Cancer Res Treat.
2021 Jan;53(1):212-222. 10.4143/crt.2020.219.
Cervical Cancer Screening Rate and Willingness among Female Migrants in Shenzhen, China: Three-Year Changes in Citywide Surveys
- Affiliations
-
- 1Department of Healthcare, Affiliated Shenzhen Maternity and Child Healthcare Hospital, Southern Medical University, Shenzhen, China
- 2Research Team of Cervical Cancer Prevention Project in Shenzhen, Affiliated Shenzhen Maternity and Child Healthcare Hospital, Southern Medical University, Shenzhen, China
- 3Department of Gynecology, Affiliated Shenzhen Maternity and Child Healthcare Hospital, Southern Medical University, Shenzhen, China
- KMID: 2510663
- DOI: http://doi.org/10.4143/crt.2020.219
Abstract
- Purpose
This study attempted to detect the changes of cervical cancer screening rate and willingness among female migrants, and the associated socio-demographic factors in Shenzhen city.
Materials and Methods
Two citywide surveys were conducted using a multistage random cluster sampling method in 2011 and 2014, respectively. Data on demographic characteristics, screening participation, and willingness to screen were collected. Logistic regression models were applied to detect possible associated socio-demographic characteristics, and their variations with survey years.
Results
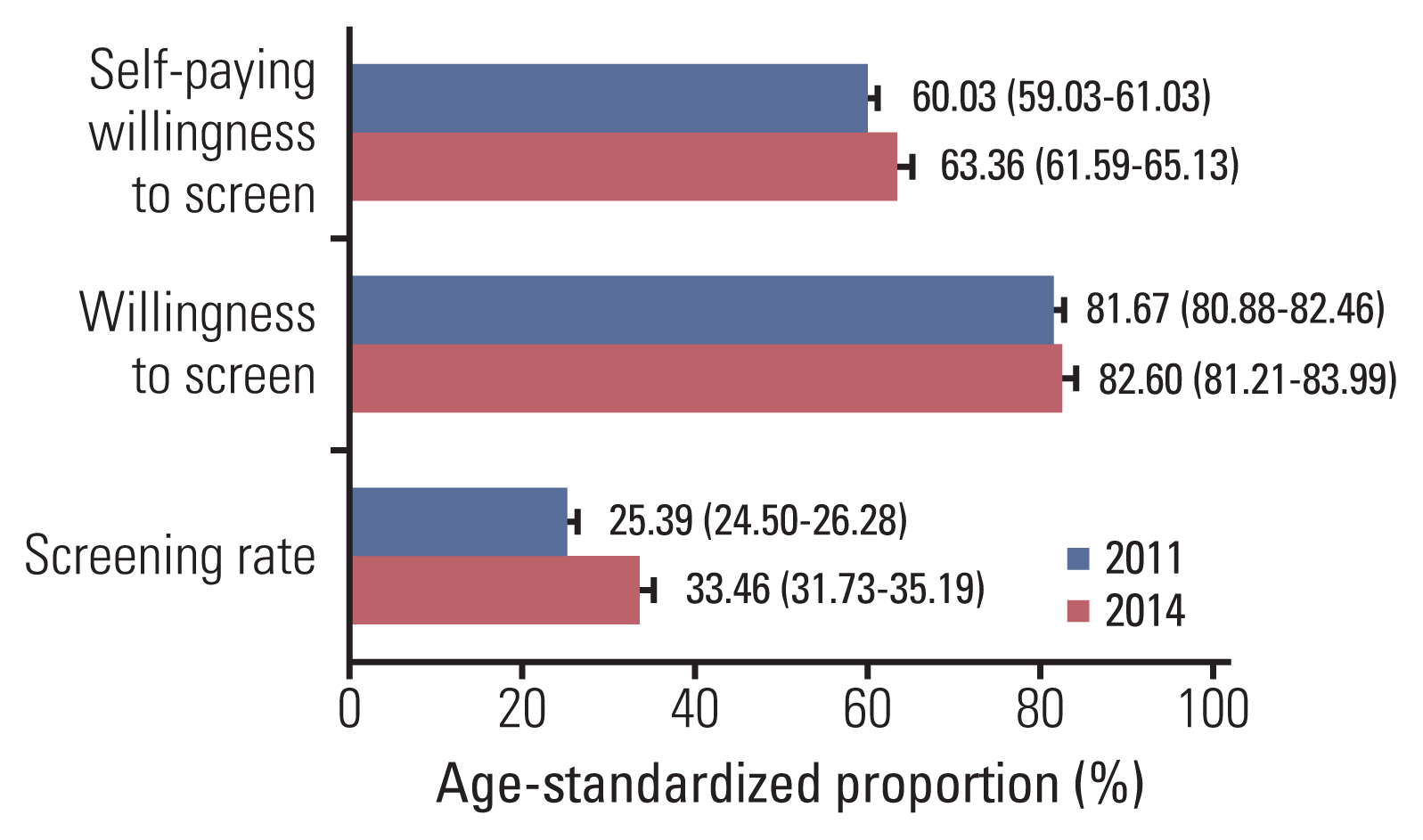
In total, 12,017 female migrants were enrolled, with a mean age (standard deviation) of 36.73 (6.55) years. From 2011 to 2014, the screening rate increased (25.8% vs. 35.1%, p < 0.001), while the willingness to screen remained stable (82.2% vs. 82.8%, p=0.46). Overall, socio-demographic characteristics of female migrants, including age, marital status, education, monthly income, employment, and medical insurance, were found to be positively associated with screening participation. Similar impacts in relation to willingness were observed except for age. However, these associations varied with survey years, mainly in the contributions of education and monthly income to screening participation, as well as age, monthly income, and medical insurance to willingness of being screened.
Conclusion
Identifying changes of associated socio-demographic factors precisely is warranted of necessity, which provides novel clues to adjust targeted actions regularly in promoting cervical cancer screening participation among female migrants in Shenzhen.
