J Korean Ophthalmol Soc.
2015 Apr;56(4):638-642. 10.3341/jkos.2015.56.4.638.
A Case of Malignant Glaucoma in a Vitrectomized Eye
- Affiliations
-
- 1HanGil Eye Hospital, Incheon, Korea. eyecjy@hanmail.net
- KMID: 2215719
- DOI: http://doi.org/10.3341/jkos.2015.56.4.638
Abstract
- PURPOSE
To report a case of malignant glaucoma in an eye vitrectomized 5 years previously due to endophthalmitis.
CASE SUMMARY
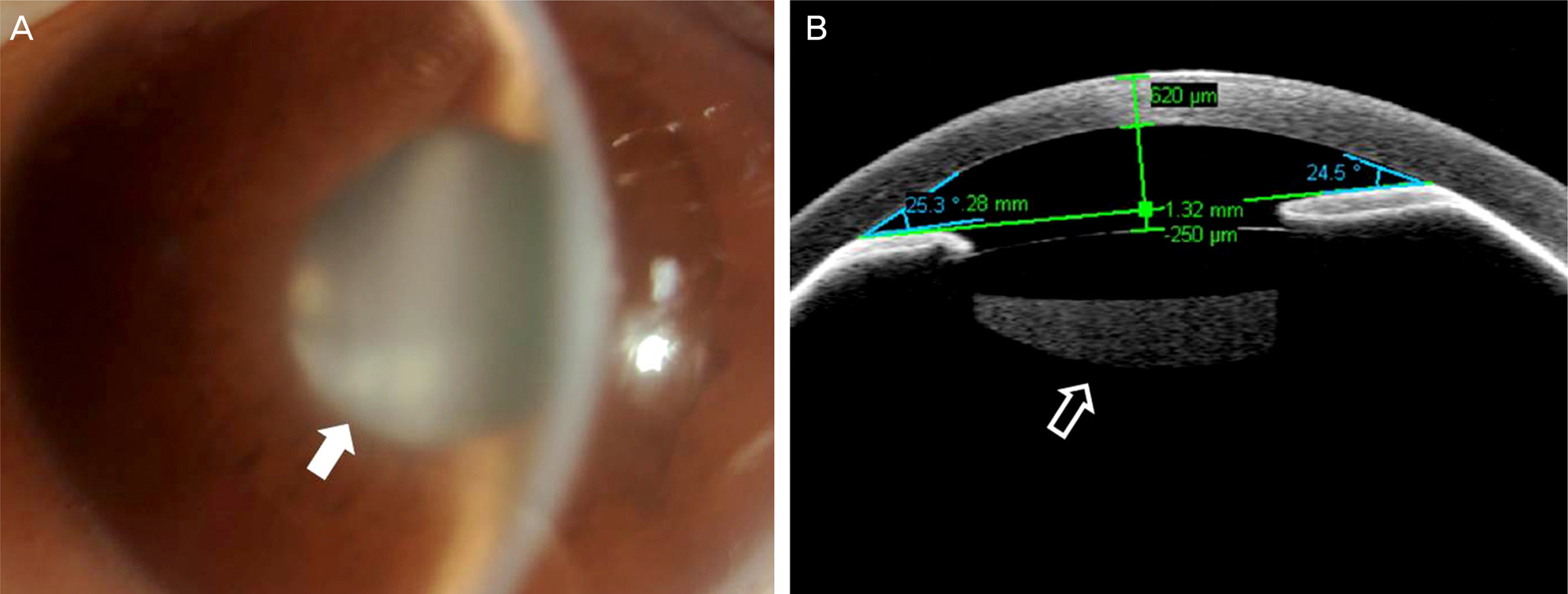
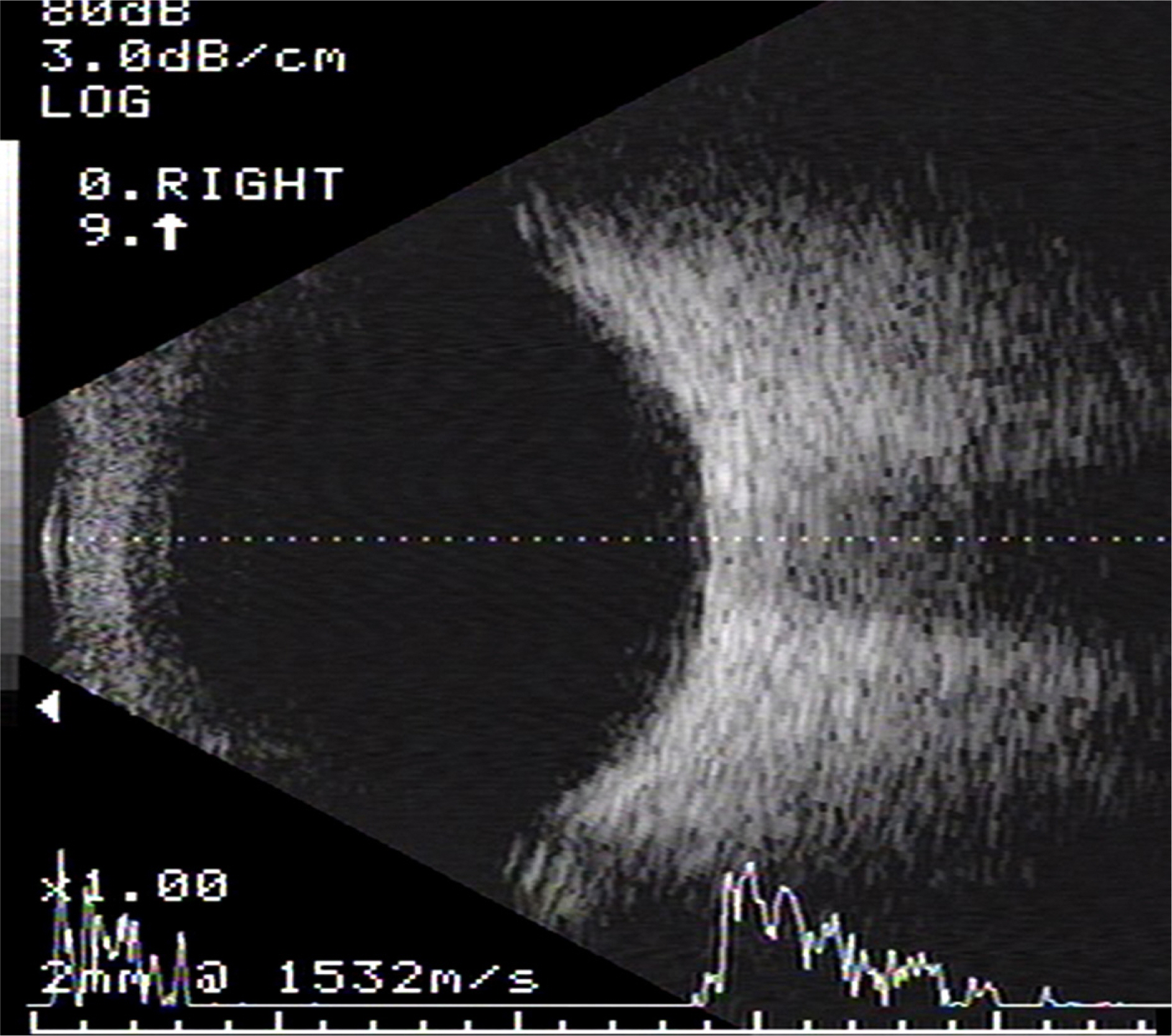
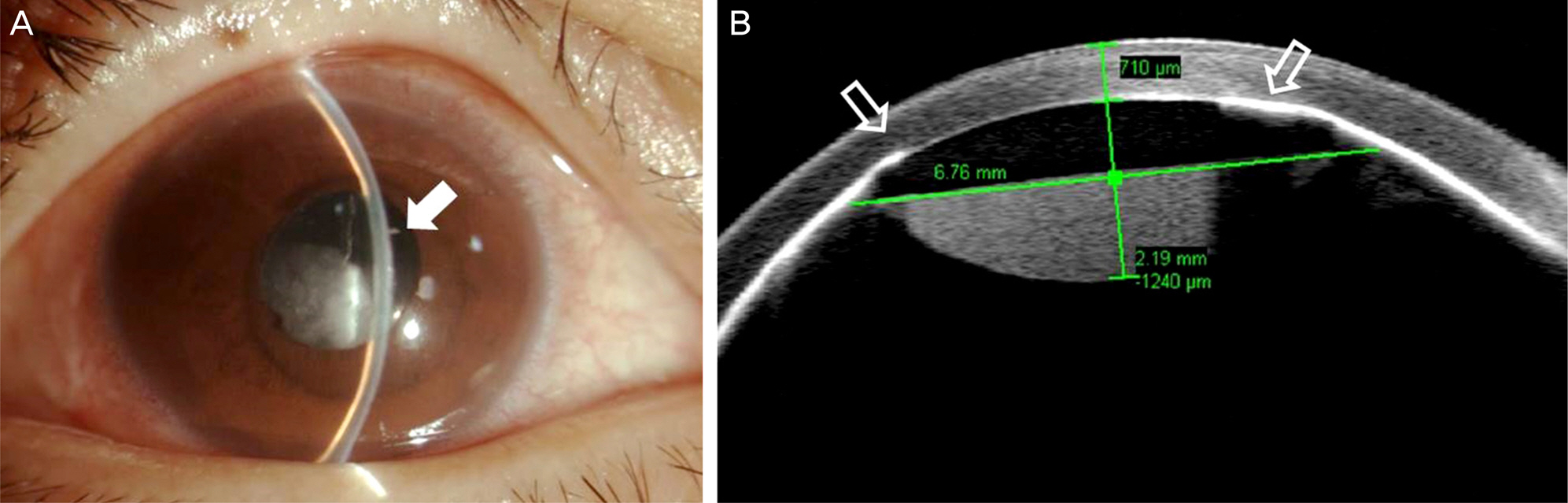
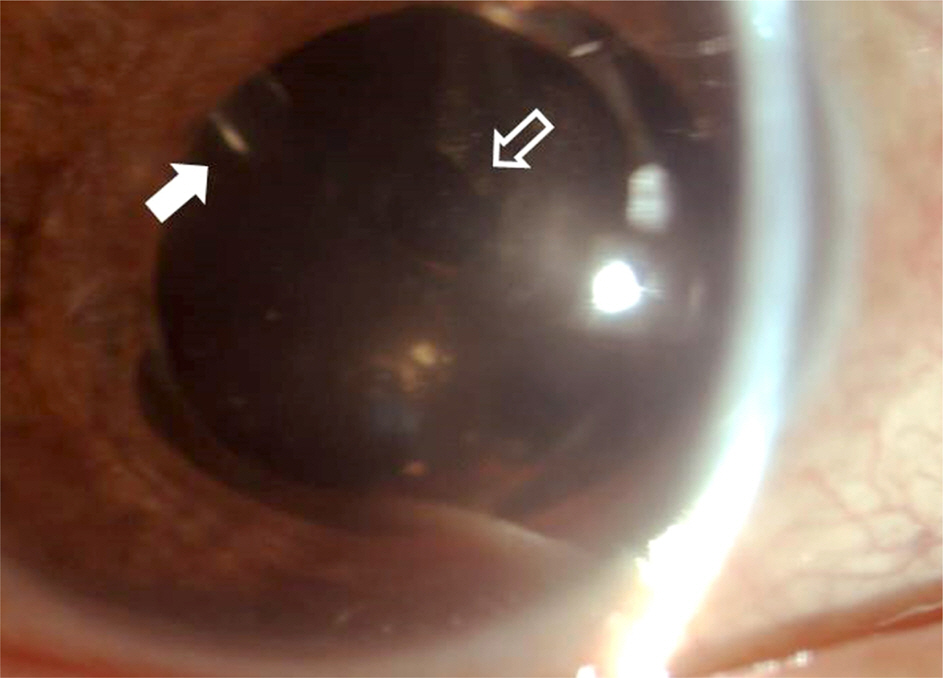
A 55-year-old male visited clinic due to a painful right eye 2 days in duration. Five years ago, he suffered endophthalmitis in his right eye and underwent pars plana vitrectomy. On slit-lamp examination, shallow anterior chamber depth of 2 central