Anesth Pain Med.
2021 Jul;16(3):279-283. 10.17085/apm.21006.
Liver transplantation of a patient with extreme thrombocytopenia - A case report -
- Affiliations
-
- 1Department of Anesthesiology and Pain Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea
- 2Department of Transplantation Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea
- KMID: 2519057
- DOI: http://doi.org/10.17085/apm.21006
Abstract
- Background
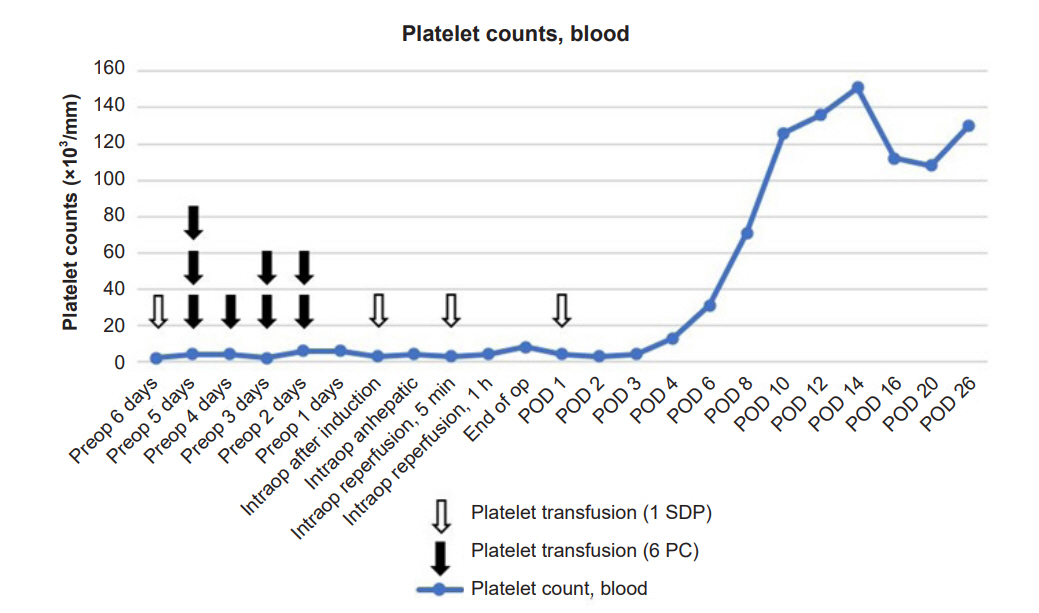
Patients with chronic liver disease (CLD) planned for liver transplantation (LT) often show severe thrombocytopenia, but there is a lack of evidence in deciding the threshold for prophylactic platelet transfusion. Case: A 47-year-old women with acute liver failure was referred for LT. Despite daily transfusion of platelets, platelet counts remained under 10,000/µl. During LT, 2 units of single donor platelets (SDP) were transfused. Although platelet counts remained extremely low (3,000–4,000/µl) no diffuse oozing was observed and the blood loss was 860 ml. Postoperatively, there was no sign of active bleeding or oozing, and the patient received only 1 unit SDP transfusion.
Conclusions
CLD patients may have severe thrombocytopenia. However, primary hemostasis may not be significantly hindered due to the existence of rebalanced hemostasis. Prophylactic platelet transfusion in these patients should not be decided based on platelet counts only, but also take other coagulation tests and clinical signs into consideration.
Figure
Reference
-
1. Giannini EG. Review article: thrombocytopenia in chronic liver disease and pharmacologic treatment options. Aliment Pharmacol Ther. 2006; 23:1055–65.2. Estcourt LJ, Birchall J, Allard S, Bassey SJ, Hersey P, Kerr JP, et al. British Committee for Standards in Haematology. Guidelines for the use of platelet transfusions. Br J Haematol. 2017; 176:365–94.3. Saab S, Brown RS Jr. Management of thrombocytopenia in patients with chronic liver disease. Dig Dis Sci. 2019; 64:2757–68.4. Bang SR, Ahn HJ, Kim GS, Yang M, Gwak MS, Ko JS, et al. Predictors of high intraoperative blood loss derived by simple and objective method in adult living donor liver transplantation. Transplant Proc. 2010; 42:4148–50.5. Han B, Lee SY, Kim GS. Anesthetic management of a chronic liver disease patient with very low platelet counts by considering a rebalanced hemostasis - a case report -. Anesth Pain Med. 2018; 13:419–22.6. Wu Z, Zhou J, Pankaj P, Peng B. Laparoscopic splenectomy for immune thrombocytopenia (ITP) patients with platelet counts lower than 1 × 109/L. Int J Hematol. 2011; 94:533–8.7. Aster RH. Pooling of platelets in the spleen: role in the pathogenesis of "hypersplenic" thrombocytopenia. J Clin Invest. 1966; 45:645–57.8. Afdhal N, McHutchison J, Brown R, Jacobson I, Manns M, Poordad F, et al. Thrombocytopenia associated with chronic liver disease. J Hepatol. 2008; 48:1000–7.9. Feys HB, Canciani MT, Peyvandi F, Deckmyn H, Vanhoorelbeke K, Mannucci PM. ADAMTS13 activity to antigen ratio in physiological and pathological conditions associated with an increased risk of thrombosis. Br J Haematol. 2007; 138:534–40.10. Potze W, Porte RJ, Lisman T. Management of coagulation abnormalities in liver disease. Expert Rev Gastroenterol Hepatol. 2015; 9:103–14.11. Chang FY, Singh N, Gayowski T, Wagener MM, Mietzner SM, Stout JE, et al. Thrombocytopenia in liver transplant recipients: predictors, impact on fungal infections, and role of endogenous thrombopoietin. Transplantation. 2000; 69:70–5.12. Witte M, Langnas AN, Hirst K, Stratta RJ, Shaw BW Jr. Impact of liver transplantation on the reversal of hypersplenism. Transplant Proc. 1993; 25:1987.13. Peck-Radosavljevic M. Thrombocytopenia in chronic liver disease. Liver Int. 2017; 37:778–93.14. Hirooka M, Ochi H, Hiraoka A, Koizumi Y, Tanaka T, Sunago K, et al. Role of severe thrombocytopenia in preventing platelet count recovery in thrombocytopenic patients with chronic liver disease. J Gastroenterol Hepatol. 2020; 35:299–304.15. Pereboom IT, de Boer MT, Haagsma EB, Hendriks HG, Lisman T, Porte RJ. Platelet transfusion during liver transplantation is associated with increased postoperative mortality due to acute lung injury. Anesth Analg. 2009; 108:1083–91.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Successful kidney transplantation from a live donor with immune thrombocytopenia: a case report
- Levodopa-induced Thrombocytopenia
- A case report of anesthesia management in the liver transplantation recipient with porphyria: A case report
- Liver transplantation for azithromycin-induced severe liver injury: a case report
- Total Hip Arthroplasty in Patient with Osteonecrosis of the Femoral Head Following Liver Transplantation: Case Report