Prevalence, Risk Factors and Cutoff Values for Bronchial Hyperresponsiveness to Provocholine in 7-Year-Old Children
- Affiliations
-
- 1Department of Pediatrics, Childhood Asthma Atopy Center, Environmental Health Center, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea. sjhong@amc.seoul.kr
- 2Department of Pediatrics, Seoul National University Hospital, Seoul, Korea.
- 3Department of Pediatrics, International St. Mary's Hospital, Catholic Kwandong University Hospital, Incheon, Korea.
- 4Department of Pediatrics, Hallym University Sacred Heart Hospital, Anyang, Korea.
- 5Department of Pediatrics, Seoul National University Bundang Hospital, Seongnam, Korea.
- 6Department of Pediatrics, National Health Insurance Service Ilsan Hospital, Goyang, Korea.
- 7Department of Pediatrics, Gachon University Gil Medical Center, Incheon, Korea.
- 8Department of Pediatrics, College of Medicine, Chungbuk National University, Cheongju, Korea.
- 9Department of Pediatrics, The Catholic University of Korea College of Medicine, Daejeon, Korea.
- 10Department of Pediatrics, Presbyterian Medical Center, Jeonju, Korea.
- 11Department of Pediatrics, Chonnam National University Hospital, Chonnam National University Medical School, Gwangju, Korea.
- 12Department of Pediatrics, Gwangju Veterans Hospital, Gwangju, Korea.
- 13Department of Pediatrics, Catholic University of Daegu School of Medicine, Daegu, Korea.
- 14Department of Pediatrics, Ulsan University Hospital, Ulsan, Korea.
- 15Department of Pediatrics, Pusan National University Yangsan Hospital, Yangsan, Korea.
- 16Department of Pediatrics, Dong-A University College of Medicine, Busan, Korea.
- 17Department of Pediatrics, Health Science Institute, Gyeongsang National University College of Medicine, Jinju, Korea.
- KMID: 2418045
- DOI: http://doi.org/10.4168/aair.2018.10.5.466
Abstract
- BACKGROUND
A US Food and Drug Administration (FDA)-approved drug methacholine chloride (Provocholine®) was recently introduced to Korea where it is now widely used in clinical practice. We aimed to evaluate the prevalence, risk factors and cutoff value of bronchial hyperresponsiveness (BHR) to Provocholine in 7-year-old children.
METHODS
Six hundred and thirty-three children from the Panel Study on Korean Children who visited 16 regional hospitals were evaluated. Skin prick tests, spirometry and bronchial provocation tests for Provocholine as well as a detailed history and physical examinations were performed. The bronchial provocation test was reliably performed on 559 of these children.
RESULTS
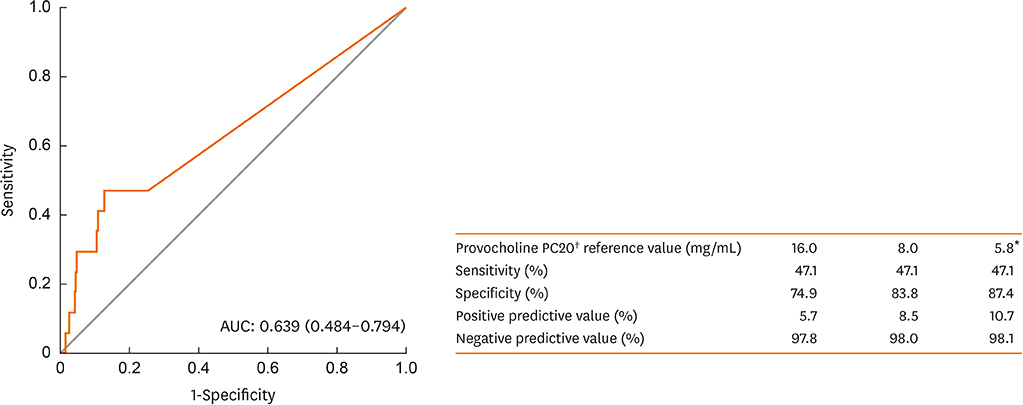
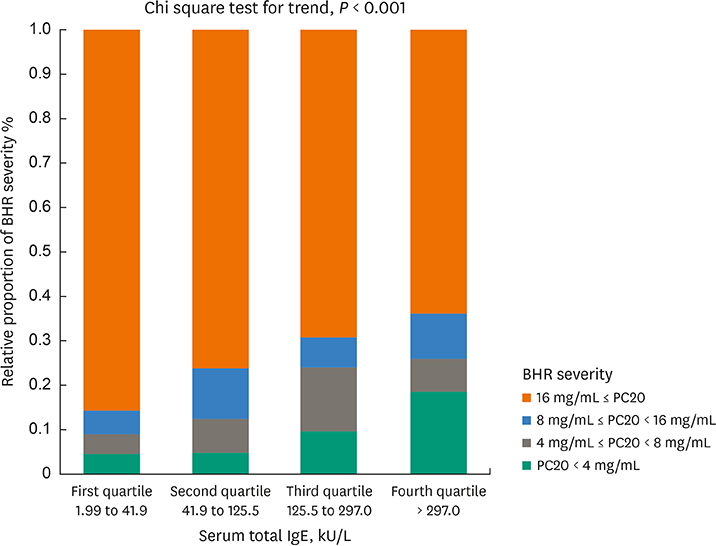
