Yonsei Med J.
2014 Jan;55(1):84-91. 10.3349/ymj.2014.55.1.84.
The Clinical, Radiological, and Bronchoscopic Findings and Outcomes in Patients with Benign Tracheobronchial Tumors
- Affiliations
-
- 1Division of Pulmonary and Critical Care Medicine, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea. hjk3425@skku.edu
- KMID: 1779890
- DOI: http://doi.org/10.3349/ymj.2014.55.1.84
Abstract
- PURPOSE
We evaluated the characteristics of and treatment outcomes in patients with benign tracheobronchial tumors.
MATERIALS AND METHODS
We reviewed the records of patients with benign tracheobronchial tumors who underwent bronchoscopic intervention with mechanical removal and Nd: YAG laser cauterization, and evaluated the characteristics and treatment outcomes of 55 patients with hamartomas, leiomyomas, papillomas, typical carcinoids, or schwannomas seen between April 1999 and July 2012.
RESULTS
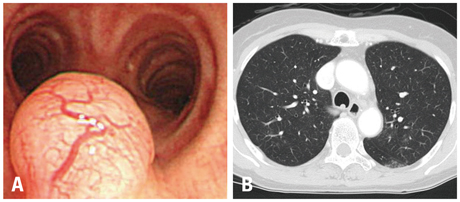
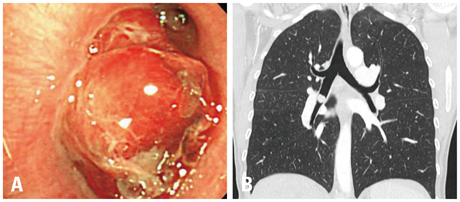
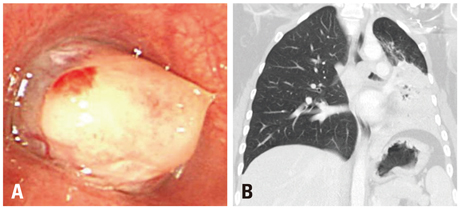
The most common tumors were hamartoma (n=24), leiomyoma (n=16), papilloma (n=7), typical carcinoid (n=5), and schwannoma (n=3). Forty-one patients (75%) had symptoms. On chest computed tomography, 35 patients (64%) had round or ovoid lesions, accompanied by atelectasis (n=26, 47%) or obstructive pneumonia (n=17, 31%). Fatty components (n=9, 16%) and calcifications (n=7, 13%) were observed only in hamartomas, leiomyomas, and typical carcinoids. At bronchoscopy, the typical findings were categorized according to tumor shape, surface, color, and visible vessels. Fifty (91%) patients underwent complete resection. Forty patients (73%) achieved successful bronchoscopic removal defined as complete resection without complications or recurrence. Recurrences occurred in four papillomas, one leiomyoma, and one typical carcinoid. The proportions of tumor types (p=0.029) differed between the successful and unsuccessful removal groups, and a pedunculated base (p<0.001) and no spontaneous bleeding (p=0.037) were more frequent in the successful removal group.
CONCLUSION
We described clinical, radiological, and typical bronchoscopic findings in patients with benign tracheobronchial tumors; these findings might help to differentiate such tumors. Bronchoscopic intervention was a useful treatment modality, and tumor type, pedunculated base, and vascularity may influence successful tumor removal.
MeSH Terms
Figure
Reference
-
1. Arrigoni MG, Woolner LB, Bernatz PE, Miller WE, Fontana RS. Benign tumors of the lung. A ten-year surgical experience. J Thorac Cardiovasc Surg. 1970; 60:589–599.2. Thomas R, Christopher DJ, Thangakunam B, Samuel R. Tracheal schwannoma as a mimic of bronchial asthma. Singapore Med J. 2012; 53:e95–e96.3. Takeda S, Hashimoto T, Kusu T, Kawamura T, Nojiri T, Funakoshi Y, et al. Management and surgical resection for tracheobronchial tumors institutional experience with 12 patients. Interact Cardiovasc Thorac Surg. 2007; 6:484–489.
Article4. Stevic R, Milenkovic B, Stojsic J, Pesut D, Ercegovac M, Jovanovic D. Clinical and radiological manifestations of primary tracheobronchial tumours: a single centre experience. Ann Acad Med Singapore. 2012; 41:205–211.5. Otani Y, Yoshida I, Kawashima O, Yamagishi T, Ishikawa S, Ohtaki A, et al. Benign tumors of the lung: a 20-year surgical experience. Surg Today. 1997; 27:310–312.
