Allergy Asthma Immunol Res.
2020 May;12(3):467-484. 10.4168/aair.2020.12.3.467.
Increasing Prevalence and Mortality of Asthma With Age in Korea, 2002–2015: A Nationwide, Population-Based Study
- Affiliations
-
- 1Office of Biostatistics, Ajou Research Institute for Innovative Medicine, Ajou University Medical Center, Suwon, Korea.
- 2Department of Biomedical Informatics, Ajou University School of Medicine, Suwon, Korea.
- 3Department of Clinical Pharmacology and Therapeutics, CHA Bundang Medical Center, CHA University, Seongnam, Korea.
- 4Department of Allergy and Clinical Immunology, Ajou University School of Medicine, Suwon, Korea. hspark@ajou.ac.kr
- 5College of Pharmacy, Korea University, Sejong, Korea.
- KMID: 2471230
- DOI: http://doi.org/10.4168/aair.2020.12.3.467
Abstract
- PURPOSE
The prevalence of asthma is increasing globally as the world population increases; however, and the prevalence and mortality of asthma have not been extensively investigated. Also, the effects of severity and aging on asthma prevalence and mortality are unknown. We aimed to investigate trends of the prevalence and mortality of asthma as well as health care uses and costs over 14 years according to disease severity by using real-world data in Korea.
METHODS
Using the National Health Insurance Sharing Service database, we extracted asthmatic patients having diagnosis codes of asthma and prescription records of antiasthmatic medications from 2002 to 2015 and categorized them according to asthma exacerbation and regular treatment. We defined asthma-associated death in terms of patients' prescription records within 3 months before all-cause death, then linked with the Cause of Death Statistics. The annual asthma-related health care uses and costs were analyzed.
RESULTS
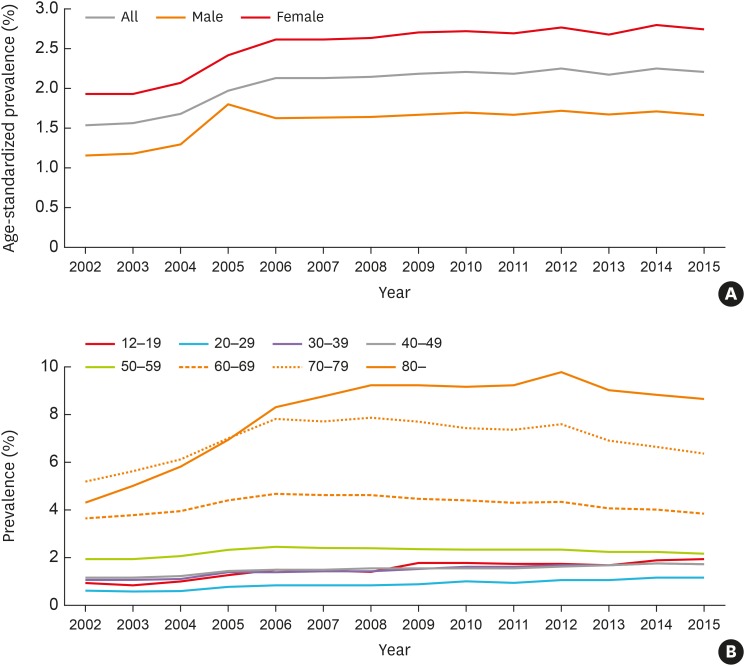
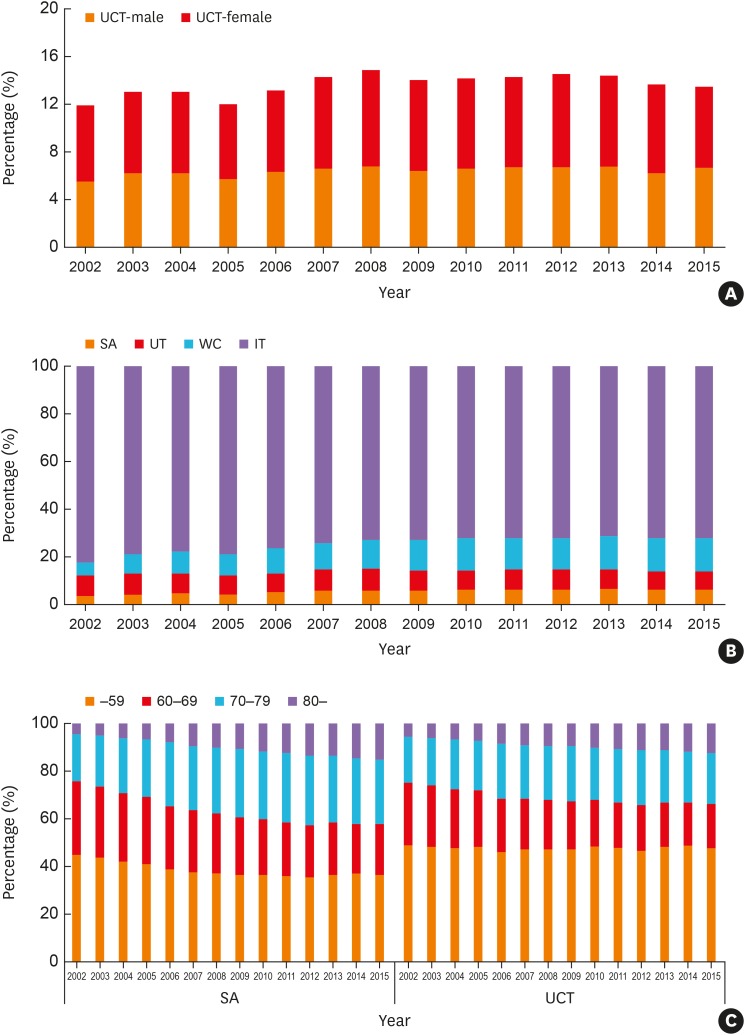
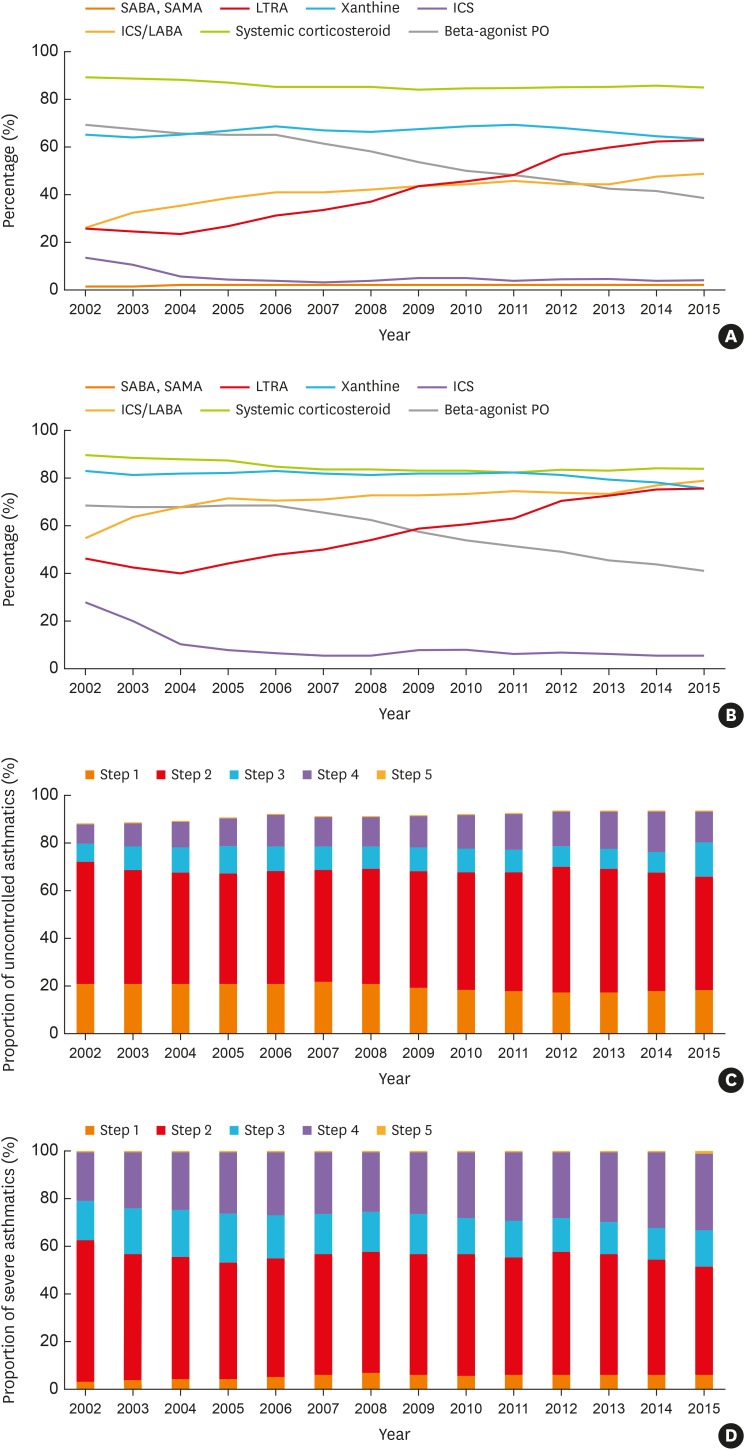
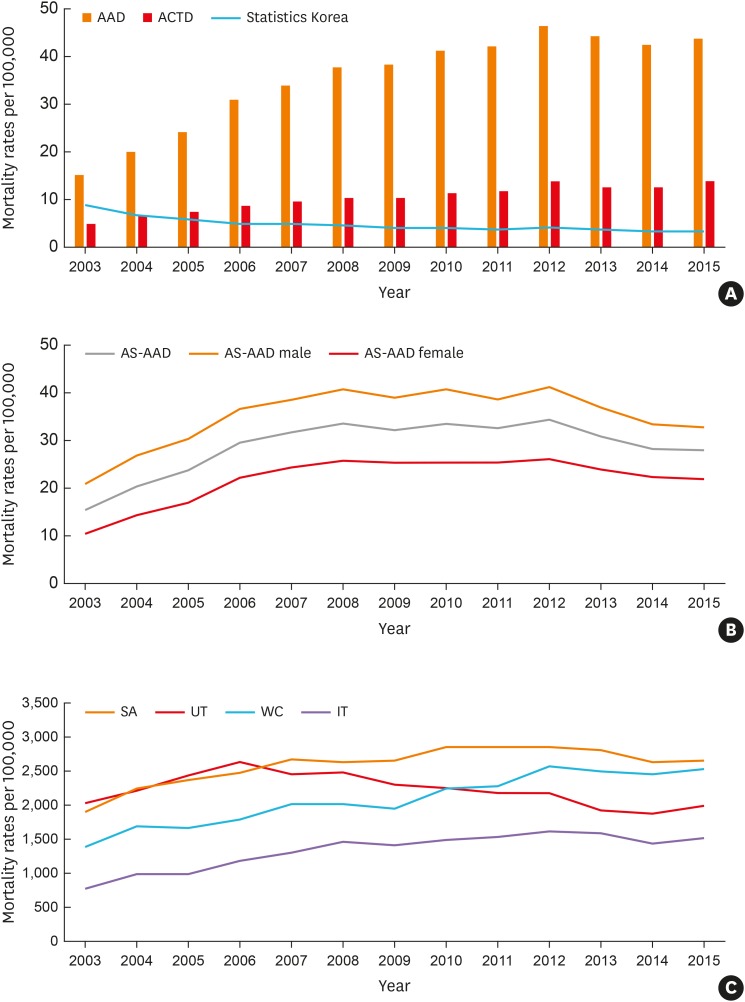
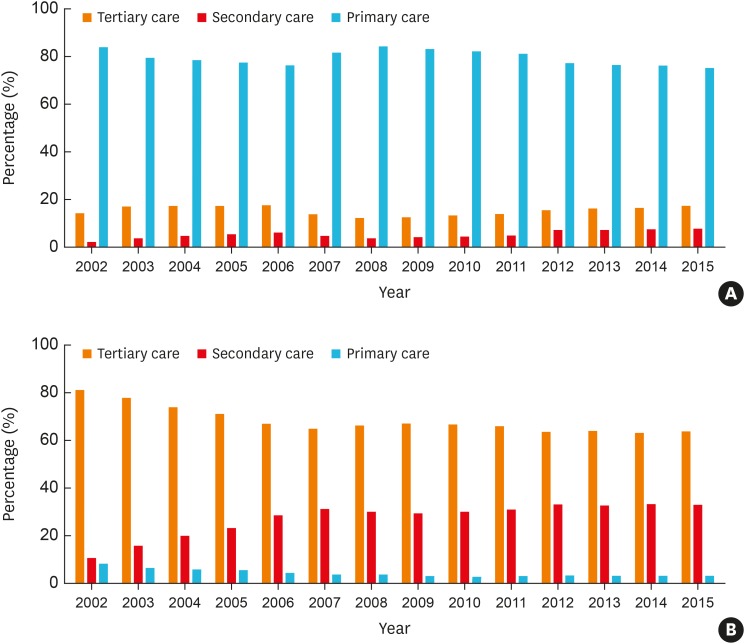