The prevalence of ever-diagnosed asthma via medical records was 7.7%, and that of current asthma (wheezy episode in the last 12 months + diagnosed asthma by physicians) was 3.2%. The prevalence of BHR to Provocholine was 17.2% and 25.8%, respectively, for a PC20 < 8 and < 16 mg/mL. The risk factors for BHR (PC20 < 16 mg/mL) were atopic dermatitis diagnosis and current dog ownership, whereas those for current asthma were allergy rhinitis diagnosis, a history of bronchiolitis before the age of 3, recent use of analgesics/antipyretics and maternal history of asthma. The BHR prevalence trend showed an increase along with the increased immunoglobulin E (IgE) quartile. The cutoff value of PC20 for the diagnosis of current asthma in children at age 7 was 5.8 mg/mL (sensitivity: 47.1%, specificity: 87.4%).
CONCLUSIONS
BHR to Provocholine (PC20 < 8 mg/mL) was observed in 17.2% of 7-year-olds children from the general population and the cutoff value of PC20 for the diagnosis of current asthma was 5.8 mg/mL in this age group. The risk factors for BHR and current asthma showed discrepancies suggesting different underlying mechanisms. Bronchial provocation testing with Provocholine will be a useful clinical tool in the future.
Keyword
MeSH Terms
-
Animals
Asthma
Bronchial Hyperreactivity
Bronchial Provocation Tests
Bronchiolitis
Child*
Dermatitis, Atopic
Diagnosis
Dogs
Humans
Hypersensitivity
Immunoglobulin E
Immunoglobulins
Korea
Medical Records
Methacholine Chloride*
Ownership
Physical Examination
Prevalence*
Rhinitis
Risk Factors*
ROC Curve
Sensitivity and Specificity
Skin
Spirometry
United States Food and Drug Administration
Immunoglobulin E
Immunoglobulins
Methacholine Chloride
Figure
Cited by 2 articles
-
Risk Factors and Comorbidities Associated With the Allergic Rhinitis Phenotype in Children According to the ARIA Classification
Sungsu Jung, So-Yeon Lee, Jisun Yoon, Hyun-Ju Cho, Young-Ho Kim, Dong In Suh, Song-I Yang, Ji-won Kwon, Gwang Cheon Jang, Yong Han Sun, Sung-Il Woo, You-Sook Youn, Kang Seo Park, Eun Lee, Hwa Jin Cho, Myung-Hee Kook, Hye Ryoung Yi, Hai Lee Chung, Ja Hyeong Kim, Hyung Young Kim, Jin A Jung, Hyang-Ok Woo, Jeom-Kyu Lee, Woo-Sung Chang, Nam Hee Do, Hyejoo Cho, Soo-Jong Hong
Allergy Asthma Immunol Res. 2020;12(1):72-85. doi: 10.4168/aair.2020.12.1.72.Indoor pet ownership in infancy is a risk factor for the development of sensitization to pets and asthma in childhood
Sungsu Jung, Soo Ran Noh, So-Yeon Lee, Jisun Yoon, Hyun-Ju Cho, Young-Ho Kim, Dong In Suh, Song-I Yang, Ji-won Kwon, Gwang Cheon Jang, Yong Han Sun, Sung-Il Woo, You-Sook Youn, Kang Seo Park, Eun Lee, Hwa Jin Cho, Myung-Hee Kook, Hye Ryoung Yi, Hai Lee Chung, Ja Hyeong Kim, Hyung Young Kim, Jin A Jung, Hyang-Ok Woo, Soo-Jong Hong
Allergy Asthma Respir Dis. 2019;7(2):99-105. doi: 10.4168/aard.2019.7.2.99.
