J Korean Soc Surg Hand.
2017 Sep;22(3):208-213. 10.12790/jkssh.2017.22.3.208.
Cutaneous Cryptococcosis Caused by Intravenous Line in Patient with Rheumatoid Arthritis
- Affiliations
-
- 1Department of Orthopedic Surgery, Yeungnam University Medical Center, Daegu, Korea. radiorth@ynu.ac.kr
- 2Department of Plastic Surgery, Yeungnam University Medical Center, Daegu, Korea.
- 3Department of Pathology, Yeungnam University Medical Center, Daegu, Korea.
- KMID: 2391219
- DOI: http://doi.org/10.12790/jkssh.2017.22.3.208
Abstract
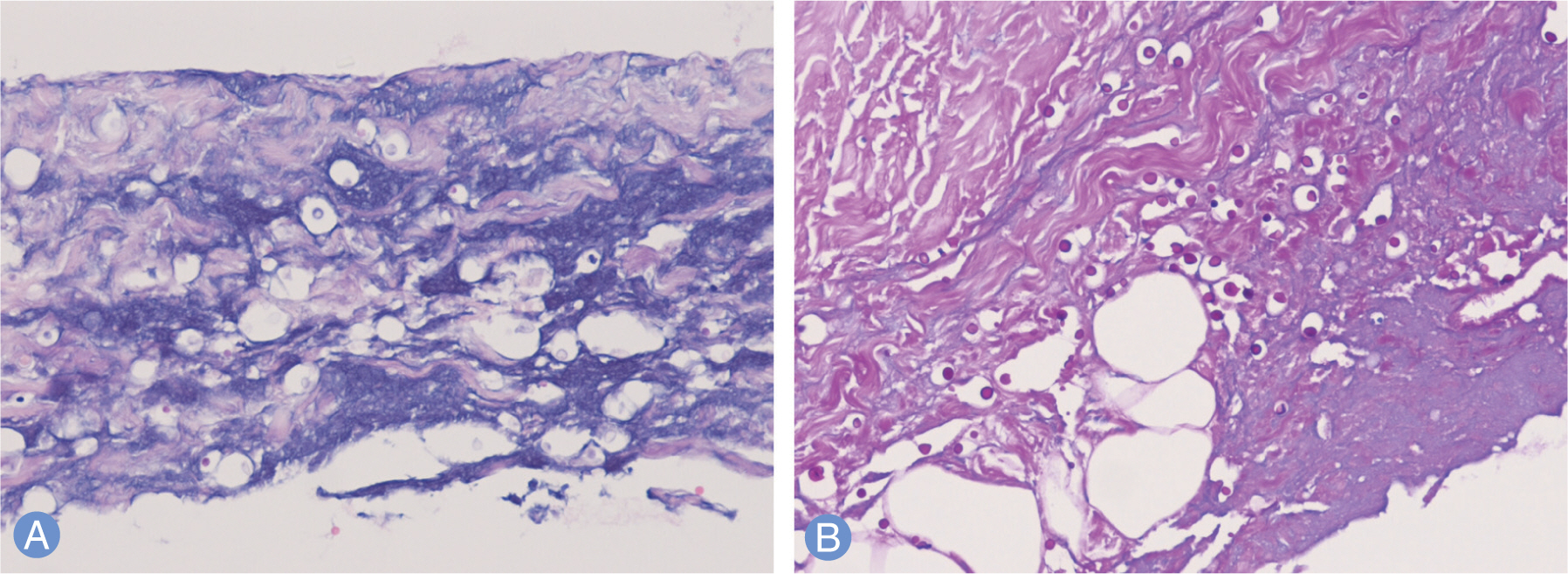
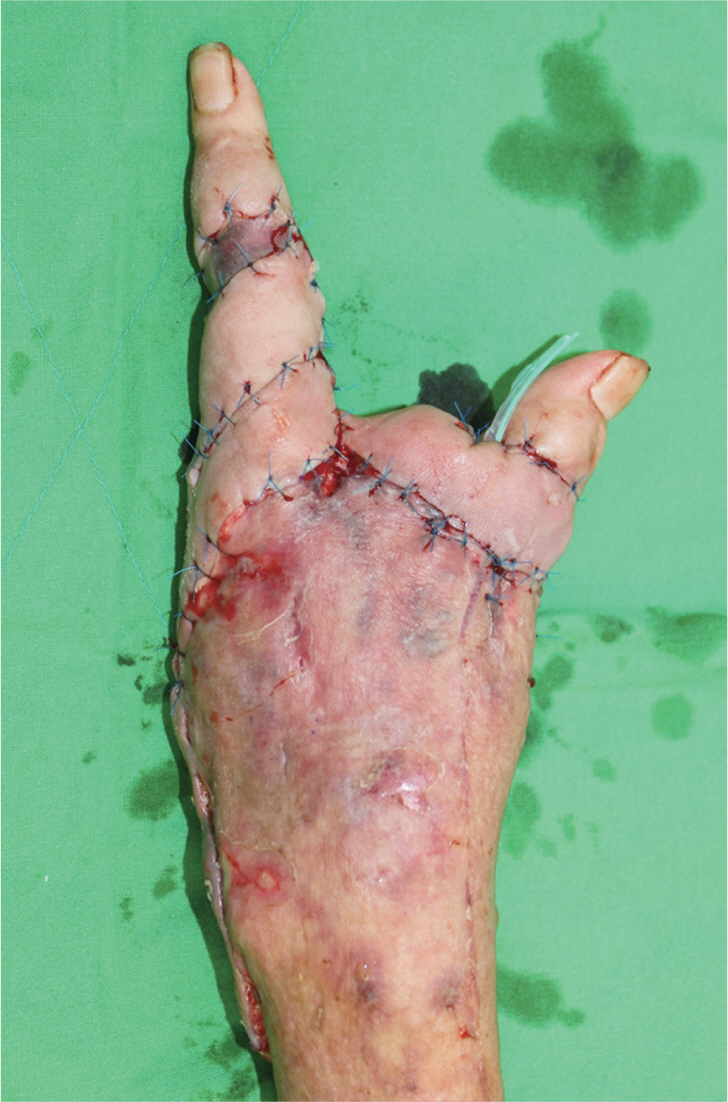
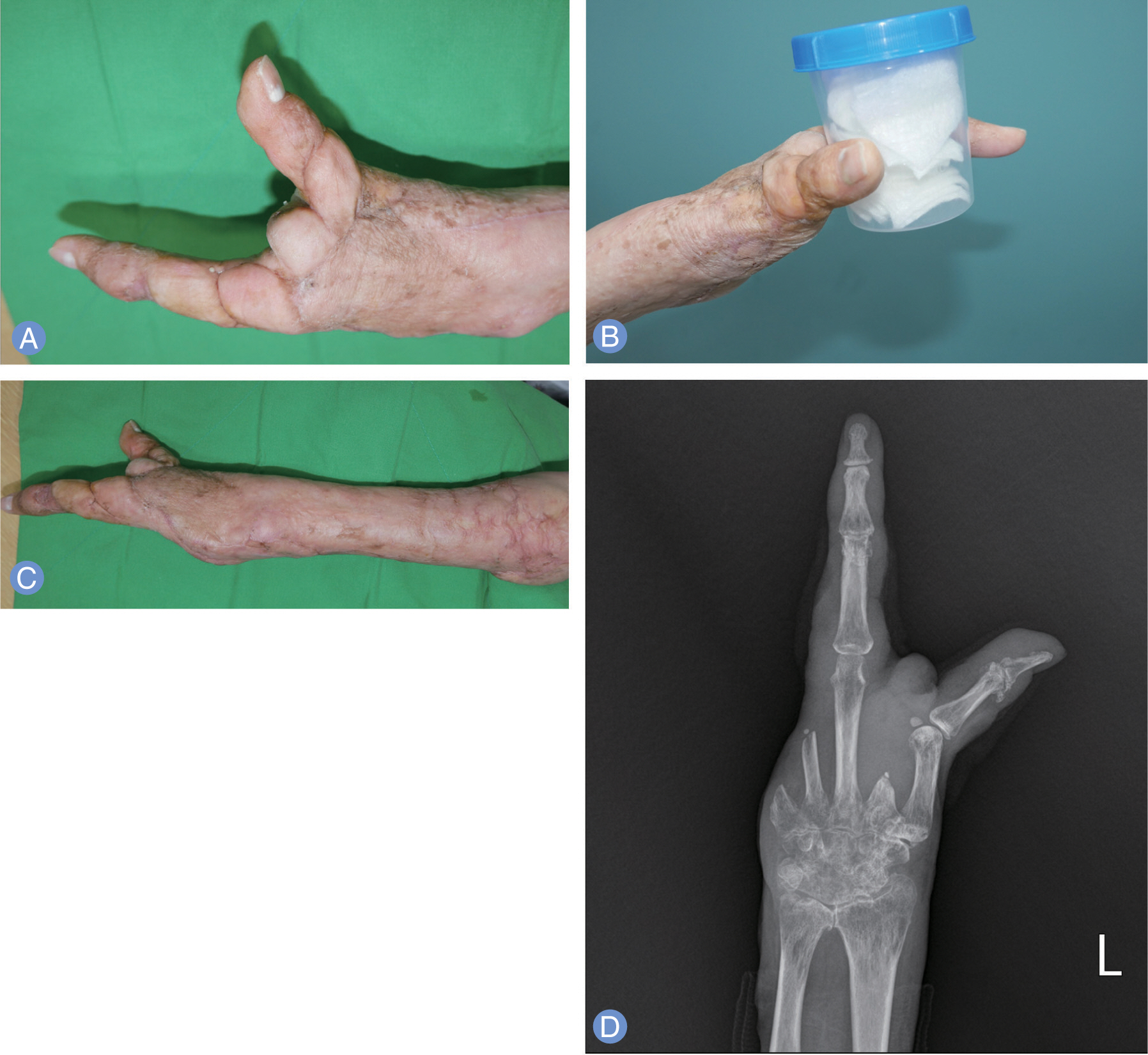
- Primary cutaneous cryptococcosis is a fungal infection caused by Cryptococ cus neoformans which is frequently occurred in the immunosuppressed host. The treatment of primary cutaneous cryptococcosis is mainly fluconazole, and the prognosis is relatively good. We report a case of primary cutaneous cryptococcosis due to intravenous line on the left forearm after lumbar stenosis surgery in a patient with rheumatoid arthritis, who finally underwent second, fourth, and fifth ray amputation.