Keyword
Figure
Reference
-
References
1. Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018; 68:394–424.
Article2. Chen W, Zheng R, Baade PD, Zhang S, Zeng H, Bray F, et al. Cancer statistics in China, 2015. CA Cancer J Clin. 2016; 66:115–32.
Article3. Saslow D, Solomon D, Lawson HW, Killackey M, Kulasingam SL, Cain J, et al. American Cancer Society, American Society for Colposcopy and Cervical Pathology, and American Society for Clinical Pathology screening guidelines for the prevention and early detection of cervical cancer. CA Cancer J Clin. 2012; 62:147–72.
Article4. Catarino R, Schafer S, Vassilakos P, Petignat P, Arbyn M. Accuracy of combinations of visual inspection using acetic acid or lugol iodine to detect cervical precancer: a meta-analysis. BJOG. 2018; 125:545–53.
Article5. Di J, Rutherford S, Chu C. Review of the cervical cancer burden and population-based cervical cancer screening in China. Asian Pac J Cancer Prev. 2015; 16:7401–7.
Article6. Wang B, He M, Chao A, Engelgau MM, Saraiya M, Wang L, et al. Cervical cancer screening among adult women in China, 2010. Oncologist. 2015; 20:627–34.
Article7. Bao H, Zhang L, Wang L, Zhang M, Zhao Z, Fang L, et al. Significant variations in the cervical cancer screening rate in China by individual-level and geographical measures of socioeconomic status: a multilevel model analysis of a nationally representative survey dataset. Cancer Med. 2018; 7:2089–100.
Article8. Statistics Bureau of Shenzhen Municipality. Shenzhen statistical yearbook, 2011 [Internet]. Shenzhen: Statistics Bureau of Shenzhen Municipality;2011. [cited 2020 Aug 10]. Available from: http://tjj.sz.gov.cn/zwgk/zfxxgkml/tjsj/tjnj/201202/t2-0120221_1806408.htm .9. Li H, Chung RY, Wei X, Mou J, Wong SY, Wong MC, et al. Comparison of perceived quality amongst migrant and local patients using primary health care delivered by community health centres in Shenzhen, China. BMC Fam Pract. 2014; 15:76.
Article10. Lin W, Wang Y, Liu Z, Chen B, Yuan S, Wu B, et al. Inequalities in awareness and attitude towards HPV and its vaccine between local and migrant residents who participated in cervical cancer screening in Shenzhen, China. Cancer Res Treat. 2020; 52:207–17.
