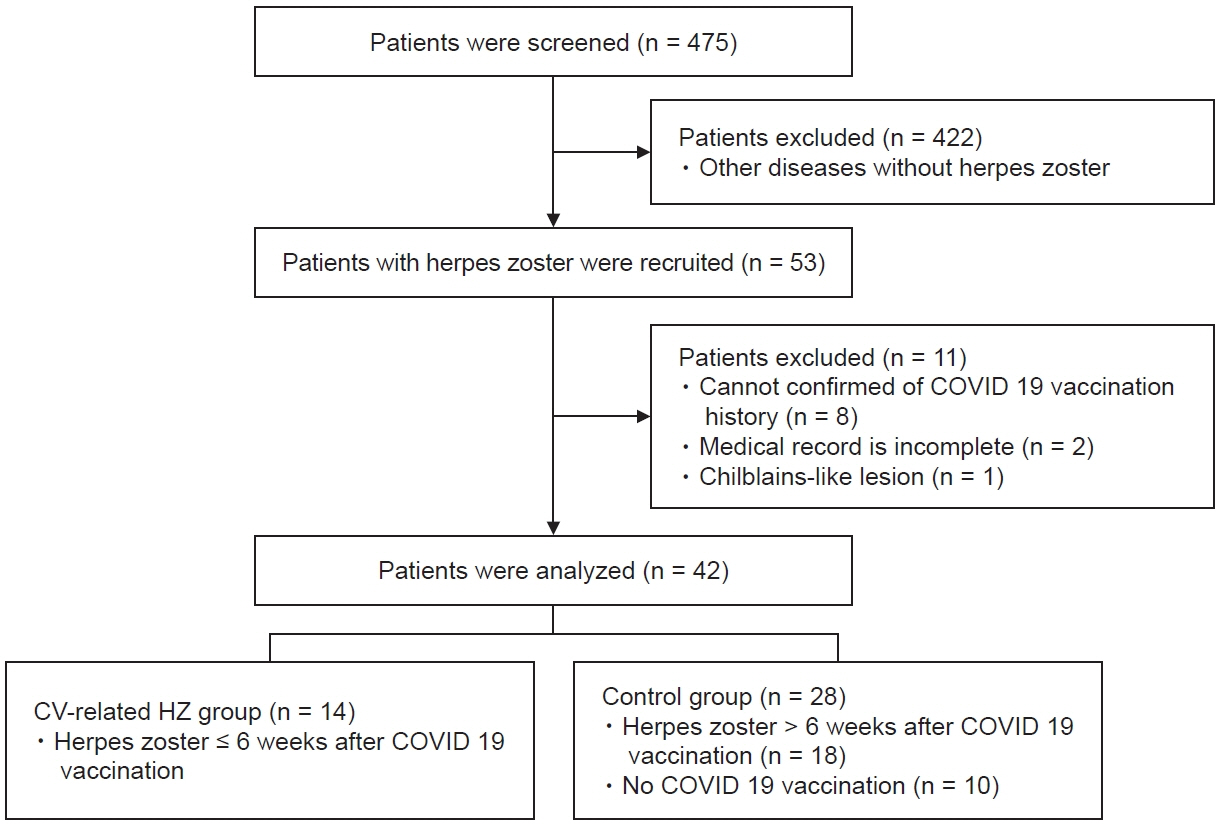
Herpes zoster (HZ) is one of the most common cutaneous adverse reactionsassociated with the coronavirus disease 2019 (COVID-19) vaccine and has been widely reported. This study aimed to evaluate HZ following COVID-19 vaccination from the viewpointof pain management.Methods: A retrospective study was conducted on 42 patients with HZ who visited the painclinic between August 2021 and October 2021. Medical records were reviewed to comparepain severity, treatment methods, treatment duration, and incidence rate of postherpeticneuralgia (PHN) in patients who received COVID-19 vaccination within 6 weeks prior to developing symptoms compared with other patients with HZ.Results: Fourteen patients developed HZ within 6 weeks after vaccination and were significantly younger than the other HZ groups. There were no significant differences in the frequency of prodromal pain, location of pain, pain severity, treatment methods, treatmentduration, or incidence of PHN compared with the other HZ groups.Conclusions: COVID-19 vaccination-related HZ showed clinical features similar to those ofthe other HZ.