Keyword
MeSH Terms
Figure
Reference
-
References
1. Sarosi GA, Silberfarb PM, Tosh FE. Cutaneous cryptococcosis: a sentinel of disseminated disease. Arch Dermatol. 1971; 104:1–3.
Article2. Shin DH, Kim KS, Lee JM, Choi JS, Kim KH. Primary cutaneous cryptococcosis. Ann Dermatol. 1999; 11:27–9.
Article3. Neuville S, Dromer F, Morin O, et al. Primary cutaneous cryptococcosis: a distinct clinical entity. Clin Infect Dis. 2003; 36:337–47.
Article4. Kim YG, Kim HW, Park HC, Kim JE, Ko JY, Ro YS. Primary cutaneous cryptococcosis mimicking herpes zoster. Korean J Dermatol. 2013; 51:343–7.5. Ko YJ, Hong MH, Park CM, Moon HW, Hur M, Yun YM. Primary cutaneous cryptococcosis in a patient with iatrogenic Cushing’s syndrome: a case report and review of the literature. Korean J Clin Microbiol. 2012; 15:70–3.
Article6. Revenga F, Paricio JF, Merino FJ, Nebreda T, Ramirez T, Martinez AM. Primary cutaneous cryptococcosis in an immunocompetent host: case report and review of the literature. Dermatology. 2002; 204:145–9.