Article6. Smith MA, Battafarano RJ, Meyers BF, Zoole JB, Cooper JD, Patterson GA. Prevalence of benign disease in patients undergoing resection for suspected lung cancer. Ann Thorac Surg. 2006; 81:1824–1828.
Article7. Shah H, Garbe L, Nussbaum E, Dumon JF, Chiodera PL, Cavaliere S. Benign tumors of the tracheobronchial tree. Endoscopic characteristics and role of laser resection. Chest. 1995; 107:1744–1751.8. Rodrigues AJ, Coelho D, Dias Júnior SA, Jacomelli M, Scordamaglio PR, Figueiredo VR. Minimally invasive bronchoscopic resection of benign tumors of the bronchi. J Bras Pneumol. 2011; 37:796–800.9. Sharifi N, Massoum SH, Shahri MK, Rezaei A, Ashari AA, Attar AS, et al. Endobronchial leiomyoma; report of a case successfully treated by bronchoscopic resection. J Res Med Sci. 2010; 15:364–370.10. Lamprecht B, Hutarew G, Porsch P, Wegleitner B, Studnicka M. Successful bronchoscopic cryorecanalization in a case of endobronchial lipoma. Diagn Ther Endosc. 2011; 2011:845686.
Article11. Paganin F, Prevot M, Noel JB, Frejeville M, Arvin-Berod C, Bourdin A. A solitary bronchial papilloma with unusual endoscopic presentation: case study and literature review. BMC Pulm Med. 2009; 9:40.
Article12. Stouffer CW, Allan RW, Shillingford MS, Klodell CT. Endobronchial schwannoma presenting with bronchial obstruction. Interact Cardiovasc Thorac Surg. 2010; 10:133–134.
Article13. Suzuki H, Sekine Y, Motohashi S, Chiyo M, Suzuki M, Haga Y, et al. Endobronchial neurogenic tumors treated by transbronchial electrical snaring and Nd-YAG laser abrasion: report of three cases. Surg Today. 2005; 35:243–246.
Article14. Righini CA, Lequeux T, Laverierre MH, Reyt E. Primary tracheal schwannoma: one case report and a literature review. Eur Arch Otorhinolaryngol. 2005; 262:157–160.
Article15. Kim SA, Um SW, Song JU, Jeon K, Koh WJ, Suh GY, et al. Bronchoscopic features and bronchoscopic intervention for endobronchial hamartoma. Respirology. 2010; 15:150–154.
Article16. Kwon YS, Kim H, Koh WJ, Suh GY, Chung MP, Kwon OJ, et al. Clinical characteristics and efficacy of bronchoscopic intervention for tracheobronchial leiomyoma. Respirology. 2008; 13:908–912.
Article17. Park JS, Lee M, Kim HK, Choi YS, Kim K, Kim J, et al. Primary leiomyoma of the trachea, bronchus, and pulmonary parenchyma--a single-institutional experience. Eur J Cardiothorac Surg. 2012; 41:41–45.18. Blanco I, Burgués C, Puzo C. [Proposed terms for endobronchial lesions in patients suspected of having a bronchial neoplasm]. Arch Bronconeumol. 2007; 43:36–39.
Article19. Ko JM, Jung JI, Park SH, Lee KY, Chung MH, Ahn MI, et al. Benign tumors of the tracheobronchial tree: CT-pathologic correlation. AJR Am J Roentgenol. 2006; 186:1304–1313.
Article20. Kurkcuoglu IC, Demircan S, Kurul IC, Demirag F. Endobronchial lipomatous hamartoma. Asian Cardiovasc Thorac Ann. 2005; 13:372–373.
Article21. Cosío BG, Villena V, Echave-Sustaeta J, de Miguel E, Alfaro J, Hernandez L, et al. Endobronchial hamartoma. Chest. 2002; 122:202–205.
Article22. Meisinger QC, Klein JS, Butnor KJ, Gentchos G, Leavitt BJ. CT features of peripheral pulmonary carcinoid tumors. AJR Am J Roentgenol. 2011; 197:1073–1080.
Article23. Kasahara K, Fukuoka K, Konishi M, Hamada K, Maeda K, Mikasa K, et al. Two cases of endobronchial neurilemmoma and review of the literature in Japan. Intern Med. 2003; 42:1215–1218.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Meanings and Indications of pretreatment assessment of esophageal carcinoma with bronchoscopy
- Esophageal stenosis due to tracheobronchial remnants: a case report
- CT findings of tracheobronchial tuberculosis
- Congenital esophageal stenosis due to tracheobronchial remnants
- A Case of Primary Localized Tracheobronchial Amyloidosis