Figure
Cited by 1 articles
-
Enhancing global recognition: our journey towards Emerging Sources Citation Index indexing
Min Kyoung Kim, Hyun Kang
Anesth Pain Med. 2024;19(4):267-268. doi: 10.17085/apm.24128.
Reference
-
1. Barda N, Dagan N, Ben-Shlomo Y, Kepten E, Waxman J, Ohana R, et al. Safety of the BNT162b2 mRNA Covid-19 vaccine in a nationwide setting. N Engl J Med. 2021; 385:1078–90.
Article2. Beatty AL, Peyser ND, Butcher XE, Cocohoba JM, Lin F, Olgin JE, et al. Analysis of COVID-19 vaccine type and adverse effects following vaccination. JAMA Netw Open. 2021; 4:e2140364.
Article3. Song JY, Cheong HJ, Kim SR, Lee SE, Kim SH, Noh JY, et al. Early safety monitoring of COVID-19 vaccines in healthcare workers. J Korean Med Sci. 2021; 36:e110.
Article4. Patone M, Mei XW, Handunnetthi L, Dixon S, Zaccardi F, Shankar-Hari M, et al. Risks of myocarditis, pericarditis, and cardiac arrhythmias associated with COVID-19 vaccination or SARS-CoV-2 infection. Nat Med. 2022; 28:410–22.
Article5. Garg RK, Paliwal VK. Spectrum of neurological complications following COVID-19 vaccination. Neurol Sci. 2022; 43:3–40.
Article6. Woo EJ, Mba-Jonas A, Dimova RB, Alimchandani M, Zinderman CE, Nair N. Association of receipt of the Ad26.COV2.S COVID-19 vaccine with presumptive Guillain-Barré syndrome, February-July 2021. JAMA. 2021; 326:1606–13.
Article7. Klein NP, Lewis N, Goddard K, Fireman B, Zerbo O, Hanson KE, et al. Surveillance for adverse events after COVID-19 mRNA vaccination. JAMA. 2021; 326:1390–9.
Article8. Bostan E, Yalici-Armagan B. Herpes zoster following inactivated COVID-19 vaccine: a coexistence or coincidence? J Cosmet Dermatol. 2021; 20:1566–7.
Article9. Furer V, Zisman D, Kibari A, Rimar D, Paran Y, Elkayam O. Herpes zoster following BNT162b2 mRNA COVID-19 vaccination in patients with autoimmune inflammatory rheumatic diseases: a case series. Rheumatology (Oxford). 2021; 60(SI):SI90–5.
Article10. Park JH, Lee JH, Oh JY, Heo HJ, Jung DW, Cho HG. Herpes zoster as a sequelae of various kinds of COVID-19 vaccination: a case series. Int J Pain. 2021; 12:19–23.
Article11. Psichogiou M, Samarkos M, Mikos N, Hatzakis A. Reactivation of varicella zoster virus after vaccination for SARS-CoV-2. Vaccines (Basel). 2021; 9:572.
Article12. Gringeri M, Battini V, Cammarata G, Mosini G, Guarnieri G, Leoni C, et al. Herpes zoster and simplex reactivation following COVID-19 vaccination: new insights from a vaccine adverse event reporting system (VAERS) database analysis. Expert Rev Vaccines. 2022; 21:675–84.
Article13. van Oorschot D, Vroling H, Bunge E, Diaz-Decaro J, Curran D, Yawn B. A systematic literature review of herpes zoster incidence worldwide. Hum Vaccin Immunother. 2021; 17:1714–32.
Article14. Gershon AA, Gershon MD, Breuer J, Levin MJ, Oaklander AL, Griffiths PD. Advances in the understanding of the pathogenesis and epidemiology of herpes zoster. J Clin Virol. 2010; 48(Suppl 1):S2–7.
Article15. Katsikas Triantafyllidis K, Giannos P, Mian IT, Kyrtsonis G, Kechagias KS. Varicella zoster virus reactivation following COVID-19 vaccination: a systematic review of case reports. Vaccines (Basel). 2021; 9:1013.
