J Korean Soc Surg Hand.
2013 Mar;18(1):1-8. 10.12790/jkssh.2013.18.1.1.
Comparison of Surgical Outcomes of Percutaneous K-Wire Fixation in Bony Mallet Fingers with Use of Towel Clip versus 18-Gauge Needle
- Affiliations
-
- 1Department of Orthopedic Surgery, Sung-Ae Hospital, Seoul, Korea.
- 2Department of Orthopaedic Surgery, Kwangmyung Sung-Ae Hospital, Gwangmyeong, Korea. sksub@paran.com
- KMID: 2097595
- DOI: http://doi.org/10.12790/jkssh.2013.18.1.1
Abstract
- PURPOSE
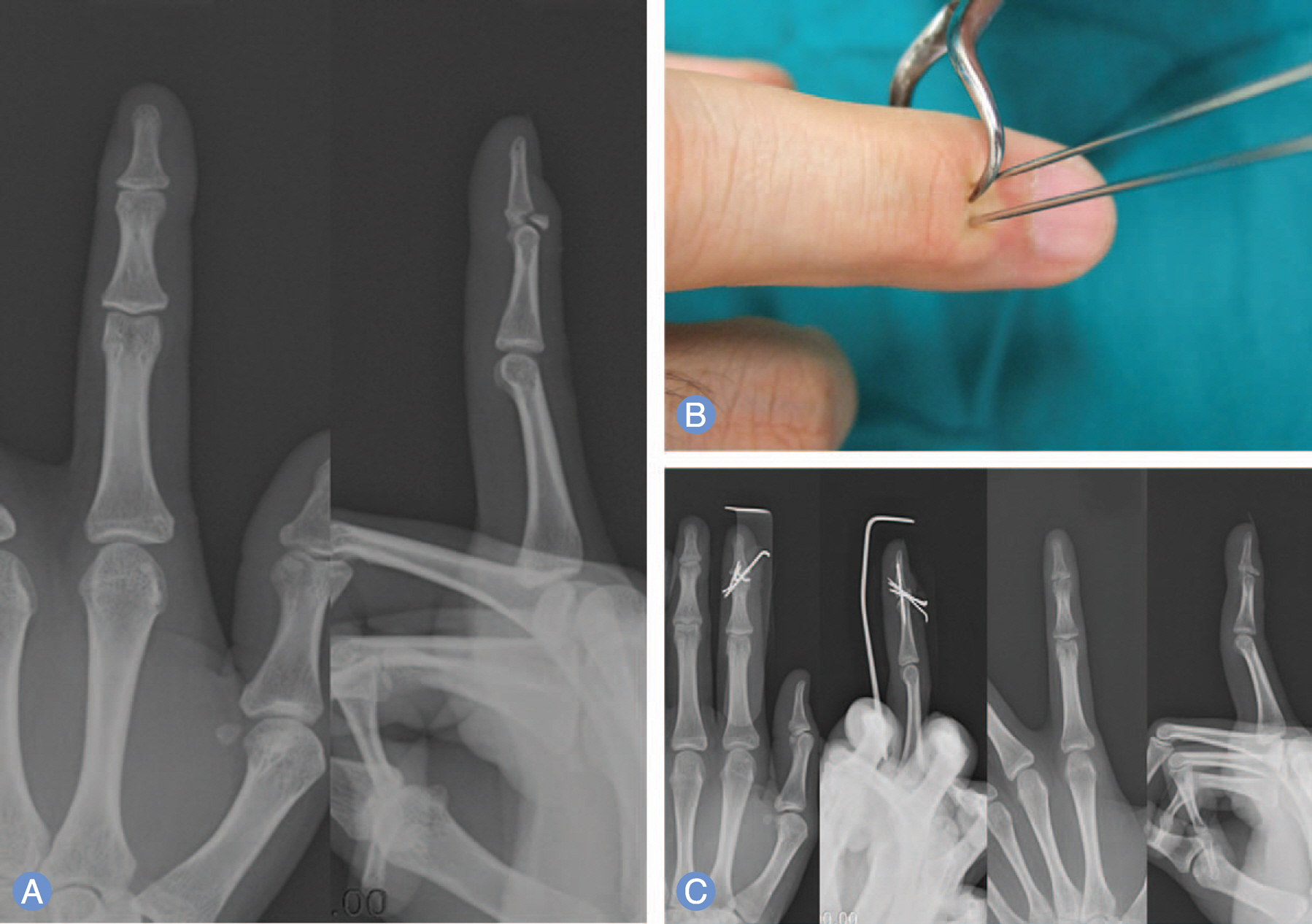
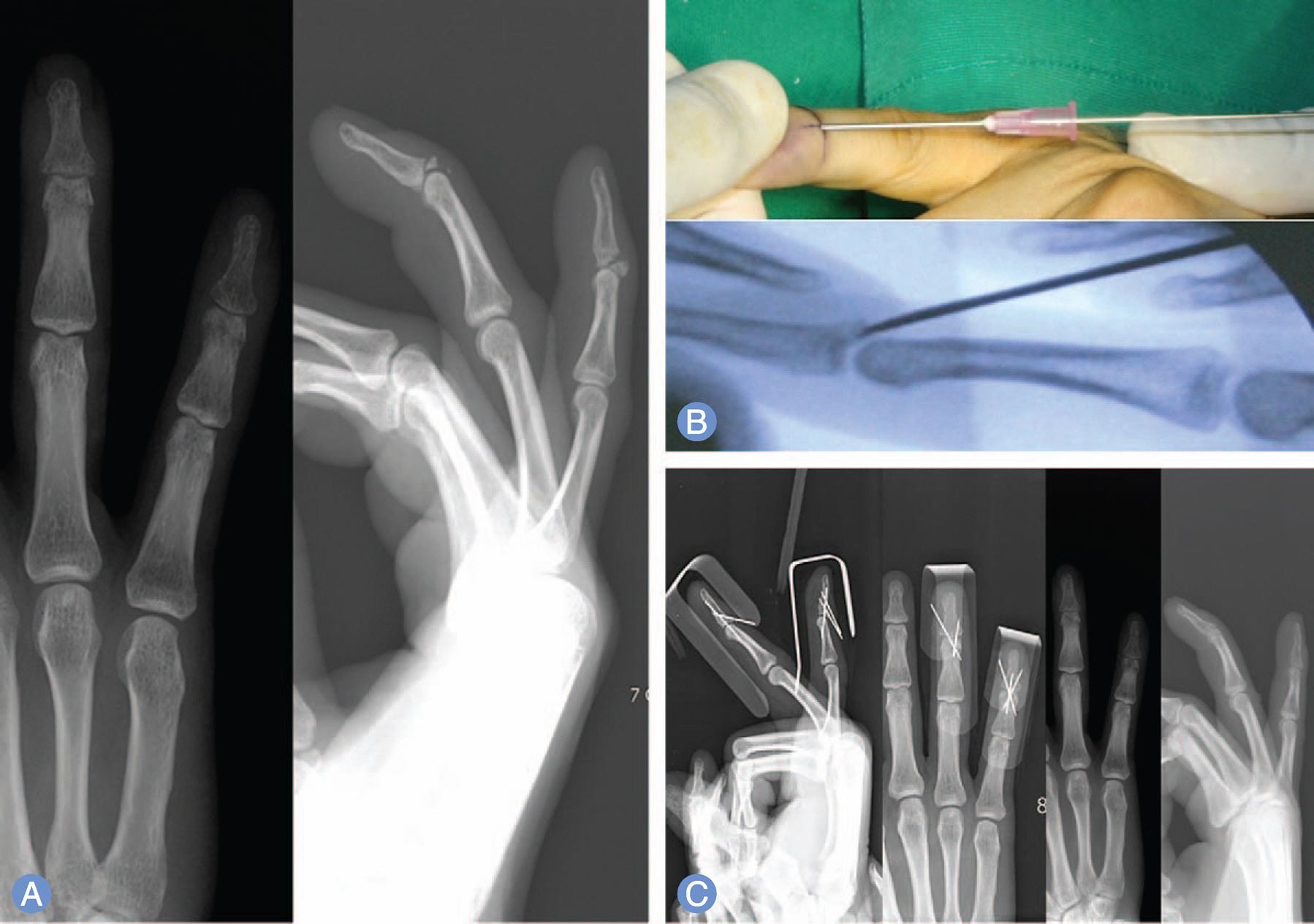
The purpose was to describe comparative analysis of the surgical outcome of percutaneous K-wire fixation of bony mallet fingers reduced with towel clip and 18-gauge needle.
METHODS
We analyzed the bony mallet finger patients with more than twelve months follow-up after percutaneous K-wire fixation. The patients were randomly divided into two groups. Eighteen fingers were treated with closed reduction using towel clip and 18 other fingers were treated with closed reduction using 18-gauge needle.
RESULTS
Radiographs showed bony union and no subluxation in all cases after K-wire removal. The average extension lag was 2.8degrees/1.9degrees, and range of motion of distal interphalangeal joint was 70.3degrees/75degrees respectively. According to Crawford's criteria, excellent results were obtained in 9/11 fingers, good results in 8/7 fingers, and poor result in 1/0 finger, respectively.