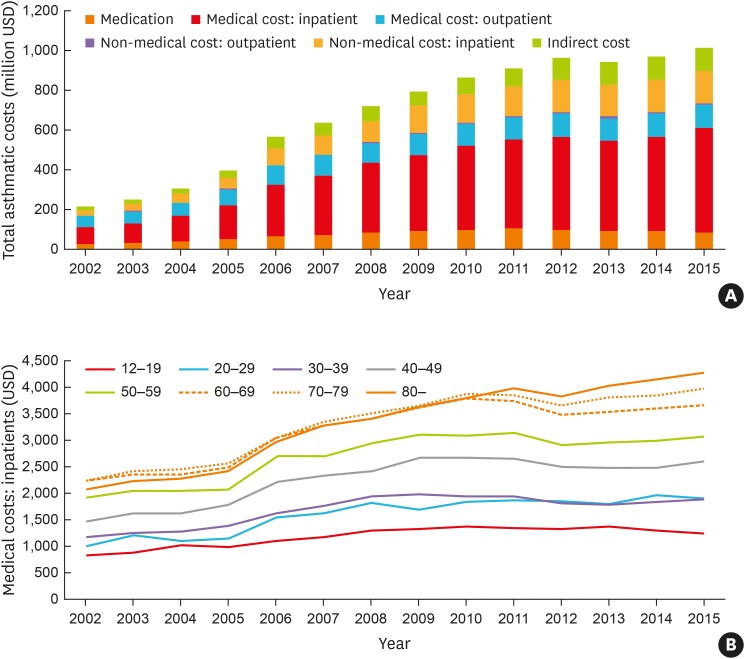
The prevalence rates of asthma (1.6% to 2.2%) and severe asthma (SA; 3.5% to 6.1% among total asthmatics) have increased steadily over the decade in Korea, where the proportion of elderly asthmatics having increased. The asthma-related health care uses and costs had increased during the study period with the highest uses/costs in SA. The asthma mortality had a steady rising trend from 16.2 to 28.0 deaths per 100,000 with the highest mortality in SA.
CONCLUSIONS
The prevalence and mortality of asthma as well as SA increases along with the burden of health care uses/costs. More active interventions, including changes in health care policies, are needed to reduce the prevalence and mortality of asthma, especially SA.
Keyword
MeSH Terms
Figure
Cited by 1 articles
-
Biological treatments for severe asthma
Hyun Jung Jin
Yeungnam Univ J Med. 2020;37(4):262-268. doi: 10.12701/yujm.2020.00647.
Reference
-
1. Zein JG, Dweik RA, Comhair SA, Bleecker ER, Moore WC, Peters SP, et al. Asthma is more severe in older adults. PLoS One. 2015; 10:e0133490. PMID: 26200463.
Article2. Holt S, Masoli M, Beasley R. The use of the self-management plan system of care in adult asthma. Prim Care Respir J. 2004; 13:19–27. PMID: 16701633.
Article3. Crescioni M, Gorina Y, Bilheimer L, Gillum RF. Trends in Health Status and Health Care Use Among Older Men. Natl Health Stat Report. 2010; 1–18.4. National Health Insurance Service (KR). Status of national health insurance benefits 2004–2010 [Internet]. Wonju: National Health Insurance Service;2011. cited 2017 Nov 22. Available from: http://www.nhic.or.kr.5. Statistics Korea. Cause of death statistics [Internet]. Daejeon: Korean Statistical Information Service;cited 2017 Feb 20. Available from: http://kosis.kr.6. Kim YK, Kim SH, Tak YJ, Jee YK, Lee BJ, Kim SH, et al. High prevalence of current asthma and active smoking effect among the elderly. Clin Exp Allergy. 2002; 32:1706–1712. PMID: 12653160.