Reference
-
1. Nair P, Martin JG, Cockcroft DC, Dolovich M, Lemiere C, Boulet LP, et al. Airway hyperresponsiveness in asthma: measurement and clinical relevance. J Allergy Clin Immunol Pract. 2017; 5:649–659.e2.
Article2. Kim SW, Han DH, Lee SJ, Lee CH, Rhee CS. Bronchial hyperresponsiveness in pediatric rhinitis patients: the difference between allergic and nonallergic rhinitis. Am J Rhinol Allergy. 2013; 27:e63–e68.
Article3. Lee E, Lee SH, Kwon JW, Kim YH, Yoon J, Cho HJ, et al. Persistent asthma phenotype related with late-onset, high atopy, and low socioeconomic status in school-aged Korean children. BMC Pulm Med. 2017; 17:45.
Article4. Kim YH, Lee E, Cho HJ, Yang SI, Jung YH, Kim HY, et al. Association between menarche and increased bronchial hyper-responsiveness during puberty in female children and adolescents. Pediatr Pulmonol. 2016; 51:1040–1047.
Article5. Thomas AO, Jackson DJ, Evans MD, Rajamanickam V, Gangnon RE, Fain SB, et al. Sex-related differences in pulmonary physiologic outcome measures in a high-risk birth cohort. J Allergy Clin Immunol. 2015; 136:282–287.
Article6. Harmsen L, Ulrik CS, Porsbjerg C, Thomsen SF, Holst C, Backer V. Airway hyperresponsiveness and development of lung function in adolescence and adulthood. Respir Med. 2014; 108:752–757.
Article7. Jayet PY, Schindler C, Künzli N, Zellweger JP, Brändli O, Perruchoud AP, et al. Reference values for methacholine reactivity (SAPALDIA study). Respir Res. 2005; 6:131.
Article8. Joseph-Bowen J, de Klerk NH, Firth MJ, Kendall GE, Holt PG, Sly PD. Lung function, bronchial responsiveness, and asthma in a community cohort of 6-year-old children. Am J Respir Crit Care Med. 2004; 169:850–854.
Article9. Leynaert B, Bousquet J, Henry C, Liard R, Neukirch F. Is bronchial hyperresponsiveness more frequent in women than in men? A population-based study. Am J Respir Crit Care Med. 1997; 156:1413–1420.10. Sears MR, Burrows B, Flannery EM, Herbison GP, Hewitt CJ, Holdaway MD. Relation between airway responsiveness and serum IgE in children with asthma and in apparently normal children. N Engl J Med. 1991; 325:1067–1071.
Article11. Brutsche MH, Downs SH, Schindler C, Gerbase MW, Schwartz J, Frey M, et al. Bronchial hyperresponsiveness and the development of asthma and COPD in asymptomatic individuals: SAPALDIA cohort study. Thorax. 2006; 61:671–677.
Article12. Kim BS, Jin HS, Kim HB, Lee SY, Kim JH, Kwon JW, et al. Airway hyperresponsiveness is associated with total serum immunoglobulin E and sensitization to aeroallergens in Korean adolescents. Pediatr Pulmonol. 2010; 45:1220–1227.
Article13. Subbarao P, Mandhane PJ, Sears MR. Asthma: epidemiology, etiology and risk factors. CMAJ. 2009; 181:E181–E190.
Article14. Homer RJ, Elias JA. Airway remodeling in asthma: therapeutic implications of mechanisms. Physiology (Bethesda). 2005; 20:28–35.
Article15. Taussig LM, Wright AL, Holberg CJ, Halonen M, Morgan WJ, Martinez FD. Tucson Children's Respiratory Study: 1980 to present. J Allergy Clin Immunol. 2003; 111:661–675.
Article16. Bahk J, Yun SC, Kim YM, Khang YH. Impact of unintended pregnancy on maternal mental health: a causal analysis using follow up data of the Panel Study on Korean Children (PSKC). BMC Pregnancy Childbirth. 2015; 15:85.
