Anat Cell Biol.
2014 Sep;47(3):188-195. 10.5115/acb.2014.47.3.188.
Variations in the origin of middle hepatic artery: a cadaveric study and implications for living donor liver transplantation
- Affiliations
-
- 1Department of Anatomy, Lady Hardinge Medical College and Associated Hospitals, New Delhi, India. drsanjib79@gmail.com
- KMID: 1882594
- DOI: http://doi.org/10.5115/acb.2014.47.3.188
Abstract
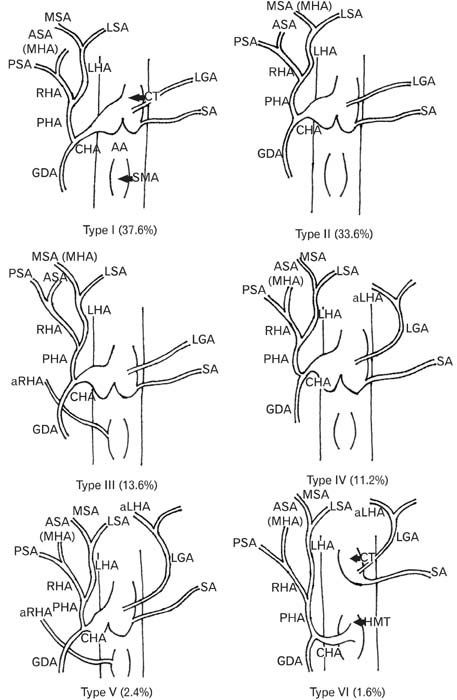
- Living donor liver transplantation has been associated with severe vascular complications like hepatic artery thrombosis, which commonly involves the hepatic segment 4. Most authors have defined the artery to this segment as the middle hepatic artery. The present study was undertaken to characterize the origin of middle hepatic artery and classify the variations observed in cadaveric livers, and also to analyze the significance (if any) of the findings in relation to living donor liver transplantation. The study was conducted on 125 adult livers, without macroscopic abnormalities, retrieved from human cadavers (age, 55-78 years; male, 77; female, 48) obtained from clinical wards. The hepatic arterial system was exposed, the origin of the middle hepatic artery was identified in each liver specimen and the variations observed in its origin were noted across all the specimen. Six types of hepatic arterial configurations were observed based on variations in the origin of middle hepatic artery, taking into consideration the presence of accessory hepatic arteries. It was noted in 19 (15.2%) livers that in the presence of an accessory left hepatic artery, the middle hepatic artery arose as a sub-branch of the right hepatic artery. Presence of the above hepatic arterial configuration in the donor could possibly be associated with an increased risk of intra-operative injury to the middle hepatic artery during right/left lobe living donor liver transplantation and this may subsequently lead to serious post-operative vascular complications like hepatic artery thrombosis.
Keyword
MeSH Terms
Figure
Cited by 2 articles
-
Variations in the branching pattern of the celiac trunk and its clinical significance
Hemamalini
Anat Cell Biol. 2018;51(3):143-149. doi: 10.5115/acb.2018.51.3.143.Anatomical variations of the hepatic artery in it’s extra hepatic journey: a cadaveric study with its clinical implications
Tintu Thottiyil Sukumaran, Susan Joseph, Swapna Ramakrishnan, Asha Joselet Mathew
Anat Cell Biol. 2022;55(3):269-276. doi: 10.5115/acb.22.043.
Reference
-
1. Brown RS Jr, Russo MW, Lai M, Shiffman ML, Richardson MC, Everhart JE, Hoofnagle JH. A survey of liver transplantation from living adult donors in the United States. N Engl J Med. 2003; 348:818–825.2. Suehiro T, Ninomiya M, Shiotani S, Hiroshige S, Harada N, Ryosuke M, Soejima Y, Shimada M, Sugimachi K. Hepatic artery reconstruction and biliary stricture formation after living donor adult liver transplantation using the left lobe. Liver Transpl. 2002; 8:495–499.3. Holbert BL, Baron RL, Dodd GD 3rd. Hepatic infarction caused by arterial insufficiency: spectrum and evolution of CT findings. AJR Am J Roentgenol. 1996; 166:815–820.4. Michels NA. Newer anatomy of the liver and its variant blood supply and collateral circulation. Am J Surg. 1966; 112:337–347.5. Couinaud C. Le foie. Etudes anatomiques et chirurgicales. Paris: Masson;1957.6. Bismuth H. Surgical anatomy and anatomical surgery of the liver. World J Surg. 1982; 6:3–9.7. Saxena R, Zucker SD, Crawford JM. Anatomy and physiology of the liver. In : Zakim D, Boyer TD, editors. Hepatology: A Textbook of Liver Disease. 4th ed. Philadelphia: WB Saunders;2003. p. 3–30.8. Hjortsjo CH. The topography of the intrahepatic duct systems. Acta Anat (Basel). 1951; 11:599–615.9. Mizumoto R, Suzuki H. Surgical anatomy of the hepatic hilum with special reference to the caudate lobe. World J Surg. 1988; 12:2–10.10. O'Rahilly R, Muller F. Human embryology and teratology. 3rd ed. New York: Wiley-Liss;1966. p. 266.11. Descomps P. Le tronc coeliaque. Paris: G. Steinheil;1910.12. Piquand G. Recherches sur l'anatomie du troce coeliaque et de ses branches. Bibliogr Anat. 1910; 19:159–201.13. Rio-Branco P. Essai sur l'anatomie et la medecine operatoire du tronc coeliaque et de ses branches, de l'artere hepatique en particulier. Paris: G. Steinheil;1912.14. Adachi B. Das Arteriensystem der Japaner. Vol. 2. Kyoto: Maruzen;1928. p. 18–71.15. Michels NA. Blood supply and anatomy of the upper abdominal organs with a descriptive atlas. Philadelphia: Lippincott Co.;1955.16. Katsume Y, Kanamaru E, Sakai K. The statistical report about thirteen anomalous cases on the branches of the celiac trunk. J Kur MA. 1978; 41:266–273.17. Ugurel MS, Battal B, Bozlar U, Nural MS, Tasar M, Ors F, Saglam M, Karademir I. Anatomical variations of hepatic arterial system, coeliac trunk and renal arteries: an analysis with multidetector CT angiography. Br J Radiol. 