CONCLUSION
18-gauge needle reduction in percutaneous K-wire fixation is considered less invasive and useful method for treatment of bony mallet finger with comparable results with towel clip reduction.
Keyword
Figure
Cited by 1 articles
-
Alternative Technique Using Opencast for Early Return to Play after Operation in Patients with Bony Mallet Finger by Sports Injury: A Retrospective Study in a Tertiary Hospital in South Korea
Kyung Ho Lee, Sung Yoon Jung, Ji Woong Kim
Korean J Sports Med. 2024;42(2):113-118. doi: 10.5763/kjsm.2024.42.2.113.
Reference
-
1. Damron TA, Engber WD. Surgical treatment of mallet finger fractures by tension band technique. Clin Orthop Relat Res. 1994; (300):133–40.
Article2. Niechajev IA. Conservative and operative treatment of mallet finger. Plast Reconstr Surg. 1985; 76:580–5.
Article3. Bischoff R, Buechler U, De Roche R, Jupiter J. Clinical results of tension band fixation of avulsion fractures of the hand. J Hand Surg Am. 1994; 19:1019–26.
Article4. Choi JY, Jung HJ, Lee HJ, Son KM, Kim YH. Treatment of bony mallet finger: closed reduction using extension block K-wire. J Korean Fract Soc. 2004; 17:362–7.
Article5. Wehbe MA, Schneider LH. Mallet fractures. J Bone Joint Surg Am. 1984; 66:658–69.6. Crawford GP. The molded polythene splint for mallet finger deformities. J Hand Surg Am. 1984; 9:231–7.
Article7. Hahn SH, Yang BK, Yi SR, Chung SW, Oh SJ. Clinical outcome of operative treatment for bony mallet finger. J Korean Soc Surg Hand. 2000; 5:68–74.8. Hillman FE. New technique for treatment of mallet fingers and fractures of distal phalanx. J Am Med Assoc. 1956; 161:1135–8.
Article9. Kim SJ, Lee KH, Ha TS. Operative treatment of the mallet finger. J Korean Orthop Assoc. 1992; 27:796–801.
Article10. Pratt DR, Bunnell S, Howard LD Jr. Mallet finger; classification and methods of treatment. Am J Surg. 1957; 93:573–8.11. Okafor B, Mbubaegbu C, Munshi I, Williams DJ. Mallet deformity of the finger. Five-year follow-up of conservative treatment. J Bone Joint Surg Br. 1997; 79:544–7.12. Stern PJ, Kastrup JJ. Complications and prognosis of treatment of mallet finger. J Hand Surg Am. 1988; 13:329–34.
Article13. Lubahn JD. Mallet finger fractures: a comparison of open and closed technique. J Hand Surg Am. 1989; 14:394–6.
Article14. Stark HH. Troublesome fractures and dislocations of the hand. American Academy of Orthopedic Surgeons , editor. Instructional course lectures. Vol 19. St. Louis: Mosby;1970. p. 130–49.15. Takami H, Takahashi S, Ando M. Operative treatment of mallet finger due to intra-articular fracture of the distal phalanx. Arch Orthop Trauma Surg. 2000; 120:9–13.16. King HJ, Shin SJ, Kang ES. Complications of operative treatment for mallet fractures of the distal phalanx. J Hand Surg Br. 2001; 26:28–31.17. Ishiguro T, Inoue K, Matsubayashi N, Ito Y, Hashizume N. A new method of closed reduction for mallet fractures. Cent Jpn Orthop Traumatol. 1988; 31:2049–51.18. Han CS, Chung DW, Jeong BO, et al. Percutaneous Kirschner wire fixation of acute mallet fractures percutaneousely reduced by towel clip. J Korean Fract Soc. 2009; 22:283–7.
Article19. Han KJ, Moon JH, Chung NS, Kang SY. Treatment of mallet fracture of the fingers by percutaneous reduction and pinning. J Korean Soc Surg Hand. 2003; 8:153–7.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Percutaneous Kirschner Wire Fixation of Acute Mallet Fractures Percutaneousely Reduced by Towel Clip
- Closed Reduction and Percutaneous K-Wire Fixation of Bony Mallet Finger Using an 18 Gauge Needle
- Intramedullary Fixation of Clavicle Fracture Percutaneously Reduced By Towel Clip
- Open Reduction and K-Wire Fixation for Mallet Finger Fractures
- "Delta(Delta) wire Technique" for Bony Mallet Finger: Surgical Technique