Korean J Ophthalmol.
2005 Mar;19(1):68-72. 10.3341/kjo.2005.19.1.68.
A Case Refort of Sandhoff Disease
- Affiliations
-
- 1Department of Ophthalmology, College of Medicine, Chungnam National University, Daejeon, Korea. irismd@cnuh.co.kr
- KMID: 1099088
- DOI: http://doi.org/10.3341/kjo.2005.19.1.68
Abstract
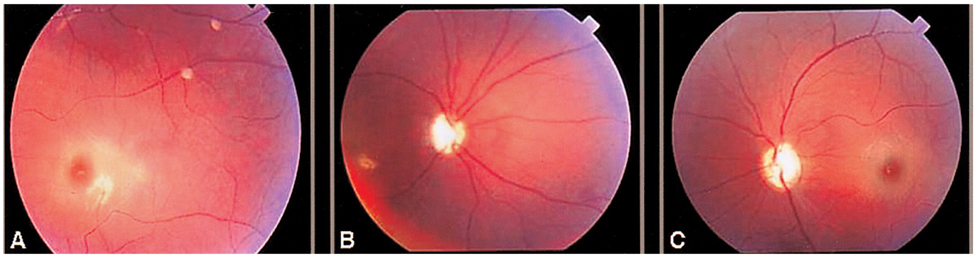
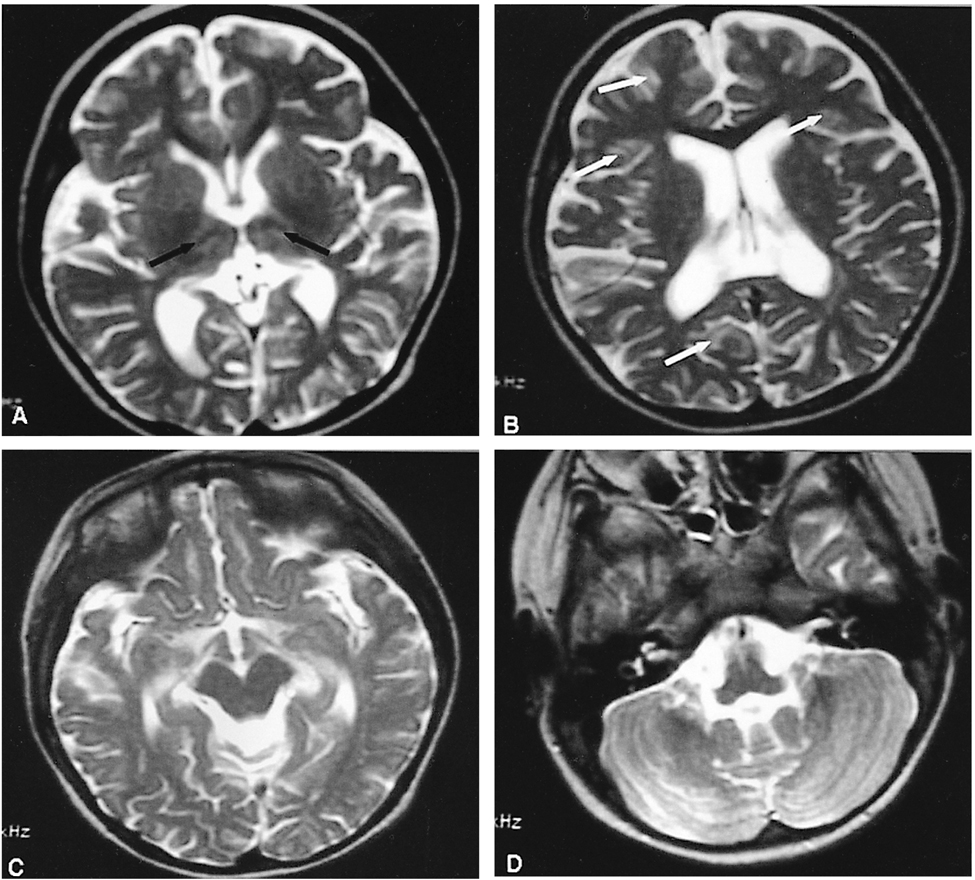
- Sandhoff disease is a rare autosomal recessive metabolic disease presenting bilateral optic atrophy and a cherry red spot in the macula. This case report presents the characteristics of a patient with Sandhoff disease as assessed by ophthalmic, neuroimaging, and laboratory procedures. Ophthalmologic examination revealed that the patient could not fixate her eyes on objects nor follow moving targets. A pale optic disc and a cherry red spot in the macula were seen in both eyes. Low signal intensity at the thalamus and high signal intensity at the cerebral white matter were noted in a T2-weighted brain MR image. A lysosomal enzyme assay using fibroblasts showed the marked reduction of both total beta-hexosaminidases, A and B. Based on the above clinical manifestations and laboratory findings, we diagnosed the patient as having Sandhoff disease.