2010; 83:661–667.18. Chitra R. Clinically relevant variations of the coeliac trunk. Singapore Med J. 2010; 51:216–219.19. Prakash , Rajini T, Mokhasi V, Geethanjali BS, Sivacharan PV, Shashirekha M. Coeliac trunk and its branches: anatomical variations and clinical implications. Singapore Med J. 2012; 53:329–331.20. Hiatt JR, Gabbay J, Busuttil RW. Surgical anatomy of the hepatic arteries in 1000 cases. Ann Surg. 1994; 220:50–52.21. Nayak SB, Vasudeva SK. Vascular variations of liver and gallbladder: a case report. Anat Cell Biol. 2013; 46:217–219.22. Healey JE Jr, Schroy PC, Sorensen RJ. The intrahepatic distribution of the hepatic artery in man. J Int Coll Surg. 1953; 20:133–148.23. Onishi H, Kawarada Y, Das BC, Nakano K, Gadzijev EM, Ravnik D, Isaji S. Surgical anatomy of the medial segment (S4) of the liver with special reference to bile ducts and vessels. Hepatogastroenterology. 2000; 47:143–150.24. Futara G, Ali A, Kinfu Y. Variations of the hepatic and cystic arteries among Ethiopians. Ethiop Med J. 2001; 39:133–142.25. Kishi Y, Sugawara Y, Kaneko J, Akamatsu N, Imamura H, Asato H, Kokudo N, Makuuchi M. Hepatic arterial anatomy for right liver procurement from living donors. Liver Transpl. 2004; 10:129–133.26. Wang S, He X, Li Z, Peng Z, Tam NL, Sun C, Hu A, Huang J. Characterization of the middle hepatic artery and its relevance to living donor liver transplantation. Liver Transpl. 2010; 16:736–741.27. Yoshimura H, Uchida H, Ohishi H, Honda N, Ohue S, Kinoshita Y, Katsuragi M, Matuso N, Hosogi Y, Hatakeyama M. Evaluation of "M-point" in hepatic artery to identify left medial segment of liver. Angiographic study. Eur J Radiol. 1986; 6:195–198.28. Kamel IR, Kruskal JB, Pomfret EA, Keogan MT, Warmbrand G, Raptopoulos V. Impact of multidetector CT on donor selection and surgical planning before living adult right lobe liver transplantation. AJR Am J Roentgenol. 2001; 176:193–200.29. Jin GY, Yu HC, Lim HS, Moon JI, Lee JH, Chung JW, Cho BH. Anatomical variations of the origin of the segment 4 hepatic artery and their clinical implications. Liver Transpl. 2008; 14:1180–1184.30. Daseler EH, Anson BJ. The cystic artery and constituents of the hepatic pedicle: a study of 500 specimens. Surg Gynecol Obstet. 1947; 85:47–63.31. Koops A, Wojciechowski B, Broering DC, Adam G, Krupski-Berdien G. Anatomic variations of the hepatic arteries in 604 selective celiac and superior mesenteric angiographies. Surg Radiol Anat. 2004; 26:239–244.32. Couinaud C. Le foie. Etudes anatomiques et chirurgicales. Paris: Masson & Cie;1954. p. 146–186.33. Couinaud C. Surgical anatomy of the liver revisited: embryology. Paris: Couinaud;1989. p. 11–24.34. Fan ST, Lo CM, Liu CL, Wang WX, Wong J. Safety and necessity of including the middle hepatic vein in the right lobe graft in adult-to-adult live donor liver transplantation. Ann Surg. 2003; 238:137–148.35. Sakamoto Y, Takayama T, Nakatsuka T, Asato H, Sugawara Y, Sano K, Imamura H, Kawarasaki H, Makuuchi M. Advantage in using living donors with aberrant hepatic artery for partial liver graft arterialization. Transplantation. 2002; 74:518–521.36. Aramaki O, Sugawara Y, Kokudo N, Takayama T, Makuuchi M. Branch patch reconstruction in living donor liver transplantation: arterialization of grafts with replaced type arteries. Transplantation. 2006; 82:1541–1543.37. Sakai H, Okuda K, Yasunaga M, Kinoshita H, Aoyagi S. Reliability of hepatic artery configuration in 3D CT angiography compared with conventional angiography: special reference to living-related liver transplant donors. Transpl Int. 2005; 18:499–505.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Hepatic Artery Reconstruction Using the Right Gastroepiploic Artery for Hepatic Artery Inflow in a Living Donor Liver Transplantation
- Successful Management of Splenic Artery Steal Syndrome after Living Donor Liver Transplantation
- Revolution and Refinement of Surgical Techniques for Living Donor Partial Liver Transplantation
- Liver abscess developed after cadaveric liver transplantation due to ligation of an accessory right hepatic artery of the donor graft
- Hepatic Artery Anastomosis in Liver Transplantation