Article16. Rodríguez-Jiménez P, Chicharro P, Cabrera LM, Seguí M, Morales-Caballero Á, Llamas-Velasco M, et al. Varicella-zoster virus reactivation after SARS-CoV-2 BNT162b2 mRNA vaccination: report of 5 cases. JAAD Case Rep. 2021; 12:58–9.
Article17. Desai HD, Sharma K, Shah A, Patoliya J, Patil A, Hooshanginezhad Z, et al. Can SARS-CoV-2 vaccine increase the risk of reactivation of Varicella zoster? A systematic review. J Cosmet Dermatol. 2021; 20:3350–61.
Article18. Johnson RW, Rice AS. Clinical practice. Postherpetic neuralgia. N Engl J Med. 2014; 371:1526–33.19. Tontodonati M, Ursini T, Polilli E, Vadini F, Di Masi F, Volpone D, et al. Post-herpetic neuralgia. Int J Gen Med. 2012; 5:861–71.20. Tartari F, Spadotto A, Zengarini C, Zanoni R, Guglielmo A, Adorno A, et al. Herpes zoster in COVID-19-positive patients. Int J Dermatol. 2020; 59:1028–9.
Article21. Maia CMF, Marques NP, de Lucena EHG, de Rezende LF, Martelli DRB, Martelli-Júnior H. Increased number of herpes zoster cases in Brazil related to the COVID-19 pandemic. Int J Infect Dis. 2021; 104:732–3.
Article22. Alhasawi A, Kamel MI, Elmasry S, Kamel WA, Hassan A. Impact of COVID-19 vaccination on varicella zoster virus reactivation: a case control study. Microbiol Infect Dis. 2021; 5:1–6.
Article23. Hertel M, Heiland M, Nahles S, von Laffert M, Mura C, Bourne PE, et al. Real-world evidence from over one million COVID-19 vaccinations is consistent with reactivation of the varicella-zoster virus. J Eur Acad Dermatol Venereol. 2022; 36:1342–8.24. Català A, Muñoz-Santos C, Galván-Casas C, Roncero Riesco M, Revilla Nebreda D, Solá-Truyols A, et al. Cutaneous reactions after SARS-CoV-2 vaccination: a cross-sectional Spanish nationwide study of 405 cases. Br J Dermatol. 2022; 186:142–52.
Article25. McMahon DE, Amerson E, Rosenbach M, Lipoff JB, Moustafa D, Tyagi A, et al. Cutaneous reactions reported after Moderna and Pfizer COVID-19 vaccination: a registry-based study of 414 cases. J Am Acad Dermatol. 2021; 85:46–55.
Article26. Drolet M, Brisson M, Levin MJ, Schmader KE, Oxman MN, Johnson RW, et al. A prospective study of the herpes zoster severity of illness. Clin J Pain. 2010; 26:656–66.
Article27. Lapolla W, Digiorgio C, Haitz K, Magel G, Mendoza N, Grady J, et al. Incidence of postherpetic neuralgia after combination treatment with gabapentin and valacyclovir in patients with acute herpes zoster: open-label study. Arch Dermatol. 2011; 147:901–7.
Article28. Patil SA, Dygert L, Galetta SL, Balcer LJ, Cohen EJ. Apparent lack of association of COVID-19 vaccination with herpes zoster. Am J Ophthalmol Case Rep. 2022; 26:101549.
Article29. Koumaki D, Krueger-Krasagakis SE, Papadakis M, Katoulis A, Koumaki V, Evangelou G, et al. Herpes zoster viral infection after AZD1222 and BNT162b2 coronavirus disease 2019 mRNA vaccines: a case series. J Eur Acad Dermatol Venereol. 2022; 36:e85–6.
Article30. Chu CW, Jiesisibieke ZL, Yang YP, Wu PC, Lin HL, Tung TH. Association of COVID-19 vaccination with herpes zoster: a systematic review and meta-analysis. Expert Rev Vaccines. 2022; 21:601–8.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Herpes zoster ophthalmicus after COVID-19 vaccine booster in healthy younger adult: a case report
- Two Cases of Herpes Zoster in healthy Children after Varicella Vaccination
- Herpes zoster vaccine in Korea
- A Case Report of Herpes Zoster Ophthalmicus and Meningitis After COVID-19 Vaccination
- A Case of Aphthous Stomatitis in a Healthy Adult Following COVID-19 Vaccination: Clinical Reasoning