Article17. Crapo RO, Casaburi R, Coates AL, Enright PL, Hankinson JL, Irvin CG, et al. Guidelines for methacholine and exercise challenge testing-1999. This official statement of the American Thoracic Society was adopted by the ATS Board of Directors, July 1999. Am J Respir Crit Care Med. 2000; 161:309–329.18. Lee SI. Prevalence of childhood asthma in Korea: international study of asthma and allergies in childhood. Allergy Asthma Immunol Res. 2010; 2:61–64.
Article19. Ahn K, Kim J, Kwon HJ, Chae Y, Hahm MI, Lee KJ, et al. The prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and eczema in Korean children: nationwide cross-sectional survey using complex sampling design. J Korean Med Assoc. 2011; 54:769–778.
Article20. Kwon JW, Kim BJ, Song Y, Seo JH, Kim TH, Yu J, et al. Changes in the prevalence of childhood asthma in Seoul from 1995 to 2008 and its risk factors. Allergy Asthma Immunol Res. 2011; 3:27–33.
Article21. Hong SJ, Ahn KM, Lee SY, Kim KE. The prevalences of asthma and allergic diseases in Korean children. Korean J Pediatr. 2008; 51:343–350.
Article22. D'Amato G, Pawankar R, Vitale C, Lanza M, Molino A, Stanziola A, et al. Climate change and air pollution: effects on respiratory allergy. Allergy Asthma Immunol Res. 2016; 8:391–395.23. Kim MS, Kim YH, Suh DI, Koh YY, Kim BJ, Kim HB, et al. The prevalence of bronchial hyperresponsiveness in elementary school children and its associated factors. Allergy Asthma Respir Dis. 2014; 2:171–178.
Article24. Arshad SH, Kurukulaaratchy RJ, Fenn M, Matthews S. Early life risk factors for current wheeze, asthma, and bronchial hyperresponsiveness at 10 years of age. Chest. 2005; 127:502–508.
Article25. Schwartz J, Schindler C, Zemp E, Perruchoud AP, Zellweger JP, Wüthrich B, et al. Predictors of methacholine responsiveness in a general population. Chest. 2002; 122:812–820.
Article26. Futrakul S, Deerojanawong J, Prapphal N. Risk factors of bronchial hyperresponsiveness in children with wheezing-associated respiratory infection. Pediatr Pulmonol. 2005; 40:81–87.
Article27. Ernst P, Ghezzo H, Becklake MR. Risk factors for bronchial hyperresponsiveness in late childhood and early adolescence. Eur Respir J. 2002; 20:635–639.
Article28. Polgar G, Weng TR. The functional development of the respiratory system from the period of gestation to adulthood. Am Rev Respir Dis. 1979; 120:625–695.29. Busse WW. The contribution of viral respiratory infections to the pathogenesis of airway hyperreactivity. Chest. 1988; 93:1076–1082.
Article30. Zhong NS, Chen RC, Yang MO, Wu ZY, Zheng JP, Li YF. Is asymptomatic bronchial hyperresponsiveness an indication of potential asthma? A two-year follow-up of young students with bronchial hyperresponsiveness. Chest. 1992; 102:1104–1109.31. Lee E, Kim YH, Han S, Yang SI, Jung YH, Seo JH, et al. Different cutoff values of methacholine bronchial provocation test depending on age in children with asthma. World J Pediatr. 2017; 13:439–445.
Article32. Mitchell EA, Beasley R, Keil U, Montefort S, Odhiambo J; ISAAC Phase Three Study Group. The association between tobacco and the risk of asthma, rhinoconjunctivitis and eczema in children and adolescents: analyses from Phase Three of the ISAAC programme. Thorax. 2012; 67:941–949.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Effects of Obesity and Smoking on Bronchial Hyperresponsiveness in Korean Adults
- The effect of immunotherapy on nonspecific bronchial hyperresponsiveness in bronchial asthma and allergic rhinitis
- A 10 Year Follow-up of Childhood Asthma: Potential Risk Factors on Persistence of Nonspecific Bronchial Hyperresponsiveness
- Bronchial Hyperresponsiveness in Workers Exposed to Isocyanates
- Changes in Bronchial Hyperresponsiveness in Children with Asthma