Ann Rehabil Med.
2021 Feb;45(1):33-41. 10.5535/arm.20149.
Clinical Factors Associated With Successful Gastrostomy Tube Weaning in Patients With Prolonged Dysphagia After Stroke
- Affiliations
-
- 1Department of Physical Medicine and Rehabilitation, Kosin University College of Medicine, Busan, Korea
- KMID: 2513228
- DOI: http://doi.org/10.5535/arm.20149
Abstract
Objective
To investigate the clinical factors associated with successful gastrostomy tube weaning in patients with prolonged dysphagia after stroke.
Methods
This study involved a retrospective medical chart review of patients diagnosed with prolonged dysphagia after stroke who underwent gastrostomy tube insertion between May 2013 and January 2020. Forty-seven patients were enrolled and consequently divided into gastrostomy tube sustaining and weaning groups. The numbers of patients in the sustaining and weaning groups were 31 and 16, respectively. The patients’ demographic data, Korean version of Mini-Mental State Examination (K-MMSE) score, Korean version of the Modified Barthel Index (K-MBI), Functional Dysphagia Scale (FDS) score, and Penetration-Aspiration Scale (PAS) score were compared between the two groups. A videofluoroscopic swallowing study was performed before making the decision of gastrostomy tube weaning. The clinical factors associated with gastrostomy tube weaning were then investigated.
Results
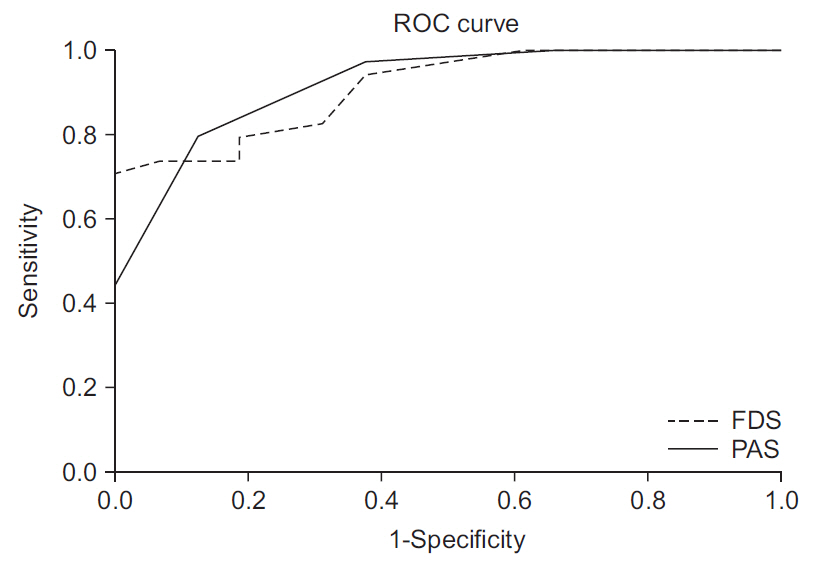
There were significant differences in age; history of aspiration pneumonia; K-MMSE, FDS, and PAS scores; and K-MBI between the groups. In the multiple logistic regression analysis, the FDS (odds ratio [OR]=0.791; 95% confidence interval [CI], 0.634–0.987) and PAS scores (OR=0.205; 95% CI, 0.059–0.718) were associated with successful gastrostomy tube weaning. In the receiver operating characteristic curve analysis, the FDS and PAS were useful screening tools for successful weaning, with areas under the curve of 0.911 and 0.918, respectively.
Conclusion
In patients with prolonged dysphagia, the FDS and PAS scores are the only factors associated with successful gastrostomy tube weaning. An evaluation of the swallowing function is necessary before deciding to initiate gastrostomy tube weaning.
Keyword
Figure
Reference
-
1. Gonzalez-Fernandez M, Ottenstein L, Atanelov L, Christian AB. Dysphagia after stroke: an overview. Curr Phys Med Rehabil Rep. 2013; 1:187–96.
Article2. Qureshi AZ, Jenkins RM, Thornhill TH. Percutaneous endoscopic gastrostomy versus nasogastric tube feeding during neurorehabilitation. Ifs, ands, or buts. Neurosciences (Riyadh). 2016; 21:69–71.
Article3. Rahnemai-Azar AA, Rahnemaiazar AA, Naghshizadian R, Kurtz A, Farkas DT. Percutaneous endoscopic gastrostomy: indications, technique, complications and management. World J Gastroenterol. 2014; 20:7739–51.
Article4. Park RH, Allison MC, Lang J, Spence E, Morris AJ, Danesh BJ, et al. Randomised comparison of percutaneous endoscopic gastrostomy and nasogastric tube feeding in patients with persisting neurological dysphagia. BMJ. 1992; 304:1406–9.