MeSH Terms
-
Atrophy
Cerebral Cortex/*pathology
Child, Preschool
Female
Humans
Isoenzymes/deficiency
Lipid Metabolism, Inborn Errors/*diagnosis/enzymology
Magnetic Resonance Imaging
Ocular Motility Disorders/*diagnosis
Optic Disk/*pathology
Retinal Diseases/*diagnosis
Sandhoff Disease/*diagnosis/enzymology
Thalamus/pathology
beta-N-Acetylhexosaminidase/deficiency
Figure
Reference
-
1. Sandhoff K, Conzelmann E, Neufeld EF, et al. Scriver CV, Beaudet AL, Sly WS, Valle D, editors. The GM2 gangliosidosis. The Metabolic Basis of Inherited Disease. 1989. New York: McGraw-Hill;1807–1839.2. O'Dowd BF, Klavins MH, Willard HF, et al. Molecular heterogenicity in the infantile and juvenile forms of Sandhoff disease (O-variant GM2 gangliosidosis). J Biol Chem. 1985. 261:12680–12685.3. Der Kaloustian VM, Khoury MJ, Hallal R, et al. Sandhoff disease: a prevalent form of infantile GM2 gangliosidosis in Lebanon. Am J Hum Genet. 1981. 33:85–89.4. Cashman N, Antel JP, Hancock LW, et al. N-acetyl-β-hexosaminidase β locus defect and juvenile motor neuron disease: a case study. Ann Neurol. 1986. 19:568–572.5. Oonk JGW, Van der Helm HJ, Martin JJ. Spinocerebellar degeneration: hexosaminidase A and B deficiency in two adult sisters. Neurology. 1979. 29:380–384.6. Federico A, Ciacci G, D'Amore A, et al. GM2 gangliosidosis with hexosamindase A and B defect: report of a family with motor neuron disease like phenotype. J Inher Metab Dis. 1986. 9:S307–S310.7. Gomez-Lira M, Sangalli A, Mottes M, et al. A common beta hexosaminidase gene mutation in an adult Sandhoff disease patients. Hum Genet. 1995. 96:417–422.8. Barbeau A, Plasse L, Cloutier T, et al. Lysosomal enzymes in ataxia: discovery of two new cases of late onset hexosaminidase A and B deficiency (adult Sandhoff disease) in French Canadians. Can J Neurol Sci. 1984. 11:601–606.9. Wakamatsu N. Recent advance in molecular genetics of GM2 gangliosidosis. Nippon Rinsho. 1995. 53:2988–2993.10. Gravel RA, Clarke JT, Kaback MM, et al. Scriver CR, Beaudet AL, Sly WS, Valle D, editors. The GM2 gangliosidoses. The metabolic and molecular bases of inherited disease. 1995. 7th ed. New York: McGraw-Hill;2839–2879.11. O'Brien JS, Okada S, Chen A, Fillerup DL. Tay-Sachs disease: detection of heterozygotes and homozygotes by serum hexosaminidase assay. N Eng J Med. 1970. 283:15–20.12. Hittmair K, Wimberger D, Bernert G, et al. MRI in a case of Sanhoff's disease. Neuroradiology. 1996. 38:S178–S180.13. Koelfen W, Freund M, Jaschke W, et al. GM2 gangliosidois (Sandhoff's disease): two year follow up by MRI. Neuroradiology. 1994. 36:152–154.