Article7. Song WJ, Lee JH, Kang Y, Joung WJ, Chung KF. Future risks in patients with severe asthma. Allergy Asthma Immunol Res. 2019; 11:763–778. PMID: 31552713.
Article8. Kwon JW, Kim BJ, Song Y, Seo JH, Kim TH, Yu J, et al. Changes in the prevalence of childhood asthma in Seoul from 1995 to 2008 and its risk factors. Allergy Asthma Immunol Res. 2011; 3:27–33. PMID: 21217922.
Article9. Zhang Y, Zhang L. Increasing prevalence of allergic rhinitis in China. Allergy Asthma Immunol Res. 2019; 11:156–169. PMID: 30661309.
Article10. To T, Simatovic J, Zhu J, Feldman L, Dell SD, Lougheed MD, et al. Asthma deaths in a large provincial health system. A 10-year population-based study. Ann Am Thorac Soc. 2014; 11:1210–1217. PMID: 25166217.
Article11. Kim SY, Jung JY, Park MS, Kang YA, Kim EY, Kim SK, et al. Increased prevalence of self-reported asthma among Korean adults: an analysis of KNHANES I and IV data. Lung. 2013; 191:281–288. PMID: 23483196.
Article12. Cho SH, Park HW, Rosenberg DM. The current status of asthma in Korea. J Korean Med Sci. 2006; 21:181–187. PMID: 16614498.
Article13. Kim JA, Yoon S, Kim LY, Kim DS. Towards actualizing the value potential of Korea Health Insurance Review and Assessment (HIRA) Data as a resource for health research: strengths, limitations, applications, and strategies for optimal use of HIRA data. J Korean Med Sci. 2017; 32:718–728. PMID: 28378543.
Article14. Chung KF, Wenzel SE, Brozek JL, Bush A, Castro M, Sterk PJ, et al. International ERS/ATS guidelines on definition, evaluation and treatment of severe asthma. Eur Respir J. 2014; 43:343–373. PMID: 24337046.15. Kim YH, Shin SJ, Park JY, Jung YJ, Kim JM, Lee TJ, et al. Costing methods in Healthcare. Seoul: National Evidence-based Healthcare Collaborating Agency;2013.16. Kim DK, Park YB, Oh YM, Jung KS, Yoo JH, Yoo KH, et al. Korean asthma guideline 2014: summary of major updates to the Korean asthma guideline 2014. Tuberc Respir Dis. 2016; 79:111–120.
Article17. Becker AB, Abrams EM. Asthma guidelines: the Global Initiative for Asthma in relation to national guidelines. Curr Opin Allergy Clin Immunol. 2017; 17:99–103. PMID: 28118238.
Article18. Kang SY, Song WJ, Cho SH, Chang YS. Time trends of the prevalence of allergic diseases in Korea: a systematic literature review. Asia Pac Allergy. 2018; 8:e8. PMID: 29423375.
Article19. Tarraf H, Aydin O, Mungan D, Albader M, Mahboub B, Doble A, et al. Prevalence of asthma among the adult general population of five Middle Eastern countries: results of the SNAPSHOT program. BMC Pulm Med. 2018; 18:68. PMID: 29751756.
Article20. Global Initiative for Asthma. Global strategy for asthma management and prevention [Internet]. Fontana: Global Initiative for Asthma;2018. cited 2019 Mar 22. Available from: http://ginasthma.org/gina-reports/.21. Kim S, Kim J, Kim K, Kim Y, Park Y, Baek S, et al. Healthcare use and prescription patterns associated with adult asthma in Korea: analysis of the NHI claims database. Allergy. 2013; 68:1435–1442. PMID: 24131085.
Article22. Park SY, Kim JH, Kim HJ, Seo B, Kwon OY, Chang HS, et al. High prevalence of asthma in elderly women: findings from a Korean National Health Database and Adult Asthma Cohort. Allergy Asthma Immunol Res. 2018; 10:387–396. PMID: 29949835.