Article5. Kim CJ, Chun MH, Ha SB. Comparison of percutaneous endoscopic gastrostomy and nasogastric tube feeding in dysphagic stroke. J Korean Acad Rehabil Med. 1997; 21:1110–7.6. Yi Y, Yang EJ, Kim J, Kim WJ, Min Y, Paik NJ. Predictive factors for removal of percutaneous endoscopic gastrostomy tube in post-stroke dysphagia. J Rehabil Med. 2012; 44:922–5.
Article7. Ickenstein GW, Kelly PJ, Furie KL, Ambrosi D, Rallis N, Goldstein R, et al. Predictors of feeding gastrostomy tube removal in stroke patients with dysphagia. J Stroke Cerebrovasc Dis. 2003; 12:169–74.
Article8. Han TR, Paik NJ, Park JW. Quantifying swallowing function after stroke: a functional dysphagia scale based on videofluoroscopic studies. Arch Phys Med Rehabil. 2001; 82:677–82.
Article9. Rosenbek JC, Robbins JA, Roecker EB, Coyle JL, Wood JL. A penetration-aspiration scale. Dysphagia. 1996; 11:93–8.
Article10. Cohen DL, Roffe C, Beavan J, Blackett B, Fairfield CA, Hamdy S, et al. Post-stroke dysphagia: a review and design considerations for future trials. Int J Stroke. 2016; 11:399–411.
Article11. Han TR, Paik NJ, Park JW, Kwon BS. The prediction of persistent dysphagia beyond six months after stroke. Dysphagia. 2008; 23:59–64.
Article12. Butler SG, Markley L, Sanders B, Stuart A. Reliability of the penetration aspiration scale with flexible endoscopic evaluation of swallowing. Ann Otol Rhinol Laryngol. 2015; 124:480–3.
Article13. Lee JH, Kim SB, Lee KW, Lee SJ, Park JG, Ri JW. Associating factors regarding nasogastric tube removal in patients with Dysphagia after stroke. Ann Rehabil Med. 2014; 38:6–12.
Article14. Hwang JM, Cheong YS, Kang MG, Chun SM, Min YS, Lee YS, et al. Recommendation of nasogastric tube removal in acute stroke patients based on videofluoroscopic swallow study. Ann Rehabil Med. 2017; 41:9–15.
Article15. Broadley S, Croser D, Cottrell J, Creevy M, Teo E, Yiu D, et al. Predictors of prolonged dysphagia following acute stroke. J Clin Neurosci. 2003; 10:300–5.
Article16. Kumar S, Doughty C, Doros G, Selim M, Lahoti S, Gokhale S, et al. Recovery of swallowing after dysphagic stroke: an analysis of prognostic factors. J Stroke Cerebrovasc Dis. 2014; 23:56–62.
Article17. Daniels SK, Pathak S, Mukhi SV, Stach CB, Morgan RO, Anderson JA. The relationship between lesion localization and dysphagia in acute stroke. Dysphagia. 2017; 32:777–84.
Article18. Martino R, Foley N, Bhogal S, Diamant N, Speechley M, Teasell R. Dysphagia after stroke: incidence, diagnosis, and pulmonary complications. Stroke. 2005; 36:2756–63.19. Thornton FJ, Fotheringham T, Alexander M, Hardiman O, McGrath FP, Lee MJ. Amyotrophic lateral sclerosis: enteral nutrition provision. Endoscopic or radiologic gastrostomy? Radiology. 2002; 224:713–7.20. Galaski A, Peng WW, Ellis M, Darling P, Common A, Tucker E. Gastrostomy tube placement by radiological versus endoscopic methods in an acute care setting: a retrospective review of frequency, indications, complications and outcomes. Can J Gastroenterol. 2009; 23:109–14.
Article21. Oto T, Kandori Y, Ohta T, Domen K, Koyama T. Predicting the chance of weaning dysphagic stroke patients from enteral nutrition: a multivariate logistic modelling study. Eur J Phys Rehabil Med. 2009; 45:355–62.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Comparison of Percutaneous Endoscopic Gastrostomy and Nasogastric Tube Feeding in Dysphagic Stroke
- Selection of Enteral Feeding in Poststroke Dysphagia
- Prognostic Indicators in Dysphagia Recovery
- Gastroesophageal Reflux during Nasogastric Tube Feeding versus Oroesophageal Tube Feeding in Stroke Patients: A 24 Hour Esophageal pH-monitoring
- Conversion of Percutaneous Endoscopic Gastrostomy to Gastrojejunostomy Under Fluoroscopic Guidance for Treatment of Gastrocutaneous Fistula