corneal thickness and corneal edema were observed along with remnant cortical lens material behind the intraocular lens. Intraocular pressure was 68 mm Hg measured using applanation tonometry. Maximal medical treatment failed to lower the intraocular pressure on the first day of visit. The very next day, anterior chamber became shallower less than 0.5 central corneal thickness and intraocular pressure was 70 mm Hg. Posterior capsular syndrome was suspected on anterior optical coherence tomography and neodymium:yttrium-aluminum-garnet laser posterior capsulotomy was performed, however, normal anterior chamber could not be restored. Despite continuous medical therapy for 3 weeks, the patient's symptoms worsened and intraocular pressure increased over 99 mm Hg and therefore, the Ahmed glaucoma valve was implanted. One day after the operation, intraocular pressure decreased to 10 mm Hg and anterior chamber depth became deeper with the depth of over 5 central corneal thickness. At the final visit 4 months postoperatively, intraocular pressure and normal anatomy of the anterior segment were well maintained.
CONCLUSIONS
Malignant glaucoma syndrome can occur even in vitrectomized eyes and capsular block syndrome can initiate this. Malignant glaucoma syndrome in a vitrectomized eye resistant to maximal medical treatment can be treated with Ahmed valve implantation.
Keyword
MeSH Terms
Figure
Reference
-
References
1. Graefe Av. Beitrage zur pathologie und therapie des glaukoms. Archives of Ophthalmology. 1869; 15:108.2. Shaffer RN, Hoskins HD Jr. Ciliary block (malignant) glaucoma. Ophthalmology. 1978; 85:215–21.