Article7. Kim JH, Shin DJ, Byun YS, Kim SW, Kim TE. Cryptococcal tenosynovitis of the hand in a patient with rheumatiod arthritis: a case report. J Korean Soc Surg Hand. 2011; 16:251–4.8. Kim YJ, Seo SJ, Ro BI. A case of primary cutaneous cryptococcosis misdiagnosel as skin tuberculosis. Korean J Med Mycol. 2003; 8:16–20.9. Noble RC, Fajardo LF. Primary cutaneous cryptococcosis: review and morphologic study. Am J Clin Pathol. 1972; 57:13–22.
Article10. Chen SC, Sorrell TC, Chang CC, Paige EK, Bryant PA, Slavin MA. Consensus guidelines for the treatment of yeast infections in the haematology, oncology and intensive care setting, 2014. Intern Med J. 2014; 44:1315–32.
Article
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Cryptococcal Tenosynovitis of the Hand in a Patient with Rheumatiod Arthritis: A Case Report
- A Case of Pulmonary Cryptococcosis in a Patient with Rheumatoid Arthritis
- Three Cases of Cryptococcosis with Cutaneous Manifestations
- A Case of Cutaneous Cryptococcosis Resembling Pyoderma Gangrenosum
- A Case of Disseminated Cryptococcosis with Skin Involvement in a Rheumatic Arthritis Patient During Long-term Tacrolimus Therapy