Hip Pelvis.
2020 Mar;32(1):50-57. 10.5371/hp.2020.32.1.50.
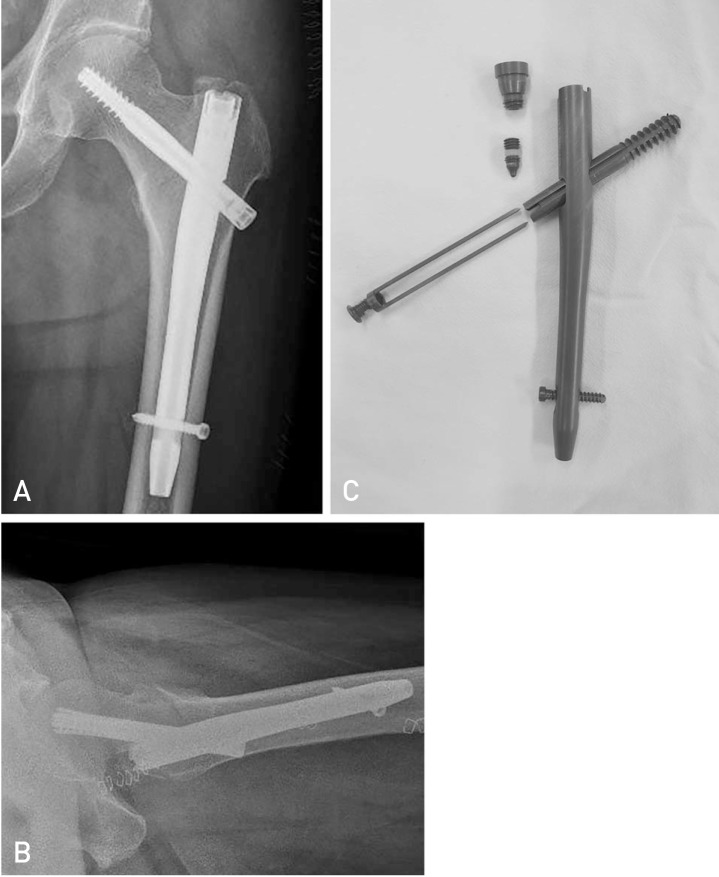
A Comparison of U-blade Gamma3 and Gamma3 Nails Used for the Treatment of Intertrochanteric Fractures
- Affiliations
-
- 1Department of Orthopedic Surgery, Seoul Medical Center, Seoul, Korea. hananina@seoulmc.or.kr
- 2Department of Orthopedic Surgery, Korea University Guro Hospital, Seoul, Korea.
- KMID: 2471131
- DOI: http://doi.org/10.5371/hp.2020.32.1.50
Abstract
- PURPOSE
To compare outcomes (i.e., clinical and radiological findings, postoperative complication) in the fixation of intertrochanteric fractures with U-blade Gamma3 and Gamma3 nails.
MATERIALS AND METHODS
A review of 162 patients (both male and female) treated for intertrochanteric fractures between December 2012 and December 2018 was conducted. All patients were older than 65 years of age and treated with U-blade Gamma3 (n=90) or Gamma3 (n=72) nails. Evaluations included: (i) screw-head position, (ii) fracture-reduction status, (iii) time to union, (iv) cases of cut-out, (v) tip-apex distance, and (vi) lag screw sliding distance. Differences in pre- and postoperative ambulatory ability was also investigated.
RESULTS
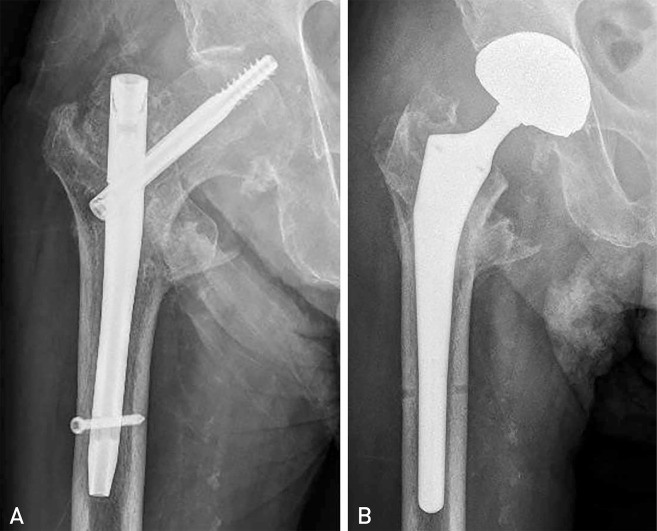
There were no significant differences in baseline demographics between the two groups. While the lag-screw sliding distance was significantly shorter in U-blade Gamma3 nail group (4.7 mm vs. 3.6 mm; P=0.025), the mean time to union was similar between the groups (P=0.053). Three and six cases of cut-out were noted in the U-blade Gamma3 and Gamma3 nail groups, respectively (P=0.18), however no other postoperative complications were noted in either group. Lastly, there was no difference between the change from pre- to postoperative activity level between the groups (P=0.753).