Article3. Weiss DI, Shaffer RN. Ciliary block (malignant) glaucoma. Trans Am Acad Ophthalmol Otolaryngol. 1972; 76:450–61.4. Levene R. A new concept of malignant glaucoma. Arch Ophthalmol. 1972; 87:497–506.
Article5. Chandler PA. Malignant glaucoma. Am J Ophthalmol. 1951; 34:993–1000.
Article6. Eltz H, Gloor B. [Trabeculectomy in cases of angle closure glaucoma--successes and failures (author's transl)]. Klin Monbl Augenheilkd. 1980; 177:556–61.7. Simmons RJ. Malignant glaucoma. Br J Ophthalmol. 1972; 56:263–72.
Article8. Tham CC, Kwong YY, Leung DY, et al. Phacoemulsification versus combined phacotrabeculectomy in medically controlled chronic angle closure glaucoma with cataract. Ophthalmology. 2008; 115:2167–73.e2.
Article9. Tham CC, Kwong YY, Leung DY, et al. Phacoemulsification versus combined phacotrabeculectomy in medically uncontrolled chronic angle closure glaucoma with cataracts. Ophthalmology. 2009; 116:725–31. 731.e1-3.
Article10. Tham CC, Kwong YY, Leung DY, et al. Phacoemulsification vs phacotrabeculectomy in chronic angle-closure glaucoma with cataract: complications [corrected]. Arch Ophthalmol. 2010; 128:303–11.11. Foster PJ, Johnson GJ. Glaucoma in China: how big is the prob-lem? Br J Ophthalmol. 2001; 85:1277–82.
Article12. Shahid H, Salmon JF. Malignant glaucoma: a review of the modern literature. J Ophthalmol. 2012; 2012:852659.
Article13. Shaffer RN. The role of vitreous detachment in aphakic and malignant glaucoma. Trans Am Acad Ophthalmol Otolaryngol. 1954; 58:217–31.14. Quigley HA, Friedman DS, Congdon NG. Possible mechanisms of primary angle-closure and malignant glaucoma. J Glaucoma. 2003; 12:167–80.
Article15. Quigley HA. Angle-closure glaucoma-simpler answers to complex mechanisms: LXVI Edward Jackson Memorial Lecture. Am J Ophthalmol. 2009; 148:657–69.e1.
Article16. Fatt I. Hydraulic flow conductivity of the vitreous gel. Invest Ophthalmol Vis Sci. 1977; 16:565–8.17. Lynch MG, Brown RH, Michels RG, et al. Surgical vitrectomy for pseudophakic malignant glaucoma. Am J Ophthalmol. 1986; 102:149–53.
Article18. Reed JE, Thomas JV, Lytle RA, Simmons RJ. Malignant glaucoma induced by an intraocular lens. Ophthalmic Surg. 1990; 21:177–80.
Article19. Massicotte EC, Schuman JS. A malignant glaucoma-like syndrome following pars plana vitrectomy. Ophthalmology. 1999; 106:1375–9.
Article20. Vélez M, Velásquez LF, Rojas S, et al. Capsular block syndrome: a case report and literature review. Clin Ophthalmol. 2014; 8:1507–13.21. Pinarci EY, Bayar SA, Sizmaz S, et al. Late capsular block syndrome presenting with posterior capsule opacification. J Cataract Refract Surg. 2012; 38:672–6.
Article22. Sia DI, Gilhotra J. Late-onset capsular block syndrome. Int Ophthalmol. 2012; 32:455–7.
Article23. Rana M, Jiang L, Ilango B, Yang YC. Late-onset capsular block syndrome: unusually delayed presentation. Case Rep Ophthalmol. 2013; 4:299–302.
Article24. Huerva V, Sánchez MC, Ascaso FJ, Soldevila J. Late postoperative capsular block syndrome: a case series studied before and after Nd:YAG laser posterior capsulotomy. Eur J Ophthalmol. 2015; 25:27–32.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Positional Intraocular Pressure of Vitrectomized and Normal Fellow Eyes
- Malignant Glaucoma in a Pseudophakic Eye with Slack Lens Zonules
- The Outcome of Inferonasal Trabeculectomy in Diabetic Patients Who Expected or Had Vitrectomy
- Sutured Posterior Chamber Intraocular Lens in the Vitrectomized Eye: Comparison of PMMA and Acrysof(R) Foldable Lenses
- Clinical Study on Anterior Chamber Intraocular Lens Implantation in Completely Vitrectomized Eyes