Article23. Dilokthornsakul P, Lee TA, Dhippayom T, Jeanpeerapong N, Chaiyakunapruk N. Comparison of health care utilization and costs for patients with asthma by severity and health insurance in Thailand. Value Health Reg Issues. 2016; 9:105–111. PMID: 27881251.
Article24. Kim CY, Park HW, Ko SK, Chang SI, Moon HB, Kim YY, et al. The financial burden of asthma: a nationwide comprehensive survey conducted in the republic of Korea. Allergy Asthma Immunol Res. 2011; 3:34–38. PMID: 21217923.
Article25. Masoli M, Fabian D, Holt S, Beasley R. Global Initiative for Asthma (GINA) Program. The global burden of asthma: executive summary of the GINA Dissemination Committee report. Allergy. 2004; 59:469–478. PMID: 15080825.
Article26. Statistics Korea. Annual report on the causes of death statistics [Internet]. Daejeon: Statistics Korea;2018. cited 2018 Jul 25. Available from: http://kostat.go.kr/portal/eng/surveyOutline/5/1/index.static.27. Park SY, Kim JH, Kwon HS, Kim TB, Moon HB, Cho YS, et al. Elderly women and asthma: findings from Korea national health investigations and asthma cohort. Eur Respir J. 2017; 50:PA640.
Article28. United Nations, Department of Economics and Social Affairs, Population Division. World population ageing 2017 - Highlights (ST/ESA/SER.A/397). New York: United Nations;2017.29. Choi JY, Yoon HK, Lee JH, Yoo KH, Kim BY, Bae HW, et al. Current status of asthma care in South Korea: nationwide the Health Insurance Review and Assessment Service database. J Thorac Dis. 2017; 9:3208–3214. PMID: 29221297.
Article30. Kim MH, Kim SH, Park SY, Ban GY, Kim JH, Jung JW, et al. Characteristics of adult severe refractory asthma in Korea analyzed from the severe asthma registry. Allergy Asthma Immunol Res. 2019; 11:43–54. PMID: 30479076.
Article31. Braido F. Failure in asthma control: reasons and consequences. Scientifica (Cairo). 2013; 2013:549252. PMID: 24455432.
Article32. Godard P, Chanez P, Siraudin L, Nicoloyannis N, Duru G. Costs of asthma are correlated with severity: a 1-yr prospective study. Eur Respir J. 2002; 19:61–67. PMID: 11843329.
Article33. Serra-Batlles J, Plaza V, Morejón E, Comella A, Brugués J. Costs of asthma according to the degree of severity. Eur Respir J. 1998; 12:1322–1326. PMID: 9877485.
Article34. Cisternas MG, Blanc PD, Yen IH, Katz PP, Earnest G, Eisner MD, et al. A comprehensive study of the direct and indirect costs of adult asthma. J Allergy Clin Immunol. 2003; 111:1212–1218. PMID: 12789219.
Article35. Bahadori K, Doyle-Waters MM, Marra C, Lynd L, Alasaly K, Swiston J, et al. Economic burden of asthma: a systematic review. BMC Pulm Med. 2009; 9:24. PMID: 19454036.
Article36. Ogura S, Jakovljevic MM. Editorial: Global population aging - health care, social and economic consequences. Front Public Health. 2018; 6:335. PMID: 30515374.
Article37. Antonicelli L, Bucca C, Neri M, De Benedetto F, Sabbatani P, Bonifazi F, et al. Asthma severity and medical resource utilisation. Eur Respir J. 2004; 23:723–729. PMID: 15176687.
Article38. Stanford R, McLaughlin T, Okamoto LJ. The cost of asthma in the emergency department and hospital. Am J Respir Crit Care Med. 1999; 160:211–215. PMID: 10390402.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Cancer Statistics in Korea: Incidence, Mortality, Survival, and Prevalence in 2015
- Disease-Specific Mortality and Prevalence Trends in Korea, 2002–2015
- The Current Status of Asthma in Korea
- Epidemiologic study of asthma prevalence
- Cancer Statistics in Korea: Incidence, Mortality, Survival, and Prevalence in 2014