CONCLUSION
Of all the clinical and radiological outcomes assessed, the only significant improvement between those treated with U-Blade Gamma and Gamma3 nails was a shorter lag-screw sliding distance. These findings should benefit clinicians when deciding between the use of U-Blade Gamma or Gamma3 nails.
Keyword
Figure
Reference
-
1. Kyle RF, Cabanela ME, Russell TA, et al. Fractures of the proximal part of the femur. Instr Course Lect. 1995; 44:227–253. PMID: 7797861.
Article2. Lee YS, Huang HL, Lo TY, Huang CR. Dynamic hip screw in the treatment of intertrochanteric fractures: a comparison of two fixation methods. Int Orthop. 2007; 31:683–688. PMID: 17036223.
Article3. Ma KL, Wang X, Luan FJ, et al. Proximal femoral nails antirotation, Gamma nails, and dynamic hip screws for fixation of intertrochanteric fractures of femur: a meta-analysis. Orthop Traumatol Surg Res. 2014; 100:859–866. PMID: 25453927.
Article4. Niu E, Yang A, Harris AH, Bishop J. Which fixation device is preferred for surgical treatment of intertrochanteric hip fractures in the United States? A survey of orthopaedic surgeons. Clin Orthop Relat Res. 2015; 473:3647–3655. PMID: 26208608.
Article5. Dávid A, von der Heyde D, Pommer A. [Therapeutic possibilities in trochanteric fractures. Safe--fast--stable]. Orthopade. 2000; 29:294–301. German. PMID: 10851690.6. Friedl W, Clausen J. [Experimental examination for optimized stabilisation of trochanteric femur fractures, intra- or extramedullary implant localisation and influence of femur neck component profile on cut-out risk]. Chirurg. 2001; 72:1344–1352. German. PMID: 11766660.7. Kempf I, Grosse A, Taglang G, Favreul E. [Gamma nail in the treatment of closed trochanteric fractures. Results and indications apropos of 121 cases]. Rev Chir Orthop Reparatrice Appar Mot. 1993; 79:29–40. French. PMID: 8284466.8. Wu D, Ren G, Peng C, Zheng X, Mao F, Zhang Y. InterTan nail versus Gamma3 nail for intramedullary nailing of unstable trochanteric fractures. Diagn Pathol. 2014; 9:191. PMID: 25269555.
Article9. Yoo J, Kim S, Jung H, Hwang J. Clinical outcomes of U-blade Gamma3 nails used to treat patients with trochanteric fractures: retrospective multicenter study. Hip Pelvis. 2019; 31:95–101. PMID: 31198776.
Article10. Lenich A, Vester H, Nerlich M, Mayr E, Stöckle U, Füchtmeier B. Clinical comparison of the second and third generation of intramedullary devices for trochanteric fractures of the hip--Blade vs screw. Injury. 2010; 41:1292–1296. PMID: 20728885.
Article11. Lang NW, Arthold C, Joestl J, et al. Does an additional antirotation U-Blade (RC) lag screw improve treatment of AO/OTA 31 A1-3 fractures with gamma 3 nail? Injury. 2016; 47:2733–2738. PMID: 27832831.
Article12. Cleveland M, Bosworth DM, Thompson FR, Wilson HJ Jr, Ishizuka T. A ten-year analysis of intertrochanteric fractures of the femur. J Bone Joint Surg Am. 1959; 41:1399–1408. PMID: 13849408.
Article13. Baumgaertner MR, Curtin SL, Lindskog DM, Keggi JM. The value of the tip-apex distance in predicting failure of fixation of peritrochanteric fractures of the hip. J Bone Joint Surg Am. 1995; 77:1058–1064. PMID: 7608228.
Article14. Queally JM, Harris E, Handoll HH, Parker MJ. Intramedullary nails for extracapsular hip fractures in adults. Cochrane Database Syst Rev. 2014; (9):CD004961. PMID: 25212485.
Article15. Sommers MB, Roth C, Hall H, et al. A laboratory model to evaluate cutout resistance of implants for pertrochanteric fracture fixation. J Orthop Trauma. 2004; 18:361–368. PMID: 15213501.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Comparison of the U-Blade Gamma3 Nail and the Zimmer Natural Nail for the Treatment of Intertrochanteric Fracture
- Clinical Outcomes of U-blade Gamma3 Nails Used to Treat Patients with Trochanteric Fractures: Retrospective Multicenter Study
- Helical Blade versus Lag Screw for Treatment of Intertrochanteric Fracture
- Blade Plate Fixation for Failed Internal Fixation of Intertrochanteric Hip fractures
- Excessive Sliding of the Helical Blade and the Femoral Neck Fracture after Insertion of Proximal Femoral Nail Anti-Rotation for Type A2 Intertrochanteric Fractures - A Case Report -