J Korean Med Sci.
2012 Aug;27(8):870-875. 10.3346/jkms.2012.27.8.870.
Abdominal Aortic Calcification is Associated with Diastolic Dysfunction, Mortality, and Nonfatal Cardiovascular Events in Maintenance Hemodialysis Patients
- Affiliations
-
- 1Division of Nephrology, Department of Internal Medicine, Incheon St. Mary's Hospital, Incheon, Korea. imkidney@catholic.ac.kr
- 2Department of Internal Medicine, College of Medicine, The Catholic University of Korea, Incheon, Korea.
- 3Department of Radiology, College of Medicine, The Catholic University of Korea, Incheon, Korea.
- KMID: 1714197
- DOI: http://doi.org/10.3346/jkms.2012.27.8.870
Abstract
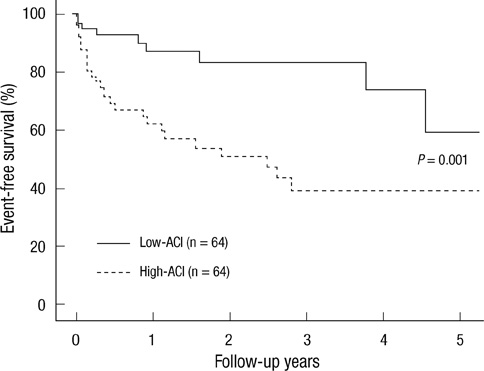
- This study evaluated the significance of aortic calcification index (ACI), an estimate of abdominal aortic calcification by plain abdominal computed tomography (CT), in terms of left ventricular (LV) diastolic dysfunction, mortality, and nonfatal cardiovascular (CV) events in chronic hemodialysis patients. Hemodialysis patients who took both an abdominal CT and echocardiography were divided into a low-ACI group (n = 64) and a high-ACI group (n = 64). The high-ACI group was significantly older, had a longer dialysis vintage and higher comorbidity indices, and more patients had a previous history of CV disease than the low-ACI group. The ACI was negatively correlated with LV end-diastolic volume or LV stroke volume, and was positively correlated with the ratio of peak early transmitral flow velocity to peak early diastolic mitral annular velocity (E/E' ratio), a marker of LV diastolic function. The E/E' ratio was independently associated with the ACI. The event-free survival rates for mortality and nonfatal CV events were significantly lower in the high-ACI group compared with those in the low-ACI group, and the ACI was an independent predictor for all-cause deaths and nonfatal CV events. In conclusion, ACI is significantly associated with diastolic dysfunction and predicts all-cause mortality and nonfatal CV events in hemodialysis patients.
Keyword
MeSH Terms
-
Adult
Age Factors
Aged
Aged, 80 and over
Aorta, Abdominal
Blood Flow Velocity
Blood Pressure
Calcinosis/*etiology
Cardiovascular Diseases/*complications
Disease-Free Survival
Echocardiography
Female
Follow-Up Studies
Humans
Kaplan-Meier Estimate
Kidney Failure, Chronic/*complications/mortality
Male
Middle Aged
Predictive Value of Tests
Prognosis
Regression Analysis
Renal Dialysis
Risk Factors
Tomography, X-Ray Computed
Ventricular Dysfunction, Left/complications/*physiopathology
Figure
Reference
-
1. Foley RN, Murray AM, Li S, Herzog CA, McBean AM, Eggers PW, Collins AJ. Chronic kidney disease and the risk for cardiovascular disease, renal replacement, and death in the United States Medicare population, 1998 to 1999. J Am Soc Nephrol. 2005. 16:489–495.2. London GM, Guerin AP, Marchais SJ, Metivier F, Pannier B, Adda H. Arterial media calcification in end-stage renal disease: impact on all-cause and cardiovascular mortality. Nephrol Dial Transplant. 2003. 18:1731–1740.3. Raggi P, Bellasi A. Clinical assessment of vascular calcification. Adv Chronic Kidney Dis. 2007. 14:37–43.4. Witteman JC, Kok FJ, van Saase JL, Valkenburg HA. Aortic calcification as a predictor of cardiovascular mortality. Lancet. 1986. 2:1120–1122.5. Raggi P, Bellasi A, Ferramosca E, Islam T, Muntner P, Block GA. Association of pulse wave velocity with vascular and valvular calcification in hemodialysis patients. Kidney Int. 2007. 71:802–807.6. Sigrist M, Bungay P, Taal MW, McIntyre CW. Vascular calcification and cardiovascular function in chronic kidney disease. Nephrol Dial Transplant. 2006. 21:707–714.7. Fujiu A, Ogawa T, Matsuda N, Ando Y, Nitta K. Aortic arch calcification and arterial stiffness are independent factors for diastolic left ventricular dysfunction in chronic hemodialysis patients. Circ J. 2008. 72:1768–1772.8. Kabaya T, Nitta K, Kimura H, Kawashima A, Narusawa K, Nihei H. Increased aortic calcification index in hemodialysis patients. Nephron. 1999. 81:354–355.9. Nitta K, Akiba T, Uchida K, Kawashima A, Yumura W, Kabaya T, Nihei H. The progression of vascular calcification and serum osteoprotegerin levels in patients on long-term hemodialysis. Am J Kidney Dis. 2003. 42:303–309.10. Nitta K, Akiba T, Uchida K, Otsubo S, Otsubo Y, Takei T, Ogawa T, Yumura W, Kabaya T, Nihei H. Left ventricular hypertrophy is associated with arterial stiffness and vascular calcification in hemodialysis patients. Hypertens Res. 2004. 27:47–52.11. Takei T, Otsubo S, Uchida K, Matsugami K, Mimuro T, Kabaya T, Akiba T, Nitta K. Effects of sevelamer on the progression of vascular calcification in patients on chronic haemodialysis. Nephron Clin Pract. 