Article11. Li JB, Qiao YL. Exploration of cervical cancer preventive experiences in city: 10 years of cervical cancer prevention in Shenzhen. China Cancer. 2015; 24:971–2.12. Wang LD, Lam WW, Fielding R. Cervical cancer prevention practices through screening and vaccination: a cross-sectional study among Hong Kong Chinese women. Gynecol Oncol. 2015; 138:311–6.
Article13. Chan CW, Choi KC, Wong RS, Chow KM, So WK, Leung DY, et al. Examining the cervical screening behaviour of women aged 50 or above and its predicting factors: a population-based survey. Int J Environ Res Public Health. 2016; 13:1195.
Article14. Gu C, Chan CW, He GP, Choi KC, Yang SB. Chinese women’s motivation to receive future screening: the role of social-demographic factors, knowledge and risk perception of cervical cancer. Eur J Oncol Nurs. 2013; 17:154–61.
Article15. Jia Y, Li S, Yang R, Zhou H, Xiang Q, Hu T, et al. Knowledge about cervical cancer and barriers of screening program among women in Wufeng County, a high-incidence region of cervical cancer in China. PLoS One. 2013; 8:e67005.
Article16. Pan XF, Zhao ZM, Sun J, Chen F, Wen QL, Liu K, et al. Acceptability and correlates of primary and secondary prevention of cervical cancer among medical students in southwest China: implications for cancer education. PLoS One. 2014; 9:e110353.
Article17. Wu E, Tiggelaar SM, Jiang T, Zhao H, Wu R, Wu R, et al. Cervical cancer prevention-related knowledge and attitudes among female undergraduate students from different ethnic groups within China, a survey-based study. Women Health. 2018; 58:661–84.
Article18. Johnson CE, Mues KE, Mayne SL, Kiblawi AN. Cervical cancer screening among immigrants and ethnic minorities: a systematic review using the Health Belief Model. J Low Genit Tract Dis. 2008; 12:232–41.19. Chua GT, Ho FK, Tung KT, Wong RS, Cheong KN, Yip PS, et al. Sexual behaviors and intention for cervical screening among HPV-vaccinated young Chinese females. Vaccine. 2020; 38:1025–31.
Article20. Chang HK, Myong JP, Byun SW, Lee SJ, Lee YS, Lee HN, et al. Factors associated with participation in cervical cancer screening among young Koreans: a nationwide cross-sectional study. BMJ Open. 2017; 7:e013868.
Article21. Bao HL, Wang LH, Wang LM, Fang LW, Zhang M, Zhao ZP, et al. Study on the coverage of cervical and breast cancer screening among women aged 35–69 years and related impact of socioeconomic factors in China, 2013. Zhonghua Liu Xing Bing Xue Za Zhi. 2018; 39:208–12.22. Zhao XL, Xu XQ, Duan XZ, Rezhake R, Hu SY, Wang Y, et al. Comparative performance evaluation of different HPV tests and triaging strategies using self-samples and feasibility assessment of thermal ablation in ‘colposcopy and treat’ approach: a population-based study in rural China. Int J Cancer. 2020; 147:1275–85.
Article23. Lin W, Zhou L, Hu H, Chen B, Yuan S, Wu B, et al. The number and gender of children synergistically impact on a mother’s practice of human papillomavirus testing and attitudes towards vaccination in Shenzhen, China. Cancer Epidemiol. 2020; 65:101682.
Article24. Statistics Bureau of Shenzhen Municipality. Shenzhen statistical yearbook, 2015 [Internet]. Shenzhen: Statistics Bureau of Shenzhen Municipality;2015. [cited 2020 Aug 10]. Available from: http://tjj.sz.gov.cn/zwgk/zfxxgkml/tjsj/tjnj/201606/t2-0160607_3686823.htm .
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Inequalities in Awareness and Attitude towards HPV and Its Vaccine between Local and Migrant Residents Who Participated in Cervical Cancer Screening in Shenzhen, China
- Women's Willingness to Pay for Cancer Screenin
- Breast and Cervical Cancer Screening Behavior in Female Cancer Survivors: The Korea National Health and Nutrition Examination Survey, 2007–2012
- Aplasia of the Internal Carotid Artery with Dandy-Walker Variant
- Comments on the Article “Arthroscopic Treatment for Femoroacetabular Impingement with Extraspinal Diffuse Idiopathic Skeletal Hyperostosis”: To the Editor