2008. 108:c278–c283.12. Taniwaki H, Ishimura E, Tabata T, Tsujimoto Y, Shioi A, Shoji T, Inaba M, Inoue T, Nishizawa Y. Aortic calcification in haemodialysis patients with diabetes mellitus. Nephrol Dial Transplant. 2005. 20:2472–2478.13. Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987. 40:373–383.14. de Simone G, Devereux RB, Roman MJ, Alderman MH, Laragh JH. Relation of obesity and gender to left ventricular hypertrophy in normotensive and hypertensive adults. Hypertension. 1994. 23:600–606.15. Schiller NB, Shah PM, Crawford M, DeMaria A, Devereux R, Feigenbaum H, Gutgesell H, Reichek N, Sahn D, Schnittger I, et al. Recommendations for quantitation of the left ventricle by two-dimensional echocardiography. American Society of Echocardiography Committee on Standards, Subcommittee on Quantitation of Two-Dimensional Echocardiograms. J Am Soc Echocardiogr. 1989. 2:358–367.16. Rakowski H, Appleton C, Chan KL, Dumesnil JG, Honos G, Jue J, Koilpillai C, Lepage S, Martin RP, Mercier LA, et al. Canadian consensus recommendations for the measurement and reporting of diastolic dysfunction by echocardiography: from the investigators of consensus on diastolic dysfunction by echocardiography. J Am Soc Echocardiogr. 1996. 9:736–760.17. Nagueh SF, Middleton KJ, Kopelen HA, Zoghbi WA, Quinones MA. Doppler tissue imaging: a noninvasive technique for evaluation of left ventricular relaxation and estimation of filling pressures. J Am Coll Cardiol. 1997. 30:1527–1533.18. Guerin AP, London GM, Marchais SJ, Metivier F. Arterial stiffening and vascular calcifications in end-stage renal disease. Nephrol Dial Transplant. 2000. 15:1014–1021.19. Shoji T, Nishizawa Y, Kawagishi T, Kawasaki K, Taniwaki H, Tabata T, Inoue T, Morii H. Intermediate-density lipoprotein as an independent risk factor for aortic atherosclerosis in hemodialysis patients. J Am Soc Nephrol. 1998. 9:1277–1284.20. Chertow GM, Raggi P, Chasan-Taber S, Bommer J, Holzer H, Burke SK. Determinants of progressive vascular calcification in haemodialysis patients. Nephrol Dial Transplant. 2004. 19:1489–1496.21. Honkanen E, Kauppila L, Wikstrom B, Rensma PL, Krzesinski JM, Aasarod K, Verbeke F, Jensen PB, Mattelaer P, Volck B. Abdominal aortic calcification in dialysis patients: results of the cord study. Nephrol Dial Transplant. 2008. 23:4009–4015.22. Sharma R, Pellerin D, Gaze DC, Mehta RL, Gregson H, Streather CP, Collinson PO, Brecker SJ. Mitral peak doppler e-wave to peak mitral annulus velocity ratio is an accurate estimate of left ventricular filling pressure and predicts mortality in end-stage renal disease. J Am Soc Echocardiogr. 2006. 19:266–273.23. Westermann D, Kasner M, Steendijk P, Spillmann F, Riad A, Weitmann K, Hoffmann W, Poller W, Pauschinger M, Schultheiss HP, et al. Role of left ventricular stiffness in heart failure with normal ejection fraction. Circulation. 2008. 117:2051–2060.24. Foley RN, Parfrey PS, Harnett JD, Kent GM, Murray DC, Barre PE. The prognostic importance of left ventricular geometry in uremic cardiomyopathy. J Am Soc Nephrol. 1995. 5:2024–2031.25. Fathi R, Isbel N, Haluska B, Case C, Johnson DW, Marwick TH. Correlates of subclinical left ventricular dysfunction in ESRD. Am J Kidney Dis. 2003. 41:1016–1025.26. Graham RJ, Gelman JS, Donelan L, Mottram PM, Peverill RE. Effect of preload reduction by haemodialysis on new indices of diastolic function. Clin Sci (Lond). 2003. 105:499–506.27. Shanahan CM, Cary NR, Salisbury JR, Proudfoot D, Weissberg PL, Edmonds ME. Medial localization of mineralization-regulating proteins in association with Monckeberg's sclerosis: evidence for smooth muscle cell-mediated vascular calcification. Circulation. 1999. 100:2168–2176.28. Wang AY, Wang M, Lam CW, Chan IH, Zhang Y, Sanderson JE. Left ventricular filling pressure by doppler echocardiography in patients with end-stage renal disease. Hypertension. 2008. 52:107–114.
- Full Text Links
- Actions
-
Cited
- CITED
-
- Close
- Share
- Similar articles
-
- Clinical Implication of Vascular Calcification in Patients Undergoing Hemodialysis: The End or the Beginning of Disease
- Serum Osteoprotegerin Levels and the Extent of Aortic Calcification in Hemodialysis Patients
- Association between mortality and abdominal aortic calcification and their progression in hemodialysis patients
- Surgical Repair of Abdominal Aortic Aneurysm under Epidural Anesthesia in Patient with Chronic Obstructive Pulmonary Disease : A case report
- Predictive Value of Echocardiographic Parameters for Clinical Events in Patients Starting Hemodialysis